Flow chart for pathophysiology for asthma
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Generating Image
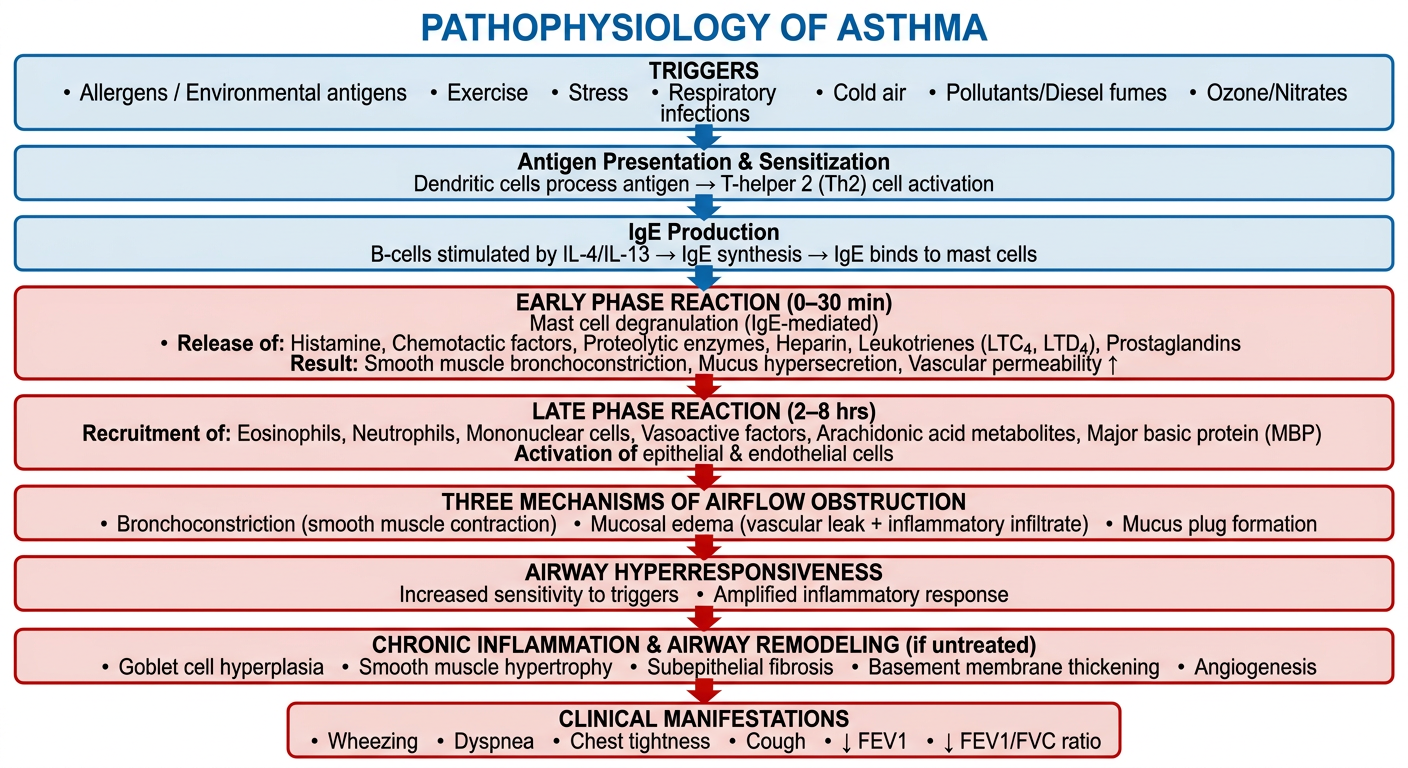
Here is the flowchart, and below is a structured walkthrough of each step:
Pathophysiology of Asthma
1. Triggers
Allergens, exercise, stress, respiratory infections, cold air, pollutants (diesel fumes, ozone, nitrates).
