Detail explain of ra vs os vs reactive arthritis vs gout vs pseudo gout
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
rheumatoid arthritis hand joints X-ray
Searching Images
gout tophus urate crystals podagra
Reading File
Searching Images
pseudogout CPPD calcium pyrophosphate crystals knee chondrocalcinosis
Searching Images
reactive arthritis keratoderma blenorrhagica sausage digit dactylitis
I have comprehensive data from all sources. Now I'll compile the full detailed comparison.
Arthritis Comparison: RA vs OA vs Reactive Arthritis vs Gout vs Pseudogout
1. Rheumatoid Arthritis (RA)
Pathophysiology
RA is a chronic systemic autoimmune inflammatory disease in which cellular and humoral immune mechanisms cause destruction of synovial tissue. The key steps:
- Genetic predisposition via HLA-DR (particularly HLA-DR4 "shared epitope") triggers an immune response against citrullinated self-proteins (e.g., citrullinated vimentin, fibrinogen)
- Activated T-cells, B-cells, and macrophages infiltrate the synovium → synovial lining cells and subsynovial vessels proliferate → forming pannus (invasive granulation tissue)
- Pannus secretes matrix metalloproteinases (MMPs) and cytokines (TNF-α, IL-1, IL-6) → cartilage and bone erosion
- Rheumatoid factor (RF) = IgM autoantibody against Fc portion of IgG; Anti-CCP antibodies = highly specific (95%) and appear years before symptoms
- TNF-α plays a central role → basis for biologic therapy
Epidemiology
- Prevalence: 1–2% of adults; peak onset 20–50 years
- Women:Men = 3:1 (estrogen effect); 70% have insidious onset
- Higher concordance in monozygotic twins (MHC class II gene influence)
Clinical Features
| Feature | Detail |
|---|---|
| Pattern | Symmetric polyarthritis |
| Joints affected | PIP, MCP, wrists (sparing DIP) → "MCP/wrist" hallmark |
| Morning stiffness | >1 hour (hallmark) |
| Onset | Insidious, weeks to months |
| Deformities | Swan-neck, boutonnière, ulnar deviation, Z-thumb |
| Extra-articular | Rheumatoid nodules (20–30%), scleritis, pleuritis, pericarditis, Felty syndrome, vasculitis, interstitial lung disease |
ACR 1987 Diagnostic Criteria (need ≥4 of 7; symptoms ≥6 weeks)
- Morning stiffness ≥1 hour
- Arthritis of ≥3 joint areas
- Arthritis of hand joints (PIP, MCP, wrist)
- Symmetric arthritis
- Rheumatoid nodules
- Positive RF
- Radiographic changes (erosions, juxta-articular osteopenia on X-ray)
Investigations
- RF positive: ~70–80% (not specific — can be positive in SLE, Sjögren, infections, elderly)
- Anti-CCP (anti-citrullinated peptide): highly specific (~95%), positive even in seronegative RF
- ESR/CRP: elevated (disease activity markers)
- Synovial fluid: WBC >2,000/mm³ (inflammatory), no crystals
- X-ray: juxta-articular osteopenia → joint space narrowing → erosions → deformities
Treatment
Goal: Treat to target (T2T); early aggressive DMARD therapy
- NSAIDs: symptomatic only, no disease modification
- Conventional DMARDs (csDMARDs):
- Methotrexate (MTX) — anchor drug, 15–25 mg/week; monitor LFTs, CBC
- Hydroxychloroquine (mild disease): 200 mg BID, ophthalmology follow-up
- Sulfasalazine: 2–3 g/day in divided doses
- Leflunomide
- Biologic DMARDs:
- Anti-TNF: etanercept, adalimumab, infliximab
- IL-6 inhibitors: tocilizumab
