I now have everything needed for a comprehensive, well-illustrated Chapter 1. Let me compose the full response:
Chapter 1: The Nervous System — Organization, Synaptic Transmission & Special Senses
Part 1 — Synaptic Transmission
The Synapse
The synapse has two sides: presynaptic and postsynaptic, indicating the usual direction of information flow. The presynaptic side is generally an axon terminal; the postsynaptic side is usually a dendrite or soma of another neuron. The narrow space between them is the synaptic cleft.
"At most synapses, information in the form of electrical impulses traveling down the axon is converted by the presynaptic terminal into a chemical signal that crosses the synaptic cleft. On the postsynaptic membrane, this chemical signal is converted again into an electrical one."
— Neuroscience: Exploring the Brain, 5th Ed.
A. Chemical Synapses
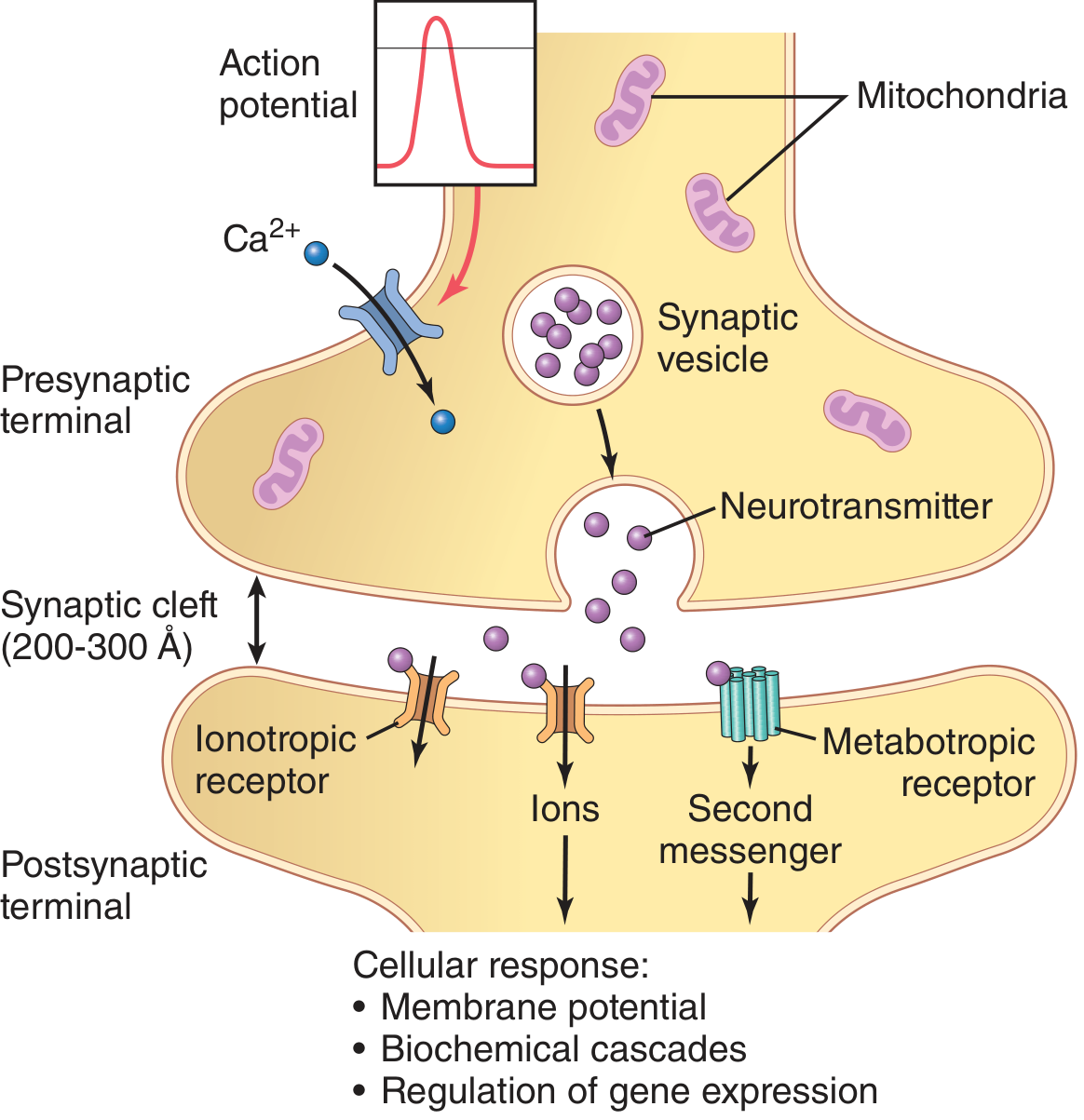
Chemical synapses transmit signals in one direction only (presynaptic → postsynaptic). This is the predominant synapse type in the CNS.
