describe GI system clinical examination in detail
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Searching Images
abdominal examination quadrants anatomy regions
Searching Images
liver palpation percussion hepatomegaly splenomegaly clinical signs
Loading Image
Loading Image
Loading Image
Here is a comprehensive, structured account of the GI system clinical examination, drawn from Yamada's Textbook of Gastroenterology, Goldman-Cecil Medicine, Harrison's Principles of Internal Medicine, and Sleisenger & Fordtran's Gastrointestinal and Liver Disease.
GI System Clinical Examination
1. History Taking
A thorough history precedes and directs every step of the examination.
Chief Complaint & Character of Symptoms
Pain is the most common GI complaint. Characterize it using SOCRATES:
- Site: Localizes to a quadrant (e.g., RUQ → biliary/hepatic, RLQ → appendix/ileocecal, LLQ → sigmoid/colon, epigastric → gastric/duodenal/pancreatic)
- Onset: Sudden ("bolt of lightning") suggests perforation or vascular catastrophe; insidious suggests inflammation or neoplasm
- Character: Crampy/colicky (hollow viscus — bowel obstruction, biliary colic), burning (PUD, GERD), tearing (aortic dissection), dull/aching (solid organ)
- Radiation: To the right shoulder (biliary/diaphragmatic); to the back (pancreatitis, AAA); to the groin (ureteral colic)
- Severity & Timing: Constant vs. episodic; relationship to meals (biliary pain after fatty foods; duodenal ulcer relieved by eating; gastric ulcer or mesenteric ischemia worsened by eating)
- Exacerbating/relieving factors: Peritonitis → patient lies still; visceral pain (renal colic, early appendicitis) → patient writhes
Associated Symptoms
- Nausea & vomiting: Clear vomitus → gastric outlet obstruction; feculent vomitus → distal small bowel or colonic obstruction
- Dysphagia/odynophagia: Points to esophageal pathology
- Anorexia, weight loss: Suggest malignancy, chronic inflammation, malabsorption
- Bowel habit changes: Diarrhea, constipation, tenesmus, hematochezia, melena, steatorrhea
- Jaundice, dark urine, pale stools: Biliary obstruction or hepatocellular disease
- Fever, chills, night sweats: Infectious or inflammatory process
- Flatulence, bloating: Malabsorption, IBS, bacterial overgrowth
Past Medical & Drug History
Prior abdominal surgeries, IBD, PUD, renal calculi, pelvic inflammatory disease — all suggest recurrence. Systemic illnesses (scleroderma, SLE, sickle cell, porphyria) may have GI manifestations. Chronic NSAID or antacid use suggests PUD.
Family & Social History
Alcohol and tobacco use (pancreatitis, hepatic cirrhosis, GI malignancies); family history of colorectal cancer, inflammatory bowel disease, or metabolic liver disease (hemochromatosis, Wilson's disease, α1-antitrypsin deficiency).
2. General Inspection
Before touching the patient, observe:
- General appearance: Pallor (anemia from GI blood loss), cachexia (malignancy, malabsorption), jaundice
- Posture and movement: A patient lying absolutely still, guarding the abdomen → peritonitis; a patient writhing → visceral/colic pain. Gentle shaking of the bed elicits sharp pain in peritonitis but not visceral pain
- Vital signs: Hemodynamic instability (hypotension, tachycardia) → urgent surgical cause (perforated viscus, ruptured AAA, hemorrhage). Tachypnea may indicate metabolic acidosis (DKA, mesenteric ischemia)
- Breathing pattern: Shallow, rapid breathing → intraabdominal sepsis or peritonitis
3. Peripheral Signs (Hands to Toes)
GI disease, especially hepatic, leaves fingerprints throughout the body before the abdomen itself shows gross changes.
