Cough 1 year Chest heaviness 1 year Shortness of breath 1 year Fever 8 months Cough with sputum white 7 days Loss of appetite 7 days
Checking Date & Time
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Loading Image
Clinical Assessment
Symptom Timeline Analysis
| Symptom | Duration | Significance |
|---|---|---|
| Cough | 1 year | Chronic — cardinal TB symptom |
| Chest heaviness | 1 year | Consistent with parenchymal involvement / pleural disease |
| Shortness of breath | 1 year | Progressive lung compromise |
| Fever | 8 months | Prolonged constitutional symptom |
| Productive cough (white sputum) | 7 days | Acute exacerbation / secondary infection |
| Loss of appetite | 7 days | Constitutional worsening |
The chronicity (1 year of pulmonary symptoms + 8 months of fever) with recent productive change is the key clinical signal.
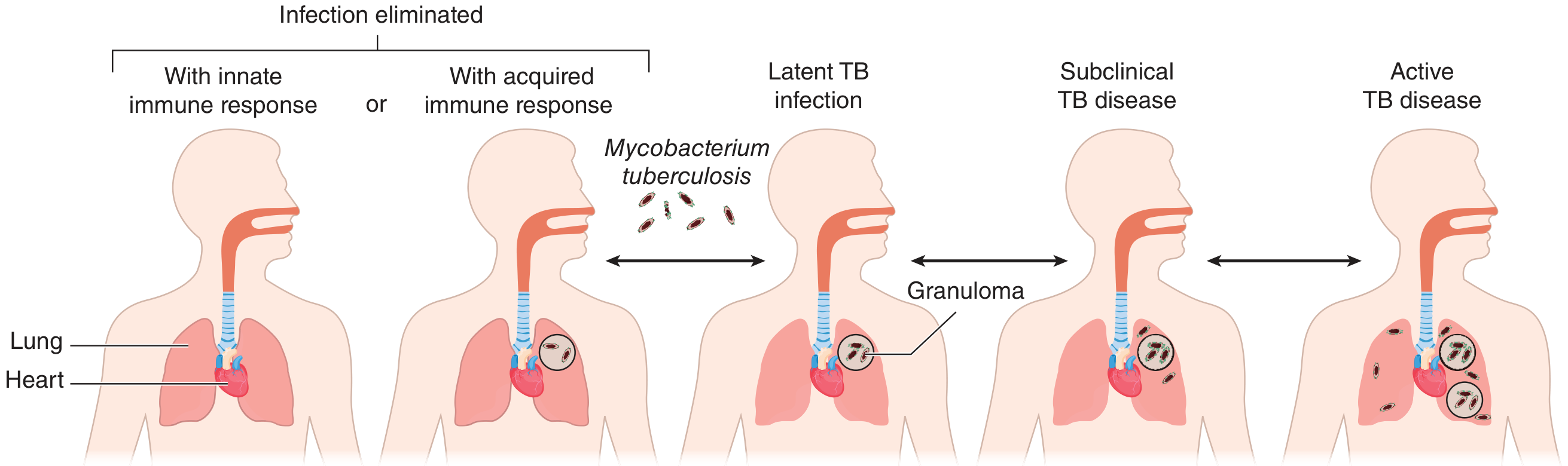
Most Likely Diagnosis: Active Pulmonary Tuberculosis (TB)
This presentation is a textbook picture of reactivation (post-primary) pulmonary TB:
"The most common symptom of pulmonary TB is a persistent cough, which can be productive or nonproductive and accompanied by fever, chills, night sweats, and weight loss; hemoptysis may occur in advanced disease." — Goldman-Cecil Medicine
"The systemic features of TB include fever in approximately 35–80%, malaise, and weight loss" — Murray & Nadel's Textbook of Respiratory Medicine
Why this fits:
- Chronic cough (≥1 year) is the cardinal symptom of pulmonary TB
- Prolonged low-grade fever (8 months) — classic constitutional feature
- Chest heaviness + dyspnea — parenchymal destruction, pleural involvement, or extensive infiltrates
- Productive white sputum (7 days) — active disease with mucoid secretions; purulent change or hemoptysis would suggest further progression
- Anorexia — weight loss is a hallmark constitutional symptom
Differential Diagnosis
| Diagnosis | Supporting Features | Against |
|---|---|---|
| Pulmonary TB ⭐ | Chronic cough, prolonged fever, constitutional symptoms | — |
| Chronic pulmonary histoplasmosis | Mimics TB with upper-lobe cavitation, productive cough, fever, weight loss | Usually in endemic areas; smokers with structural lung disease |
| Lung abscess / chronic pneumonia | Productive cough, fever, chest pain | Typically shorter course; often more acute |
| Lung cancer | Chronic cough, weight loss, chest heaviness | Less fever; usually older smokers |
| Pulmonary actinomycosis | Chronic cough, dyspnea, fever, weight loss | Rare; associated with dental/aspiration history |
| COPD + infection | Cough, dyspnea, sputum | Fever less prominent; no true constitutional syndrome |
| Bronchiectasis | Chronic productive cough | Fever less characteristic; usually copious mucopurulent sputum |
Diagnostic Workup
First-line (Mandatory)
- Chest X-ray — look for upper-lobe infiltrates, cavitation, consolidation, pleural effusion, miliary pattern
- Sputum AFB smear microscopy × 3 — standard in high-incidence settings (two same-day specimens is acceptable per WHO)
- Sputum mycobacterial culture — gold standard; takes 2–6 weeks