Mechanism of transmission:
- An action potential arrives at the presynaptic terminal
- Voltage-gated Ca²⁺ channels open → Ca²⁺ influx
- Ca²⁺ triggers fusion of synaptic vesicles with the presynaptic membrane
- Neurotransmitter is released into the synaptic cleft (200–300 Å wide)
- Neurotransmitter binds to postsynaptic receptors — either ionotropic (direct ion channel opening) or metabotropic (G-protein/second messenger cascade)
- Result: change in postsynaptic membrane potential, biochemical cascades, or gene expression
Fig. Chemical synapse: action potential → Ca²⁺ influx → neurotransmitter release → ionotropic or metabotropic receptor activation (Guyton & Hall Medical Physiology)
Postsynaptic receptor types:
| Receptor Type | Mechanism | Speed | Example |
|---|
| Ionotropic | Ligand-gated ion channel | Fast (ms) | AMPA, GABA-A, nAChR |
| Metabotropic | G-protein → 2nd messenger | Slow (seconds) | mGluR, GABA-B, muscarinic |
Neurotransmitter inactivation occurs by:
- Reuptake into the presynaptic terminal via monoamine transporters (SERT, NET, DAT — SLC6 family, 12-transmembrane proteins)
- Enzymatic degradation (e.g., acetylcholinesterase for ACh)
- Diffusion away from the cleft
B. Electrical Synapses
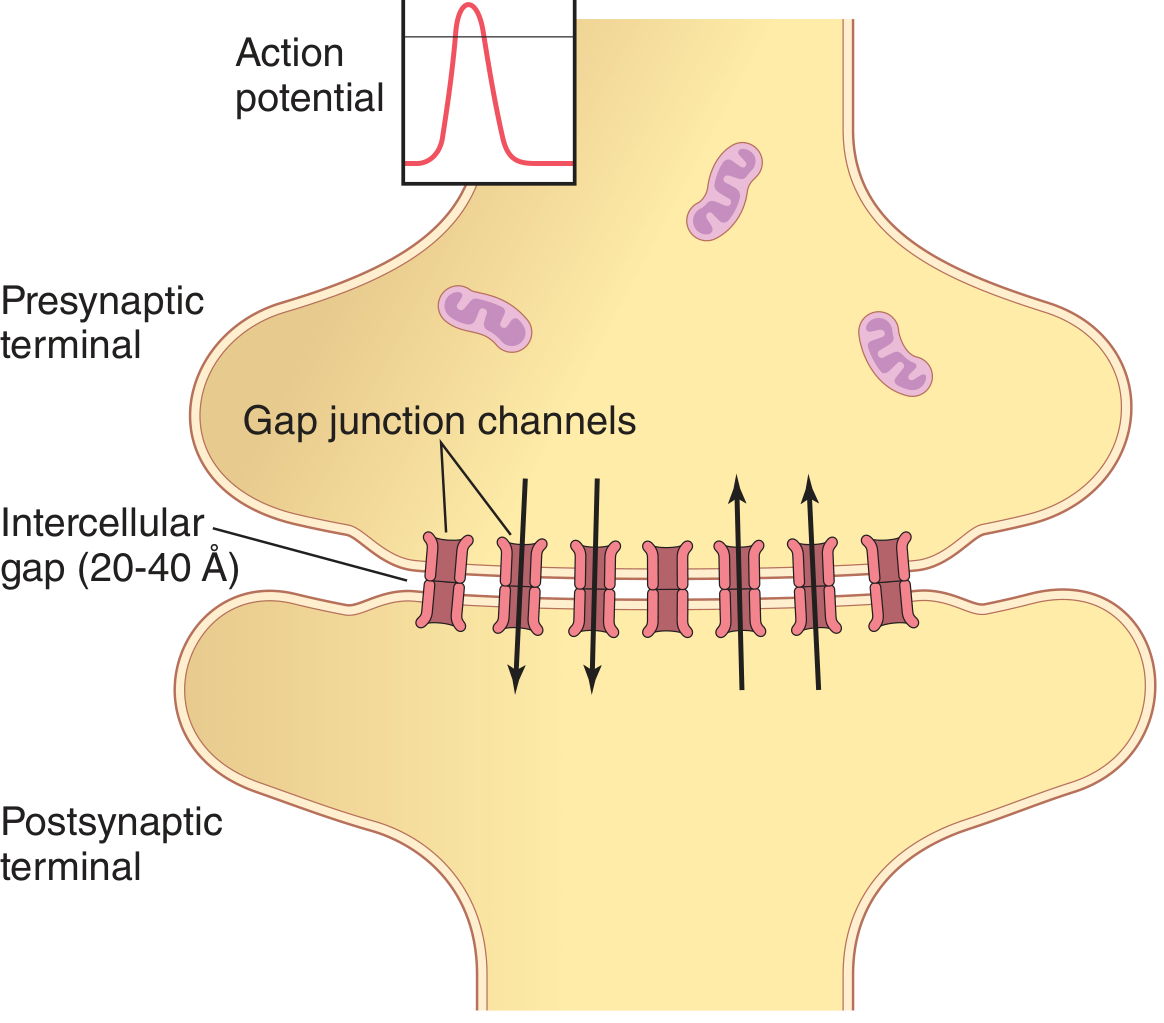
Fig. Electrical synapse: connexin gap junction channels allow bidirectional ionic current flow (Guyton & Hall Medical Physiology)
Electrical synapses use gap junctions (connexin proteins) that physically connect the cytoplasm of two neurons. The intercellular gap is only 20–40 Å.