- Anti-CD20: rituximab
- Co-stimulation blocker: abatacept
- Glucocorticoids: bridge therapy or for flares (not long-term due to side effects)
- Surgery: joint replacement for end-stage disease
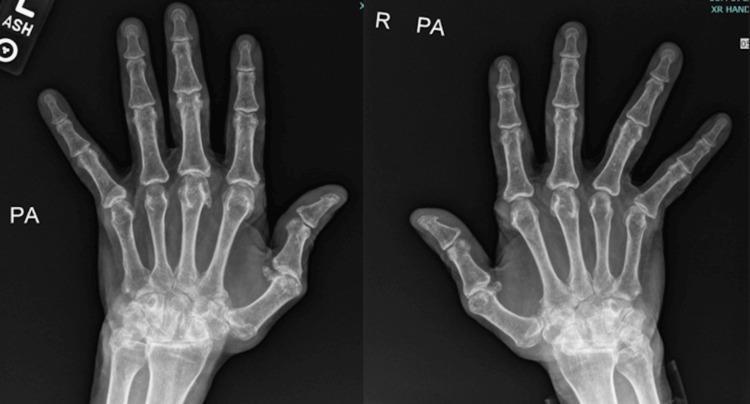
2. Osteoarthritis (OA)
Pathophysiology
OA is a degenerative (non-inflammatory) joint disease — the most common joint disease. Matrix breakdown exceeds synthesis:
- Mechanical stress + aging → chondrocyte dysfunction → reduced proteoglycan/collagen II production
- Subchondral bone remodeling → sclerosis + osteophyte formation
- Mild inflammation (synovitis) is secondary, driven by locally produced cytokines (IL-1β, IL-6), but NOT the primary pathology
- Risk factors: age, obesity, prior joint injury, repetitive use, female sex (post-menopause)
Clinical Features
| Feature | Detail |
|---|---|
| Pattern | Asymmetric or bilateral (weight-bearing joints + DIP/PIP of hands) |
| Joints affected | DIP > PIP (hands), 1st CMC, knees, hips, spine (sparing MCP/wrist) |
| Stiffness | <30 min (post-rest stiffness/"gelling"), worsens with use |
| Bony nodules | Heberden's nodes (DIP) and Bouchard's nodes (PIP) |
| No systemic features | No extra-articular manifestations |
| Crepitus | Joint crepitus on movement |
Investigations
- Labs: ESR, CRP, RF — all NORMAL (distinguishes from RA)
- Synovial fluid: non-inflammatory WBC < 2,000/mm³, clear/yellow
- X-ray (4 classic signs):
- Joint space narrowing (asymmetric)
- Osteophytes (bony spurs)
- Subchondral sclerosis
- Subchondral cysts (Mnemonic: "JOSS")
Treatment
- Non-pharmacological: weight loss, physiotherapy, exercise, orthotics
- Topical NSAIDs: first-line for knee/hand OA
- Oral NSAIDs: use cautiously (GI/renal risk)
- Intra-articular corticosteroids: short-term relief
- Intra-articular hyaluronic acid: modest benefit
- Duloxetine: for chronic pain component
- Surgery: osteotomy, joint replacement (TKR/THR)
- Note: No DMARDs — OA is not autoimmune; NSAIDs/physiotherapy remain cornerstone
3. Reactive Arthritis (ReA)
Definition & Pathophysiology
Reactive arthritis = aseptic arthritis triggered by an extra-articular infection (GI or GU tract), occurring 1–3 weeks after the infection. The joint itself is sterile.
- GI pathogens: Salmonella typhimurium, Yersinia enterocolitica, Shigella flexneri, Campylobacter jejuni
- GU pathogen: Chlamydia trachomatis (most common in developed countries)
- Mechanism: Bacterial antigens (fragments or even viable Chlamydia) traffic to the synovium → activate immune response → synovitis. PCR studies have found viable Chlamydia in joints in a metabolically altered state
- HLA-B27 strongly associated (found in 60–80% of cases) — B27 confers risk for onset, axial involvement, and chronicity
- Part of the seronegative spondyloarthropathy spectrum (RF negative)
- Affects 2–7% of those with triggering GI infection; up to 20% in B27-positive individuals
Clinical Features
Classic triad (Reiter's syndrome): "Can't see, can't pee, can't bend the knee"
- Arthritis: asymmetric oligoarthritis, lower extremity predominance (knee, ankle, MTP)
- Urethritis/cervicitis: dysuria, urethral discharge (cervicitis may be asymptomatic in women — leads to underdiagnosis)
