define essential hypertension
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
I now have comprehensive information from multiple authoritative textbooks. Here is a well-synthesized definition and overview:
Essential Hypertension
Definition
Essential hypertension (also called primary hypertension) is a sustained elevation in arterial blood pressure for which no single identifiable or reversible cause can be found. It accounts for 85–90% of all hypertension in adults (Goldman-Cecil Medicine). The remaining 10–15% is secondary hypertension, attributable to specific causes such as renal artery stenosis, primary aldosteronism, or monogenic disorders.
The term "essential" is historical and somewhat misleading — it does not mean the hypertension is necessary, but rather that it is idiopathic. Most modern texts prefer the term primary hypertension.
Pathophysiology
The underlying mechanisms are multifactorial, involving genetic predisposition and environmental triggers:
1. Impaired Renal Pressure Natriuresis
The most central defect is the kidneys' failure to excrete sufficient sodium at normal arterial pressures. This leads to:
- Fluid volume expansion → increased cardiac output → peripheral vasoconstriction → elevated blood pressure
- A new steady state ("resetting of pressure natriuresis") is reached, but only at the cost of chronically elevated pressure. (Robbins & Cotran Pathologic Basis of Disease)
2. Obesity and Sympathetic Activation
Excess adiposity accounts for up to 65–75% of the risk for developing primary hypertension. Key mechanisms include:
- Increased sympathetic nerve activity (especially renal) driven by leptin and other adipokines
- Activation of the renin-angiotensin-aldosterone system (RAAS) → raised angiotensin II and aldosterone
- Physical compression of the kidneys by perinephric fat
- Reduced arterial baroreceptor sensitivity (Guyton & Hall Textbook of Medical Physiology)
3. Increased Systemic Vascular Resistance
The primary hemodynamic abnormality in established essential hypertension is elevated systemic vascular resistance (Goldman-Cecil Medicine). Vasoconstrictive stimuli and structural vessel wall remodeling perpetuate this state.
4. Genetic Factors
- Heritability is estimated at ~30%; concordance is higher in monozygotic than dizygotic twins
-
500 genetic variants from genome-wide association studies are linked to blood pressure
- Rare Mendelian forms (Liddle syndrome, Gordon syndrome, apparent mineralocorticoid excess) illustrate how sodium-channel mutations can cause hypertension — highlighting sodium metabolism's central role (Goldman-Cecil Medicine; Robbins & Cotran)
5. Environmental / Behavioral Factors
- High dietary sodium (hypertension is rare at < 50 mmol/day sodium intake)
- Physical inactivity
- Heavy alcohol consumption (≥3 drinks/day → sympathetic activation via withdrawal)
- Obstructive sleep apnea → nocturnal sympathetic surges
- Low dietary potassium intake
Clinical Features
- The vast majority of patients are asymptomatic — hypertension is often detected incidentally
- Some experience sleep disturbance or reduced exercise tolerance
- On physical examination, the earliest sign is typically hypertensive retinopathy
- Secondary hypertension should be excluded, especially in younger patients or those with resistant hypertension