- Xpert MTB/RIF (GeneXpert) — WHO-recommended initial test; detects M. tuberculosis AND rifampicin resistance in 90 minutes; preferred over smear alone
Per Murray & Nadel:
"All adults suspected of having active pulmonary TB should have at least two sputum specimens collected for AFB smear microscopy and mycobacterial culture and at least one sputum specimen for nucleic acid amplification testing (NAAT)."
Second-line
- TST (Mantoux) / IGRA — supports latent vs. active distinction; a positive test alone does not confirm active disease
- Full blood count — leukocytosis, anemia, elevated ESR/CRP
- HIV test — mandatory (HIV co-infection alters presentation and management)
- CT chest — more sensitive than CXR, especially for cavity detection, miliary pattern, lymphadenopathy
- Bronchoscopy + BAL — if sputum not obtainable or smear negative with high suspicion
- Blood cultures — if miliary TB suspected (especially in HIV+)
Management (if TB confirmed)
Standard DOTS Regimen (WHO/CDC)
Intensive phase (2 months):
| Drug | Abbreviation |
|---|---|
| Isoniazid (H) | INH |
| Rifampicin (R) | RIF |
| Pyrazinamide (Z) | PZA |
| Ethambutol (E) | EMB |
Continuation phase (4 months):
- Isoniazid + Rifampicin (2HRZE / 4HR)
Note: Ethambutol is bacteriostatic; the other three are bactericidal. Drug susceptibility testing is essential before finalizing the regimen.
Supportive measures
- Nutritional support (high-protein diet)
- Respiratory isolation until smear-negative (at least 2 weeks of effective treatment)
- Contact tracing and notification (TB is a notifiable disease)
- Monitor liver function (hepatotoxicity from INH, RIF, PZA)
- Pyridoxine (Vitamin B6) with INH to prevent peripheral neuropathy
If drug-resistant TB suspected
- Xpert MTB/RIF detects rifampicin resistance → triggers DST panel
- MDR-TB (resistant to INH + RIF) requires specialist referral and second-line agents (fluoroquinolones, bedaquiline, linezolid)
Red Flags Requiring Urgent Attention
- Hemoptysis → cavitary disease, Rasmussen aneurysm, aspergilloma in old cavity
- Worsening dyspnea → extensive disease, pleural effusion, pneumothorax
- Altered mental status / meningism → TB meningitis
- HIV seropositivity → changes threshold for smear negativity; CT scan becomes essential; immune reconstitution inflammatory syndrome (IRIS) risk if ART started
Summary
This patient has a high pre-test probability for active pulmonary tuberculosis based on 1 year of constitutional and respiratory symptoms with prolonged fever. The recent productive cough may represent disease progression. Initiate sputum AFB/Xpert testing and chest imaging immediately. Do not delay empirical workup — early diagnosis is critical both for patient outcomes and public health transmission control.
"Early and accurate diagnosis is critically important to TB care and control... Diagnostic delays result in ongoing transmission in the community and more severe, progressive disease." — Murray & Nadel's Textbook of Respiratory Medicine
Sources: Goldman-Cecil Medicine (International Ed.); Murray & Nadel's Textbook of Respiratory Medicine; Harrison's Principles of Internal Medicine 22E (2025)
This is a shared conversation. Sign in to Orris to start your own chat.