| Sign | Significance |
|---|---|
| Leukonychia (white nails) | Hypoalbuminaemia, advanced liver disease |
| Clubbing | IBD (Crohn's, UC), cirrhosis, GI lymphoma |
| Dupuytren's contracture | Alcoholic liver disease |
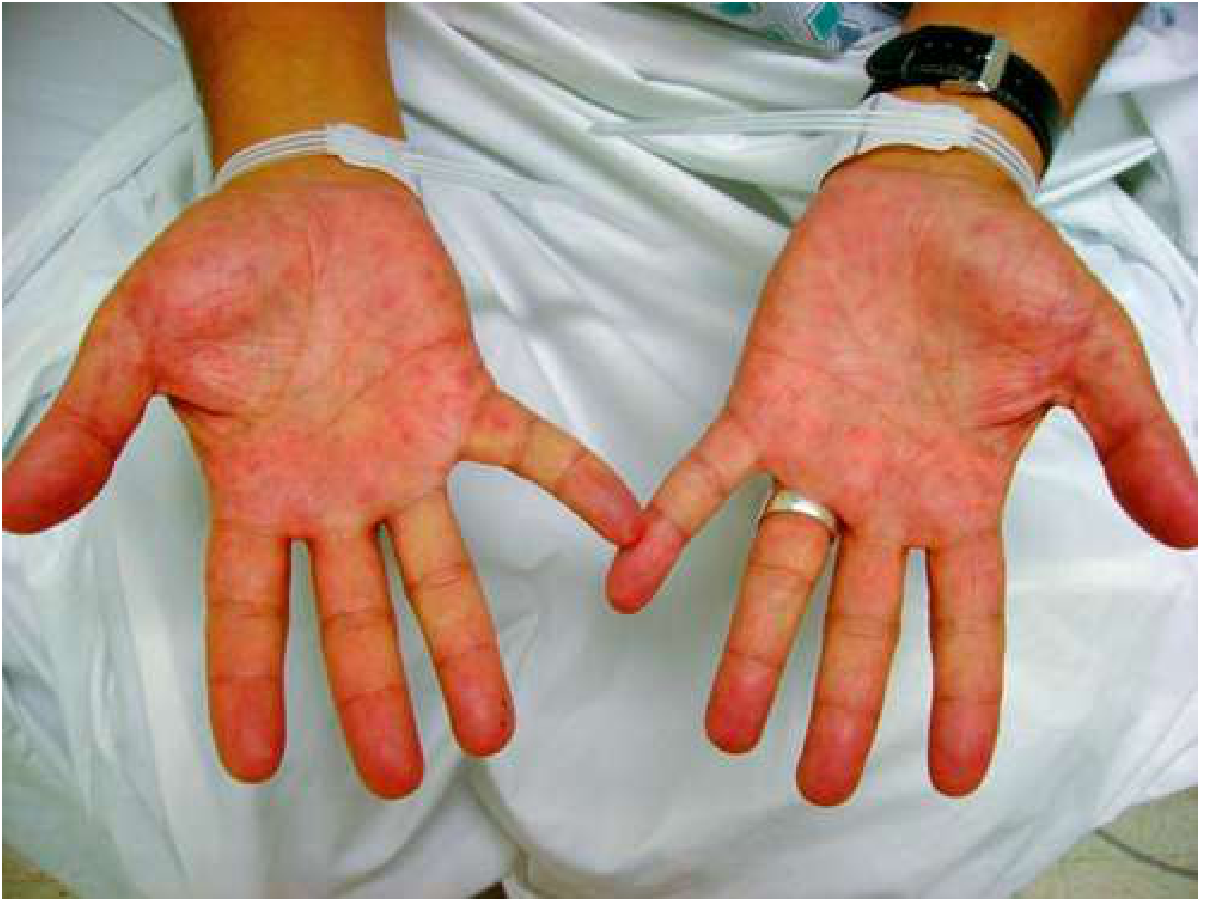
| Palmar erythema | Liver disease, pregnancy |
| Asterixis (liver flap) | Hepatic encephalopathy |
| Spider naevi | Liver disease (>5 significant; fill from center outward; only on arms, face, upper torso) |
| Parotid enlargement | Alcoholic liver disease |
| Icterus (jaundice) | Best seen in the sclera under natural light; detectable when bilirubin >43 μmol/L (2.5 mg/dL); in dark-skinned patients, inspect sublingual mucous membranes |
| Gynecomastia, testicular atrophy | Hyperestrogenemia from cirrhosis (especially alcoholic) |
| Scratch marks | Pruritus from cholestatic liver disease |
| Petechiae, ecchymoses | Impaired clotting factor production, hypersplenism |
| Peripheral edema | Hypoalbuminaemia, portal hypertension |
| Lymphadenopathy | Virchow's node (left supraclavicular) → upper GI malignancy; Sister Mary Joseph nodule (periumbilical) → intra-abdominal malignancy |
Palmar erythema — a classic peripheral sign of liver disease:
4. Abdominal Examination
The patient should be supine with hips and knees slightly flexed (to relax the abdominal wall), arms at the sides. The abdomen should be exposed from the nipple line to the thighs. The examiner should be at the patient's right side.