Vascular Pathology
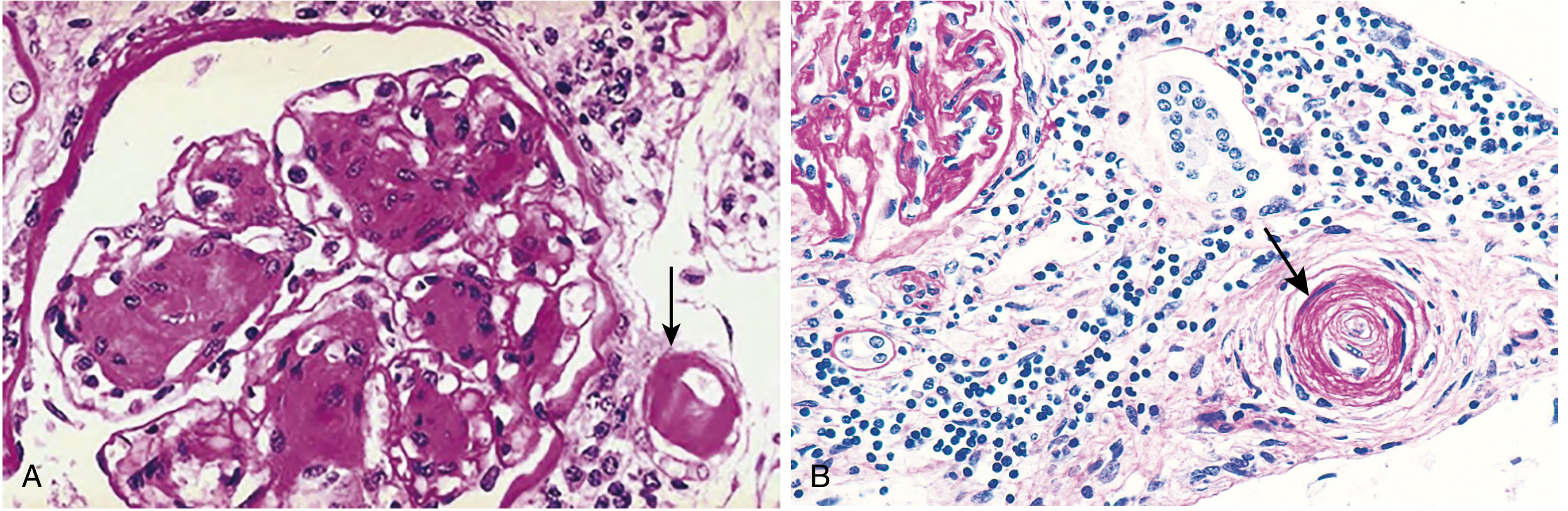
Chronic hypertension causes two main forms of small vessel injury (Robbins & Cotran):
| Lesion | Description | Setting |
|---|---|---|
| Hyaline arteriolosclerosis | Homogeneous pink hyaline thickening, luminal narrowing | Benign hypertension, elderly, diabetes |
| Hyperplastic arteriolosclerosis | Concentric "onion-skin" laminations; may include fibrinoid necrosis | Malignant/severe hypertension |
Key Points Summary
| Feature | Detail |
|---|---|
| Prevalence | 85–90% of all hypertension cases |
| Cause | Unknown (multifactorial) |
| Primary hemodynamic defect | ↑ Systemic vascular resistance |
| Core renal defect | Impaired pressure natriuresis |
| Heritability | ~30% |
| Key risk factors | Obesity, high sodium, inactivity, alcohol, sleep apnea |
| Symptoms | Usually none ("silent killer") |
Sources: Goldman-Cecil Medicine (International Ed.); Guyton & Hall Textbook of Medical Physiology; Robbins, Cotran & Kumar Pathologic Basis of Disease; Katzung's Basic and Clinical Pharmacology (16th ed.)
select a p drug for e hypertension in step wise step as WHO
Finding Sources
Finding Sources
Searching the Web
WHO stepwise treatment essential hypertension preferred drug selection 2023 2024
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Searching the Web
WHO hypertension treatment guidelines stepwise approach drug selection 2023
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
I now have excellent content from Goldman-Cecil Medicine and the textbooks. Let me compile the comprehensive stepwise answer drawing from the WHO-aligned approach and major guideline comparisons found in the textbooks.
Stepwise Drug Selection for Essential Hypertension
(Based on WHO-aligned guidelines and major evidence-based frameworks — Goldman-Cecil Medicine, Katzung's Pharmacology, Lippincott Pharmacology)
Before Any Drug: Lifestyle Modification (Foundation Step)
All guidelines require lifestyle changes first for stage 1 / uncomplicated hypertension (can lower SBP by 7–15 mmHg):
| Intervention | SBP Reduction |
|---|---|
| DASH / Mediterranean diet | ~6 mmHg |
| Sodium restriction (<1500 mg/day) | 5–10 mmHg |
| Aerobic exercise 90–150 min/week | 4–8 mmHg |
| Weight loss (per 1 kg) | ~1 mmHg |
| Alcohol ≤2 drinks/day (men), ≤1 (women) | 2–4 mmHg |
| Smoking cessation | Indirect CV benefit |
Step 1 — First-Line Monotherapy (or Low-Dose Dual Therapy)
The four preferred first-line drug classes (WHO and major guidelines):
| Class | Example Drugs | Notes |
|---|---|---|
| Thiazide/thiazide-like diuretic | Chlorthalidone 12.5–25 mg, Indapamide 1.25–2.5 mg, Hydrochlorothiazide 12.5–25 mg | Preferred in elderly, Black patients, isolated systolic HTN |
| ACE inhibitor (ACEi) | Enalapril, Lisinopril, Ramipril | Preferred in diabetes, CKD with proteinuria, HF; avoid in pregnancy |
| Angiotensin Receptor Blocker (ARB) | Losartan, Valsartan, Irbesartan | Use if ACEi not tolerated (cough, angioedema) |
| Dihydropyridine Calcium Channel Blocker (CCB) | Amlodipine 5–10 mg, Nifedipine XL | Preferred in elderly, Black patients, angina |
Race consideration (JNC/AHA): In Black patients, thiazide diuretic or CCB is preferred over ACEi/ARB alone as monotherapy (ACEi/ARB less effective as monotherapy in this group).