- Conjunctivitis/uveitis: bilateral conjunctivitis (painful); acute anterior uveitis (unilateral, less painful)
Additional features:
- Dactylitis ("sausage digit"): diffuse swelling of an entire digit — pathognomonic of spondyloarthropathy
- Enthesitis: Achilles tendinitis, plantar fasciitis
- Keratoderma blennorrhagicum: painless hyperkeratotic papules/plaques on palms and soles — clinically identical to pustular psoriasis
- Circinate balanitis: painless shallow ulcerations on glans penis
- Oral painless ulcers
- Sacroiliitis: asymmetrical (vs. bilateral in AS)
- Nail dystrophy (pitting, onycholysis)
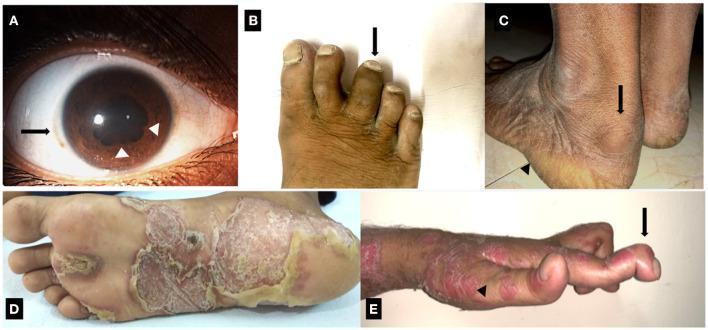
Investigations
- RF and ANA: negative (seronegative)
- HLA-B27: positive in majority
- ESR/CRP/WBC: elevated during acute phase
- Synovial fluid: inflammatory WBC; no crystals; culture negative (aseptic)
- STI screen: urethral/cervical swab for Chlamydia; stool cultures for GI pathogens
- X-ray: periostitis, new bone formation at entheses; asymmetric sacroiliitis (vs. symmetric in AS); "fluffy" periosteal reaction at calcaneus; bulky non-marginal syndesmophytes (vs. marginal in AS)
Treatment
- NSAIDs: first-line for arthritis symptoms (indomethacin preferred)
- Antibiotics: for active Chlamydia infection (doxycycline/azithromycin); little effect once arthritis established; prolonged antibiotics (3-month doxycycline/azithromycin) may benefit post-Chlamydia chronic ReA
- Intra-articular corticosteroids: for persistent monoarticular disease
- Sulfasalazine or MTX: for chronic/refractory cases (>6 months)
- Anti-TNF biologics: refractory/severe chronic disease
- Prognosis: Most resolve in 3–12 months; ~15% develop chronic arthritis; B27-positive patients more likely to develop ankylosing spondylitis
4. Gout
Pathophysiology
Gout = monosodium urate (MSU) crystal deposition disease due to hyperuricemia
- Uric acid is the end product of purine catabolism (humans lack uricase)
- 90% of patients: reduced renal excretion of uric acid
- 10%: overproduction of uric acid
- Triggers for acute attacks: dietary purines (red meat, shellfish), alcohol (especially beer — ethanol blocks renal urate excretion), dehydration, surgery, diuretics (thiazides, loop), aspirin, trauma
- MSU crystal formation occurs in cooler, more acidic environments → explains predilection for 1st MTP, heel, ankle
- Crystals → phagocytosed by neutrophils → activate NLRP3 inflammasome → IL-1β release → acute inflammatory cascade (neutrophil recruitment, prostaglandins, bradykinin)
Clinical Stages
| Stage | Features |
|---|---|
| Asymptomatic hyperuricemia | Elevated uric acid (>7 mg/dL men; >6 mg/dL women) with no symptoms; usually takes ≥20 years before first attack; treatment NOT recommended |
| Acute gouty arthritis | Sudden severe monoarthritis, peak within 24 hrs, resolves in days–weeks even untreated |
| Intercritical gout | Symptom-free periods between attacks; crystals still present in joints |
| Chronic tophaceous gout | Persistent tophi (chalky urate deposits) in joints, earlobes, Achilles tendon; can mimic RA |
Clinical Features
- 1st MTP joint (podagra) in 50% of initial attacks; eventually involved in 75–90%
- Also: heel, ankle, knee, midtarsal joints, olecranon bursa
- Severe pain, swelling, erythema, warmth — patient can't tolerate even bedsheet touching the joint