The classic sequence is: Inspection → Auscultation → Percussion → Palpation (auscultation before percussion/palpation avoids disturbing bowel sounds).
4.1 Inspection
Inspect systematically, looking for:
- Abdominal distension: The 6 Fs — Fat, Fluid (ascites), Flatus, Faeces, Foetus, Fibroid/mass; or the catastrophic 7th — Fatal (obstruction/volvulus)
- Surgical scars: Location suggests prior procedures; may hint at adhesion-related obstruction
- Dilated veins (caput medusae): Periumbilical venous engorgement radiating outward implies recanalization of the umbilical vein in portal hypertension
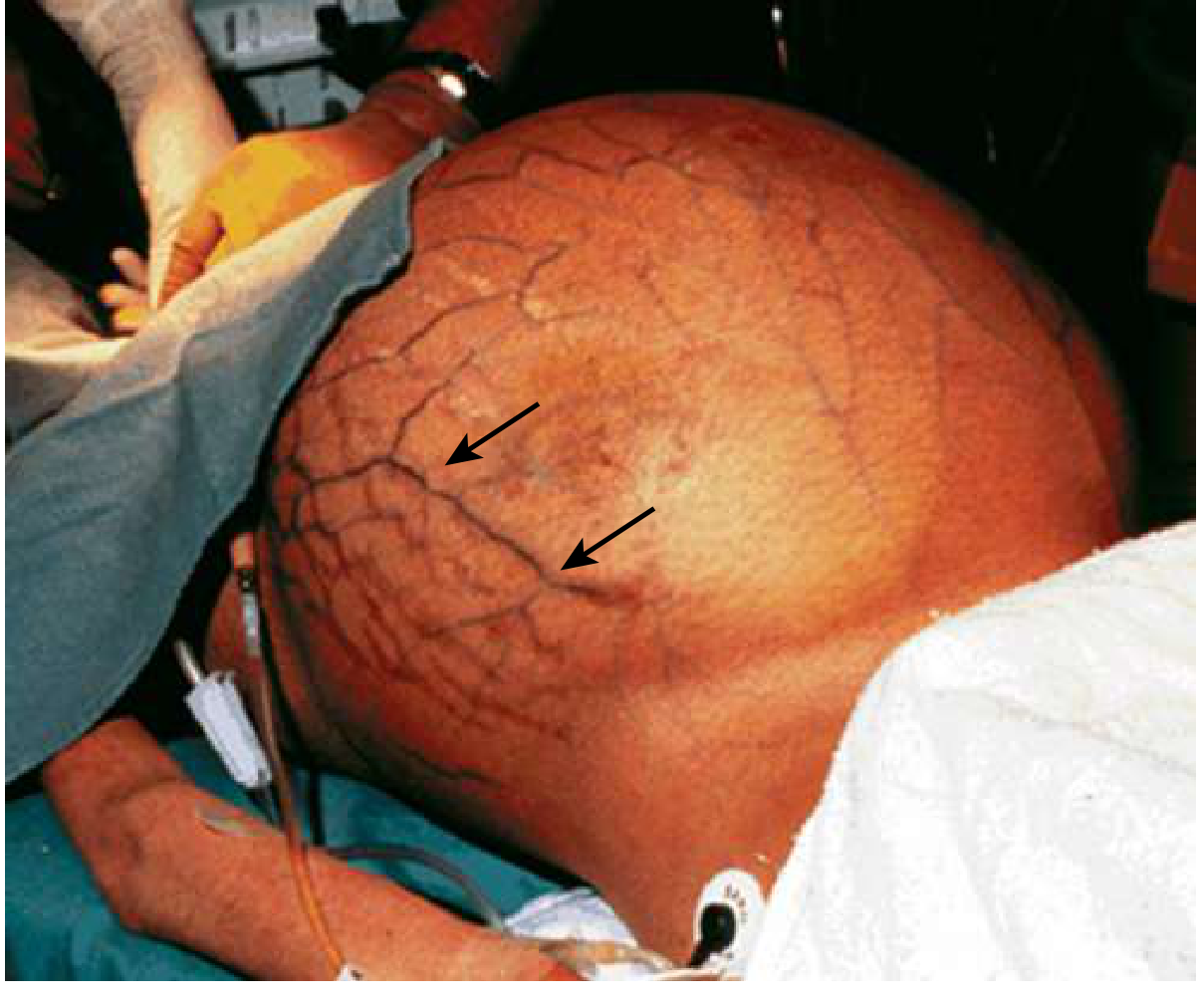
