management of rashes in groin area due to sweating and tight clothes
Reading File
Finding Sources
Finding Sources
Searching the Web
intertrigo groin rash management treatment guidelines 2024
Searching PubMed
intertrigo management treatment
Reading File
Reading File
Loading Image
I now have comprehensive information from multiple authoritative textbooks and current guidelines. Here's the complete management guide:
Groin Rash (Intertrigo) — Causes, Diagnosis & Management
Intertrigo is an irritant/inflammatory dermatitis of skin folds caused by friction, heat, and moisture. The groin (inguinal and perineal folds) is one of the most commonly affected sites.
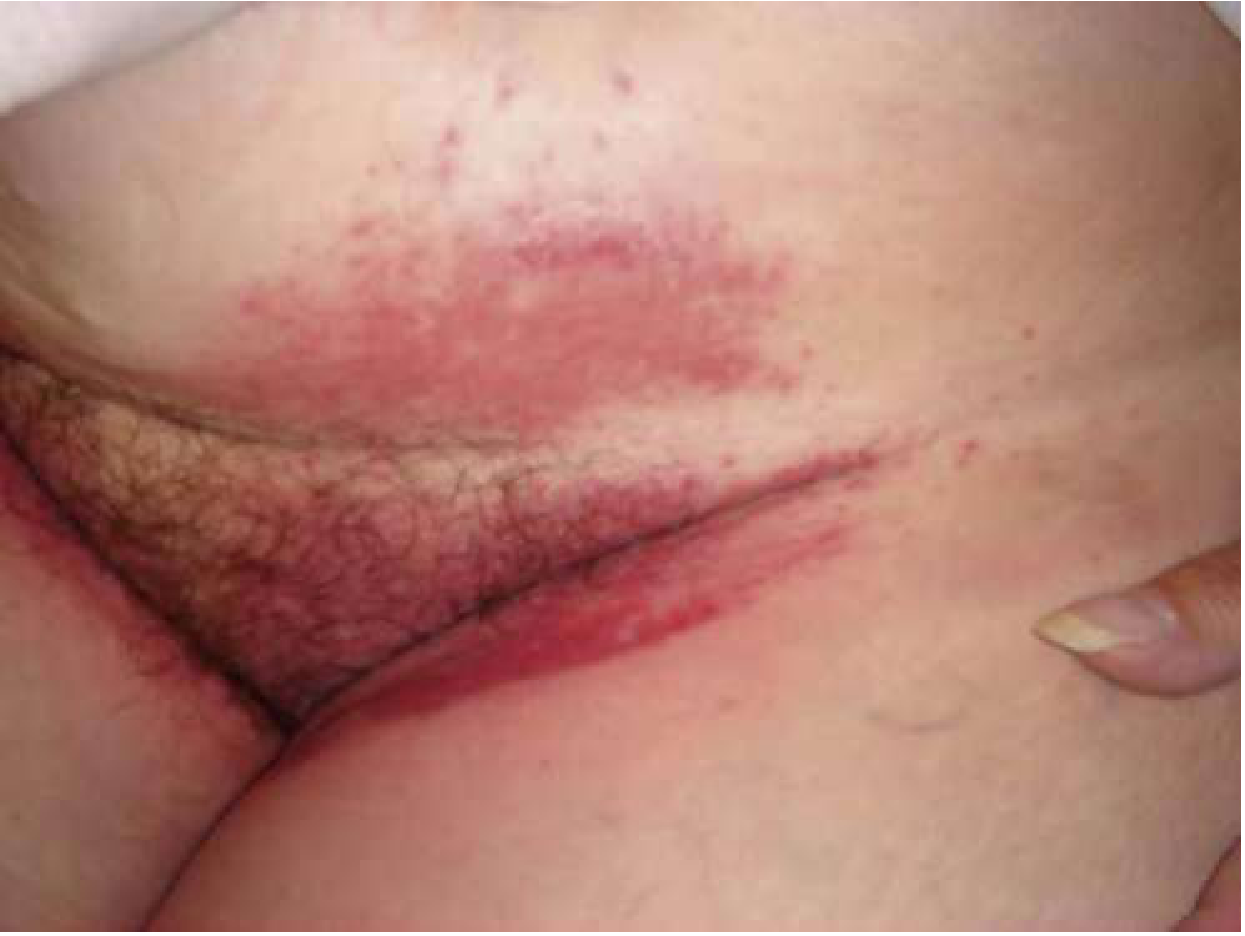
Understanding What's Happening
Tight clothes + sweat traps moisture → skin maceration → friction damage → secondary infection by fungi (Candida, dermatophytes) or bacteria (Staphylococcus, Streptococcus, Pseudomonas, Corynebacterium). The inflamed fold becomes erythematous, macerated, with erosions, fissures, burning and itching. - Andrews' Diseases of the Skin, p. 314
Predisposing factors: obesity, diabetes, hot/humid weather, immunosuppression, incontinence, elderly or young age.
