Basic mode and newer mode of ventilation
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Loading Image
Loading Image
Here is a comprehensive overview of basic and newer modes of mechanical ventilation, drawn from multiple authoritative surgical and pulmonary textbooks.
Modes of Mechanical Ventilation
The mode defines the relationship between mandatory, assisted, supported, and spontaneous breath types, plus how inspiratory phase variables are controlled. Every ventilator mode sets four core parameters: (1) breath size (tidal volume or inspiratory pressure), (2) rate, (3) PEEP, and (4) FiO₂. — Sabiston Textbook of Surgery
Basic / Standard Modes
1. Controlled Mechanical Ventilation (CMV)
The ventilator delivers all breaths at a preset rate; the patient cannot trigger the machine. Used in heavily sedated or paralyzed patients. Two subtypes:
- Volume-Controlled Ventilation (VCV): preset tidal volume, airway pressure is variable — used when CO₂ clearance and minute ventilation must be tightly controlled.
- Pressure-Controlled Ventilation (PCV): preset inspiratory pressure, tidal volume is variable — preferred when compliance is very poor and barotrauma risk is high.
In CMV, prolonged use promotes diaphragmatic atrophy and contractility dysfunction.
2. Assist-Control Ventilation (AC)
The most commonly used mode. The ventilator delivers a full breath either when triggered by the patient's effort or, if no effort occurs within a set interval, independently by the machine. Every breath — patient-initiated or machine-initiated — delivers a full preset breath (volume or pressure target).
- AC-VC (Volume Control): tidal volume set at 6–8 mL/kg predicted body weight; plateau pressure must be kept < 30 cm H₂O.
- AC-PC (Pressure Control): inspiratory pressure set; minute ventilation must be closely monitored because changes in compliance alter tidal volume.
AC is associated with low work of breathing since every breath is fully supported. — Current Surgical Therapy 14e; Sabiston Textbook of Surgery
3. Synchronized Intermittent Mandatory Ventilation (SIMV)
A hybrid of AC and pressure support. The ventilator delivers mandatory breaths at a set rate, synchronized with the patient's effort. Spontaneous breaths above the mandatory rate are supported only by the set pressure support level (not full machine breath).
- If sedation is deep or rate set high → functionally equivalent to VC
- If rate set low → functionally equivalent to PSV with occasional "sigh" breaths
- Useful for gradual weaning by reducing mandatory rate over time
Key distinction from AC: in AC, every patient-triggered breath gets full support; in SIMV, spontaneous breaths above the set rate get only partial pressure support. — Sabiston; Current Surgical Therapy 14e
4. Pressure Support Ventilation (PSV)
A purely spontaneous mode — no mandatory breaths. Every breath is patient-triggered and augmented by a preset inspiratory pressure; flow-cycled (breath ends when flow drops to ~25% of peak). Analogous to BiPAP.
- Requires the patient to have a reliable respiratory drive (apnea alarms mandatory)
- Reduces work of breathing
- Primary use: ventilator weaning and liberation
- Can be used stand-alone or embedded within SIMV
5. Continuous Positive Airway Pressure (CPAP)
Spontaneous mode with no mandatory rate. A constant positive pressure maintained throughout the respiratory cycle. The patient controls all breaths; no inspiratory pressure support is added. Used primarily for weaning trials and in non-invasive settings.