- Attacks often begin at night (↓ temperature, dehydration during sleep)
- Low-grade fever, leukocytosis may accompany severe attacks (can mimic septic arthritis)
- Tophi: chalky-white subcutaneous nodules; common sites = 1st MTP, olecranon bursa, ear helix, Achilles tendon
- Gout in women and elderly: often polyarticular, can mimic RA; tophi mistaken for rheumatoid nodules
Investigations
- Serum uric acid: usually >8 mg/dL during attack (can be normal during acute flare as uric acid redistributes)
- Synovial fluid (GOLD STANDARD): needle-shaped crystals with negative birefringence (yellow when parallel to compensator axis, blue when perpendicular) under polarized light; WBC 10,000–100,000/mm³; culture negative
- 24-hr urine uric acid: distinguishes underexcretion vs. overproduction
- X-ray (chronic gout): "rat-bite" erosions with overhanging edge (punched-out erosions with sclerotic margins), soft tissue tophi; periarticular calcification uncommon (contrast with pseudogout)
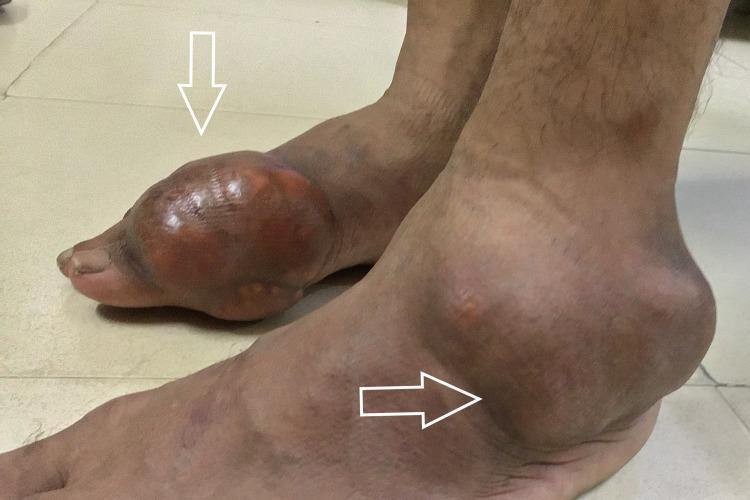
Treatment
Acute attack:
- NSAIDs (e.g., indomethacin 50 mg TID): first-line if no contraindications
- Colchicine: 1.2 mg then 0.6 mg 1 hr later (first 36 hours most effective); inhibits microtubule polymerization → inhibits neutrophil migration
- Corticosteroids: (oral, IM, or intra-articular) if NSAIDs/colchicine contraindicated; prednisone 0.5 mg/kg/day tapering over 7–10 days
- IL-1 inhibitors (anakinra, canakinumab): refractory/polyarticular attack
Urate-lowering therapy (ULT) — start when attack fully resolved:
- Indications: ≥2 attacks/year, tophi, uric acid nephropathy/stones, radiographic erosions
- Allopurinol (xanthine oxidase inhibitor): start low (100 mg/day), titrate; paradoxically can trigger attacks if started during active gout
- Febuxostat: alternative XOI, more potent; cardiovascular concerns in some guidelines
- Probenecid: uricosuric; second-line (avoid if GFR <50 or uric acid stones)
- Pegloticase (IV recombinant uricase): refractory tophaceous gout
- Target: serum uric acid <6 mg/dL (<5 mg/dL with tophi)
- Prophylaxis during ULT initiation: low-dose colchicine or NSAID for 3–6 months (mobilization flares)
5. Pseudogout (CPPD — Calcium Pyrophosphate Crystal Deposition Disease)
Pathophysiology
Pseudogout = calcium pyrophosphate dihydrate (CPPD) crystal deposition in hyaline cartilage and fibrocartilage:
- Degradation of articular cartilage proteoglycans (which normally inhibit mineralization) allows CPP crystallization around chondrocytes
- Crystals form in cartilage matrix → rupture → seed the joint → NLRP3 inflammasome activation → IL-1β → acute inflammation (like gout)
- Even without inflammation, crystals disrupt cartilage structure/function
- ANKH gene mutation: encodes inorganic pyrophosphate transporter — linked to familial CPPD
- Sporadic (idiopathic) vs. hereditary vs. secondary
Secondary CPPD causes (associated metabolic disorders):
- Hyperparathyroidism (↑ Ca²⁺)
- Hemochromatosis (↑ Fe²⁺ inhibits pyrophosphatase)
- Hypomagnesemia (Mg²⁺ normally inhibits CPP crystallization)
- Hypothyroidism
- Ochronosis (alkaptonuria)
- Diabetes mellitus
- Previous joint damage/trauma
Epidemiology
