Cytokines
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Loading Image
Loading Image
I now have comprehensive material from Roitt's Essential Immunology, Robbins Basic Pathology, and Medical Microbiology. Here is a thorough overview of cytokines.
Cytokines
Definition
Cytokines are structurally diverse polypeptides that function as messenger molecules, communicating signals from one cell type to another. They instruct target cells to proliferate, differentiate, secrete additional cytokines, migrate, or undergo apoptosis. Cytokines signal via high-affinity plasma membrane receptors and are typically active at very low (nanomolar–picomolar) concentrations. - Roitt's Essential Immunology, p. 245
General Properties
| Property | Detail |
|---|---|
| Nature | Secreted polypeptides (also membrane-anchored forms exist, e.g., TNF) |
| Action range | Primarily autocrine (act on the producing cell) and paracrine (act on neighboring cells); rarely endocrine |
| Concentration | Active at nanomolar (10⁻⁹) to picomolar (10⁻¹²) ranges |
| Specificity | High affinity and specificity for cognate receptors |
| Regulation | mRNA instability (AU-rich 3'-UTR sequences), decoy receptors, receptor antagonists |
Cytokines act in hierarchical cascades — some (TNF, IL-1 family) exert powerful systemic "upstream" effects generating dozens of additional inflammatory mediators, while others (IL-2, IL-4, IL-12) have more restricted downstream effects on specific cell types.
Classification
1. Interleukins (IL-1 to IL-38)
The most important cytokine grouping; mediators of communication between leukocytes. Members belong to diverse structural classes — membership is defined by biological activity on leukocytes, not structural homology. ~37 interleukins described.
2. By Immune Response Role
| Category | Key Examples | Main Source | Function |
|---|---|---|---|
| Innate immune cytokines | TNF, IL-1, IL-6, IL-12, IFN-γ, type I IFNs, chemokines | Macrophages, DCs, NK cells, endothelial/epithelial cells | Induce inflammation, fever, inhibit viral replication |
| Adaptive immune cytokines | IL-2, IL-4, IL-5, IL-17, IFN-γ | CD4⁺ T lymphocytes | Lymphocyte proliferation, differentiation, effector activation |
| Immunosuppressive/regulatory | TGF-β, IL-10 | Treg cells, macrophages | Limit and terminate immune responses |
| Colony-stimulating factors | IL-3, IL-7, G-CSF, GM-CSF | Marrow stromal cells, T cells, macrophages | Stimulate hematopoiesis, increase leukocyte production |
| Chemokines | CXCL8 (IL-8), CCL2 (MCP-1), RANTES | Innate immune cells | Chemotaxis — direct cell migration to infection/injury sites |