Breath Types Within Modes
| Breath Type | Variable Set | Variable Free | Notes |
|---|---|---|---|
| Volume Control (VC) | Tidal volume (6–8 mL/kg PBW) | Airway pressure | Monitor plateau pressure < 30 cmH₂O |
| Pressure Control (PC) | Inspiratory pressure | Tidal volume | Monitor minute ventilation closely |
| Pressure-Regulated Volume Control (PRVC) | Volume target + pressure limit | Dynamic pressure | Software adjusts pressure breath-to-breath to hit volume target |
| Pressure Support (PSV) | Inspiratory pressure | Volume + rate | Flow-cycled; spontaneous only |
PRVC is a newer "dual-control" mode: ventilator software monitors lung compliance each cycle and adjusts inspiratory pressure for the next breath to hit a target tidal volume. When compliance improves, pressure is automatically reduced. — Current Surgical Therapy 14e
The Pressure-Volume Curve and Safe Window
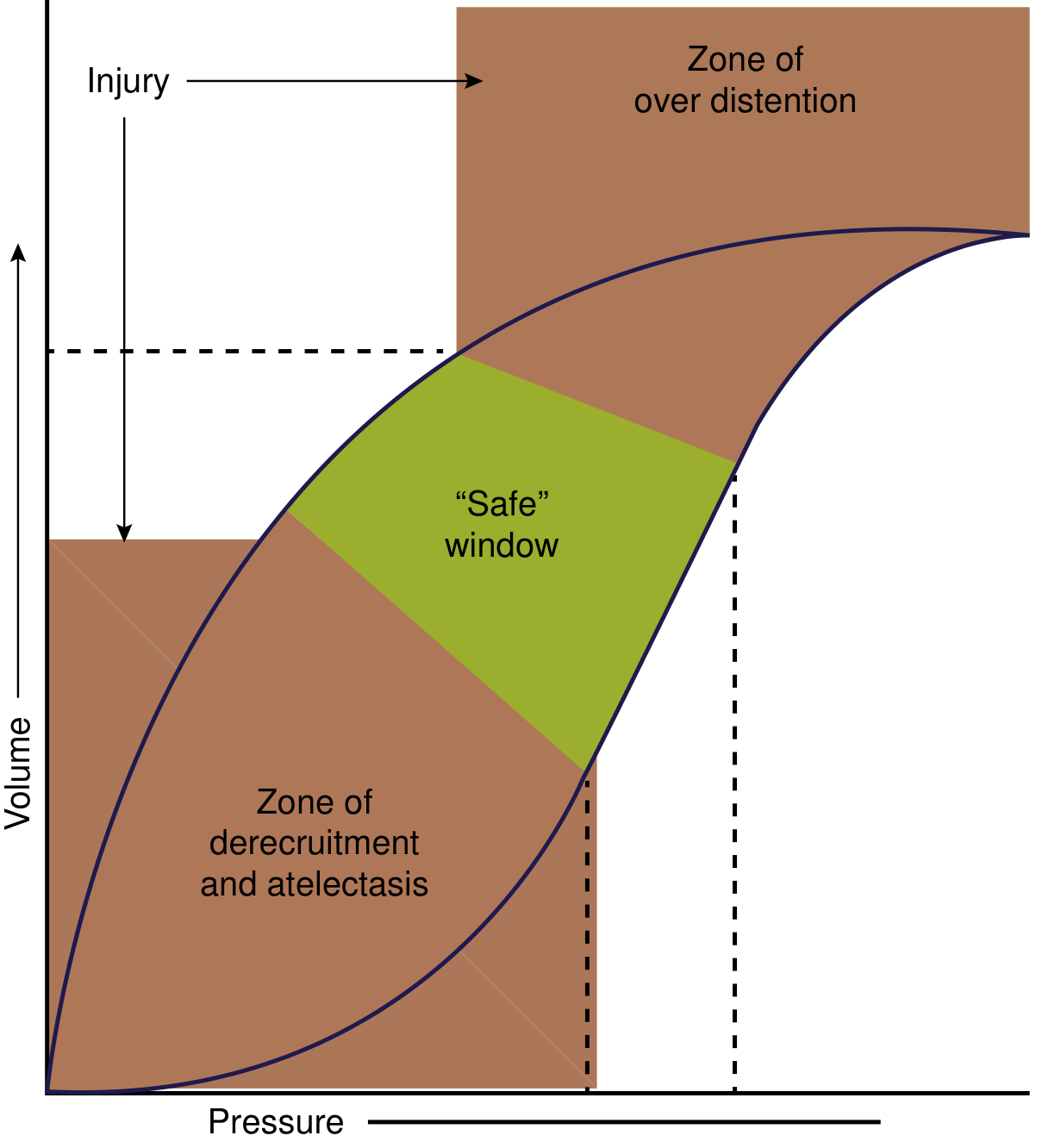
Pressure-volume curve of a diseased lung (e.g., ARDS). Ventilation must stay within the "safe" window: above the lower inflection point (to avoid derecruitment/atelectasis) and below the upper inflection point (to avoid overdistension/barotrauma). — Current Surgical Therapy 14e
Newer / Advanced Modes
6. Airway Pressure Release Ventilation (APRV)
APRV applies two levels of CPAP — a high pressure (P-high) held for a long time (T-high) and a brief "release" to a low pressure (P-low) for a very short time (T-low). Spontaneous breathing is permitted (and encouraged) at both pressure levels.
