Imaging cameras in radiology in detail , principle , components, workings and image processing work station in detail
imaging cameras radiology principles components image processing workstation detailed
radiology imaging camera types CCD flat panel detector gamma camera principles components
imaging camera radiology principles components workstation image processing
radiology image processing workstation PACS DICOM window level postprocessing MRI CT
imaging camera radiology flat panel detector gamma camera image intensifier
Imaging Cameras in Radiology: Principles, Components, Workings & Image Processing Workstations
Overview
- Image Intensifier + Video Camera (classical fluoroscopy)
- Charge-Coupled Device (CCD) / CMOS Cameras (digital fluoroscopy, some CR/DR systems)
- Flat-Panel Detectors (FPD) — direct and indirect conversion (modern DR/fluoroscopy)
- Gamma Camera (nuclear medicine: SPECT, planar scintigraphy)
- Computed Radiography (CR) Phosphor Plate Systems
1. Image Intensifier + Video Camera System
Principle
Components
| Component | Function |
|---|---|
| Input Phosphor | Converts X-rays to light photons (typically CsI/NaI crystals in a columnar structure) |
| Photocathode | Thin metal layer (cesium–antimony alloy) on the back of the input phosphor; converts light to electrons (photoelectric effect) |
| Electrostatic Lenses | Series of focusing electrodes that keep emitted electrons in spatial alignment during travel |
| Anode | ~25,000 V accelerating potential; accelerates electrons from cathode to output phosphor |
| Output Phosphor | Smaller than input phosphor; electrons strike it, re-emitting visible light as a bright, minified image |
| Optical Coupling System | High-resolution lenses, mirrors, or fiber optics that route output light to the camera |
| Video Camera (CCTV/CCD) | Converts the light image to an electronic signal |
Working
- X-rays pass through the patient and strike the input phosphor (10–40 cm diameter), generating light photons.
- These photons release electrons from the photocathode (photoelectric effect).
- Electrons are accelerated toward the anode by ~25 kV and focused by electrostatic lenses — preserving spatial geometry.
- Electrons converge onto the smaller output phosphor (~2.5 cm), producing a bright, inverted, minified image. Brightness gain = minification gain × flux gain (overall ~5,000–10,000×).
- The light image is coupled optically to a closed-circuit TV (CCTV) camera for display.
Resolution: ~4–5 lp/mm at the output phosphor; degrades to ~1–2 lp/mm through the TV coupling chain. — Rockwood & Green's Fractures in Adults, 10th ed.
Magnification Modes
2. CCD and CMOS Cameras
Principle
Components
- Photosensitive pixel array — typically amorphous silicon or crystalline silicon elements
- Charge transfer register — shifts charge from pixel to pixel in sequence to a read-out amplifier
- Analog-to-Digital Converter (ADC) — converts the analog charge to a digital value (12–14 bit depth common)
- Fiber optic coupler or lens — demagnifies the scintillator image down to CCD chip size
- Scintillator layer — converts X-rays to visible light (CsI:Tl or Gd₂O₂S) before reaching the CCD
Working
- X-rays strike the scintillator (e.g., CsI) → converted to visible light.
- Light is funneled via fiber optics or demagnifying lenses onto the CCD chip.
- Each pixel accumulates charge in proportion to light intensity.
- Charge is read row by row through the transfer register.
- ADC converts analog charges to digital pixel values → pixel matrix → image.
A CCD with a 1,024 × 1,024 matrix can achieve resolution of ~10 lp/mm. Digital output enables computer post-processing and digital subtraction angiography (DSA). — Rockwood & Green's Fractures in Adults, 10th ed.