- Robbins & Kumar Basic Pathology, p. 162
Key Proinflammatory Cytokines
The "big three" proinflammatory (acute-phase) cytokines are TNF-α, IL-1, and IL-6, produced primarily by activated macrophages. - Medical Microbiology 9e, p. 79
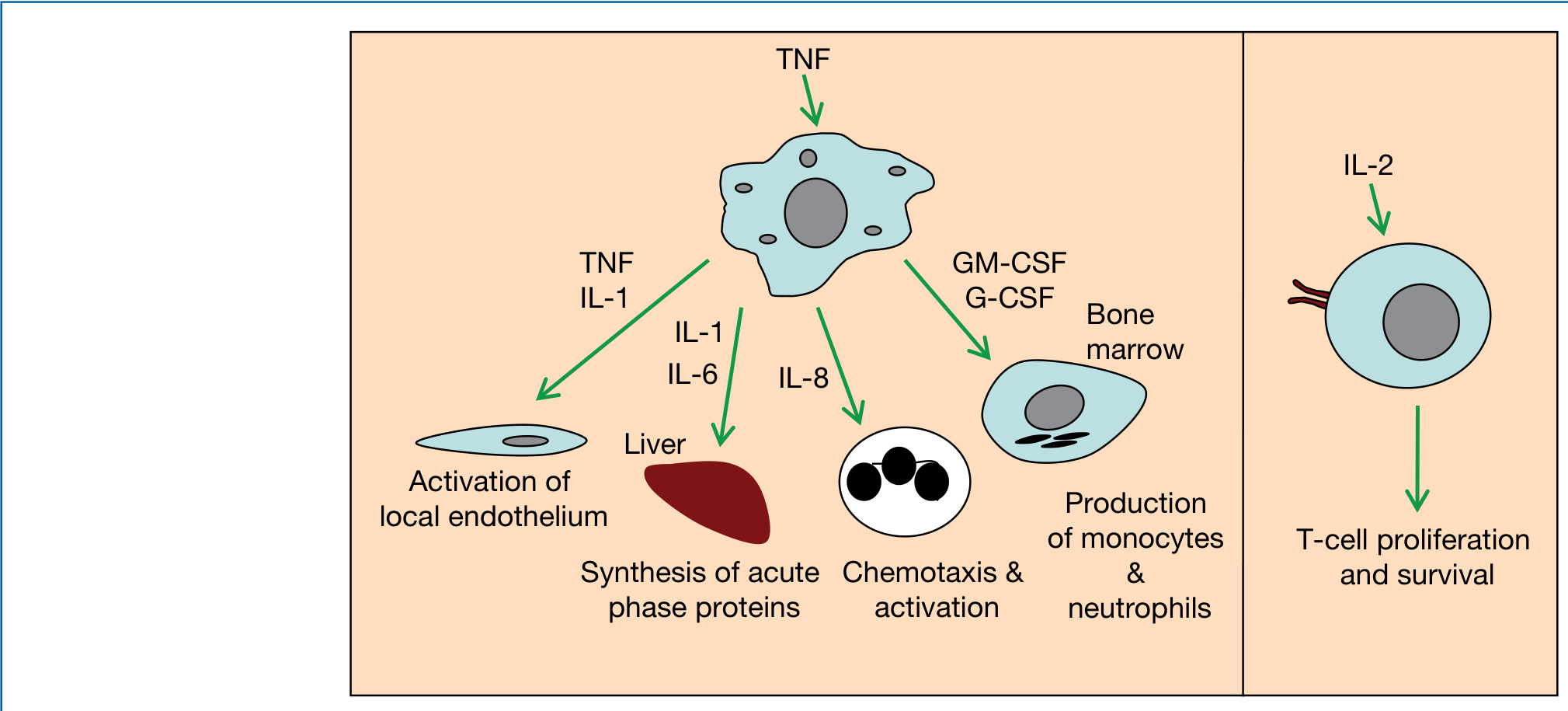
TNF-α
- The "ultimate mediator of inflammation"
- Induces expression of adhesion molecules and chemokines on endothelium
- Activates neutrophils and macrophages; promotes apoptosis in certain cells
- Loosens endothelial tight junctions → diapedesis
- Systemically: fever (hypothalamic action), cachexia, acute-phase protein synthesis by liver
- At high concentrations → septic shock
- Also upregulates production of IL-1, IL-6, and chemokines
IL-1 (α and β)
- Produced by macrophages, neutrophils, epithelial and endothelial cells
- IL-1β requires cleavage by the inflammasome to become active
- Endogenous pyrogen; promotes local and systemic inflammation
- Growth factor (unlike TNF, cannot induce apoptosis alone, insufficient to cause septic shock)
IL-6
- Produced by many cell types
- Stimulates acute-phase protein synthesis in the liver
- Promotes neutrophil production in bone marrow
- Activates T and B lymphocytes
IL-12 and IL-23
Both share a p40 subunit (IL-12 also has p35; IL-23 also has p19):
- IL-12: promotes NK-cell function; required for Th1 responses (enhances macrophage activation)
- IL-23: promotes Th17 responses from memory T cells (enhances neutrophil action)
Chemokines
A specialized subfamily (~8–10 kDa) primarily directing leukocyte migration. Classified by cysteine arrangement:
| Class | Example | Receptor | Main function |
|---|---|---|---|
| CXC | CXCL8 (IL-8) | CXCR1/2 | Neutrophil recruitment |
| CC | CCL2 (MCP-1/MCP-1) | CCR2 | Macrophage recruitment |
| CC | CCL5 (RANTES) | CCR1/3/5 | T cell, NK cell, eosinophil recruitment |
Functional classes:
- Inflammatory chemokines: inducibly expressed, rapidly evolving, promiscuous (bind multiple receptors), coordinate innate/adaptive cell migration to infection sites
- Homeostatic chemokines: constitutively expressed, highly conserved, guide immune cells to correct body compartments under non-infectious conditions (e.g., T cells to lymph nodes, B cells to follicles)
Cytokine Receptors
Six major receptor superfamilies exist. The most important for signaling are:
Hematopoietin (type I/II) receptors — operate through shared signaling subunits (γc, βc, or gp130), mediating hetero- or homodimer formation upon cytokine binding. These couple to the JAK–STAT pathway.