- Skin findings: Herpes zoster (dermatomal vesicles suggesting zoster affecting T6–T12); striae (Cushing's syndrome, rapid weight gain); jaundiced skin
- Cullen's sign: Periumbilical ecchymosis → retroperitoneal hemorrhage (e.g., acute hemorrhagic pancreatitis, ruptured AAA)
- Grey-Turner's sign: Flank ecchymosis → same causes as Cullen's
- Visible peristalsis: Suggests gastric outlet obstruction or small bowel obstruction (ladder pattern)
- Pulsatile mass in epigastrium: Suggests AAA
- Umbilical hernias: Often present in long-standing ascites
Gross ascites — marked abdominal distension due to fluid accumulation:
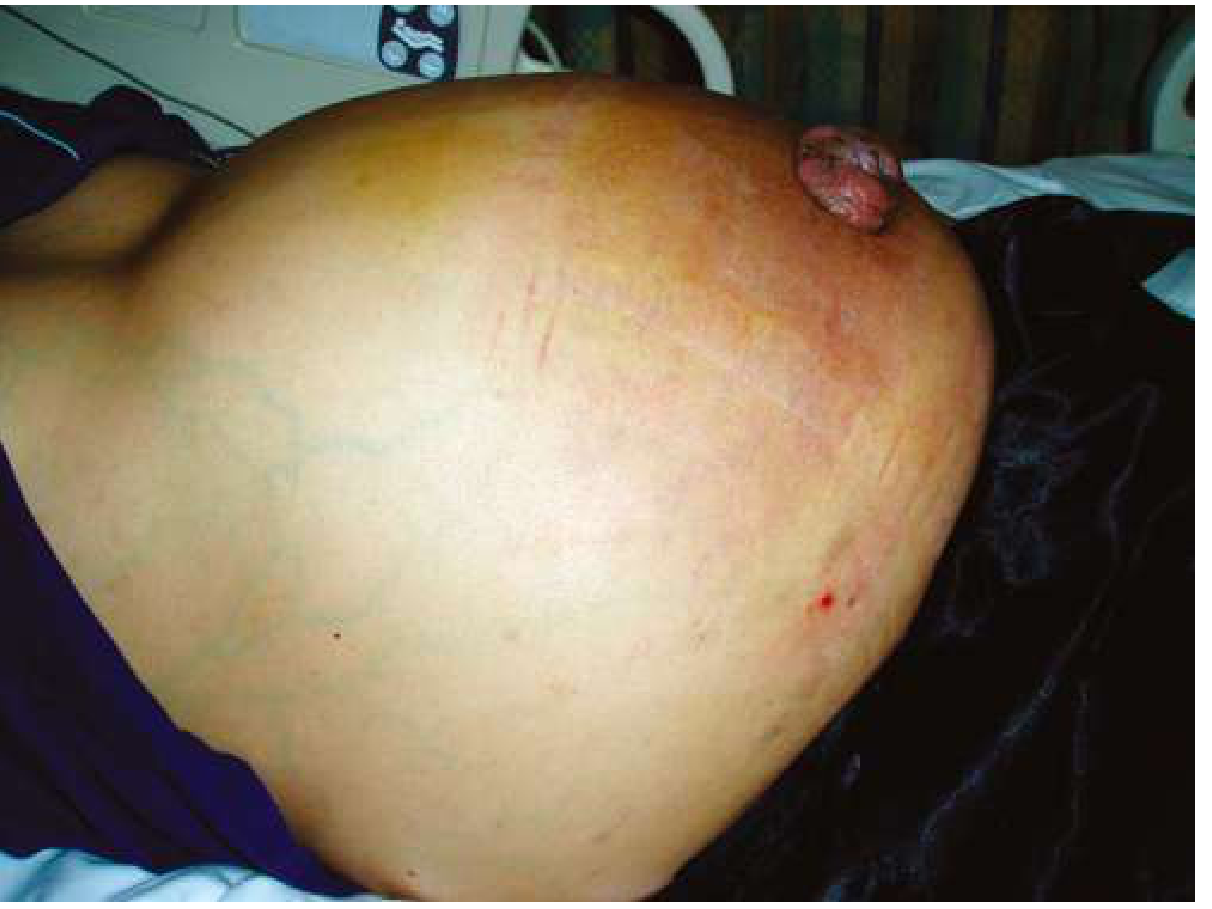
4.2 Auscultation
Auscultate before percussion and palpation on the undisturbed abdomen.
