A 28 year old thin with low fat percentage girl.cqm to gynec opd with small breast size as she concerned about her married life she want to increase her breast size how can it possible without hormonal tablet
Checking Date & Time
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Loading Image
Here is a comprehensive, clinically structured answer for this gynecology OPD scenario.
Breast Augmentation (Augmentation Mammoplasty) — Non-Hormonal Options
A thin woman with low body fat percentage having small breasts is a classic candidate for augmentation mammoplasty. This is a well-established surgical field with two main non-hormonal options:
1. Surgical Implant-Based Augmentation (Augmentation Mammoplasty)
"Many patients seek surgical intervention to increase breast size in a procedure known as augmentation mammoplasty. Breast volume is increased by insertion of a synthetic implant specifically designed for this purpose." — Schwartz's Principles of Surgery, 11th Ed.
Implant Types:
| Type | Filling Material | Notes |
|---|---|---|
| Silicone gel implants | Cohesive silicone gel | Most natural feel; FDA approved ≥22 years for cosmetic use |
| Saline implants | Sterile saline | Adjustable volume; if ruptured, saline is safely absorbed |
Both have an outer silicone elastomer shell. Choice depends on patient build, desired outcome, and surgeon preference.
Implant Placement Planes:
| Placement | Pros | Cons |
|---|---|---|
| Subglandular (above pectoralis) | May address mild pre-existing ptosis | More visible/palpable in thin patients with low fat |
| Partially submuscular / Dual plane (under pectoralis) | Better camouflage in thin patients; preferred mammographic surveillance | Slightly more recovery |
Key point for this patient: Since she has low fat percentage, submuscular placement is generally preferred — it provides better soft-tissue coverage and reduces visible implant edges.
Incision Approaches:
- Periareolar — scar at skin junction, minimally visible
- Inframammary fold (IMF) — hidden in natural fold (most common)
- Axillary — remote, no breast scar
- Transumbilical — rarely used
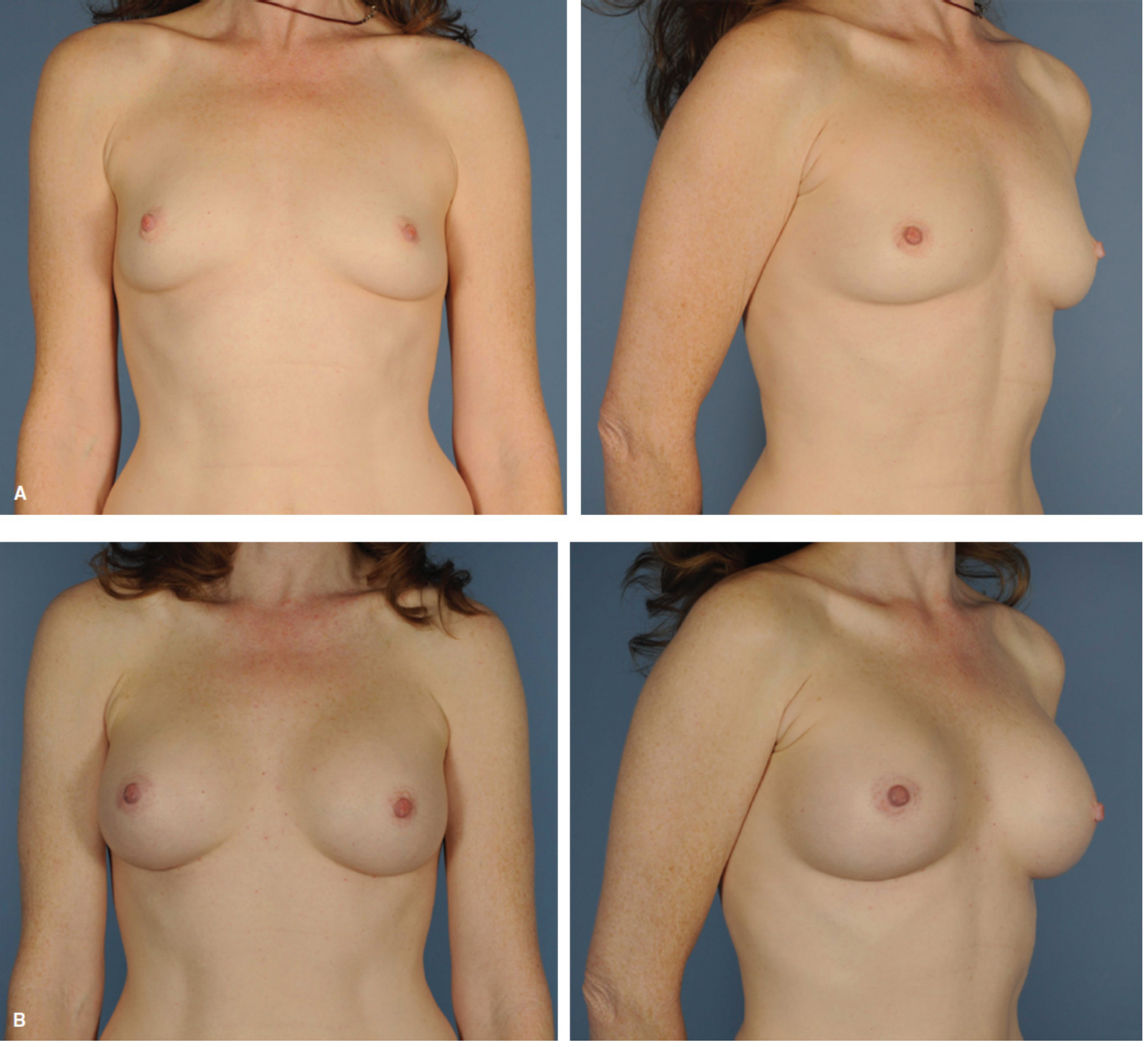
2. Autologous Fat Grafting (Lipofilling)
"Autologous fat grafting has gained increased interest and has been applied to various areas of aesthetic and reconstructive surgery. Specific applications include fat grafting to augment breast aesthetics." — Schwartz's Principles of Surgery, 11th Ed.
How it works:
- Fat is harvested by liposuction from donor sites (abdomen, thighs, flanks)
- Processed by centrifugation/filtering to isolate viable adipocytes
- Injected in small micro-aliquots into the breast using blunt cannulas