Signal Transduction: JAK–STAT Pathway
The canonical cytokine signaling pathway:
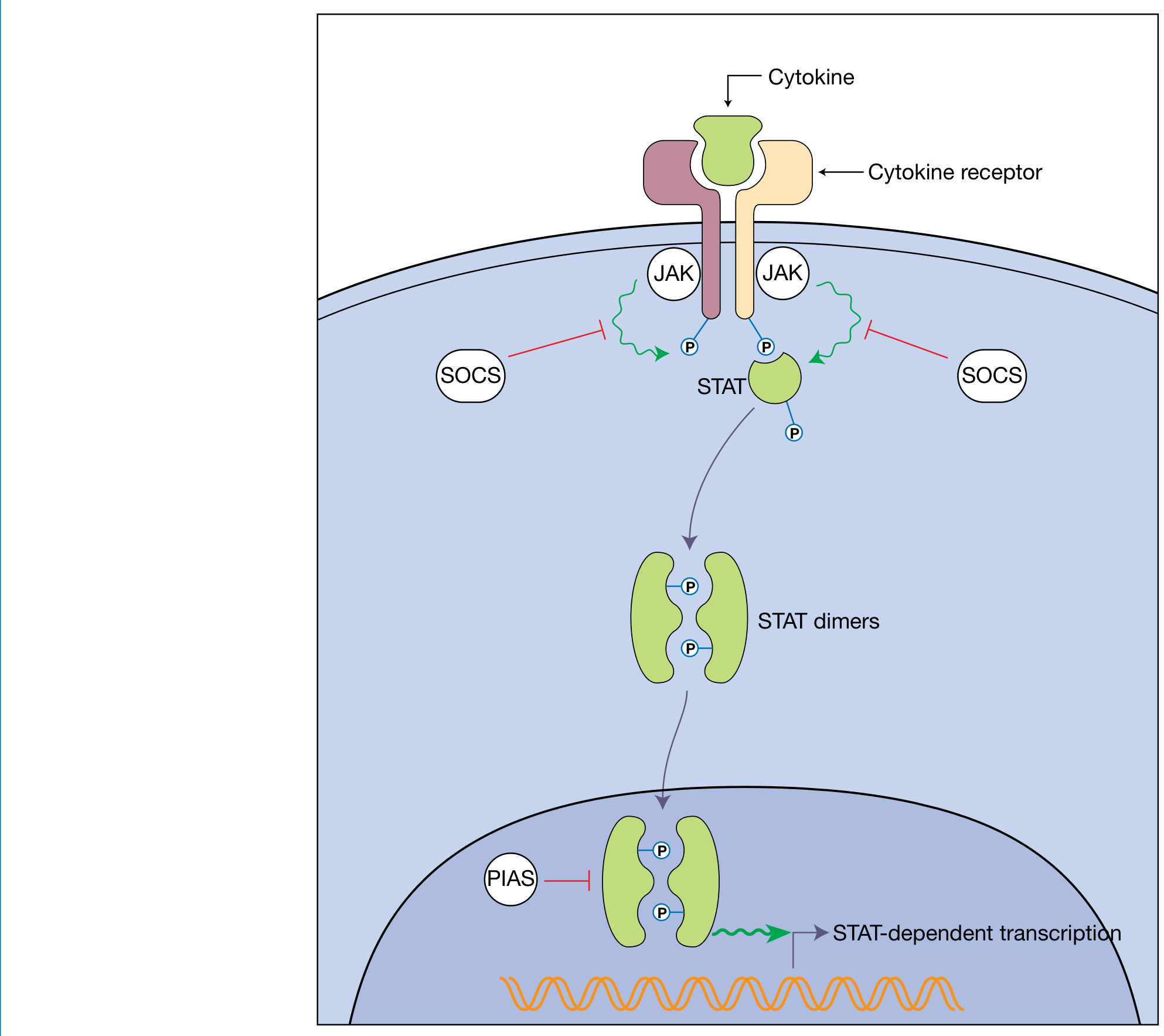
- Cytokine binds to its receptor → receptor dimerization/oligomerization
- JAKs (constitutively associated with receptor cytoplasmic tails) are brought into proximity → reciprocal phosphorylation → JAK activation
- Active JAKs phosphorylate tyrosine residues on receptor cytoplasmic tails → docking sites created
- STATs (cytoplasmic transcription factors with SH2 domains) are recruited, phosphorylated by JAKs
- Phosphorylated STATs dimerize, dissociate from receptor, translocate to nucleus
- STAT dimers activate transcription of target genes
4 JAKs (JAK1, JAK2, JAK3, TYK2) and 7 STATs (STAT1–6, including STAT5a/b) exist, engaged in distinct, non-redundant combinations by different cytokines.