| Feature | Chemical | Electrical |
|---|
| Direction | One-way | Bidirectional |
| Delay | ~0.5 ms | Near-instantaneous |
| Mechanism | Neurotransmitter | Gap junction current |
| Modifiability | High (plasticity) | Low |
| Location | Widespread in CNS | Hypothalamic hormone neurons, retina, cardiac muscle |
Functional role of electrical synapses: coordinate synchronous firing of large neuronal groups, detect coincident subthreshold depolarizations, enable simultaneous hormone secretion in hypothalamic neurons.
C. Neurotransmitters
Major neurotransmitter classes:
| Class | Examples | Actions |
|---|
| Amino acids | Glutamate (excitatory), GABA, Glycine (inhibitory) | Primary fast signaling |
| Monoamines | Dopamine, Norepinephrine, Serotonin | Modulation, mood, reward |
| Acetylcholine | ACh | NMJ, autonomic, cortical arousal |
| Neuropeptides | Substance P, Enkephalins, NPY | Pain, satiety, slow modulation |
| Purines | ATP, Adenosine | Neuromodulation |
| Gases | NO, CO | Retrograde signaling |
G-protein second messenger pathway (metabotropic): neurotransmitter binds receptor → G-protein α subunit activates → (1) ion channel opening, (2) adenylyl cyclase → cAMP, (3) intracellular enzyme activation, (4) gene transcription. The G protein is inactivated when GTP bound to α is hydrolyzed to GDP.
Neurotransmitter transporters belong to the SLC6 gene family:
- SERT (serotonin transporter) — substrate: serotonin; false substrate: MDMA (Ecstasy)
- NET (norepinephrine transporter) — false substrate: amphetamine, dopamine
- DAT (dopamine transporter) — target of cocaine
(Stahl's Essential Psychopharmacology)
Part 2 — Central Nervous System
A. Brain Regions
1. Cerebrum
The cerebral hemispheres consist of:
- Cerebral cortex — four lobes: frontal, parietal, temporal, occipital; separated by sulci
- White matter (subcortical)
- Deep nuclei: basal ganglia, hippocampus, amygdala
Cortical functional areas:
- Primary motor cortex — upper motor neurons projecting to spinal cord
- Primary somatosensory cortex — receives peripheral sensory input
- Primary visual cortex (occipital), Primary auditory cortex (temporal)
- Association areas — integrate diverse information; the limbic association area handles motivation, memory, and emotion
Basal ganglia (caudate, putamen, globus pallidus): receive input from all cortical lobes; project via thalamus to frontal cortex to assist movement regulation.
Hippocampus: memory consolidation (part of limbic system).
Amygdala: emotion processing; communicates with autonomic nervous system via the hypothalamus.
Thalamus: relay station — processes nearly all sensory information going to the cortex and all motor information from cortex to brainstem/spinal cord.
Hypothalamus: regulates body temperature, food intake, water balance; endocrine control of pituitary (releases releasing/inhibiting hormones into hypophysial portal blood); contains posterior pituitary neurons secreting ADH and oxytocin.
(Costanzo Physiology, 7th Ed.)
2. Cerebellum
"The cerebellum helps control the rate, range, force, and direction of movements (collectively known as synergy). Damage to the cerebellum results in lack of coordination."
The cerebellum lies in the posterior fossa, attached to the brainstem by three cerebellar peduncles (afferent + efferent fibers).