- Age: predominantly >50 years; prevalence rises sharply with age — up to 60% of those ≥85 years
- Equal sex distribution (vs. gout's male predominance)
- Often asymptomatic (incidental chondrocalcinosis on X-ray)
Clinical Features
| Presentation | Description |
|---|---|
| Acute pseudogout | Sudden monoarthritis — most commonly knee (then wrist, elbow, shoulder, ankle); mimics septic arthritis; lasts weeks to months (vs. days in gout) |
| Chronic CPPD | Persistent joint pain with superimposed flares — can mimic OA or RA |
| Chondrocalcinosis | Asymptomatic X-ray finding of cartilage calcification |
| Crowned dens syndrome | CPPD deposition around odontoid process → acute neck pain, fever, meningism |
- Unlike gout, CPPD commonly affects the knee (gout prefers 1st MTP)
- Large joint predominance: knee > wrist > shoulder > ankle
- Attacks may be triggered by: illness, surgery, trauma, IV contrast, bisphosphonates
Crystal Characteristics
| Feature | Gout (MSU) | Pseudogout (CPPD) |
|---|---|---|
| Shape | Needle-shaped | Rhomboid (0.5–5 μm) |
| Birefringence | Negatively birefringent | Positively birefringent (weakly) |
| Color under compensator | Yellow when parallel | Blue when parallel |
| Site of crystal formation | Periarticular (synovial fluid) | In hyaline cartilage / fibrocartilage |
| X-ray | "Rat-bite" erosions | Chondrocalcinosis (cartilage calcification) |
Investigations
- Synovial fluid: rhomboid crystals with weak positive birefringence (blue when parallel to axis under compensated polarized light); WBC 10,000–50,000/mm³
- X-ray: chondrocalcinosis — linear/punctate radiopaque calcifications in hyaline cartilage or fibrocartilage (knee menisci, wrist TFCC, symphysis pubis) — pathognomonic
- Ultrasound: hyperechoic deposits within the substance of hyaline cartilage (vs. gout's "double contour" sign on cartilage surface)
- Dual-energy CT (DECT): can color-code CPPD from MSU crystals
- Metabolic screen: calcium, PTH, magnesium, iron/ferritin, TFTs, blood glucose (for secondary causes)
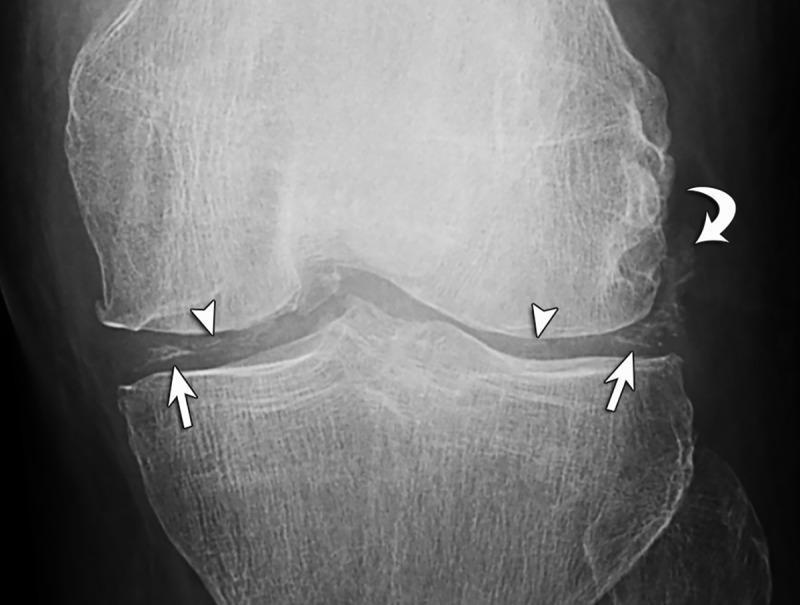
Treatment
Acute attack:
- NSAIDs: high-dose (indomethacin, naproxen)
- Colchicine: effective (same mechanism as gout)
- Intra-articular corticosteroids: excellent if septic arthritis ruled out and ≤2 joints involved; aspiration alone also provides symptomatic relief
- Systemic corticosteroids: polyarticular or contraindications to above
- IL-1 inhibitors: refractory cases
Chronic/prophylaxis:
- Low-dose colchicine (0.5–1 mg/day): reduces frequency of recurrent attacks
- Hydroxychloroquine or MTX: for chronic inflammatory CPPD mimicking RA
- No equivalent of ULT for CPPD: no treatment currently prevents or reverses crystal formation
Comprehensive Comparison Table
| Feature | RA | OA | Reactive Arthritis | Gout | Pseudogout |
|---|---|---|---|---|---|
| Mechanism | Autoimmune (anti-CCP, RF) | Mechanical degeneration | Post-infectious (sterile) | MSU crystal deposition | CPP crystal deposition |
| Age/Sex | 20–50 yrs, F>M (3:1) | >50 yrs, F>M | 20–40 yrs, M>F | 40–60 yrs M, post-menopausal F | >50 yrs, equal |
| Onset | Insidious, weeks | Gradual, years | Acute, 1–3 wks post-infection | Sudden (overnight), acute | Sudden, acute |