3. Flat-Panel Detectors (FPD)
A. Indirect Conversion FPD (TFT-Photodiode Array)
- Scintillator layer — thallium-doped CsI (columnar structure reduces lateral light spread) or gadolinium oxysulfide (GOS/Gadox)
- Photodiode array — amorphous silicon (a-Si) photodiodes; each photodiode = one pixel
- Thin-Film Transistor (TFT) array — one TFT per pixel; acts as a switch to read out accumulated charge
- Gate driver circuitry — activates TFT rows sequentially
- Charge amplifiers and ADCs — amplify and digitize signal per column
- X-rays → scintillator → multiple visible light photons per X-ray
- Light photons → photodiodes → electron-hole pairs → charge accumulation
- TFT switches activate row by row; charge flows to column amplifiers
- ADCs digitize the signal → pixel matrix → image
B. Direct Conversion FPD (Amorphous Selenium)
- Amorphous selenium (a-Se) layer — photoconductive material; X-rays liberate electron-hole pairs
- Bias voltage (~1,000–5,000 V across a-Se layer) — drifts charges to collection electrodes
- TFT array — collects and reads out charge
- ADCs — digitization
- X-rays interact with a-Se → direct generation of electron-hole pairs
- Electric field separates charges → electrons/holes drift to electrodes
- TFT array reads out accumulated charge → ADC → pixel value
Direct conversion uses amorphous selenium photoconductors within FPDs; indirect conversion uses a scintillator (most commonly CsI:Tl or gadolinium compounds) with either a CCD or TFT array. — Grainger & Allison's Diagnostic Radiology
4. Gamma Camera (Nuclear Medicine)
Principle
Components
| Component | Role |
|---|---|
| Collimator | Lead plate with parallel (or diverging/converging/pinhole) holes; only accepts γ-rays traveling in a specific direction; provides spatial localization |
| NaI(Tl) Scintillation Crystal | Large single crystal (up to 60×40 cm, 6–13 mm thick); γ-ray interaction → scintillation light photons; hermetically sealed in aluminum |
| Perspex Light Guide | Optical coupling between crystal and PMT array |
| PMT Array (30–100 tubes) | Each tube: photocathode → dynode chain → anode; amplifies light signal ~10⁶×; position weighted average determines x-y interaction location |
| Preamplifiers | Convert anode current to voltage pulses proportional to energy absorbed |
| Pulse Height Analyzer (PHA) | Energy window selection: accepts γ-rays of the correct photopeak energy; rejects scattered photons |
| Anger Position Network / ADC | Calculates x-y coordinates from weighted PMT signals; modern systems are fully digital |
| Computer/Image Matrix | Builds up the image pixel-by-pixel from accepted events |
Working
- Radiopharmaceutical emits γ-rays in all directions inside the patient.
- Collimator accepts only γ-rays traveling ≈ perpendicular to its face (for parallel-hole type); all others are absorbed in the lead septa.
- Accepted γ-rays enter the NaI(Tl) crystal → interaction (photoelectric or Compton) → scintillation flashes.
- Light spreads to multiple PMTs; signal amplitude of each PMT is proportional to its proximity to the interaction point.
- Anger position circuit: x-y coordinates calculated by a weighted centroid of all PMT signals.
- PHA: total pulse height (sum of all PMTs) = γ-ray energy → only events within the photopeak window are accepted.
- Accepted events are placed at their calculated x-y position in the image matrix (commonly 64×64 to 512×512).
- Acquisition ends when preset count or time is reached → image displayed on monitor.