Three main divisions:
| Division | Primary Input | Function |
|---|
| Vestibulocerebellum | Vestibular organs | Balance, eye movements |
| Spinocerebellum | Spinal cord | Synergy (coordination) of movement |
| Pontocerebellum | Cerebral cortex (via pons) | Planning and initiation of movements |
Cerebellar cortex layers (from inside out):
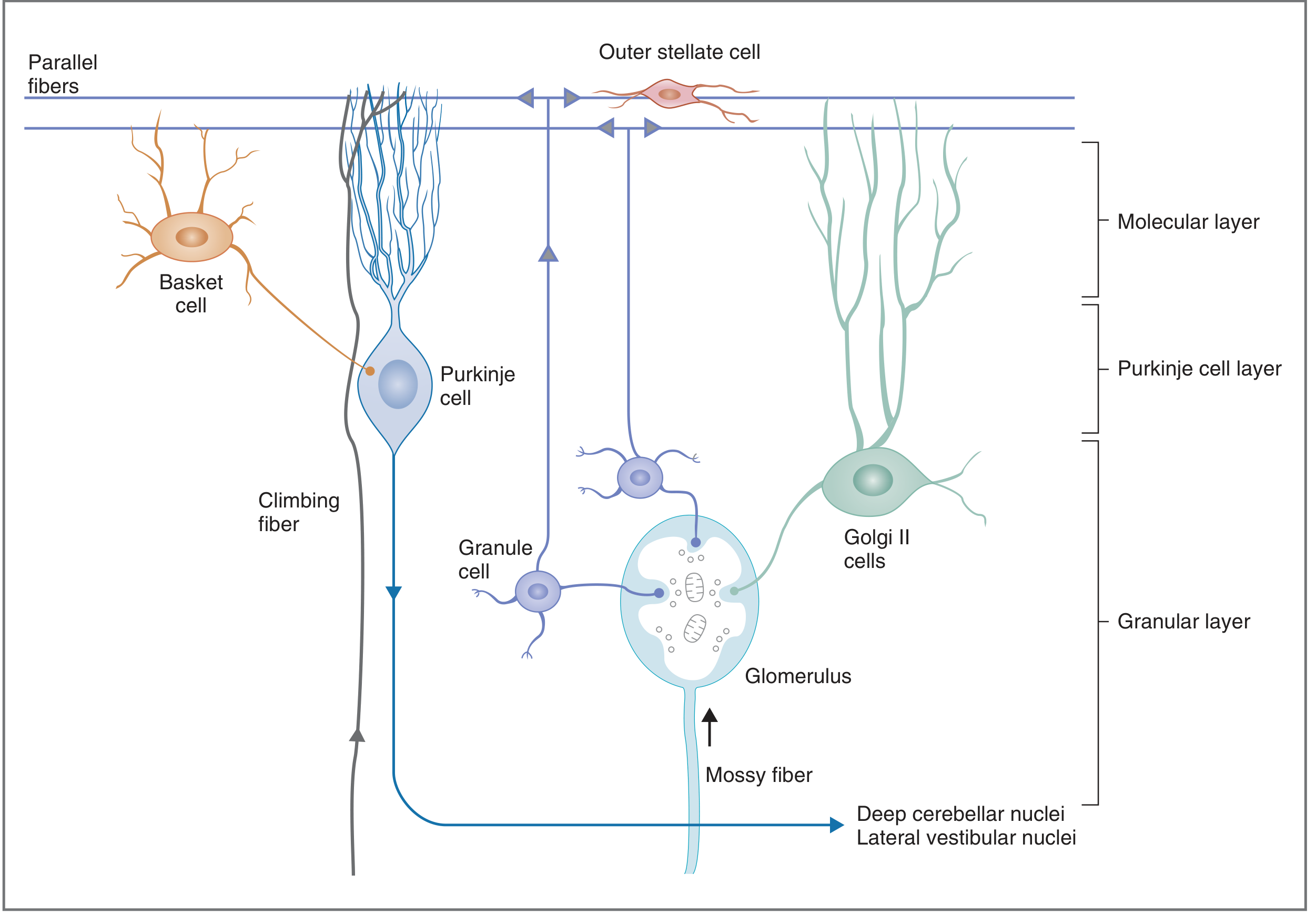
Fig. Cerebellar cortex structure — granular layer (granule cells, Golgi II), Purkinje cell layer (inhibitory output), molecular layer (parallel fibers, basket/stellate cells). Mossy fibers and climbing fibers provide the two excitatory inputs (Costanzo Physiology, 7th Ed.)
- Granular layer (innermost): granule cells + Golgi II cells; mossy fiber input
- Purkinje cell layer (middle): output always inhibitory (GABAergic)
- Molecular layer (outermost): parallel fibers (axons of granule cells), basket cells, stellate cells
Two input systems:
- Climbing fibers (from inferior olive) → directly on Purkinje cells; generate complex spikes; role in motor learning
- Mossy fibers (majority of input) → via granule cells → parallel fibers → Purkinje cells
3. Brainstem
The brainstem consists of the midbrain, pons, and medulla oblongata. Key functions:
- Houses nuclei for cranial nerves III–XII
- Contains reticular formation (arousal, consciousness, cardiorespiratory control)
- Mediates relay of information between cerebral cortex and spinal cord
- Controls vital functions: respiration, heart rate, blood pressure, swallowing, vomiting
Midbrain: superior and inferior colliculi (visual and auditory reflexes); red nucleus, substantia nigra (motor control).