- Normal bowel sounds: Intermittent, low-pitched gurgles every 5–15 seconds
- Absent bowel sounds: Listen for at least 2 minutes in more than one quadrant before declaring silent. Complete absence → peritonitis or adynamic (paralytic) ileus
- High-pitched, rushing, hyperactive sounds synchronous with crampy pain → mechanical small bowel obstruction (the "borborygmi" or "tinkling" of obstruction)
- Bruit over the aorta/renal arteries: Vascular stenosis, AVM
- Succussion splash: Splashing sound on shaking the patient → gastric outlet obstruction (retained fluid in stomach)
- Stethoscope palpation trick: Press the stethoscope gently onto an area of suspected tenderness while appearing to auscultate — notable discrepancy with manual palpation suggests functional/non-organic pain
4.3 Percussion
Percussion precedes deep palpation and is less painful than rebound testing for peritonitis.
General abdomen:
- Tympany (resonance): Air-filled bowel — normal over most of abdomen
- Dullness: Solid organ or fluid
Peritonitis detection: Sharp pain on gentle percussion is the preferred method of detecting peritoneal irritation — it is as sensitive as rebound tenderness but significantly less painful for the patient.
Abdominal distension differentiation:
- Tympanic throughout → gaseous distension (obstruction, ileus, aerophagia)
- Dullness in flanks (flank dullness) → ascites (highest sensitivity at 94%)
Ascites — shifting dullness:
- Patient supine — percuss from midline toward the right flank until dullness is detected (the air-fluid interface)
- Mark the spot; ask the patient to roll toward you (lateral decubitus)
- Re-percuss at the same spot — if now tympanic, shifting dullness is confirmed (fluid has moved with gravity)
- Repeat on the other side for confirmation
- Shifting dullness is the most sensitive clinical sign for ascites; its absence reliably rules it out
Fluid wave (fluid thrill):
- Place the ulnar border of an assistant's hand firmly on the abdomen's midline (to dampen transmission through the abdominal wall)
- Tap one lateral flank sharply — the transmitted wave is felt by the examiner's other hand on the opposite flank
- Positive fluid wave has highest specificity for ascites among bedside signs
- Positive predictors (in order of sensitivity): flank dullness 94%, shifting dullness, fluid wave
Liver percussion:
- Liver is dull on percussion
- Percuss the right upper quadrant from above (noting upper border of liver dullness, normally ~5th intercostal space) and from below (ascending from RLQ until dullness is reached)
- Liver span in the mid-clavicular line: normally 6–12 cm
- Diminished span → cirrhosis (shrunken liver) or free gas (perforated viscus produces loss of liver dullness)
- Increased span → hepatomegaly (congestion, infiltration, malignancy, NAFLD)
Spleen percussion:
- Dullness to percussion between the 9th and 11th ribs in the left midaxillary line suggests splenomegaly
- Normally, the left midaxillary line is tympanic (gastric air bubble)
- Traube's space (6th rib above, midaxillary line laterally, left costal margin below): dullness here suggests splenomegaly or pleural effusion
Bladder: Suprapubic dullness → urinary retention, pelvic mass
4.4 Palpation
Technique: Position the patient with knees and hips flexed. Examiner's hand warm, fingers flat. Begin in the quadrant farthest from the site of maximum tenderness and move toward it. Start with light palpation (1–2 cm depth), progressing to deep palpation (4–5 cm) only if tolerated.