Differential Diagnosis
Before treating, exclude look-alikes:
| Condition | Distinguishing Features |
|---|---|
| Candidal intertrigo | Satellite papules/pustules at margins; KOH positive |
| Tinea cruris | Raised scaly border; KOH shows hyphae; spares scrotum |
| Erythrasma | Coral-red fluorescence on Wood's lamp (Corynebacterium) |
| Inverse psoriasis | Well-demarcated, non-scaly, silvery plaques elsewhere on body |
| Streptococcal intertrigo | Fiery-red, moist, shiny, foul odor, no satellite lesions |
| Seborrheic dermatitis | Greasy scales; also in scalp/nasolabial folds |
| Contact/allergic dermatitis | Ask about deodorants, creams, hygiene sprays |
- Tintinalli's Emergency Medicine, p. 1696; Andrews' Diseases of the Skin, p. 314
Management
1. General Measures (First Line for All Cases)
The primary goal is eliminating maceration — reducing heat, friction, and moisture:
-
Keep the area dry and cool — after exercise/sweating, shower and dry thoroughly with a soft towel, or use a hairdryer on a cool/low setting
-
Loose, breathable clothing — switch from tight synthetic fabrics to loose cotton or moisture-wicking polyester; avoid occlusive dressings
-
Absorbent powders — talc or cornstarch powder applied to the fold reduces friction and moisture
-
Skin fold separation — place cotton gauze or InterDry Ag silver-impregnated textile between apposing surfaces; wicks moisture and has antimicrobial activity lasting up to 5 days
-
Compresses — aluminum acetate (Burow's solution) 1:40, dilute vinegar (¼ cup white vinegar + ¾ cup water), or wet tea bags applied for 5–10 min to weeping/moist areas; follow with cool blow-drying
-
Zinc oxide paste — excellent barrier, especially if urine or fecal soiling is a factor
-
Air conditioning where possible in hot/humid climates
-
Andrews' Diseases of the Skin, p. 314; Tintinalli's Emergency Medicine, p. 1696
2. Topical Pharmacological Treatment
| Situation | Treatment |
|---|---|
| Simple intertrigo (no infection) | Antiperspirants/drying agents (aluminium chloride); consider 1% hydrocortisone cream for inflammation — short course only |
| Fungal superinfection (Candida or dermatophyte) | Topical antifungals BID: ketoconazole 2%, clotrimazole 1%, miconazole 2%, or nystatin powder — until rash resolves |
| Bacterial superinfection | Topical mupirocin or fusidic acid; if spreading, oral antibiotics covering Staphylococcus/Streptococcus (e.g., cefalexin, amoxicillin-clavulanate) |
| Inflammation + infection | Combine low-potency topical steroid (hydrocortisone) with an antifungal — never steroid alone |
| Erythrasma (Corynebacterium) | Topical erythromycin or oral erythromycin/clarithromycin |
⚠️ Steroid caution: Use only low-potency steroids (1% hydrocortisone) in flexural areas — stronger steroids cause skin atrophy and striae in the already thin epidermis of folds. Limit to 1–2 weeks. - StatPearls: Intertrigo
3. Oral Treatment (Resistant/Recurrent Cases)
- Oral fluconazole 100–200 mg daily for 7 days — for resistant fungal infections
- For recurrent candidal intertrigo: weekly fluconazole prophylaxis has evidence for prevention
- Castellani paint (fuchsin-based antiseptic) — useful adjunct for weepy, infected folds
4. Novel/Refractory Options
- Botulinum toxin type A injected into predisposed areas — dries out the fold, reduces hyperhidrosis, prevents recurrent intertrigo in patients with inguinal hyperhidrosis
- Moisture-wicking silver textiles (e.g., InterDry Ag) — evidence from case series for complicated intertrigo
- Andrews' Diseases of the Skin, p. 314
Prevention (Stopping Recurrence)
- Wear loose-fitting, breathable underwear — cotton or moisture-wicking fabrics; change after exercise
- Daily cleansing with a mild pH-balanced cleanser; dry the fold completely (hairdryer on cool)
- Maintain healthy weight — obesity is the strongest risk factor
- Control diabetes — hyperglycemia feeds Candida
- Antifungal powder (miconazole or nystatin powder) prophylactically in high-risk individuals
- Avoid prolonged use of topical steroids
When to Refer / Red Flags
- No improvement after 2–3 weeks of treatment → dermatology referral
- Signs of cellulitis (spreading redness, warmth, fever) → systemic antibiotics urgently
- Suspected hidradenitis suppurativa (recurrent painful nodules/sinuses)
- Hidden ulcers developing in skin folds → risk of sepsis
- Diagnosis uncertain — KOH/fungal culture, or skin biopsy may be needed
Key takeaway: Most groin rashes from sweating and tight clothing are intertrigo ± secondary candidal/bacterial infection. The cornerstone of treatment is keeping the area dry and cool, wearing loose clothing, and applying topical antifungals when infection is suspected — with a brief course of low-potency steroids only when significant inflammation is present.
This is a shared conversation. Sign in to Orris to start your own chat.