Pons: pontine nuclei relay cortical signals to cerebellum; pneumotaxic center for breathing; cranial nerve nuclei V, VI, VII, VIII.
Medulla oblongata: cardiovascular and respiratory centers; inferior olive (input to cerebellum); cranial nerve nuclei IX, X, XI, XII; pyramidal (corticospinal) decussation.
B. Spinal Cord Anatomy and Functions
The spinal cord extends from the foramen magnum to approximately L1–L2, where it terminates as the conus medullaris. It has 31 segments: 8 cervical (C1–C8), 12 thoracic (T1–T12), 5 lumbar (L1–L5), 5 sacral (S1–S5), 1 coccygeal.
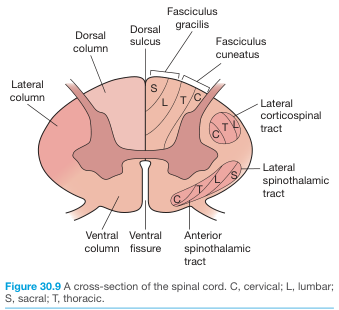
Fig. Spinal cord cross-section showing major ascending (sensory) and descending (motor) tracts and somatotopic organization (Bailey & Love's Surgery, 28th Ed.)
Internal organization:
- Gray matter (butterfly-shaped): neuron cell bodies
- Dorsal horn: sensory processing (laminae I–VI)
- Ventral horn: lower motor neurons (laminae VII–IX)
- Intermediate zone (lamina VII): interneurons; T1–L2 = sympathetic preganglionic neurons; S2–S4 = parasympathetic preganglionic neurons
- White matter: myelinated axon tracts
Major ascending (sensory) tracts:
| Tract | Information | Route |
|---|
| Dorsal columns (fasciculus gracilis + cuneatus) | Fine touch, vibration, proprioception | Ipsilateral → decussates at medulla |
| Lateral spinothalamic | Pain, temperature | Decussates at cord level |
| Anterior spinothalamic | Crude touch, pressure | Decussates at cord level |
| Dorsal spinocerebellar | Proprioception to cerebellum | Ipsilateral |
Major descending (motor) tracts:
| Tract | Origin | Function |
|---|
| Lateral corticospinal | Primary motor cortex (decussates at medulla) | Voluntary limb movement |
| Anterior corticospinal | Motor cortex | Axial muscles |
| Rubrospinal | Red nucleus (midbrain) | Limb flexors |
| Reticulospinal | Reticular formation | Posture, gait, autonomic |
Part 3 — Peripheral Nervous System (PNS)
A. Somatic Nervous System
Carries voluntary motor commands to skeletal muscle (via lower motor neurons from the ventral horn) and sensory information from the periphery (skin, muscle, joints) back to the CNS.
Somatic sensory receptors:
- Meissner's corpuscles (light touch), Pacinian corpuscles (vibration/pressure), Merkel discs (sustained touch), Ruffini endings (stretch), free nerve endings (pain/temperature)
Somatic reflex arc: sensory receptor → afferent neuron → spinal cord interneuron → efferent neuron → effector (muscle)
B. Autonomic Nervous System (ANS)
The ANS controls involuntary functions: cardiac muscle, smooth muscle, glands. It always has a two-neuron chain: preganglionic → ganglionic synapse → postganglionic → effector.
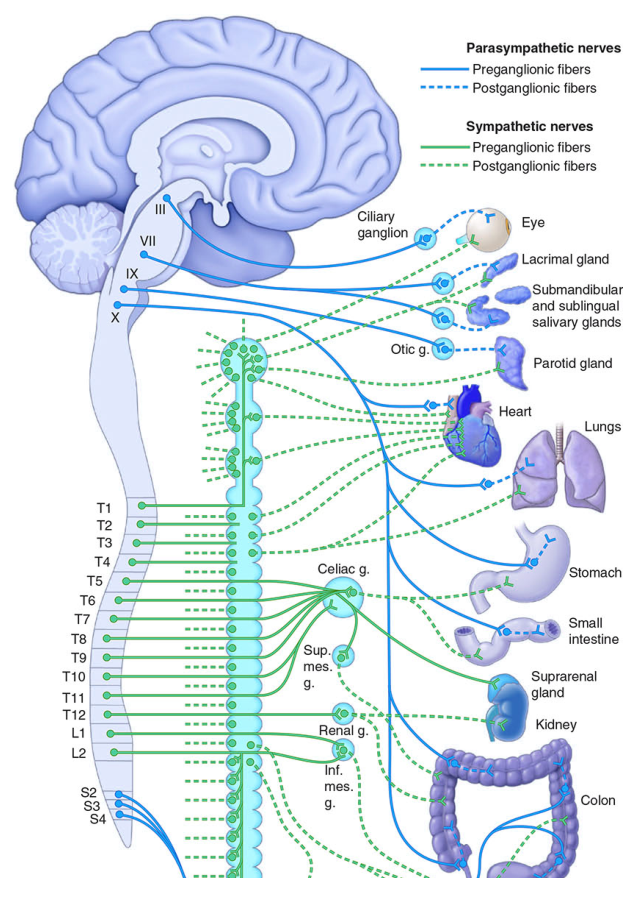
Fig. Autonomic nervous system — parasympathetic (orange) from cranial nerves III/VII/IX/X + sacral S2–S4; sympathetic (green) from T1–L2 thoracolumbar cord (Harrison's Principles of Internal Medicine, 21st Ed.)