Light palpation:
- Detects superficial tenderness, guarding, skin hypersensitivity
- Guarding: Involuntary reflex increase in abdominal wall muscle tone, present throughout the respiratory cycle (vs. voluntary guarding, which relaxes during inspiration or with distraction)
- Rigidity: Severe form of involuntary guarding — "board-like" abdomen; indicates advanced peritonitis
- Pain with gentle percussion or light palpation → peritonitis
- The traditional rebound tenderness test (deep pressure then sudden release) should be abandoned — it causes unnecessary pain and is no more accurate than percussion for detecting peritonitis
Deep palpation:
- Detects organomegaly, masses, deep tenderness
- A pulsatile, tender epigastric mass → AAA
- Evaluate all hernial orifices (inguinal, femoral, umbilical) and surgical scars for incarcerated hernias
4.5 Organ-Specific Palpation
Liver
- Begin in the right lower quadrant and move upward toward the costal margin, so the edge is felt as you ascend on inspiration
- Normal liver edge: smooth, slightly tender, up to 2 cm below the right costal margin in thin individuals
- Hepatomegaly: Tender, enlarged, smooth → acute viral hepatitis, alcoholic hepatitis, hepatic congestion (right heart failure); Hard, irregular → cirrhosis; Multiple nodules → metastatic disease
- Scratch test: Bell of stethoscope over RUQ; scratch the skin moving from mid-abdomen toward the liver — amplified sound localizes the liver edge (useful when obesity or ascites obscures palpation)
- Ballot test / dipping method: In the presence of ascites, apply a quick downward pressure with fingertips below the costal margin to "ballot" the liver edge up through the fluid
Gallbladder
- Not normally palpable
- Murphy's sign: Place fingers under the right costal margin at the midclavicular line; ask the patient to take a deep breath — a positive sign is the patient abruptly stopping inspiration due to pain as the inflamed gallbladder descends onto the examiner's fingers; indicates acute cholecystitis (sensitivity ~65%, specificity ~87%)
- Courvoisier's law: A palpable, non-tender gallbladder in a jaundiced patient → malignant biliary obstruction (pancreatic head carcinoma), not cholelithiasis
Spleen
- Begin in the right lower quadrant and move diagonally toward the left costal margin (an enlarged spleen enlarges toward the RLQ)
- Normal spleen is not palpable; a palpable spleen tip = splenomegaly
- Ballotment: If not palpable, place one hand behind the left lower thorax and push forward; palpate anteriorly to feel the spleen between both hands
- Splenomegaly in chronic liver disease → portal hypertension; also seen in acute viral hepatitis, infiltrative disorders
- The splenic notch may be felt on its medial border, distinguishing it from other masses
Kidneys
- Bimanual palpation: one hand posteriorly in the renal angle, one anteriorly on the abdomen — "ballot" the kidney
- Normal kidneys are not palpable except in thin individuals
- Ballottable, enlarged kidneys → polycystic kidney disease, hydronephrosis, renal tumors
- Renal angle tenderness (CVAT): Fist percussion at the costovertebral angle → pain in pyelonephritis or perinephric abscess
4.6 Special Maneuvers
These have low sensitivity but high specificity — a positive result is diagnostically useful:
| Sign | Technique | Significance |
|---|---|---|
| Rovsing's sign | Deep palpation of LLQ causes pain in RLQ | Appendicitis |
| Psoas sign | Extend the right hip with the patient lying on the left side; pain on extension | Retrocecal appendicitis; inflamed psoas |
| Obturator sign | Flex and internally rotate right hip; pain in RLQ | Pelvic appendicitis |
| Carnett's sign | Tenderness increases with abdominal wall muscle contraction (patient lifts head) | Abdominal wall pain (not visceral) |
| Iliopsoas test | Pain on right hip flexion against resistance | Psoas abscess, appendicitis |
| Cough test | Localized abdominal pain elicited by coughing | Peritoneal irritation (sensitivity >78%, specificity 79–95%) |
5. Rectal Examination (Digital Rectal Examination, DRE)
The DRE is obligatory when GI bleeding is suspected (melena, unexplained anemia), in constipation, or when ano-rectal pathology is being evaluated.
Technique: Patient in left lateral decubitus position (Sims' position) or knee-elbow position. Inspect the perianal skin first (fissures, fistulae, hemorrhoids, condylomata, skin tags). Apply lubricant and gently insert gloved index finger.