| Parameter | Typical Setting |
|---|---|
| P-high | 25–30 cm H₂O |
| P-low | 0 cm H₂O |
| T-high | Long (I:E ratio often 7:1 to 10:1) |
| T-low | Very short (~0.4–0.8 s) |
- Tidal volume generated = difference between P-high and P-low
- Achieves high mean airway pressure → improved alveolar recruitment
- Hemodynamically well tolerated with minimal sedation
- Used in severe hypoxemia and ARDS
- A recent meta-analysis (nearly 19 years of data) suggested a mortality benefit in acute hypoxemic respiratory failure vs. conventional modes
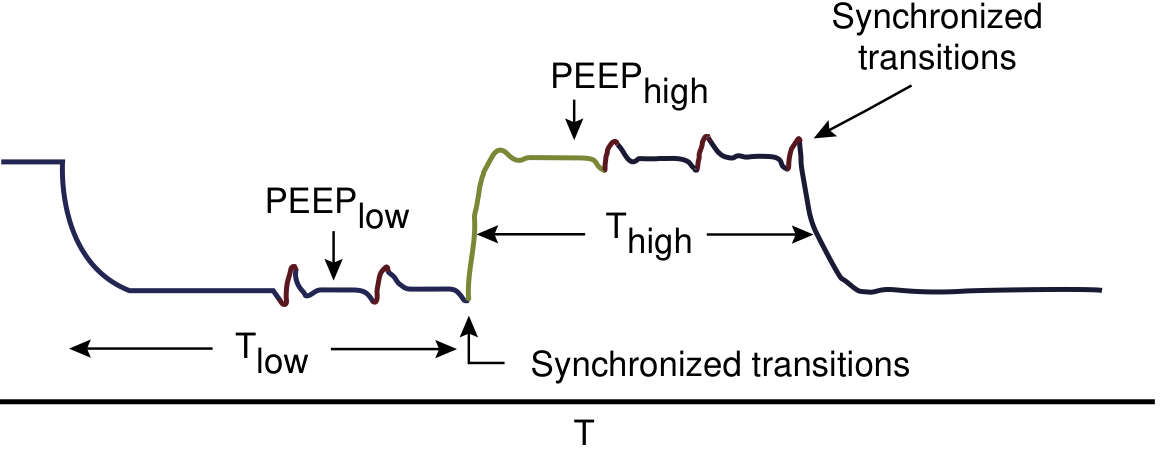
Bilevel/APRV waveform: The ventilator cycles between a high CPAP level (T-high) and a low release pressure (T-low), with spontaneous breaths superimposed at both levels. — Current Surgical Therapy 14e
7. Bilevel Positive Airway Pressure Ventilation (BiLevel / DUOPAP)
Similar to APRV in concept — two PEEP levels with spontaneous breathing allowed at both — but uses a longer T-low (more time at low pressure), resulting in a less extreme I:E ratio than classic APRV. The distinction between APRV and bilevel is mainly in the T-low setting. — Sabiston
8. High-Frequency Oscillatory Ventilation (HFOV)
Delivers extremely small tidal volumes (less than anatomical dead space) at very high frequencies (3–15 Hz / 180–900 breaths/min). Gas exchange occurs via mechanisms beyond bulk flow (asymmetric velocity profiles, molecular diffusion).
- Used as a salvage mode or bridge to ECMO in severe ARDS
- Physiologically appealing for lung protection in ARDS
- Clinical trials (e.g., OSCILLATE, OSCAR) have not shown survival benefit in adults; may even increase mortality in some subgroups
- May have benefit in pediatric ARDS
9. Proportional Assist Ventilation (PAV) / Proportional Pressure Support (PPS)
A newer mode where the ventilator generates pressure in proportion to the patient's own inspiratory effort (both flow and volume). The clinician sets a "gain" rather than a fixed pressure. This maintains patient-ventilator synchrony dynamically and reduces asynchrony. — Fishman's Pulmonary Diseases
Key Concepts: Ventilator-Induced Lung Injury (VILI)
All modes must be set to avoid VILI, caused by:
- Barotrauma — excess airway pressure
- Volutrauma — alveolar overdistension from large tidal volumes
- Atelectrauma — cyclic recruitment/derecruitment
- Biotrauma — inflammatory mediator release from injured lung
Universal protective targets regardless of mode:
- Tidal volume: 6–8 mL/kg predicted body weight
- Plateau pressure: < 30 cm H₂O
- Monitor for auto-PEEP (measured via expiratory hold)
Summary Comparison
| Mode | Mandatory Breaths | Spontaneous Breaths | Primary Use |
|---|---|---|---|
| CMV/VC | Full control, preset | None | Paralyzed/apneic patients |
| AC (VC or PC) | Yes (backup rate) | Full support | Most ICU patients |
| SIMV | Yes (set rate) | Partial (PS only) | Weaning |
| PSV | None | Full support | Weaning, cooperative patients |
| PRVC | Yes (dual control) | — | Better lung protection |
| APRV | Pressure release | Superimposed | ARDS, severe hypoxemia |
| HFOV | Oscillation | None | Refractory ARDS, bridge to ECMO |
| PAV | Proportional | Proportional | Reduce asynchrony |
Sources: Sabiston Textbook of Surgery; Current Surgical Therapy 14e; Fishman's Pulmonary Diseases and Disorders
