Short note on synovial joints
Reading File
Finding Sources
Searching Images
synovial joint structure anatomy diagram
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a short note on synovial joints, drawn from Gray's Anatomy for Students, the THIEME Atlas of Anatomy, and Junqueira's Basic Histology.
Synovial Joints
Definition
Synovial joints (also called diarthroses or true joints) are freely movable articulations in which the opposing bone surfaces are separated by a fluid-filled articular cavity. They are the most common and functionally important type of joint in the body.
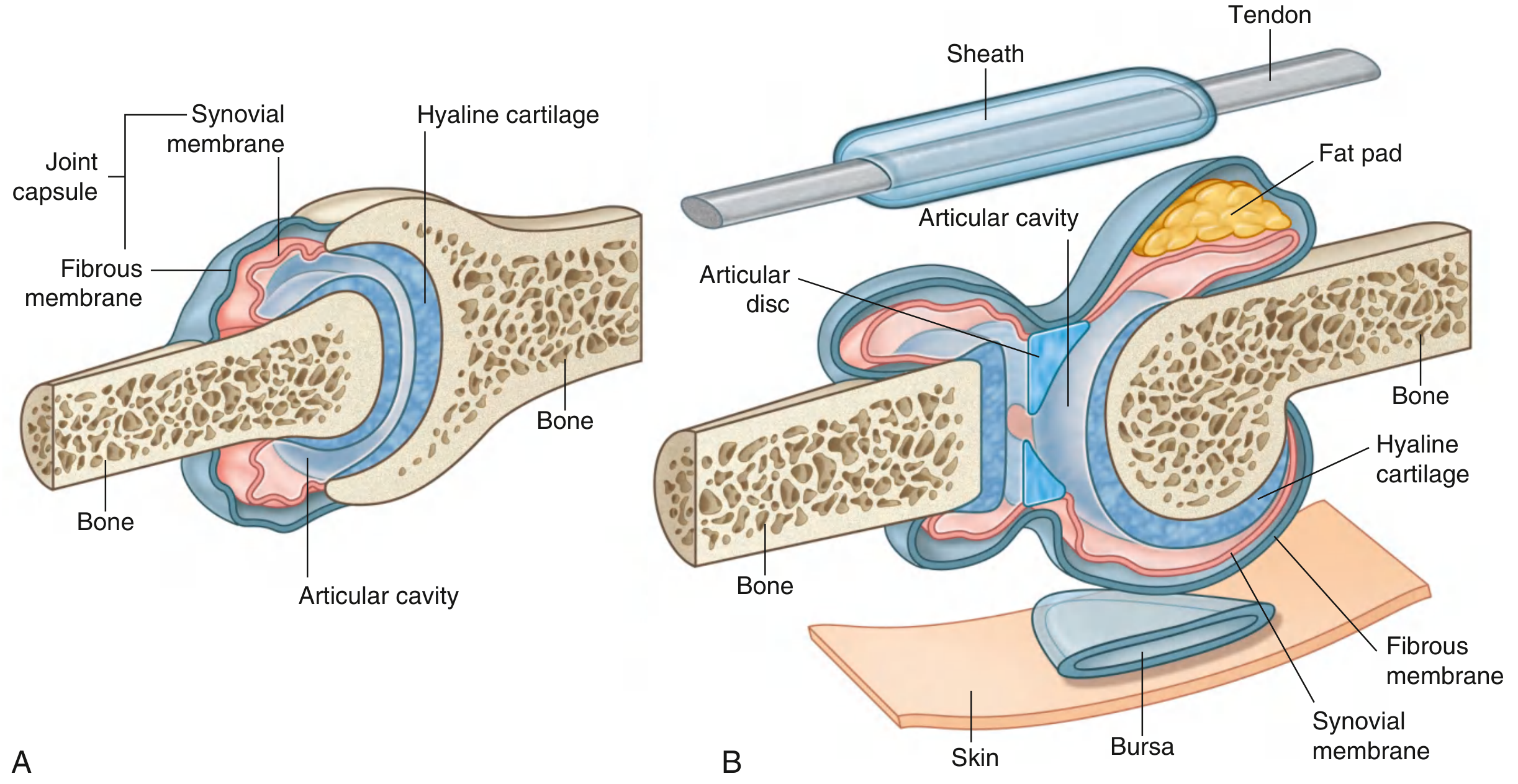
Essential Features
All synovial joints share the following characteristic components:
| Component | Description |
|---|---|
| Articular cartilage | Hyaline cartilage covers opposing bone surfaces; avoids direct bone-on-bone contact; absorbs compressive forces |
| Articular (joint) cavity | A potential space between the articulating surfaces filled with synovial fluid |
| Joint capsule | Surrounds the joint; has two layers: an outer fibrous membrane (dense connective tissue, stabilises the joint) and an inner synovial membrane |
| Synovial membrane | Highly vascular lining that produces synovial fluid; not a true epithelium — cells lack a basal lamina |
| Synovial fluid | Clear, viscous fluid that lubricates articular surfaces and nourishes avascular articular cartilage |
| Ligaments | Thickenings of the fibrous capsule or separate extracapsular bands; primary stabilisers |
Synovial Membrane — Histology
The synovial membrane contains two specialised cell types (synoviocytes):
- Type A cells (macrophage-like) — derived from blood monocytes; phagocytose wear debris from synovial fluid
- Type B cells (fibroblast-like) — mesenchyme-derived; synthesise hyaluronan and proteoglycans, which give synovial fluid its viscosity and lubricating properties
Capillaries in the synovial membrane are fenestrated, facilitating exchange of water and nutrients between blood and joint fluid. — Junqueira's Basic Histology, 17e
Accessory Intra-articular Structures
Not all joints have these, but they improve congruency and load distribution:
- Menisci — crescent-shaped fibrocartilage wedges (e.g., knee); increase contact area and absorb shock