Findings to assess:
- Anal sphincter tone: Decreased in neurological disease; increased in anal fissure (protective spasm)
- Rectal masses or polyps
- Stool character: Presence, consistency, color; test for occult blood (FOBT)
- Blood: Bright red (lower GI source) or melaenic stool (upper GI source)
- Prostate (in males): Size, tenderness, consistency — enlarged/nodular → carcinoma; tender → prostatitis
- Uterus/cervix (in females): Via vaginal/rectal palpation of the pelvis
- Peritoneal inflammation: "Hot Douglas" — exquisite tenderness on anterior wall of rectum (anterior pouch of Douglas) → pelvic peritonitis, pelvic abscess, perforated appendix
6. Completion of the Examination
The GI examination is incomplete without:
- Hernia orifices: Inguinal, femoral, umbilical, incisional
- Genitalia: Always examined in patients with acute abdominal pain; scrotal edema in ascites
- Chest examination: Rales and elevated JVP → right heart failure causing hepatic congestion; basal dullness → pleural effusion (hepatic hydrothorax)
- Cardiovascular: Atrial fibrillation → mesenteric arterial embolism
- Lymphadenopathy: Axillary, inguinal, Virchow's node (left supraclavicular) for GI malignancy
- Skin: Jaundice, scratch marks, ecchymoses, telangiectasias
7. Summary: Key Signs and Their Significance
| Clinical Finding | Likely Significance |
|---|---|
| Cullen's / Grey-Turner's sign | Retroperitoneal hemorrhage (pancreatitis, ruptured AAA) |
| Caput medusae | Portal hypertension |
| Shifting dullness + fluid wave | Ascites |
| Murphy's sign | Acute cholecystitis |
| Courvoisier's gallbladder | Malignant biliary obstruction |
| Rovsing's / Psoas / Obturator sign | Appendicitis |
| Board-like rigidity | Perforation/peritonitis |
| Spider naevi + palmar erythema | Chronic liver disease |
| Asterixis | Hepatic encephalopathy |
| Virchow's node | Upper GI malignancy (Troisier's sign) |
| Liver span <6 cm | Cirrhosis (shrunken liver) |
| Liver span >12 cm | Hepatomegaly |
| Traube's space dullness | Splenomegaly |
Sources: Yamada's Textbook of Gastroenterology, 7th ed. | Goldman-Cecil Medicine, International Ed. | Harrison's Principles of Internal Medicine, 22nd ed. (2025) | Sleisenger & Fordtran's Gastrointestinal and Liver Disease, 11th ed.
what are the conditions increasing eosinophils list and explain with mnemonics shortly
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
I have comprehensive data. Now I'll compose the answer with mnemonics.
Conditions Causing Eosinophilia
Definition: Eosinophilia = blood eosinophils > 0.5 × 10⁹/L (>500/µL). Eosinophil production is driven by IL-5; migration is guided by eotaxin.
Master Mnemonic: "NAACP DIABETES"
(Each letter = a category)
| Letter | Category |
|---|---|
| N | Neoplasms (lymphoma, leukemia) |
| A | Allergic / Atopic conditions |
| A | Addison's disease (adrenal insufficiency) |
| C | Collagen vascular / Connective tissue diseases |
| P | Parasites (helminths mainly) |
| D | Drugs |
| I | Idiopathic (Hypereosinophilic syndrome) |
| A | Asthma & pulmonary eosinophilia |
| B | Blood disorders (myeloproliferative) |
| E | Eosinophilic GI / skin disorders |
| T | Transplant rejection |
| E | Endocrine (Addison's, pituitary) |
| S | Skin disorders (atopic dermatitis, eosinophilic fasciitis) |
Simpler Mnemonic: "CHINA PAD"
(Commonly used in clinical exams)
| Letter | Category | Examples |
|---|---|---|
| C | Collagen / Connective tissue | Eosinophilic granulomatosis with polyangiitis (EGPA/Churg-Strauss), SLE, PAN |
| H | Helminthic / Parasitic infections | Ascaris, Strongyloides, hookworm, Toxocara, Trichinella, Wuchereria |
| I | Idiopathic Hypereosinophilic Syndrome (HES) | Eos >1500/µL >6 months, end-organ damage |
| N | Neoplasms | Hodgkin lymphoma, T-cell lymphoma, myeloproliferative neoplasms, eosinophilic leukemia |