Negative regulation:
- SOCS proteins (8 members: CIS, SOCS1–7): STAT-induced feedback inhibitors — directly inhibit JAK kinase activity or promote JAK ubiquitination and proteasomal degradation
- PIAS proteins: block STAT binding to DNA or recruit transcriptional co-repressors
JAKs also signal through Ras-MAP kinase and PI3K–PLCγ pathways. - Roitt's Essential Immunology, p. 256
Cytokines in Pathology and Therapeutics
| Condition | Cytokine Involvement | Therapeutic Relevance |
|---|---|---|
| Septic shock | Massive overproduction of TNF, IL-1 | Anti-TNF biologics |
| Rheumatoid arthritis | TNF-α, IL-1, IL-6, IL-12, IL-15, IL-18, IL-23 from synoviocytes | TNF antagonists (dramatically effective) |
| Inflammatory bowel disease | IL-1, TNF, IL-6, IL-8 via NF-κB | Anti-TNF, anti-IL-12/23 (ustekinumab) |
| Hematopoietic reconstitution | G-CSF, GM-CSF, IL-3, IL-7 | Administered after stem cell transplantation |
| Viral immunity | Type I IFNs (IFN-α, IFN-β) | Antiviral therapy |
"Inhibiting cytokine production or actions can control the harmful effects of inflammation. Patients with rheumatoid arthritis often show dramatic responses to TNF antagonists." — Robbins & Kumar Basic Pathology, p. 162
Summary Table of Key Cytokines
| Cytokine | Source | Major Actions |
|---|---|---|
| TNF-α | Macrophages, T cells | Inflammation, fever, cachexia, septic shock, endothelial activation, apoptosis |
| IL-1α/β | Macrophages, keratinocytes, endothelium | Fever, acute-phase response, T cell activation (IL-1β: inflammasome-activated) |
| IL-2 | CD4⁺ T cells | T-cell proliferation, survival |
| IL-4 | CD4⁺ Th2 cells | B-cell activation, IgE class switching, Th2 differentiation |
| IL-5 | Th2 cells | Eosinophil production and activation |
| IL-6 | Many cell types | Acute-phase proteins, B-cell differentiation, hematopoiesis |
| IL-8 (CXCL8) | Macrophages, endothelium | Neutrophil chemotaxis |
| IL-10 | T cells, macrophages | Anti-inflammatory, limits immune responses |
| IL-12 | Macrophages, DCs | NK/T-cell activation, Th1 polarization |
| IL-17 | Th17 cells | Neutrophil recruitment, mucosal defense |
| IFN-γ | T cells, NK cells | Macrophage activation, antiviral, Th1 promotion |
| TGF-β | Many cell types | Immunosuppression, fibrosis, Treg induction |
| G-CSF / GM-CSF | Marrow stroma, T cells | Hematopoiesis — granulocyte/monocyte production |
Sources: Roitt's Essential Immunology (Essentials), pp. 245–256 | Robbins & Kumar Basic Pathology, pp. 162–163 | Medical Microbiology 9e, pp. 79–80
This is a shared conversation. Sign in to Orris to start your own chat.