Limitation for this patient: She has low body fat percentage, which is a practical constraint — insufficient donor fat may limit the achievable volume increase. Only modest enlargement (usually 1 cup size per session) is reliably achievable. Multiple sessions are often required.
This is still a valid option if she refuses implants and has even minimal donor fat.
Preoperative Considerations
| Aspect | Recommendation |
|---|---|
| Breast cancer screening | Preoperative screening per ACS guidelines mandatory before elective breast surgery |
| Post-augmentation mammography | Standard screening mammograms are no longer adequate — diagnostic mammograms with radiologist present are required |
| MRI for rupture surveillance | FDA recommends MRI at 3 years post-implant, then every 2 years (for silicone implants) |
| Informed consent | Must cover all known risks and benefits of synthetic implant materials |
Known Risks to Counsel About
| Complication | Details |
|---|---|
| Capsular contracture | Scarring around implant → firmness/distortion; rates 4.6–18.3% at 6 years depending on indication — Berek & Novak's Gynecology |
| Implant rupture | Occurs in ~10% of women; MRI is gold standard for detection |
| BIA-ALCL | Rare (1–3 cases/million women/year); presents as late seroma around implant; treated with implant + capsule excision — Berek & Novak's Gynecology |
| Silicone particle seepage | Can cause palpable axillary adenopathy even without rupture |
Summary Recommendation for this Patient
| Option | Suitability |
|---|---|
| Silicone submuscular implant | Best option — reliable volume, good coverage in thin patients, natural feel |
| Saline submuscular implant | Good alternative — safer if rupture occurs |
| Autologous fat grafting | Limited by low body fat — may achieve modest result only |
| Hormonal tablets | Not indicated (patient declined) |
Referral: This patient should be referred to a plastic/reconstructive surgeon specializing in aesthetic breast surgery for preoperative assessment, implant size selection (based on chest wall measurements), and consent counseling.
Sources: Schwartz's Principles of Surgery, 11th Ed. | Mulholland & Greenfield's Surgery, 7th Ed. | Berek & Novak's Gynecology
She also don't want any surgical procedure
Checking Date & Time
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Searching the Web
non-surgical non-hormonal breast enlargement evidence based methods
Finding Sources
Searching PubMed
breast enlargement non-surgical vacuum bra technique
Searching PubMed
BRAVA external tissue expander breast augmentation
Finding Sources
This is a situation where the honest clinical answer needs to be clearly communicated. Here is a comprehensive, evidence-based response:
Non-Surgical, Non-Hormonal Breast Enlargement — What the Evidence Actually Says
This is a critically important counseling opportunity. The patient must be given honest, realistic information.