| A | Allergic / Atopic | Asthma, allergic rhinitis, atopic dermatitis, urticaria |
| P | Pulmonary eosinophilia | Löffler syndrome, eosinophilic pneumonia (acute/chronic), tropical pulmonary eosinophilia (TPE), ABPA |
| A | Addison's disease / Adrenal insufficiency | Cortisol normally suppresses eosinophils; its absence → eosinophilia |
| D | Drugs | NSAIDs, penicillin, cephalosporins, sulfonamides, phenytoin, allopurinol |
Detailed Category Breakdown
1. Parasites — "WASH" (most common worldwide cause)
Wuchereria bancrofti · Ascaris · Strongyloides · Hookworm
- Tissue-invasive helminths cause higher eosinophilia than luminal parasites
- Trichinella (muscle invasion), Toxocara (visceral larva migrans) → marked eosinophilia
- Protozoa: Dientamoeba fragilis, Isospora belli (rare)
2. Allergic / Atopic Diseases
- Asthma, allergic rhinitis, urticaria, atopic dermatitis
- Mechanism: IgE-mediated → IL-5 surge → eosinophil recruitment
3. Pulmonary Eosinophilia — "TALE"
Tropical pulmonary eosinophilia · Acute eosinophilic pneumonia · Löffler syndrome · Eosinophilic chronic pneumonia + ABPA
- Löffler syndrome: Transient pulmonary infiltrates + eosinophilia during larval lung migration
- TPE: Paroxysmal cough, bronchospasm, very high eosinophilia; caused by Wuchereria bancrofti
- ABPA (Allergic bronchopulmonary aspergillosis): Asthmatic + IgE ↑ + central bronchiectasis
4. Drugs
Common culprits: NSAIDs, penicillins, cephalosporins, sulfonamides, phenytoin, allopurinol, nitrofurantoin, gold
- Drug reaction with eosinophilia and systemic symptoms = DRESS syndrome
5. Neoplasms
- Hodgkin lymphoma and peripheral T-cell lymphoma: Paraneoplastic cytokine-driven eosinophilia
- Eosinophilic leukemia (FIP1L1-PDGFRA mutation): Clonal, responds to imatinib
- Myeloproliferative neoplasms, mastocytosis
- Solid tumors (lung, cervix, bladder): Advanced-stage paraneoplastic
6. Connective Tissue / Vasculitis
- EGPA (Churg-Strauss syndrome): Asthma + sinusitis + eosinophilia + small-vessel vasculitis
- PAN, SLE, RA
7. Idiopathic Hypereosinophilic Syndrome (HES)
- Eosinophils >1500/µL for >6 months + no secondary cause + end-organ damage (cardiac, neurologic, pulmonary)
- Subtypes: Myeloid (PDGFRA/B mutations) vs. lymphocytic vs. idiopathic
8. Addison's Disease (Adrenal Insufficiency)
- Cortisol normally promotes eosinophil apoptosis; its deficiency → accumulation
- Classic teaching: morning cortisol trough causes physiologic eosinophilia → exaggerated in Addison's
9. Skin Disorders
- Eosinophilic fasciitis, eosinophilic cellulitis (Wells syndrome), eosinophilic folliculitis, episodic angioedema with eosinophilia
10. GI Disorders
- Eosinophilic esophagitis, eosinophilic gastroenteritis, eosinophilic colitis
- IBD can have mild eosinophilia
11. Miscellaneous
- Transplant rejection
- Retroviral infections: HIV, HTLV-1
- Eosinophilia-myalgia syndrome: L-tryptophan ingestion (historical)
- Atheroembolic disease
- Interstitial nephritis
- Premature birth (neonatal eosinophilia — ~75% of low-birth-weight infants)
Degree of Eosinophilia: Quick Reference
| Degree | Count | Common Causes |
|---|---|---|
| Mild | 500–1500/µL | Allergies, drug reactions |
| Moderate | 1500–5000/µL | Parasites, asthma, EGPA |
| Severe / Hypereosinophilia | >5000/µL | HES, eosinophilic leukemia, helminthic infections |
Quick Recall Summary Mnemonic: "INDIA"
(For rapid exam recall — the 5 most tested causes)
| I | Infections (parasites — helminths) |
| N | Neoplasms (lymphoma, leukemia) |
| D | Drugs & DRESS |
| I | Idiopathic HES |
| A | Allergic / Atopic (asthma, rhinitis) |
Sources: The Washington Manual of Medical Therapeutics | Henry's Clinical Diagnosis & Management by Laboratory Methods | The Harriet Lane Handbook, 23rd ed. | Goldman-Cecil Medicine | Harrison's Principles of Internal Medicine, 22nd ed.
This is a shared conversation. Sign in to Orris to start your own chat.