More information on MV
Asking for Preferences
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Comprehensive content gathered. Here is a full deep-dive on mechanical ventilation:
Mechanical Ventilation — Comprehensive Overview
1. Objectives of Mechanical Ventilation
The goals of MV go beyond simply keeping a patient alive:
| Category | Objectives |
|---|---|
| Gas exchange | Reverse hypoxemia; relieve acute respiratory acidosis |
| Work of breathing | Decrease O₂ cost of breathing; reverse respiratory muscle fatigue |
| Pressure-volume | Prevent/reverse atelectasis; improve lung compliance |
| Lung protection | Prevent further lung injury; permit lung and airway healing |
| Systemic | Allow time to treat the underlying disease; avoid complications |
Increased work of breathing is the most common reason for intubation. It can be clinically assessed by palpating phasic sternomastoid contraction, tracheal tug, suprasternal recession, and intercostal recession — not by any single objective measurement threshold. — Fishman's Pulmonary Diseases
2. Indications for Mechanical Ventilation
Clinical indications:
- Acute hypoxemic respiratory failure (PaO₂/FiO₂ < 200 in ARDS)
- Acute hypercapnic respiratory failure (respiratory acidosis with pH < 7.20–7.25)
- Apnea or impending respiratory arrest
- Airway protection (obtunded, GCS < 8, inability to protect airway from secretions/aspiration)
- Excessive work of breathing that is unsustainable
- Refractory status asthmaticus or status epilepticus
Physiologic thresholds commonly cited (no single cutoff is definitive):
| Parameter | Threshold for Concern |
|---|---|
| Respiratory rate | > 35 breaths/min |
| PaO₂ on high-flow O₂ | < 60 mmHg |
| PaCO₂ (rising acutely) | > 50 mmHg with pH < 7.25 |
| Tidal volume (spontaneous) | < 5 mL/kg |
| Vital capacity | < 15 mL/kg |
| NIF (max inspiratory force) | Less negative than −25 cmH₂O |
3. Initial Ventilator Settings
| Parameter | Typical Initial Setting |
|---|---|
| Mode | AC-VC (most common starting mode) |
| Tidal volume (VT) | 6–8 mL/kg predicted body weight (PBW) |
| Respiratory rate | 12–20 breaths/min (adjusted for pH/PaCO₂) |
| FiO₂ | Start at 1.0, wean rapidly to ≤ 0.6 |
| PEEP | 5 cmH₂O initially; titrate up in ARDS |
| I:E ratio | 1:2 (standard); can invert in ARDS |
| Plateau pressure target | < 30 cmH₂O |
Predicted body weight (not actual) drives VT settings because lung size correlates with height, not weight — critical in obese patients.
4. Ventilator-Induced Lung Injury (VILI)
VILI is the primary hazard of mechanical ventilation itself. Four distinct mechanisms:
| Mechanism | Description |
|---|---|
| Barotrauma | Excess airway pressure ruptures alveoli → pneumothorax, pneumomediastinum, subcutaneous emphysema |
| Volutrauma | Alveolar overdistension from excessive tidal volumes → diffuse alveolar damage |
| Atelectrauma | Cyclic recruitment-derecruitment of unstable alveoli → shear stress injury |
| Biotrauma | Local cytokine release from injured lung → systemic inflammatory response |
The ARMA Trial (ARDS Network): Landmark RCT comparing VT 6 mL/kg vs. 12 mL/kg PBW in ARDS. Mortality 31% vs. 40% — a 9-point absolute reduction with low-tidal-volume ventilation. This is the strongest evidence for lung-protective ventilation. — Harrison's, 22nd Ed.