Collimator Types
| Type | Use | Effect |
|---|---|---|
| Parallel-hole | Standard imaging | 1:1 size, no magnification |
| Diverging | Large organs (lungs) | Minifies image |
| Converging | Small organs | Magnifies image |
| Pinhole | Thyroid, tear ducts | High magnification, inverted |
Modern Developments
5. Computed Radiography (CR) — Photostimulable Phosphor Plates
Principle
Components
- Imaging plate — phosphor layer on plastic backing
- Laser reader unit — red HeNe or diode laser scans the plate row by row
- Light guide / PMT — captures emitted blue/violet photostimulated luminescence (PSL)
- ADC — digitizes the PMT signal
- Plate eraser — bright white light flood erases residual signal for reuse
Working
- X-ray exposure → energy trapped in phosphor as electron-hole pairs in metastable states (latent image)
- Laser scan → stimulated luminescence emission (PSL) — light released proportional to trapped energy
- PMT collects light → ADC → digital pixel value → image reconstruction
- Flood-light erasure → plate reused
6. Image Processing Workstation (PACS)
Definition
Architecture
Modalities (CT, MRI, DR, US, NM)
↓ [DICOM]
PACS Server
(image archive + database)
↓ [network]
Reading Workstations
(high-resolution displays + processing software)
↓
RIS (Radiology Information System) integration
HIS (Hospital Information System)
Hardware Components
| Component | Specification |
|---|---|
| CPU | Multi-core high-speed processor (e.g., Intel Xeon / AMD EPYC) |
| RAM | 32–128 GB for handling large datasets (CT volumes, MRI series) |
| GPU | Dedicated GPU for 3D rendering, MPR, AI inference |
| Storage | RAID-based SSD/HDD or NAS/SAN for DICOM archiving |
| Network | Gigabit/10GbE for fast DICOM transfer |
| Displays | 2–5 high-resolution medical-grade monitors |
Displays (Medical-Grade Diagnostic Monitors)
- Spatial resolution: 2–5 megapixels (MP) for general radiology; 5 MP for mammography (non-negotiable standard)
- Luminance: ≥400 cd/m² (nits) for primary diagnostic use
- Grayscale: 10–12-bit grayscale depth (1,024–4,096 levels)
- Calibration: DICOM Part 14 GSDF (Grayscale Standard Display Function) calibration mandatory
- Brands: Barco, Eizo RadiForce, LG Medical, TOTOKU; as of 2026, Apple Pro Display XDR is FDA-cleared for diagnostic imaging
- Mammography requires dedicated FDA-approved monitors regardless
Software Functions
Core Viewing Tools
- Window/Level (W/L): Adjusts brightness (level = center of window) and contrast (width). Essential for visualizing soft tissue, bone, lung, brain windows in CT.
- Zoom & Pan: Pixel-level magnification without true resolution increase beyond native
- Cine playback: Sequential multi-frame display for CT/MRI/echocardiography series
- Measurements: Length, angle, area, volume (ROI tools); Hounsfield unit values in CT
Advanced Reconstruction & Post-Processing
- MPR (Multiplanar Reconstruction): Reformats 3D CT/MRI data into any arbitrary plane (axial, coronal, sagittal, oblique)
- MIP (Maximum Intensity Projection): Highlights highest-density voxels along a ray — ideal for vascular imaging (CT angiography, MR angiography)
- MinIP (Minimum Intensity Projection): Highlights lowest-density structures — airway imaging
- VR (Volume Rendering): Full 3D surface or semi-transparent rendering using transfer functions
- CPR (Curved Planar Reconstruction): "Unrolling" tortuous vessels for analysis
- DSA (Digital Subtraction Angiography): Subtracts a pre-contrast "mask" image from post-contrast frames to isolate vessels
- Fused imaging: PET-CT, SPECT-CT overlay of functional and anatomical data
Image Enhancement
- Smoothing / Noise reduction: Spatial filters (Gaussian, median) reduce quantum noise
- Edge enhancement: High-pass filters sharpen structures
- Histogram equalization: Redistributes pixel values to improve perceived contrast
- AI-based denoising: Deep learning models (e.g., CT noise reduction algorithms from GE, Siemens)
Nuclear Medicine Specific
- Color tables / hot maps: Assign color scales to count density
- Interpolation: Spreads counts across a larger display matrix (reduces pixelation)
- Background subtraction: Removes non-specific activity