- Articular discs — divide the joint cavity into two chambers (e.g., temporomandibular joint, sternoclavicular joint)
- Articular labra — fibrocartilaginous rims that deepen the socket (e.g., glenoid labrum of shoulder, acetabular labrum of hip)
- Fat pads — occupy recesses between synovial membrane and capsule; fill spaces as joint contours change
- Bursae — closed synovial sacs near (and sometimes communicating with) the joint; reduce friction
Types of Synovial Joints
Classified by shape of articular surfaces and axes of movement:
| Type | Axes | Movement | Example |
|---|---|---|---|
| Plane | Gliding | Sliding/gliding | Acromioclavicular joint |
| Hinge | Uniaxial | Flexion / Extension | Elbow (humero-ulnar) |
| Pivot | Uniaxial (longitudinal) | Rotation | Atlanto-axial joint |
| Bicondylar | Mainly uniaxial + limited rotation | Flex/Ext + slight rotation | Knee joint |
| Condylar (ellipsoid) | Biaxial | Flex, Ext, Abd, Add, Circumduction | Wrist joint |
| Saddle | Biaxial | Flex, Ext, Abd, Add, Circumduction | Carpometacarpal joint of thumb |
| Ball and socket | Multiaxial | All movements including rotation | Hip, shoulder |
Blood Supply, Nerve Supply & Lymphatics
- Synovial joints receive their blood supply from periarticular arterial anastomoses.
- Nerves supply the joint capsule and ligaments; articular cartilage is avascular and aneural.
- Hilton's Law: the nerve supplying a joint also supplies the muscles moving that joint and the skin over their insertions.
Clinical Relevance
- Osteoarthritis — degenerative loss of articular cartilage, narrowing of joint space; most common joint disease
- Rheumatoid arthritis — autoimmune synovitis; hyperplastic synovial membrane (pannus) erodes cartilage and bone
- Haemarthrosis / effusion — blood or excess fluid in the joint cavity, detectable clinically and on imaging
- Joint aspiration (arthrocentesis) — sampling of synovial fluid for cell count, crystals (gout, pseudogout), and culture
Sources: Gray's Anatomy for Students (9780323934237); THIEME Atlas of Anatomy: General Anatomy & Musculoskeletal System (9781626237186); Junqueira's Basic Histology, 17e (9781264930395)
This is a shared conversation. Sign in to Orris to start your own chat.