Key monitoring parameters to prevent VILI:
- Plateau pressure (measured by inspiratory hold): target < 30 cmH₂O
- Driving pressure = Plateau pressure − PEEP: target < 15 cmH₂O (emerging evidence)
- Auto-PEEP (measured by expiratory hold): reflects breath stacking/air trapping
5. PEEP — Titration and Rationale
PEEP prevents alveolar collapse at end-expiration (preventing atelectrauma) and improves oxygenation by:
- Increasing mean airway pressure
- Recruiting collapsed alveoli
- Reducing intrapulmonary shunt
Setting PEEP in ARDS (three approaches):
- ARDS Network FiO₂–PEEP table — empirical combinations of FiO₂ and PEEP levels
- Pressure-volume curve — set PEEP just above the lower inflection point
- Esophageal pressure monitoring — estimates transpulmonary pressure to individualize PEEP; however, a recent phase 2 trial showed no benefit over empirical high PEEP-FiO₂ titration
High PEEP must be balanced against hemodynamic compromise: elevated intrathoracic pressure reduces venous return and cardiac output.
6. MV in ARDS — Special Strategies
| Strategy | Evidence |
|---|---|
| Low VT (6 mL/kg PBW), plateau < 30 cmH₂O | ✅ Mortality benefit (ARMA trial) |
| Prone positioning (≥16 h/day) | ✅ Reduces 28-day mortality 32.8% → 16.0% in severe ARDS (PaO₂/FiO₂ < 150) |
| Neuromuscular blockade (cisatracurium 48h) | ⚠️ Earlier trial showed benefit; subsequent trial showed no mortality benefit — selective use in refractory asynchrony |
| Recruitment maneuvers | ❌ No mortality benefit; may increase mortality when combined with high PEEP |
| HFOV | ❌ No survival benefit in adults (OSCILLATE, OSCAR trials); may increase mortality |
| APRV | Possible mortality benefit in meta-analysis; not standard yet |
| ECMO (VV-ECMO) | ✅ Rescue therapy in severe refractory ARDS; initial use not superior to rescue use — Harrison's |
7. MV in Obstructive Disease (COPD / Asthma)
Key problem: Air trapping and auto-PEEP — incomplete exhalation leads to breath stacking and hyperinflation
Strategies:
- Permissive hypercapnia — accept higher PaCO₂ to allow longer expiratory time
- Low respiratory rate (10–14/min) and long expiratory time (I:E ≥ 1:3 or 1:4)
- Minimize PEEP in asthma (air trapping already generates intrinsic PEEP)
- Extrinsic PEEP set at ~75–85% of measured auto-PEEP in COPD to offset triggering effort
- Deep sedation ± paralysis during most severe phase of asthma
- Non-invasive positive pressure ventilation (NIPPV/BiPAP) is the preferred initial approach in COPD exacerbations — reduces need for intubation and mortality
8. Non-Invasive Ventilation (NIV) vs. Invasive MV
| Feature | NIV (BiPAP/CPAP) | Invasive MV |
|---|---|---|
| Interface | Mask (face, nasal, helmet) | Endotracheal tube |
| Airway protection | None | Full |
| VAP risk | Low | High (~15% incidence) |
| Sedation required | Minimal | Usually required |
| Best indications | COPD exacerbation, cardiogenic pulmonary edema, immunocompromised hypoxemia | Apnea, airway compromise, failure of NIV |
High-Flow Nasal Cannula (HFNC) is an intermediate step: delivers heated/humidified O₂ at 30–60 L/min, provides ~2–5 cmH₂O PEEP, reduces work of breathing. Proven non-inferior to NIV in post-extubation prophylaxis; reduces reintubation vs. conventional O₂ at 48–72h. — Washington Manual
9. Liberation from Mechanical Ventilation (Weaning)
The right approach is active liberation, not slow weaning — excessive caution extends MV time by up to 40%.