- SPECT reconstruction: Filtered back-projection (FBP) or iterative algorithms (OSEM) reconstruct 3D tomographic slices from projection data
DICOM Standard
- DICOM Store (C-STORE): Sends images to PACS
- DICOM Query/Retrieve (C-FIND/C-MOVE): Finds and fetches prior studies
- DICOM Print: Sends images to laser printers
- DICOM Worklist: Integrates with RIS for patient scheduling
Workflow Integration
- RIS-PACS integration: Radiologist receives worklist from Radiology Information System; reports are linked to images
- HL7 messaging: Interoperability with hospital EMR
- Teleradiology: Remote reading over secure VPN/internet; enables off-site or overnight reads
- AI-CAD integration: Computer-aided detection/diagnosis tools (e.g., lung nodule CAD, fracture detection) embedded in PACS viewer
Summary Comparison Table
| Camera/Detector | Radiation Detected | Primary Application | Key Detector Material | Resolution |
|---|---|---|---|---|
| Image Intensifier + CCD | X-rays | Fluoroscopy, DSA | CsI input phosphor + photocathode | 1–5 lp/mm |
| CCD/CMOS | X-rays (via scintillator) | Digital fluoroscopy, DR | CsI:Tl + a-Si photodiode | Up to 10 lp/mm |
| Indirect FPD (TFT) | X-rays | DR, digital fluoroscopy | CsI:Tl or GOS + a-Si TFT | 3–7 lp/mm |
| Direct FPD (a-Se) | X-rays | DR, mammography | Amorphous selenium | High (no light blur) |
| CR Plate | X-rays | Portable/general radiography | BaFBr:Eu²⁺ phosphor | 3–5 lp/mm |
| Gamma Camera | Gamma rays | Nuclear medicine (SPECT) | NaI(Tl) + PMT array | ~4–10 mm spatial |
Key Images for Reference
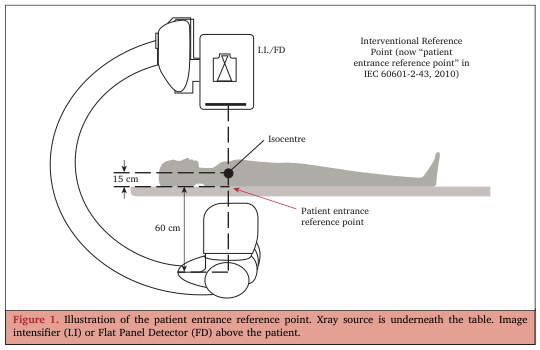
- Rockwood & Green's Fractures in Adults, 10th ed. 2025 — Fluoroscopy systems, digital fluoroscopy, CCD
- Grainger & Allison's Diagnostic Radiology — CR, DR, FPD, PACS
- Fuster & Hurst's The Heart, 15th ed. — X-ray image generation chain, catheterization lab imaging
- Radiology Cafe FRCR Physics Notes — Gamma camera components and image formation
- Cockcroft Institute Lecture 5: Gamma Cameras — Anger position network, collimator physics
- How Radiology Works — Direct vs. indirect flat panel detectors
No u know about dry cameras , its types laser and thermal camera , give me detailed notes on this ?
dry camera radiology laser camera thermal camera principles components working detailed
dry laser camera radiology medical imaging Kodak Fuji Dryview laser imager principles components film printing
dry camera radiology laser thermal camera principles components working photothermographic
dry thermal camera radiology direct thermal printing Agfa Drystar photothermographic film mechanism
dry camera laser thermal parts components DICOM print densitometer film transport printing sequence quality control
dry camera radiology DICOM print service network connectivity QC densitometer calibration comparison laser vs thermal
Dry Cameras in Radiology — Detailed Notes
What is a Dry Camera?
Classification of Dry Cameras
DRY CAMERAS
├── 1. Dry Laser Camera (Photothermographic)
│ → Two-step: Laser exposure + thermal development
│ Example: Kodak/Carestream DryView 8900, 6800, 5950
│
└── 2. Direct Thermal Print Camera
→ Single-step: Thermal print head only
Example: Agfa Drystar 5500, 5503
Part I — Dry Laser Camera (Photothermographic)
Principle
-
Step 1 — Laser Exposure (Latent Image Formation): A modulated infrared laser beam scans across a photothermographic film, releasing photons into the light-sensitive silver halide layer. The laser energy converts silver ions (Ag⁺) into metallic silver atoms, forming a latent image (invisible at this stage). The intensity of the laser is modulated in direct proportion to the pixel intensity of the digital image data received from the modality.
-
Step 2 — Thermal Development (Image Visualization): The exposed film passes over a heated rotating drum (~120–140°C for ~15 seconds). Thermal energy acts as a catalyst, driving a photothermographic reaction in which the latent silver atoms catalyze the reduction of silver behenate (Ag⁺ of a long-chain fatty acid) by reducing agents in the film. This amplifies the latent image into a fully visible, stable metallic silver image — no chemicals required.