| Feature | Sympathetic | Parasympathetic |
|---|
| Origin | Thoracolumbar (T1–L2) | Craniosacral (CN III, VII, IX, X + S2–S4) |
| Ganglia location | Paravertebral chain (near cord) | Near/in target organ |
| Preganglionic NT | ACh (nicotinic) | ACh (nicotinic) |
| Postganglionic NT | Norepinephrine (adrenergic) | ACh (muscarinic) |
| General effect | "Fight or flight" | "Rest and digest" |
| Heart | ↑ HR, ↑ contractility | ↓ HR |
| Pupil | Dilates (mydriasis) | Constricts (miosis) |
| Bronchi | Dilates | Constricts |
| GI | ↓ motility | ↑ motility |
| Sweat glands | ACh (exception!) | — |
Enteric nervous system: third division of ANS; intrinsic to the GI tract; can function independently of CNS.
C. Cranial Nerves (I–XII)
| # | Name | Type | Key Function |
|---|
| I | Olfactory | Sensory | Smell |
| II | Optic | Sensory | Vision |
| III | Oculomotor | Motor + Parasympathetic | Eye movement (SR, IR, MR, IO), pupil constriction, lens accommodation |
| IV | Trochlear | Motor | Superior oblique (eye depresses when adducted) |
| V | Trigeminal | Mixed | Facial sensation (ophthalmic/maxillary/mandibular); muscles of mastication |
| VI | Abducens | Motor | Lateral rectus (eye abduction) |
| VII | Facial | Mixed + Parasympathetic | Muscles of facial expression, taste (anterior 2/3 tongue), lacrimal/salivary glands |
| VIII | Vestibulocochlear | Sensory | Hearing (cochlear) + balance (vestibular) |
| IX | Glossopharyngeal | Mixed + Parasympathetic | Taste (posterior 1/3 tongue), pharyngeal sensation, parotid gland, carotid body |
| X | Vagus | Mixed + Parasympathetic | Visceral sensory/motor, pharynx, larynx, cardiorespiratory, GI |
| XI | Accessory | Motor | Sternocleidomastoid + trapezius |
| XII | Hypoglossal | Motor | Tongue movements |
Spinal nerves: 31 pairs (8C, 12T, 5L, 5S, 1Co), each with a dorsal root (sensory, dorsal root ganglion cell bodies) and ventral root (motor). Merge to form mixed spinal nerve → anterior and posterior rami → peripheral nerve plexuses (cervical, brachial, lumbar, sacral).
Part 4 — Special Senses
A. Vision — Eye Anatomy & Photoreceptors
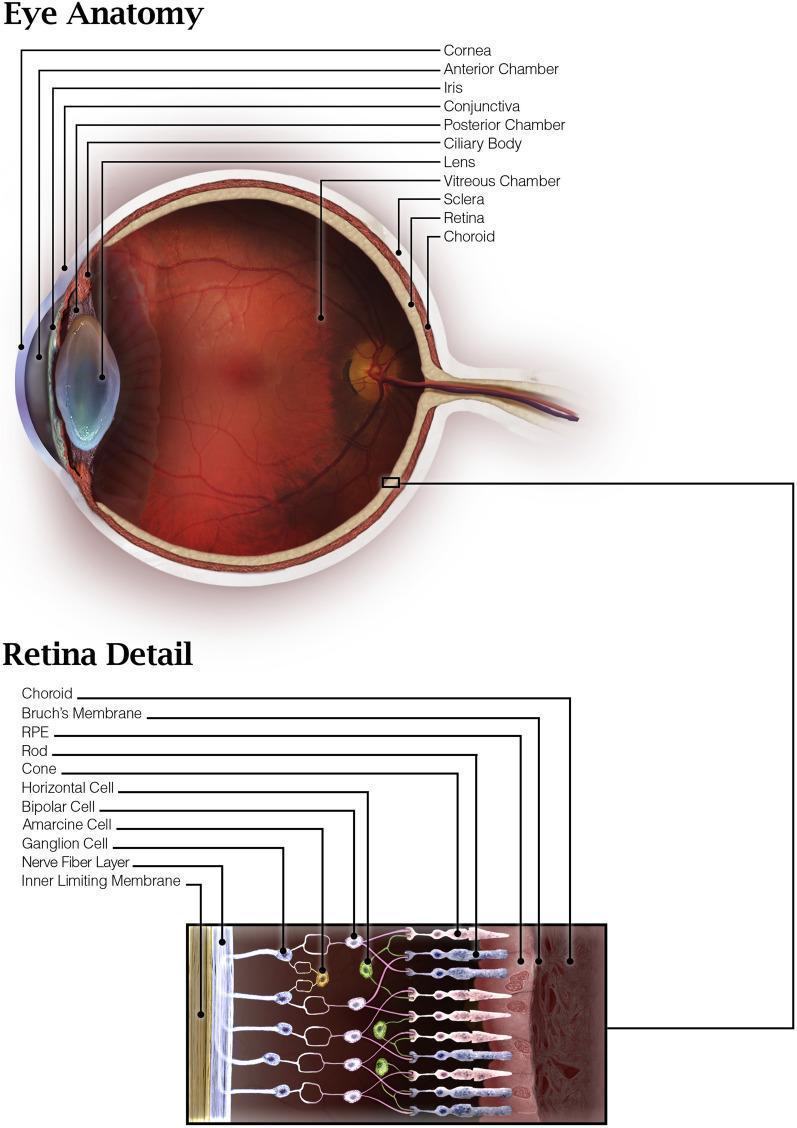