Step 1: Daily Readiness Assessment
| Criterion | Target |
|---|---|
| Underlying disease | Improving/resolved |
| Consciousness | Awake, off heavy sedation |
| FiO₂ | ≤ 0.5 |
| PEEP | < 8 cmH₂O |
| SaO₂ | > 88% |
| Hemodynamics | Stable |
| Secretions | Manageable; adequate cough |
Step 2: Weaning Predictor — Rapid Shallow Breathing Index (RSBI)
RSBI = f/VT (respiratory frequency ÷ tidal volume in liters)
- Measured during unaided spontaneous breathing (not with PS or CPAP, which falsely lower it)
- RSBI < 100 → likely to tolerate extubation (high sensitivity ≥ 0.90)
- RSBI > 100 → rapid shallow breathing pattern predicts failure
RSBI is a screening test (high sensitivity), not a confirmatory test. A positive screen should prompt an SBT, not immediate extubation. — Fishman's Pulmonary Diseases
Step 3: Spontaneous Breathing Trial (SBT)
A 30–120 minute trial of minimal ventilator support:
| Method | Details |
|---|---|
| T-piece | Disconnected from ventilator; breathes through heated/humidified circuit |
| Low PSV (5–8 cmH₂O) | Still connected; minimal pressure support to offset ETT resistance |
| CPAP 5 cmH₂O | Maintains PEEP; no inspiratory assistance |
SIMV-based weaning (gradual rate reduction) has the poorest weaning outcomes of all techniques and is not recommended as the primary weaning strategy.
SBT pass criteria:
- Comfortable, no marked anxiety or dyspnea
- RR < 35/min
- SaO₂ > 90%
- SBP 90–180 mmHg
- HR change < 20% from baseline
Step 4: Extubation Decision
Additional criteria beyond a passed SBT:
- Ability to follow commands
- Adequate cough and ability to manage secretions
- No excessive secretion burden
Post-extubation strategies:
- COPD patients — extubate to NIPPV → reduced mortality and HAP
- Chronic hypercapnic respiratory failure — NIPPV reduces reintubation rates
- General low-risk patients — HFNC reduces reintubation vs. conventional O₂ at 48–72h
10. Failure to Wean — Causes
| Category | Examples |
|---|---|
| Respiratory | Unresolved underlying disease; small ETT increasing resistance; auto-PEEP |
| Neuromuscular | Critical illness myopathy/polyneuropathy; prolonged NMB (especially with corticosteroids) |
| Metabolic | Non-AG metabolic acidosis → compensatory hyperventilation → fatigue; metabolic alkalosis → blunted drive → hypercapnia post-extubation |
| Psychological | Delirium, anxiety, PTSD interfering with SBTs |
| Cardiovascular | Weaning-induced cardiac ischemia or pulmonary edema (particularly in patients with LV dysfunction) |
11. Complications of Mechanical Ventilation
Pulmonary
- VILI (barotrauma, volutrauma, atelectrauma, biotrauma)
- Pneumothorax, pneumomediastinum
- Ventilator-Associated Pneumonia (VAP)
VAP — Key Facts
- Incidence: up to 15% of mechanically ventilated patients
- Mortality: ~50% when it occurs
- Defined as pneumonia ≥ 48h after intubation
- Common pathogens: S. aureus, P. aeruginosa, gram-negative enteric rods
- Empiric treatment: IV β-lactam (pip-tazo, cefepime, or ceftazidime) ± vancomycin/linezolid (for MRSA risk) or carbapenem (MDR gram-negative risk)
- Treatment duration: 7 days (shorter is non-inferior)
VAP Prevention Bundle
| Intervention | Efficacy |
|---|---|
| Head-of-bed elevation ≥ 30–45° | 70% VAP reduction |
| Subglottic secretion drainage ETT | 50% VAP reduction |
| Minimize ventilator circuit tubing changes | Reduces bacterial entry |
| Hand hygiene | Standard precaution |
| Daily sedation interruption + SBT | Reduces MV duration |
| Oral/dental hygiene | Reasonable, uncertain evidence |
Extrapulmonary Complications
- GI stress ulcers/bleeding → PPI or H₂ blocker prophylaxis
- DVT/PE → pharmacological ± mechanical prophylaxis
- Delirium and sleep disruption → minimize sedation, early mobility, day-night cycle
- ICU-acquired weakness (diaphragm and peripheral muscle atrophy) → minimize NMB, early physiotherapy
12. Hemodynamic Effects of Positive Pressure Ventilation
Positive pressure ventilation has the opposite hemodynamic effects to spontaneous breathing:
- Increases intrathoracic pressure → reduces venous return → reduces preload → may drop cardiac output
- High PEEP exaggerates this effect
- RV afterload may increase (alveolar overdistension compresses alveolar vessels)
- Clinically important in patients with hypovolemia or RV dysfunction — always assess fluid responsiveness when hemodynamic instability develops on the ventilator
Sources: Harrison's Principles of Internal Medicine 22E; Fishman's Pulmonary Diseases and Disorders; Washington Manual of Medical Therapeutics; Current Surgical Therapy 14e; Sabiston Textbook of Surgery
This is a shared conversation. Sign in to Orris to start your own chat.