"The dry laser camera is a two-step process involving a laser diode optic system and photothermography... The latent image is initiated by a laser beam that releases photons into the sensitive layer during exposure, leading to the conversion of silver ions (Ag⁺) into metallic silver. The film absorbs thermal energy for 15 s from a rotating drum whose temperature ranges from 120 to 140°C." — Dry Imaging Cameras, J Med Phys, PMC3137864
Components of a Dry Laser Camera
A. Film Supply & Transport Subsystem
| Component | Function |
|---|---|
| Film supply cartridge | Sealed daylight-loadable cassette containing 125 sheets; cartridge recognition chip identifies film type, size, and remaining count |
| Suction cups (vacuum pickup) | Lifts one film sheet at a time from the cartridge without touching the image area |
| Vertical transport rollers | Feed the film toward the exposure area |
| Platen rollers | Feed film onto the platen |
| Platen (flat glass pane) | Holds the film flat and stationary during laser scanning exposure |
| Film transport rollers (post-exposure) | Move the film from exposure area to the processor drum and onward |
B. Laser Optical System (Exposure Unit)
| Component | Function |
|---|---|
| Laser diode | Infrared (IR) semiconductor laser (typically ~780–830 nm wavelength); generates the modulated laser beam |
| Laser modulator | Modulates (varies) the laser beam intensity in proportion to the pixel value of each image point — brighter pixels = more laser energy = darker silver deposit |
| Collimating lens | Collimates the divergent laser beam into a parallel beam |
| Polygonal (rotating) mirror | A multi-faceted mirror rotating at high speed; deflects the laser beam in a fast sweep across the width of the film (fast-scan axis / X-direction) |
| Toroidal (f-θ) lens | Corrects the scan velocity variation caused by the rotating mirror, ensuring uniform spot size and scanning speed across the full film width |
| Fold mirrors | Redirect the beam path compactly within the camera housing |
| Film transport (slow-scan axis) | As the laser sweeps across the film (X), the film moves incrementally in the Y direction — together creating a raster scan covering the entire film area |
Optical system components: 1: Laser, 2: lens, 3: laser modulator, 4: polygonal mirror, 5: toroidal lens, 6: mirrors, 7: film transport, 8: rollers — PMC3137864
C. Thermal Processor (Development Unit)
| Component | Function |
|---|---|
| Processor drum (heating drum) | Rotating heated drum at 120–140°C (±0.1°C precision); film wraps around drum surface for ~15 seconds of thermal development |
| Flatbed heater | Maintains temperature ~1°C below drum temperature during the flatbed development phase |
| Cooling section | Removes heat from the film after development, stops the reaction and hardens the film base |
| Slack loop assembly | 3 rollers forming a film loop at the processor entrance; prevents vibration transmission from the drum back to the exposure transport (which would cause image artifacts) |
| Temperature controller | Precise electronic PID controller maintains drum temperature to ±0.1°C; critical for consistent image density (Dmax) |
D. Quality Control & Output
| Component | Function |
|---|---|
| Densitometer | Built-in optical density sensor; reads a test patch or entire image to verify Dmax (maximum density) and Dmin (minimum density/background); triggers calibration adjustments automatically |
| Sorter / Output bins | Multiple output trays (typically 3–7); images sorted by modality, patient, or exam type |
| Film receiving tray / hood | Alternative output at the top of the unit |
Printing Sequence in a Dry Laser Camera (e.g., Kodak DryView 8900)
Step 1: Suction cup lifts one film from sealed supply cartridge
↓
Step 2: Vertical transport rollers feed film upward
↓
Step 3: Film arrives at platen (flat glass pane) — the exposure area
↓
Step 4: Film-at-entrance sensor detects film; starts exposure sequence
↓
Step 5: SOP (Start of Print) sensor triggered → laser exposure begins
Polygonal mirror sweeps laser beam across film (fast scan)
Film advances incrementally (slow scan)
Each pixel intensity modulates laser power → latent image formed
↓
Step 6: Film exits platen into vertical transport rollers
↓
Step 7: Film enters slack loop assembly (prevents vibration)
↓
Step 8: Film wraps around heated processor drum (120–140°C, ~15 sec)
Photothermographic development → latent image → visible silver image
↓
Step 9: Cooling section — image fixed, film hardened
↓
Step 10: Film passes through built-in densitometer (QC check)
↓
Step 11: Output rollers deliver film to sorter bins / hood
Photothermographic Film for Dry Laser Camera
- Light-sensitive silver halide — responds to the IR laser; forms latent image (metallic silver nuclei)