Fig. Eye anatomy with retina detail — full cellular lamination from RPE and photoreceptors through ganglion cells to nerve fiber layer
Eye anatomy layers (outer → inner):
- Sclera: tough outer coat; merges anteriorly with transparent cornea (primary refractive structure)
- Uvea: choroid (vascular, nourishes retina) + ciliary body (ciliary muscle adjusts lens curvature for accommodation) + iris (controls pupil diameter)
- Lens: transparent, biconvex; changes shape for accommodation; suspended by ciliary zonule fibers
- Vitreous humor: posterior chamber; maintains globe shape
- Retina: innermost layer; contains photoreceptors
Retinal cell layers (light enters from ganglion cell side):
- Retinal pigment epithelium (RPE)
- Photoreceptors — rods and cones
- Outer plexiform layer (receptor → bipolar synapse)
- Bipolar cells, horizontal cells, amacrine cells
- Inner plexiform layer
- Ganglion cells — axons form the optic nerve (CN II)
- Nerve fiber layer
Photoreceptors:
| Rods | Cones |
|---|
| Number | ~120 million | ~6 million |
| Location | Peripheral retina | Concentrated at fovea (highest acuity) |
| Light sensitivity | Scotopic (dim light) | Photopic (bright light, color) |
| Pigment | Rhodopsin (opsin + retinal) | Three types: L (red), M (green), S (blue) |
| Acuity | Low | High |
| Color | No | Yes (trichromatic) |
Phototransduction (rods): Light → retinal isomerizes (11-cis → all-trans) → rhodopsin activation → transducin (G-protein) → phosphodiesterase activation → cGMP hydrolysis → Na⁺ channels close → hyperpolarization of photoreceptor → reduced glutamate release → signal propagation to bipolar → ganglion cells → optic nerve → lateral geniculate nucleus (thalamus) → primary visual cortex (V1, occipital lobe).
Visual pathway: optic nerves → optic chiasm (nasal fibers decussate) → optic tracts → lateral geniculate nucleus → optic radiation → visual cortex.
B. Hearing — Ear Anatomy & Sound Transduction
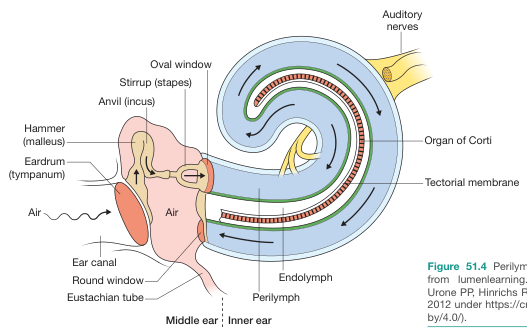
Fig. Ear anatomy showing sound pathway: air → ear canal → eardrum → malleus/incus/stapes → oval window → cochlear fluid waves → organ of Corti → auditory nerve (Bailey & Love's Surgery, 28th Ed.)
Outer ear: auricle + ear canal → funnels sound to tympanic membrane (eardrum).