| Pattern | Symmetric polyarthritis | Asymmetric, weight-bearing | Asymmetric oligoarthritis LL | Mono → polyarthritis | Mono/oligoarthritis |
| Joints | PIP, MCP, wrist (sparing DIP) | DIP, PIP, knee, hip (sparing MCP) | Knee, ankle, MTP (LL predominance) | 1st MTP (podagra), ankle, knee | Knee > wrist, shoulder |
| Stiffness | Morning stiffness >1 hr | Morning stiffness <30 min (gelling) | Variable | Not a feature | Not a feature |
| Key exam | Pannus, subluxation | Heberden's/Bouchard's nodes, crepitus | Dactylitis, keratoderma blenorrhagica | Tophi, podagra | No tophi; chondrocalcinosis on X-ray |
| RF / ANA | RF+, anti-CCP+ | Negative | Seronegative | Negative | Negative |
| HLA assoc. | HLA-DR4 | None | HLA-B27 (60–80%) | None | ANKH gene |
| Serum marker | ↑ESR, CRP, RF, anti-CCP | Normal | ↑ESR/CRP; HLA-B27+ | ↑Uric acid (>8 mg/dL) | Normal uric acid; ↑Ca²⁺ if hyperparathyroid |
| Synovial fluid | Inflammatory (WBC >2000); no crystals | Non-inflammatory (WBC <2000); no crystals | Inflammatory; no crystals; culture negative | Needle crystals, negative birefringence | Rhomboid crystals, positive birefringence |
| X-ray | Erosions, juxta-articular osteopenia, joint space narrowing | Osteophytes, subchondral sclerosis/cysts, JSN | Periostitis, asymmetric sacroiliitis | "Rat-bite" punched-out erosions with overhanging edge | Chondrocalcinosis (cartilage calcification) |
| Key pathogen | None (autoimmune) | None | Chlamydia, Salmonella, Shigella, Campylobacter, Yersinia | None (metabolic) | None (metabolic/metabolic disease) |
| Systemic features | Nodules, scleritis, ILD, vasculitis | None | Urethritis, conjunctivitis, uveitis, mucocutaneous | Renal stones, nephropathy | Usually none (except secondary metabolic cause) |
| 1st-line Rx | MTX (DMARD) | NSAIDs, PT, weight loss | NSAIDs ± antibiotics (Chlamydia) | NSAIDs / colchicine (acute); allopurinol (ULT) | NSAIDs / colchicine / intra-articular steroids |
| Disease-specific Rx | DMARDs, biologics (anti-TNF) | Joint replacement | Sulfasalazine/MTX if chronic | Allopurinol, febuxostat | Low-dose colchicine prophylaxis; no ULT |
Key Distinguishing Pearls
- Morning stiffness >1 hr → think RA (or other inflammatory arthritis); <30 min → think OA
- DIP involvement → OA (Heberden's) or psoriatic arthritis; MCP/wrist sparing DIP → RA
- 1st MTP sudden overnight pain → GOUT until proven otherwise
- Knee calcification (chondrocalcinosis) on X-ray → PSEUDOGOUT
- Urethritis + conjunctivitis + arthritis + recent GI/GU infection → REACTIVE ARTHRITIS
- Sausage digit (dactylitis) → reactive arthritis, psoriatic arthritis (spondyloarthropathy)
- Negatively birefringent needle crystals → GOUT; positively birefringent rhomboid crystals → PSEUDOGOUT
- Tophi on ear helix → chronic gout; subcutaneous nodules on extensor surface → RA nodules
- Seronegative + HLA-B27 + sacroiliitis → spondyloarthropathy (ReA, AS, psoriatic)
- Metabolic screen for pseudogout: always check hyperparathyroidism, hemochromatosis, hypomagnesemia, hypothyroidism
Sources: Textbook of Family Medicine 9e — Goldman-Cecil Medicine International Edition — Robbins & Kumar Basic Pathology — Robbins, Cotran & Kumar Pathologic Basis of Disease — Miller's Review of Orthopaedics 9e
This is a shared conversation. Sign in to Orris to start your own chat.