2. Sensitization Phase
- Antigen presented by dendritic cells → Th2 cell activation
- Th2 cells release IL-4, IL-5, IL-13
- B-cells stimulated → IgE synthesis
- IgE binds to mast cells and basophils (sensitization complete)
3. Early Phase Reaction (0–30 min)
Re-exposure to antigen → IgE-mediated mast cell degranulation:
- Preformed mediators: Histamine, chemotactic factors, heparin, proteolytic enzymes
- Secondary mediators: Leukotrienes (LTC4, LTD4), prostaglandins, PAF
Immediate effects:
- Smooth muscle bronchoconstriction
- Mucus hypersecretion
- ↑ Vascular permeability → mucosal edema
4. Late Phase Reaction (2–8 hrs)
Recruitment of inflammatory cells:
- Eosinophils, neutrophils, mononuclear cells, basophils
These release:
- Cytokines: IL-3 to IL-6, TNF-α, IFN-γ
- Arachidonic acid metabolites
- Major basic protein (MBP) from eosinophils → epithelial damage
- Activation of epithelial and endothelial cells amplifying the response
5. Three Mechanisms of Airflow Obstruction
| Mechanism | Cause |
|---|---|
| Bronchoconstriction | Smooth muscle contraction |
| Mucosal edema | Vascular leak + inflammatory infiltrate |
| Mucus plug formation | Goblet cell hypersecretion |
6. Airway Hyperresponsiveness
- Chronic inflammation lowers the threshold for bronchoconstriction
- Even mild stimuli trigger exaggerated responses
7. Chronic Inflammation → Airway Remodeling (if untreated)
- Goblet cell hyperplasia
- Smooth muscle hypertrophy
- Subepithelial fibrosis
- Basement membrane thickening
- Angiogenesis
- Leads to irreversible airflow limitation
8. Clinical Manifestations
- Wheezing, dyspnea, chest tightness, cough
- ↓ FEV₁, ↓ FEV₁/FVC ratio (< 0.75 in adults)
- Reversible with bronchodilators (unlike COPD)
Reference diagram from textbook (normal vs. asthmatic bronchus):
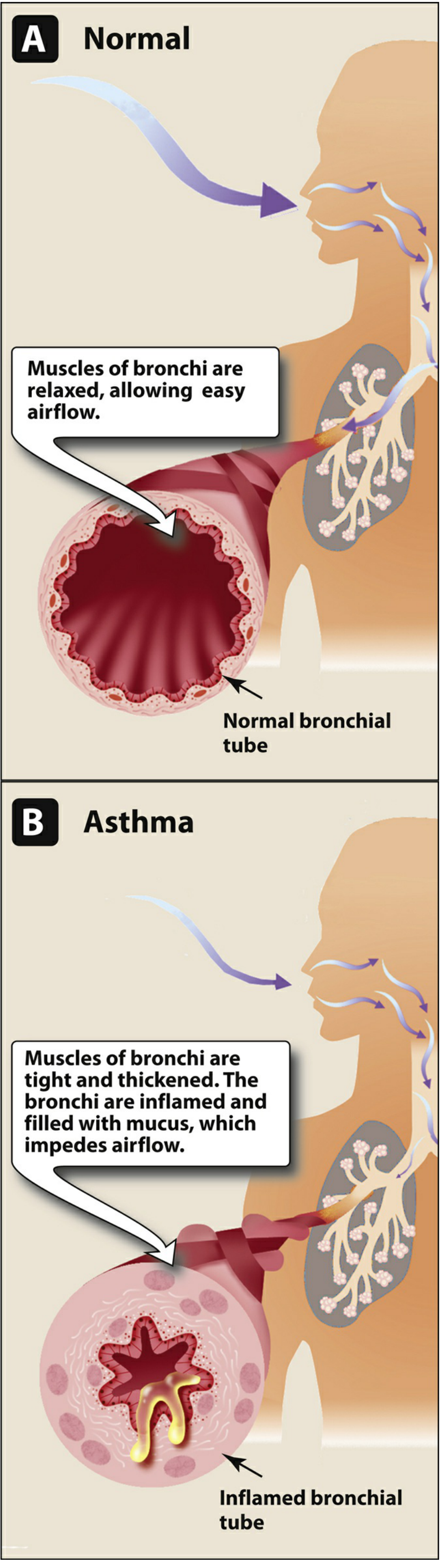
Sources: Lippincott Illustrated Reviews: Pharmacology; Swanson's Family Medicine Review
This is a shared conversation. Sign in to Orris to start your own chat.