- Silver behenate (reducible silver salt of long-chain fatty acid, e.g., silver eicosanoate/behenate) — acts as the silver "reservoir" for image development
- Reducing agents (e.g., bisphenol compounds) — activated by heat; donate electrons to reduce Ag⁺ to Ag⁰, amplifying the latent image
- Dmax (maximum density): 3.00–3.30 (varies by film type and imager)
- Dmin (background/fog density): ≤0.17
Part II — Direct Thermal Print Camera
Principle
"In thermal print head technology, tiny heaters produce images. Digital signals from various modalities are processed and converted into electrical pulses. These are then transferred to a thermal print head, whose microscopic heat resistor elements convert electrical energy into heat energy. A thermal sensitive film passes close to the print head, with transfer of heat from each element. A chemical reaction results and a pixel is developed." — PMC3137864
Components of a Direct Thermal Print Camera
A. Film Handling Subsystem
| Component | Function |
|---|---|
| Film pickup unit | Handles up to 5 different film formats; uses vacuum pump with valves to lift one film at a time |
| Vacuum pump & valves | Generates suction to grip and lift film without physical damage |
| Film transport rollers | Driven by a gearbox module; moves film through the system |
B. Thermal Print Head (Core Component)
| Component | Function |
|---|---|
| Thermal print head | A linear array of microscopic heat-resistor elements (heating elements), one per pixel column; operates at ~52.5°C |
| Heating elements (resistors) | Convert electrical pulses into heat; each element independently controlled to produce the correct gray level for each pixel |
| Pressure roller / drum | Positioned in close apposition to the print head; maintains constant, uniform pressure between film and print head to ensure even heat transfer |
| Image scanning line | The line of contact between print head and film; one row of pixels is printed per advance step |
C. Film Transport (During Printing)
D. Quality Control & Output
| Component | Function |
|---|---|
| Densitometer | Density verification; confirms image quality meets diagnostic standards |
| Film receiving tray / sorter | Sorts finished films by modality and patient records into multiple output bins |
Printing Sequence in a Direct Thermal Print Camera (e.g., Agfa Drystar 5500)
Step 1: Vacuum pump lifts one film from supply cartridge
↓
Step 2: Film fed into transport rollers (driven by gearbox module)
↓
Step 3: Film positioned between thermal print head and drum
(in close contact — drum maintains pressure)
↓
Step 4: Digital image data → converted to electrical pulses
Electrical pulses → each resistive element generates heat
Film advances one pixel row at a time
Heat → chemical reaction → pixel developed on thermosensitive film
(Row by row, full image printed)
↓
Step 5: Output rollers transport developed film out of print zone
↓
Step 6: Film passes through densitometer (automatic QC)
↓
Step 7: Film delivered to sorter bin / output tray
Direct Thermal Film
- Contains leuco dyes or silver-based thermochromic compounds in the emulsion layer
- Heat causes an irreversible chemical reaction forming a gray/black image
- Film is sensitive to heat only — not to visible or UV light
- Daylight insensitive — can be loaded in room light
- Examples: Agfa DRYSTAR DT 2B (blue base), DRYSTAR DT 2C (clear base), DRYSTAR DT 2 Mammo
Comparison: Dry Laser Camera vs. Direct Thermal Camera
| Feature | Dry Laser Camera | Direct Thermal Camera |
|---|---|---|
| Technology | Two-step: Laser + photothermography | One-step: Thermal print head |
| Image formation | Laser forms latent image → heat develops it | Heat forms image directly |
| Film type | Photothermographic (PTG) silver halide film | Thermosensitive (direct thermal) film |
| Film sensitivity | Infrared laser light + heat | Heat only (daylight insensitive) |
| Drum temperature | 120–140°C | ~52.5°C (print head) |
| Key moving part | Polygonal scanning mirror | No scanning mirror (print head spans full width) |
| Mechanical complexity | Higher (laser optics, polygon mirror, toroidal lens) | Lower (simpler mechanical path) |
| Resolution | 508 dpi, 50 µm spot | 508 dpi, 12-bit |
| Image quality | Excellent (very fine detail, low noise) | Excellent (laser-like quality per Agfa) |
| Dmax | Up to 3.3 | Up to 3.8 (mammo) |
| Examples | Kodak/Carestream DryView 8900, 6800, 5950 | Agfa Drystar 5500, 5503, 7 |
| Maintenance | Laser & optics need periodic alignment | Print head wear over time |
| Environmental | No chemicals, no wet processing | No chemicals, no wet processing |
Network and DICOM Connectivity
- DICOM Print SCP (Service Class Provider): The dry camera acts as a print server; it accepts DICOM print requests from modalities (CT, MRI, CR, DR, etc.) and workstations over the hospital network.
