Give me exam oriented notes of Atrial Fibrillation with mnemonics
Reading File
Finding Sources
Searching the Web
atrial fibrillation exam notes mnemonics CHADS2 treatment classification
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Searching Images
atrial fibrillation ECG irregularly irregular rhythm
Reading File
Reading File
I now have enough material. Let me compile comprehensive exam-oriented notes.
🫀 Atrial Fibrillation — Exam-Oriented Notes
Sources: Braunwald's Heart Disease, Fuster & Hurst's The Heart, Tintinalli's Emergency Medicine
1. DEFINITION
AF is a supraventricular arrhythmia characterized by:
- Disorganized atrial electrical activity (300–600 impulses/min)
- Irregularly irregular ventricular rhythm
- Absence of distinct P waves → replaced by fibrillatory (f) waves
Most common arrhythmia causing hospitalization (~33% of arrhythmia-related admissions). Associated with 5× ↑ stroke risk, 2× ↑ mortality, and 2× ↑ cognitive dysfunction.
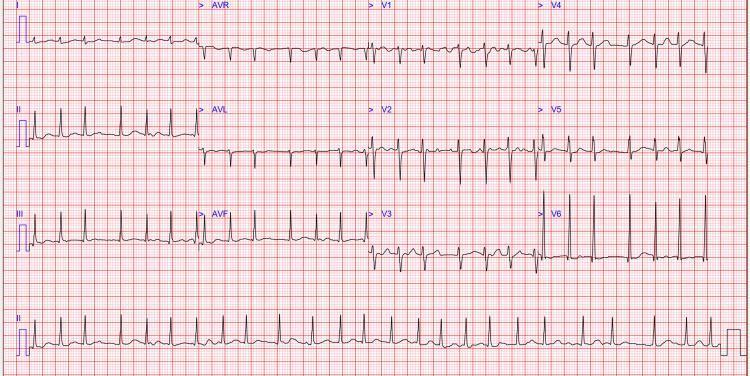
2. ECG FEATURES — "3 I's of AF"
| Feature | Detail |
|---|---|
| Irregularly Irregular RR intervals | No consistent pattern |
| Isoelectric line absent | f waves (300–600/min), variable amplitude/shape |
| Invisible P waves | Replaced by f waves; best seen in V1, II |
Ventricular rate: 100–160 bpm (untreated)
- WPW + AF → rate can exceed 250 bpm via accessory pathway ⚠️ (dangerous — avoid AV nodal blockers)
- Very rapid rate (>170 bpm) → may falsely appear regular
3. CLASSIFICATION — "PP LP"
| Type | Definition |
|---|---|
| Paroxysmal | Self-terminates within 7 days (usually <48h) |
| Persistent | Lasts >7 days; requires intervention to terminate |
| Long-standing Persistent | Continuous AF >1 year |
| Permanent | Decision made not to restore sinus rhythm |
🧠 Mnemonic: "Paroxysmal Patients Linger Permanently"Classification does not change based on effects of cardioversion or AAD therapy.
Autonomic subtypes (paroxysmal AF):
- Vagotonic AF (~25%): occurs at rest/sleep, worsened by digoxin → use disopyramide
- Adrenergic AF (~10–15%): during exertion → use beta-blockers
- Mixed/random (~60%): most common
4. CAUSES — Mnemonic "PIRATES"
| Letter | Cause |
|---|---|
| P | Pulmonary embolism / Pulmonary hypertension |
| I | Ischemic heart disease (CAD) |
| R | Rheumatic valvular disease (especially mitral stenosis) |
| A | Alcohol ("Holiday Heart"), Autonomic |
| T | Thyrotoxicosis (hyperthyroidism) |
| E | Electrolyte disturbance / Embolism |
| S | Sleep apnea / Structural heart disease (HCM, DCM, HF) |
Additional important causes:
- Hypertension (most common overall)
- Post-cardiac surgery (Post-op AF)
- Obesity, epicardial fat infiltration
- Amyloidosis, constrictive pericarditis
5. PATHOPHYSIOLOGY
Two key requirements:
- Trigger — most commonly from pulmonary vein ectopic foci (especially superior PVs)
- Substrate — atrial fibrosis, inflammation, dilatation → re-entrant circuits
Mechanisms:
- Multiple wavelet re-entry
- Rotors (stable high-frequency rotational sources)
- Atrial remodeling → fibrosis → reduced conduction velocity → perpetuation
Consequences:
- Loss of atrial kick → ↓ CO by 10–20% (worse in stiff LV/HFpEF)
- Tachycardia-induced cardiomyopathy (persistent rapid rate)
- LA thrombus → Left Atrial Appendage (LAA) is the site in 90% of cases → embolic stroke
6. CLINICAL FEATURES — Mnemonic "PFLS + Polyuria"
| Symptom | Note |
|---|---|
| Palpitations | Most common; may be absent in elderly |
| Fatigue | Often misattributed to aging |
| Lightheadedness | From ↓ CO |
| Shortness of breath / dyspnea | Especially on exertion |
| Polyuria | From atrial natriuretic peptide (ANP) release |
- 25% are asymptomatic (often elderly, persistent AF)
- Syncope: long pause on termination (sick sinus syndrome), or neurocardiogenic
- Can first present as stroke or heart failure
Exam Tip: AF + rapid irregular pulse + absent P waves on ECG = classic exam picture.
