Opthalmia neonatorum
Reading File
Finding Sources
Searching PubMed
ophthalmia neonatorum neonatal conjunctivitis
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Searching Images
ophthalmia neonatorum neonatal conjunctivitis newborn eye discharge
Here is a comprehensive overview of Ophthalmia Neonatorum (Neonatal Conjunctivitis).
Ophthalmia Neonatorum
Definition: Conjunctivitis occurring in a neonate within the first 30 days of life. It frequently signals systemic infection and demands identification of the exact cause in all but the most transient cases.
Classification & Key Features
| Type | Causative Agent | Onset | Key Findings | Treatment |
|---|---|---|---|---|
| Chemical | Erythromycin ointment prophylaxis | < 24 hours | Bilateral, watery discharge; negative Gram stain | Watchful waiting; resolves in 48 hrs |
| Gonococcal | Neisseria gonorrhoeae | 2–7 days | Intense chemosis, copious purulent discharge; gram-negative diplococci on Gram stain | Admission + IV antibiotics |
| Chlamydial | Chlamydia trachomatis | 7–14 days | Mucopurulent discharge, intense palpebral erythema | Oral + topical erythromycin |
| Other Bacterial | S. aureus, H. influenzae, E. coli, Pseudomonas | 7–14 days | Variable; identified by Gram stain/culture | Topical antibiotics (mostly) |
| Viral (HSV) | HSV-1 / HSV-2 | 14–28 days | Corneal dendrites on fluorescein; may lack skin vesicles | Admission + IV + topical antivirals |
Clinical Presentation
Critical signs: Purulent, mucopurulent, or mucoid discharge from one or both eyes in the first month of life, with diffuse conjunctival injection.