Why Breast Size Is Hard to Change Without Surgery or Hormones
The breast is composed of:
- Glandular/ductal tissue — controlled by hormonal milieu (estrogen, progesterone, prolactin)
- Adipose (fat) tissue — the dominant volume component, especially in thin women
- Stroma and Cooper's ligaments — structural scaffolding
In a thin woman with low body fat, most of the breast volume deficit is adipose tissue. Without increasing fat stores or using hormones/surgery, truly enlarging the breast is biologically very limited.
Options Available (Non-Surgical, Non-Hormonal)
1. 🥗 Nutritional Weight Gain (Targeted Body Fat Increase)
- Most physiologically logical option for a thin patient
- Increasing overall body fat percentage leads to increased adipose deposition in the breasts
- Counselling: balanced calorie surplus diet with healthy fats (nuts, avocados, dairy), resistance training to build pectoral muscle beneath the breast mound
- Realistic expectation: modest volume increase over months; depends on individual fat distribution genetics
- No risks; should be first-line recommendation
2. 💪 Chest/Pectoral Muscle Exercise
- Exercises (push-ups, chest press, chest fly, dumbbell press) strengthen the pectoralis major
- This does not directly increase breast tissue or fat, but:
- Improves breast projection and perkiness
- Creates a fuller, firmer chest contour
- Pushes the breast mound forward
- Realistic expectation: improved appearance, not true size increase
- Completely safe; recommended as adjunct
3. 🔵 External Vacuum Tissue Expander (BRAVA Device)
- A dome-shaped suction device worn over the breasts for hours daily
- Creates chronic mechanical tension → stimulates tissue expansion (angiogenesis, adipogenesis)
- Evidence: A prospective clinical trial (Myung et al., J Plast Reconstr Aesthet Surg, 2016 — PMID 27769601) showed increased vessel density via MRI during external breast expansion in Asian women
- Most published evidence uses BRAVA as a pre-conditioning step before fat grafting (surgical)
- As a standalone: very limited, modest, and temporary results; requires 10–12 hours/day for weeks
- Practical limitation: compliance is very poor; device is cumbersome
4. 👙 Supportive Bra / Padding / Shapewear
- Push-up bras, padded bras, breast enhancers, and silicone inserts
- No biological effect but provide immediate cosmetic improvement
- Entirely safe; should be discussed as a practical interim solution
- Modern options are very natural-looking and widely used
What Does NOT Work (Debunking Common Claims)
| Claim | Reality |
|---|---|
| Massage with oils/creams | No evidence of tissue volume change |
| Herbal supplements (fenugreek, fennel, saw palmetto) | Contain phytoestrogens — essentially a weak hormonal effect; not safe to call "non-hormonal" |
| Suction pumps (cheap devices) | No clinical evidence; risk of bruising, skin damage |
| Specific foods "for breasts" | No food selectively increases breast fat |
⚠️ Note on phytoestrogen-containing supplements: Patients sometimes seek "natural" herbs, but these work via weak estrogenic activity — they are a de facto hormonal intervention and should be mentioned only with that caveat.
Counseling Framework for This Patient
| Step | Action |
|---|---|
| 1. Acknowledge her concern | Validate that breast size concerns before marriage are common and deserve clinical attention |
| 2. Set realistic expectations | No non-surgical, non-hormonal method reliably increases breast size significantly |
| 3. Recommend weight gain | If BMI is low, a structured nutrition plan to increase healthy body fat is the most physiologically sound approach |
| 4. Recommend chest exercises | Improves appearance and posture |
| 5. Recommend proper bra fitting | Immediate, safe cosmetic improvement |
| 6. Address psychosocial component | If body image distress is significant, referral for psychological counseling / body image therapy may be appropriate |
| 7. Keep surgical option open | Inform her that implant-based augmentation remains available if she reconsiders in future |
Key Takeaway for the Clinician
There is no proven non-surgical, non-hormonal method that reliably and permanently increases breast volume. The most honest, ethical, and beneficial counseling combines:
- Realistic goal-setting
- Nutritional optimization
- Exercise for contour
- Practical cosmetic aids (bras/padding)
- Psychological support if needed
Referring her to a plastic surgeon for a consultation (without committing to surgery) is also appropriate — so she can make a fully informed decision with all options clearly explained.
If she ready for hormonal pill how will the result
Checking Date & Time
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Excellent — I now have strong textbook evidence to give a thorough, honest answer.