7. STROKE RISK — CHA₂DS₂-VASc Score
🧠 Mnemonic: "CHADs VASCULAR (2-1-1-1-2-1-1-1)"
| Letter | Risk Factor | Points |
|---|---|---|
| C | Congestive Heart Failure | 1 |
| H | Hypertension | 1 |
| A₂ | Age ≥75 years | 2 |
| D | Diabetes mellitus | 1 |
| S₂ | Stroke / TIA / thromboembolism (prior) | 2 |
| V | Vascular disease (MI, PAD, aortic plaque) | 1 |
| A | Age 65–74 years | 1 |
| Sc | Sex category (Female) | 1 |
Anticoagulation thresholds:
- Score 0 (men) or 1 (women): No anticoagulation
- Score 1 (men): Consider anticoagulation
- Score ≥2: Anticoagulate (Class I)
All patients ≥75 years automatically score ≥2 → anticoagulate regardless of AF type.
8. BLEEDING RISK — HAS-BLED Score
🧠 Mnemonic: "Has BLeD"
| Letter | Factor | Points |
|---|---|---|
| H | Hypertension (uncontrolled, SBP >160) | 1 |
| A | Abnormal renal/liver function | 1 each |
| S | Stroke history | 1 |
| B | Bleeding history or predisposition | 1 |
| L | Labile INR | 1 |
| E | Elderly (>65 years) | 1 |
| D | Drugs (antiplatelets/NSAIDs) or alcohol | 1 each |
Score ≥3 = high bleeding risk → does not contraindicate anticoagulation, but prompts caution and follow-up.
9. MANAGEMENT
A. Acute Management
Step 1 — Hemodynamically UNSTABLE:
→ Immediate DC cardioversion (synchronized)
Step 2 — Hemodynamically STABLE:
🧠 Mnemonic for acute AF: "ABCD"
- Anticoagulate
- Beta-blocker (rate control)
- Cardiovert (if indicated)
- Digoxin (adjunct, especially in HF)
Rate control targets:
- Rest: 60–80 bpm
- Moderate exercise: 90–115 bpm
| Drug | Use case |
|---|---|
| IV diltiazem / esmolol | First-line acute rate control |
| Beta-blockers | Rate control, adrenergic AF |
| Non-DHP CCBs (diltiazem, verapamil) | Rate control if no HF |
| Digoxin | HF with reduced EF, sedentary patients; poor at exercise rate control |
Cardioversion rules:
- AF <48 hours: Can cardiovert without prior anticoagulation (TEE optional)
- AF >48 hours or unknown duration: Anticoagulate ≥3 weeks before cardioversion, OR perform TEE to rule out LAA thrombus → then cardiovert
- Anticoagulate for ≥4 weeks after cardioversion regardless
B. Long-Term Management: Rate vs Rhythm Control
🧠 "Rate = AF accepted; Rhythm = restore sinus"
| Strategy | When to Choose |
|---|---|
| Rate control | Elderly, asymptomatic, permanent AF, large LA, failed cardioversions |
| Rhythm control | Young, symptomatic, HFrEF, first episode, short duration, small LA |
AFFIRM trial: Rate control = rhythm control in mortality outcomes (long-term).
C. Antiarrhythmic Drugs (Rhythm Control)
🧠 Mnemonic by structural heart disease:
| Situation | Drug |
|---|---|
| No structural heart disease | Flecainide, Propafenone ("pill-in-pocket") |
| HF/LV dysfunction | Amiodarone (drug of choice), Dofetilide |
| CAD | Sotalol, Amiodarone, Dofetilide |
| Hypertension with LVH | Amiodarone |
⚠️ Flecainide/propafenone are contraindicated in structural heart disease (pro-arrhythmic risk).