- DICOM Print SCU (Service Class User): Each modality or workstation sends images to the camera's IP address using the DICOM C-PRINT service.
- IP configuration: Each camera has a unique IP address on the hospital LAN; modalities are configured with the camera's IP, port number (typically 104), and AE title (Application Entity title).
- DICOM Grayscale Standard Display Function (GSDF) calibration ensures printed optical densities match the display appearance on calibrated monitors.
- DICOM Worklist integration allows images to be matched to patient demographics automatically.
Quality Control (QC) of Dry Cameras
Built-in Automatic QC
- Densitometer inside the camera reads each printed film's density
- Compares measured Dmax and Dmin against preset calibration targets
- Auto-calibration: adjusts laser power (laser cameras) or pulse width (thermal cameras) to maintain consistent density
External / Periodic QC
- SMPTE (Society of Motion Picture and Television Engineers) test pattern is printed and evaluated:
- 5% and 95% gray patches must be visually distinguishable
- Small high-contrast squares at 0% and 100% must be visible
- Spatial resolution test patterns
- Optical densitometer measurements of Dmax, Dmin, and gamma curve
- Frequency: Daily or as per ACR/departmental protocol
Advantages of Dry Cameras
- No wet chemicals — no developer, fixer, or wash water required
- No darkroom — films loaded in daylight
- Compact — tabletop or floor-standing units; easy to place near modalities
- Fast — first film delivered in ~90 seconds (Kodak DryView 5950)
- Consistent quality — automatic densitometry and calibration
- Multiformat — multiple image layouts per film (1:1, 2:2, 3:4, etc.)
- Environmentally friendly — no chemical waste disposal
- Long shelf life — sealed cartridges stable for months
- DICOM compatible — integrates seamlessly with any modality
Disadvantages
- Higher consumable cost per film compared to wet systems
- Thermal cameras: Print head wears out after millions of prints (replacement needed)
- Laser cameras: Optics (polygon mirror, laser diode) require periodic service
- Temperature sensitivity: Drum temperature drift causes density variations
- Limited to grayscale (standard diagnostic cameras); color available but not common in radiology
Clinical Applications
- CT & MRI — multiformat film prints for patient records, neurosurgery planning
- Digital Radiography (DR/CR) — routine X-ray films for orthopedics, chest, etc.
- Mammography — dedicated high-density films (Dmax 3.8) for breast imaging
- Nuclear Medicine — SPECT, bone scan, thyroid scan hard copies
- Ultrasound — obstetric, cardiac, abdominal images
- DSA / Fluoroscopy — angiography film records
- Teleradiology — printed films sent with referred patients
- Dry Imaging Cameras — J Med Phys 2011; PMC3137864 (comprehensive peer-reviewed reference)
- Carestream DRYVIEW Laser Imaging Film Technical Data Sheet TI-5021
- Agfa Drystar 5500 Reference Manual
- Kodak DryView 8150/8900 Service Manual
- Carestream DRYVIEW 5950 Laser Imager specifications