Middle ear: three ossicles amplify vibrations (~22× mechanical advantage):
- Malleus (hammer) → Incus (anvil) → Stapes (stirrup) → oval window
- Eustachian tube equalizes pressure with nasopharynx
Inner ear (cochlea):
- Bony spiral structure; tonotopic organization (base = high frequency, apex = low frequency)
- Three fluid compartments:
- Scala vestibuli (perilymph, high Na⁺) — above
- Scala media / cochlear duct (endolymph, high K⁺) — middle
- Scala tympani (perilymph) — below
- Organ of Corti sits on the basilar membrane inside the scala media
- Inner hair cells (IHCs, 1 row): primary sensory cells; relay signals to auditory nerve
- Outer hair cells (OHCs, 3 rows): amplify and tune basilar membrane movement (cochlear amplifier)
- Tectorial membrane sits above stereocilia
Sound transduction (mechanotransduction):
- Stapes vibrates oval window → pressure waves in perilymph
- Basilar membrane deflects at position corresponding to sound frequency
- Stereocilia of hair cells bend against tectorial membrane → tip links open MET (mechanotransduction) channels
- K⁺ (and Ca²⁺) influx from endolymph → hair cell depolarization
- Neurotransmitter (glutamate) released at IHC base → activates spiral ganglion neurons (CN VIII)
- Signals travel: cochlear nucleus → superior olivary complex → inferior colliculus (midbrain) → medial geniculate nucleus (thalamus) → primary auditory cortex (temporal lobe, Heschl's gyrus)
C. Taste (Gustation) — Receptors & Pathways
Taste receptor cells (TRCs) are clustered in taste buds on papillae of the tongue:
- Fungiform papillae — anterior 2/3 tongue
- Circumvallate (vallate) papillae — posterior tongue
- Foliate papillae — lateral tongue
Five primary taste modalities:
| Taste | Mechanism | Key Stimulus |
|---|
| Sweet | GPCR (T1R2+T1R3) → G-protein (gustducin) → cAMP/IP₃ | Sugars |
| Umami | GPCR (T1R1+T1R3) | Glutamate (MSG) |
| Bitter | GPCR (T2R family) | Alkaloids, toxins |
| Sour | H⁺ blocks K⁺ channels / OTOP1 channel | Acids |
| Salty | ENaC Na⁺ channels (epithelial sodium channels) | NaCl |
Taste pathway: TRCs → cranial nerves VII (anterior 2/3 tongue), IX (posterior 1/3), X (epiglottis/pharynx) → nucleus tractus solitarius (NTS) in medulla → thalamus (VPM nucleus) → primary gustatory cortex (insular cortex + frontal operculum).
D. Smell (Olfaction) — Receptors & Pathways
Olfactory receptor neurons (ORNs) are located in the olfactory epithelium (roof of nasal cavity, superior turbinate). Humans have ~400 functional olfactory receptor genes (OR genes — largest gene family in mammals).
Mechanism:
- Odorant molecules dissolve in mucus → bind olfactory receptors (GPCRs) on cilia of ORNs
- OR → Golf (Gαs type) → adenylyl cyclase → ↑ cAMP → opens CNG channels (cyclic nucleotide-gated) → Na⁺/Ca²⁺ influx → depolarization
- Ca²⁺ opens Ca²⁺-activated Cl⁻ channels → amplification
Olfactory pathway (only sense that bypasses the thalamus directly):
- ORN axons → pass through cribriform plate → olfactory bulb (CN I)
- Mitral/tufted cells → olfactory tract → piriform cortex + amygdala (primary olfactory cortex, conscious perception and emotional/memory integration)
- Piriform cortex → entorhinal cortex → orbitofrontal cortex (secondary cortex, odor identification/discrimination)
- Also → hypothalamus (autonomic + feeding responses)
Key difference from other senses: olfactory signals reach the cortex and limbic system without a mandatory thalamic relay, explaining the powerful link between smell and memory/emotion.
Summary Table — CNS Regions at a Glance
| Structure | Key Functions | Damage Effects |
|---|
| Frontal lobe | Motor, executive function, Broca's area | Contralateral weakness, personality change, aphasia |
| Parietal lobe | Somatosensory, spatial orientation | Contralateral sensory loss, neglect |
| Temporal lobe | Auditory, memory, Wernicke's area | Hearing deficits, amnesia, receptive aphasia |
| Occipital lobe | Visual processing | Visual field defects |
| Cerebellum | Coordination, balance, motor learning | Ataxia, dysmetria, intention tremor |
| Brainstem | Vital functions, CN nuclei, relay | Cranial nerve palsies, respiratory/cardiovascular failure |
| Spinal cord | Sensorimotor relay, reflexes, ANS | Paralysis, sensory loss, autonomic dysfunction |
Sources: Neuroscience: Exploring the Brain (5th Ed.) · Guyton and Hall Textbook of Medical Physiology · Costanzo Physiology (7th Ed.) · Stahl's Essential Psychopharmacology · Harrison's Principles of Internal Medicine (21st Ed.) · Bailey & Love's Surgery (28th Ed.)