D. Anticoagulation
| Agent | Notes |
|---|---|
| DOACs (dabigatran, rivaroxaban, apixaban, edoxaban) | Preferred over warfarin in non-valvular AF — no INR monitoring, fewer drug interactions |
| Warfarin | INR target 2.0–3.0 (2.0–2.5 in elderly); still used in valvular AF (mitral stenosis, prosthetic valves) |
| WATCHMAN device | Percutaneous LAA closure — alternative when anticoagulation contraindicated |
⚠️ Valvular AF (rheumatic MS, prosthetic valves) = warfarin only, DOACs not recommended.
E. Non-Pharmacologic / Interventional
| Procedure | Indication |
|---|---|
| Catheter ablation (PV isolation) | Symptomatic paroxysmal/persistent AF refractory to AAD |
| AV node ablation + pacemaker | Rate control when drugs fail ("ablate and pace") |
| Surgical MAZE procedure | At time of open heart surgery |
| WATCHMAN device | LAA occlusion when anticoagulation contraindicated |
10. SPECIAL CLINICAL SITUATIONS
| Scenario | Key Point |
|---|---|
| WPW + AF | ⚠️ DO NOT give AV nodal blockers (digoxin, verapamil, diltiazem, beta-blockers) → may accelerate conduction via accessory pathway → VF. Use procainamide or cardioversion |
| AF + Mitral Stenosis | Warfarin regardless of CHA₂DS₂-VASc score; DOACs not effective |
| Post-operative AF | Common after cardiac surgery (peak 2–3 days post-op); beta-blockers prophylactically |
| Pregnancy + AF | Heparin (LMWH) preferred; warfarin teratogenic in 1st trimester; DOACs contraindicated |
| Thyrotoxicosis AF | Treat underlying hyperthyroidism; rate control with beta-blockers |
| HFrEF + AF | Rhythm control with amiodarone; ablation improves outcomes |
11. QUICK RECALL MNEMONICS — SUMMARY TABLE
| Mnemonic | What it covers |
|---|---|
| "3 I's" | ECG: Irregularly irregular, Isoelectric absent, Invisible P waves |
| "PP LP" | Classification: Paroxysmal, Persistent, Long-standing, Permanent |
| "PIRATES" | Causes of AF |
| "PFLS + Polyuria" | Symptoms |
| "CHADs VASc" | Stroke risk score |
| "Has BLeD" | Bleeding risk score |
| "ABCD" | Acute management: Anticoagulate, Beta-block, Cardiovert, Digoxin |
| "No SHD → Flec/Prop; HF → Amio" | Antiarrhythmic drug choice |
12. HIGH-YIELD EXAM FACTS
- Most common sustained arrhythmia in clinical practice
- Most common site of thrombus in AF = Left Atrial Appendage (LAA)
- Stoke risk = 5× higher in non-valvular AF
- WPW + AF → never give verapamil/digoxin/diltiazem/beta-blockers
- Valvular AF → warfarin, not DOACs
- Cardioversion after >48h AF → anticoagulate 3 weeks prior OR TEE to exclude thrombus
- Rate control targets: 60–80 bpm rest; 90–115 bpm exercise
- Digoxin: effective at rest but NOT during exercise for rate control
- Lone AF: historically = AF in patient <60y without hypertension or structural heart disease (term now abandoned)
- Holiday heart: AF triggered by acute alcohol intake (binge drinking)
- Polyuria in AF = due to ANP (atrial natriuretic peptide) release
- AFFIRM trial: no mortality difference between rate vs rhythm control strategies
— Braunwald's Heart Disease (10e); Fuster & Hurst's The Heart (15e); Tintinalli's Emergency Medicine
Tell me about impactful trials about Atrial Fibrillation and then what are upcoming recent changes about atrial fibrillation in real life practice and answer from full text sources as much as possible
Finding Sources
Searching PubMed
"atrial fibrillation" AND ("rhythm control" OR "rate control" OR ablation OR anticoagulation)
Searching the Web
atrial fibrillation 2024 2025 practice changes new guidelines EAST-AFNET early rhythm control wearables screening
Reading File
Reading File
Reading Article
Reading Article
Reading Article
Reading Article
Reading Article
Finding Sources
Searching the Web
ESC 2024 AF guidelines AF-CARE framework changes subclinical AF wearables anticoagulation
Reading File
Reading Article
Reading Article
Reading File
Finding Sources
Reading File
Reading File
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.