Other signs: Eyelid edema, chemosis.
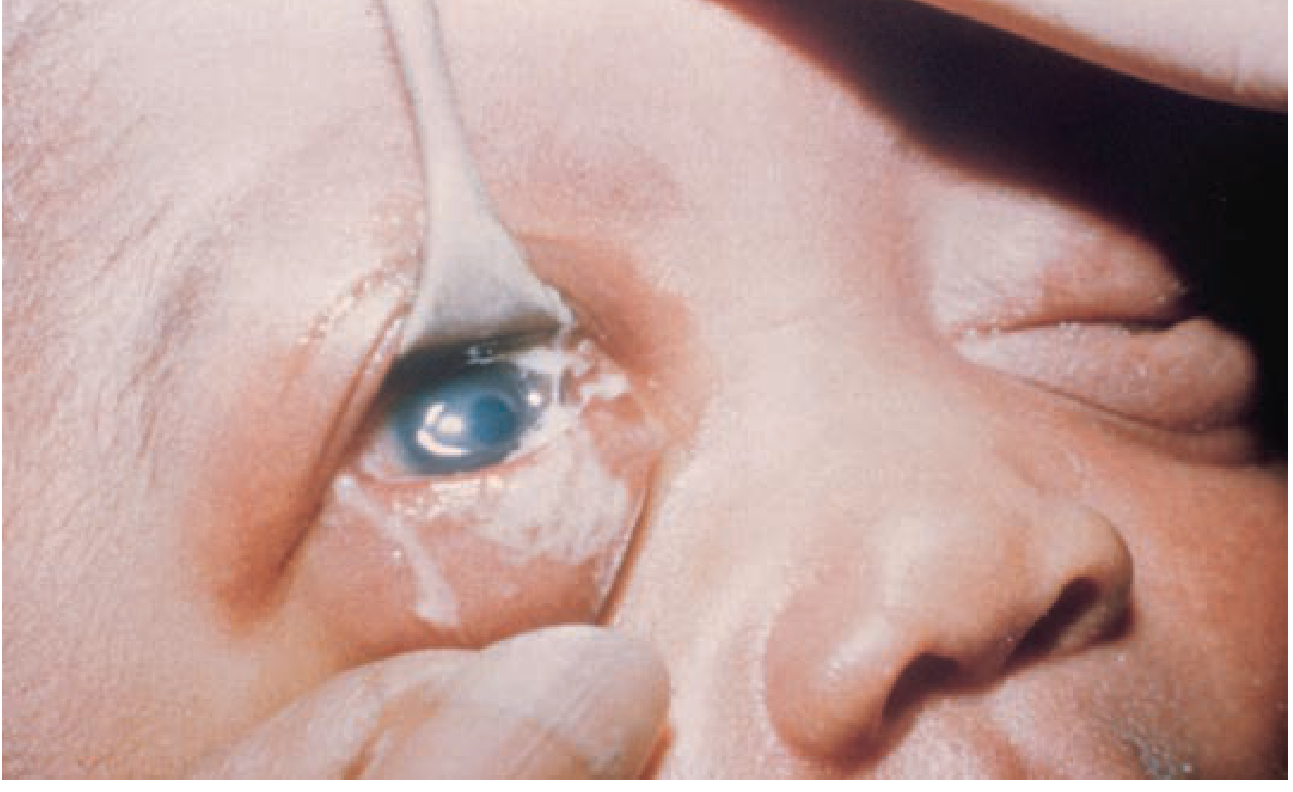
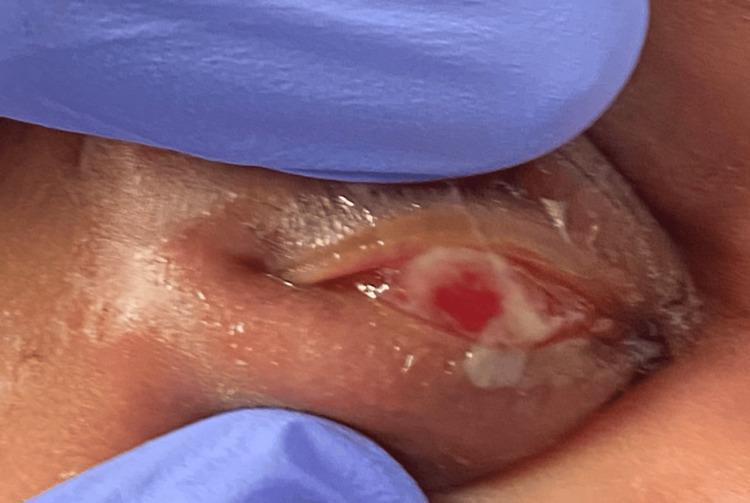
Etiology in Detail
1. Chemical
- Caused by prophylactic agents (classically silver nitrate; now erythromycin ointment).
- Self-limited, resolves within 24–36 hours; no treatment needed.
2. Gonococcal
- Acquired during passage through an infected birth canal.
- Onset 2–7 days; presents with intense bilateral chemosis and copious purulent discharge.
- The organism can penetrate intact corneal epithelium → rapid corneal ulceration and perforation if untreated.
- Half of untreated patients develop corneal clouding (major cause of blindness).
- Gram stain: gram-negative intracellular diplococci.
- Must evaluate for disseminated disease (joints, CNS, blood, CSF).
3. Chlamydial
- Most common infectious cause; C. trachomatis is a leading cause overall.
- Onset 7–14 days; bilateral mucopurulent discharge with eyelid edema and palpebral injection.
- May form pseudomembranes with bloody discharge in severe cases.
- Systemic complications: chlamydial pneumonia, rhinitis, otitis media.
- Diagnosis: Giemsa stain (intracytoplasmic basophilic inclusion bodies in epithelial cells), PCR, ELISA, DNA hybridization.
4. Other Bacterial
- Organisms: S. aureus, S. epidermidis, H. influenzae (non-typeable), E. coli, Pseudomonas.
- Non-typeable H. influenzae is uniquely severe — requires hospitalization, full septic workup, and parenteral antibiotics.
- All others: topical antibiotics usually sufficient.