Effect of Hormonal Pills on Breast Size — What to Expect
Understanding the Physiology First
Breast size in an adult woman is determined by:
- Adipose (fat) tissue — dominant component, especially in thin women
- Glandular/ductal-lobular tissue — hormonally responsive
- Stroma and ligaments — structural support
"Estrogens stimulate growth of the breasts' mammary glands plus the deposition of fat to give the breasts mass." — Guyton & Hall Medical Physiology
"During the follicular phase of the menstrual cycle, estrogen stimulates proliferation of the lactiferous duct components. After ovulation in the luteal phase, progesterone stimulates the growth of alveoli; intralobular stroma becomes edematous. Clinically, during the luteal phase, tenderness and a progressive increase in breast tissue mass may be felt." — Histology: A Text and Atlas
What Hormonal Pills Can Do
Combined Oral Contraceptive Pill (COCP — Estrogen + Progestin)
This is the most commonly used hormonal option. Here is what the evidence shows:
| Effect | Explanation |
|---|---|
| Mild breast fullness/engorgement | Estrogen stimulates ductal proliferation; progesterone stimulates lobular/alveolar growth and causes stromal edema |
| Temporary size increase | Mainly due to fluid retention and glandular swelling, especially in the first 1–3 months |
| Breast tenderness | Very common side effect; indicates glandular activity |
| Modest permanent change | Some women do notice a slight sustained increase in size, but this is variable and unpredictable |
Key limitation: In a thin woman with low body fat, the dominant volume deficit is adipose tissue. Hormonal pills do not significantly increase breast fat — they primarily act on glandular tissue. So the result will be:
- Modest at best — likely 1/2 to 1 cup size at most
- Partially reversible — much of the effect diminishes when pills are stopped
- Highly individual — some women notice a meaningful change; many do not
Options Within Hormonal Pills
| Pill Type | Estrogen Content | Expected Breast Effect |
|---|---|---|
| High-estrogen COCP (≥30 µg ethinyl estradiol) | Higher | More ductal stimulation; greater breast fullness |
| Low-estrogen COCP (<20 µg ethinyl estradiol) | Lower | Minimal breast effect |
| Progestin-only pill (mini-pill) | None | Negligible breast size effect |
| Estrogen-only pill | Estrogen only | Ductal growth without lobular development; not commonly prescribed |
For breast augmentation effect, a monophasic COCP with 30 µg ethinyl estradiol gives the best hormonal exposure.
Realistic Outcome Counseling
| Timeline | What Happens |
|---|---|
| 1st month | Breast tenderness, mild swelling/engorgement (mainly fluid) |
| 2–3 months | Some ductal and lobular glandular growth; modest sustained fullness |
| 3–6 months | Maximum effect usually reached; minimal further change after this |
| On stopping | Fluid retention resolves; glandular changes may partially persist or revert |
Bottom line: She should be told the truth — hormonal pills will produce a mild, partially temporary, and unpredictable increase in breast fullness. It is not a reliable breast enlargement method. The effect is more of a "fuller feeling" than a true size increase.
Risks to Counsel About
"There is a small (~1.2-fold) increased risk of breast cancer in women using OCs." — Robbins & Kumar Basic Pathology
| Risk | Details |
|---|---|
| Breast cancer | ~1.2-fold increased risk with OC use; resolves after stopping |
| Thromboembolism (DVT/PE) | Increased risk due to hepatic coagulation factor synthesis — contraindicated in thrombophilia |
| Cardiovascular | Low risk in women <30 years, non-smokers |
| Hepatic adenoma | Rare; associated with prolonged high-dose estrogen use |
| Cervical cancer | Small increased risk in HPV-positive women |
Summary for This Patient
| Aspect | Answer |
|---|---|
| Will pills enlarge breasts? | Mildly and partially — not dramatically |
| How much? | Likely ½–1 cup size at best; varies per individual |
| Is it permanent? | Partially — effect reduces when stopped |
| Best pill for this purpose? | Monophasic COCP with 30 µg ethinyl estradiol |
| Risks? | Small increased breast cancer risk, DVT risk — requires screening before prescribing |
| Conclusion | Pills are not a reliable breast augmentation method; expectations must be kept very realistic |
Clinical Recommendation: If she is otherwise a candidate for OCPs (no contraindications — no smoking, no thrombophilia, no migraine with aura, normal blood pressure), a trial of combined OCP for 3–6 months can be offered with realistic expectations. Pair it with nutritional counseling and chest exercises for the best combined result.
Sources: Guyton & Hall Medical Physiology | Histology: A Text and Atlas (Pawlina) | Mulholland & Greenfield's Surgery, 7e | Robbins & Kumar Basic Pathology
This is a shared conversation. Sign in to Orris to start your own chat.