Target: < 130/80 mmHg (ACC/AHA 2017) or < 140/90 mmHg (WHO/ESC/ESH)
Step 2 — Add a Second Drug (If Step 1 Fails After 4–8 Weeks)
If monotherapy is insufficient, combine two complementary agents:
Preferred combinations:
- ACEi or ARB + CCB (e.g., Ramipril + Amlodipine) ← most commonly recommended by WHO/ESC
- ACEi or ARB + Thiazide diuretic (e.g., Lisinopril + Chlorthalidone)
- CCB + Thiazide diuretic (for Black patients or when RAAS not tolerated)
⚠️ Avoid: ACEi + ARB together — minimal added BP benefit, high risk of renal impairment and hyperkalemia.
β-blockers are not recommended for initial therapy in uncomplicated hypertension — they are less effective for stroke prevention than first-line drugs.
Step 3 — Triple Therapy (If Step 2 Fails)
Add a third agent from a different class:
Standard triple combination:
ACEi/ARB + CCB + Thiazide-like diuretic
(e.g., Ramipril + Amlodipine + Indapamide)
This is the backbone of the ESC/ESH 2018 and WHO HEARTS protocol "triple pill" strategy.
Step 4 — Resistant Hypertension (Fails Triple Therapy at Optimal Doses)
Defined as BP uncontrolled on ≥3 drugs including a diuretic. Before escalating:
- Confirm adherence and rule out pseudo-resistance (white coat effect)
- Ensure long-acting thiazide-like diuretic (chlorthalidone or indapamide — not HCTZ alone)
- Check for secondary causes
Add-on options:
| Drug | Indication |
|---|---|
| Spironolactone 25–50 mg | Drug of choice for resistant HTN (aldosterone excess common) |
| β-blocker (bisoprolol, carvedilol) | If CAD, HF, or tachycardia present |
| α-blocker (doxazosin) | + BPH in men; add diuretic to prevent fluid retention |
| Central sympatholytic (clonidine) | Last resort; risk of rebound HTN on abrupt withdrawal |
| Vasodilator (minoxidil, hydralazine) | Only with concurrent diuretic + β-blocker; very late add-on |
Summary Stepwise Algorithm
STEP 0: Lifestyle modification (all patients)
↓
STEP 1: One first-line drug (thiazide / ACEi / ARB / CCB)
[Consider low-dose dual therapy if BP >20/10 above target]
↓
STEP 2: ACEi or ARB + CCB or Thiazide
↓
STEP 3: ACEi/ARB + CCB + Thiazide-like diuretic (triple pill)
↓
STEP 4: Add spironolactone ± β-blocker ± α-blocker ± clonidine
(Resistant HTN — investigate secondary causes)
Preferred Drug by Compelling Indication
| Comorbidity | Preferred Drug(s) |
|---|---|
| CKD / Proteinuria | ACEi or ARB |
| Diabetes | ACEi or ARB (± CCB or thiazide) |
| Heart failure (reduced EF) | ACEi/ARB/ARNI + β-blocker + MRA |
| Post-MI / CAD | β-blocker + ACEi/ARB |
| Elderly / Isolated systolic HTN | Thiazide-like diuretic or CCB |
| Black patients | Thiazide or CCB (first-line monotherapy) |
| Angina | CCB (amlodipine) or β-blocker |
| Pregnancy | Methyldopa, labetalol, nifedipine (ACEi/ARB contraindicated) |
| BPH | α-blocker (doxazosin) as add-on |
| Pheochromocytoma | α-blocker first (phenoxybenzamine), then β-blocker |
Key principle: Most patients need 2 or more drugs for adequate control. Single-pill combinations improve adherence. Long-acting (once-daily) agents are strongly preferred. Lifelong therapy is required in the overwhelming majority of patients.
Sources: Goldman-Cecil Medicine (International Ed.); Katzung's Basic and Clinical Pharmacology, 16th ed.; Lippincott Illustrated Reviews Pharmacology; Tintinalli's Emergency Medicine
This is a shared conversation. Sign in to Orris to start your own chat.