5. Herpes Simplex (Viral)
- Rare but devastating; caused by HSV-2 > HSV-1.
- Onset 14–28 days; corneal dendrites → geographic ulcer.
- Risk of keratitis and disseminated neonatal HSV (encephalitis, multi-organ failure).
- Maternal history of herpes infection may be absent.
- Steroid drops are strictly contraindicated.
Differential Diagnosis
- Dacryocystitis: Swelling/erythema below the inner canthus
- Nasolacrimal duct obstruction: Chronic tearing without true conjunctivitis
- Congenital glaucoma: Tearing + corneal haze + buphthalmos
Workup
- History: Maternal STI history, prenatal cultures
- Ocular exam with fluorescein staining (assess corneal involvement)
- Conjunctival scrapings for Gram and Giemsa stain
- Cultures: Blood agar + chocolate agar (in 2–10% CO₂ for gonococcal)
- Chlamydial PCR/immunofluorescent antibody test
- Viral culture (if HSV suspected — moisten swab, roll along palpebral conjunctiva)
- Systemic evaluation by primary care/paediatrics
Treatment
Chemical
- Discontinue offending agent; preservative-free artificial tears if needed; reevaluate in 24 hours.
Gonococcal
- Hospitalize; ophthalmology consult.
- Ceftriaxone 25–50 mg/kg IV/IM (max 125 mg) single dose, or cefotaxime 100 mg/kg IV/IM single dose.
- Use cefotaxime if hyperbilirubinemia is present or disseminated infection suspected (requires longer course).
- Saline irrigation of conjunctiva and fornices until discharge clears.
- Treat both parents for gonorrhoea and chlamydia.
Chlamydial
- Oral erythromycin 50 mg/kg/day in 4 divided doses × 14 days + erythromycin ophthalmic ointment QID.
- Alternative: azithromycin 20 mg/kg/day orally × 3 days.
- Topical therapy alone is not effective — systemic treatment is mandatory.
- Treat mother and partners (doxycycline 100 mg BD × 7 days; azithromycin 1 g single dose if breastfeeding/pregnant).
- All neonates with chlamydial infection should also be evaluated for N. gonorrhoeae.
Other Bacterial
- Topical bacitracin-polymyxin ointment usually sufficient.
- Non-typeable H. influenzae: admit + parenteral antibiotics.
Herpes (Viral)
- Hospitalize; full septic evaluation including LP with HSV PCR of CSF.
- IV acyclovir 20 mg/kg every 8 hours for 14–21 days.
- Topical antivirals: 1% trifluridine, 0.1% iododeoxyuridine, or 0.15% ganciclovir.
Unknown Etiology (empirical)
- Erythromycin ointment QID + erythromycin elixir 50 mg/kg/day in 4 divided doses for 2–3 weeks.
Prophylaxis
Standard regimen (CDC-recommended, given at birth):
- Erythromycin 0.5% ophthalmic ointment (agent of choice in most countries)
- Silver nitrate 1% aqueous solution (historical; being phased out)
- Tetracycline 1% ophthalmic ointment
The Canadian Paediatric Society advises against routine prophylaxis; the American Academy of Pediatrics continues to recommend it for all newborns. Povidone-iodine 0.5% is an emerging alternative — less toxic, inexpensive, and effective, but not yet widely adopted.
Key Complications
| Organism | Complication |
|---|---|
| N. gonorrhoeae | Corneal ulceration/perforation, blindness |
| C. trachomatis | Pneumonia, otitis media (inadequate treatment) |
| HSV | Disseminated infection, encephalitis |
Recent Evidence
A 2025 systematic review and meta-analysis (PMID: 39810179) examined the global epidemiology of ophthalmia neonatorum — the most current large-scale evidence available. No findings from this study contradict established management guidelines.
Sources: Tintinalli's Emergency Medicine 9e, Wills Eye Manual, Textbook of Family Medicine 9e
This is a shared conversation. Sign in to Orris to start your own chat.