Teach me about lobar penuemonia
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Reading File
Reading File
Loading Image
Loading Image
Loading Image
Reading File
Searching PubMed
"lobar pneumonia" AND "community-acquired pneumonia"
Searching PubMed
"community-acquired pneumonia" AND "diagnosis"
Lobar pneumonia is a pattern of pneumonia where inflammation and exudate fill alveoli across a large portion of one lobe, or an entire lobe, causing dense consolidation.
What it is
- Pneumonia means infection/inflammation of lung parenchyma (especially alveoli).
- In lobar pneumonia, consolidation is confluent and lobar rather than patchy.
- Classically associated with bacterial infection, especially Streptococcus pneumoniae (also possible with Klebsiella and others).
(Fishman’s Pulmonary Diseases and Disorders, p. 1640; Robbins, Cotran & Kumar Pathologic Basis of Disease, p. 662)
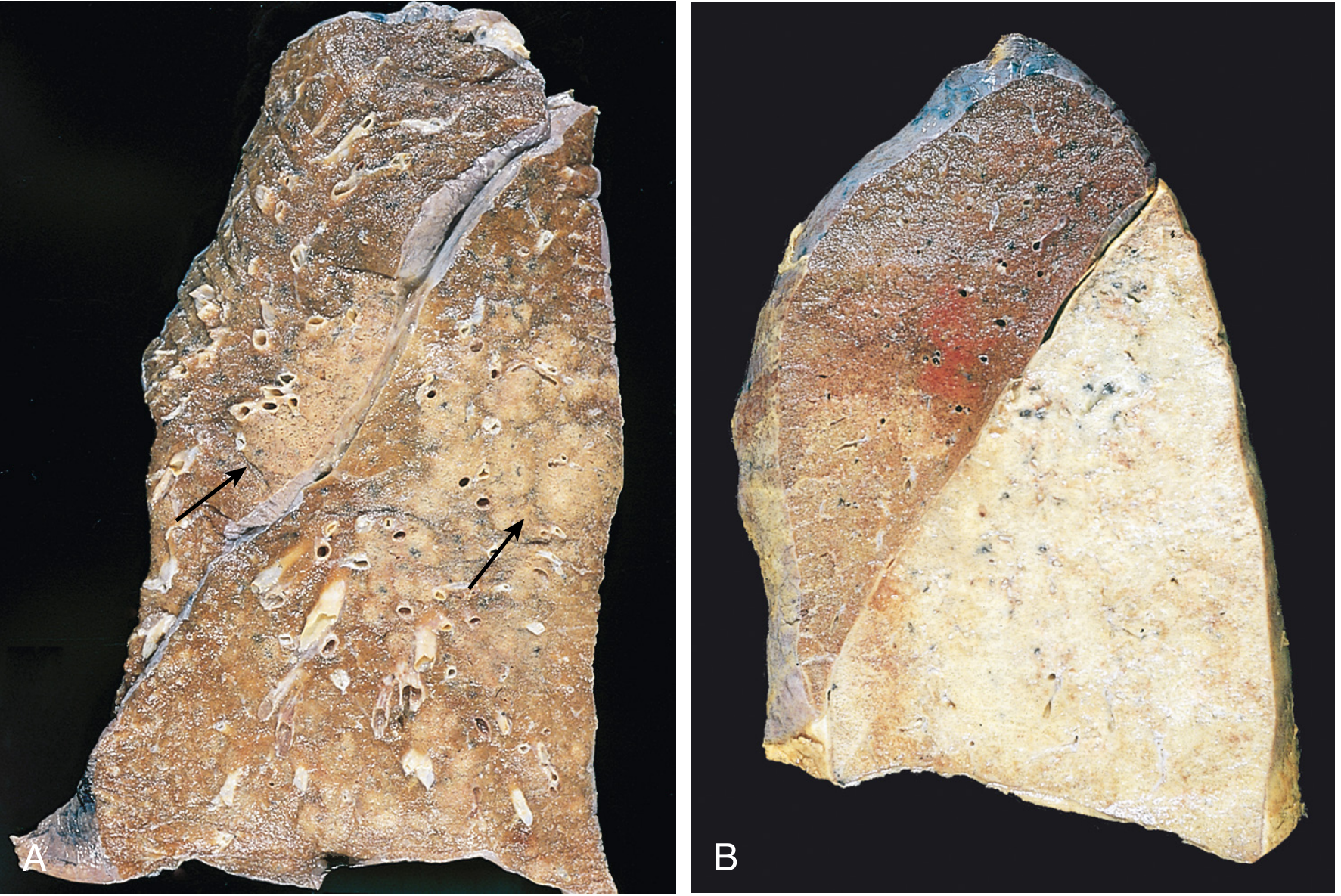
How it develops (pathology)
Classic stages described in pathology:
- Congestion: heavy, red, boggy lung; vascular engorgement and edema fluid in alveoli
- Red hepatization: alveoli fill with neutrophils, RBCs, fibrin; firm “liver-like” lobe
- Gray hepatization: RBC breakdown with persistent fibrinopurulent exudate; gray-brown appearance
- Resolution: enzymatic digestion and clearance of exudate by macrophages/resorption/expectoration, or organization
(Robbins & Kumar Basic Pathology, p. 470; Robbins, Cotran & Kumar Pathologic Basis of Disease, p. 662)
Symptoms and signs
Typical acute bacterial picture can include:
- Fever, chills/rigors
- Cough with sputum (sometimes rust-colored or purulent)
- Dyspnea
- Pleuritic chest pain
- Exam findings of consolidation (bronchial breath sounds, crackles)
(Tintinalli’s Emergency Medicine, p. 505; Robbins, Cotran & Kumar Pathologic Basis of Disease, p. 662)
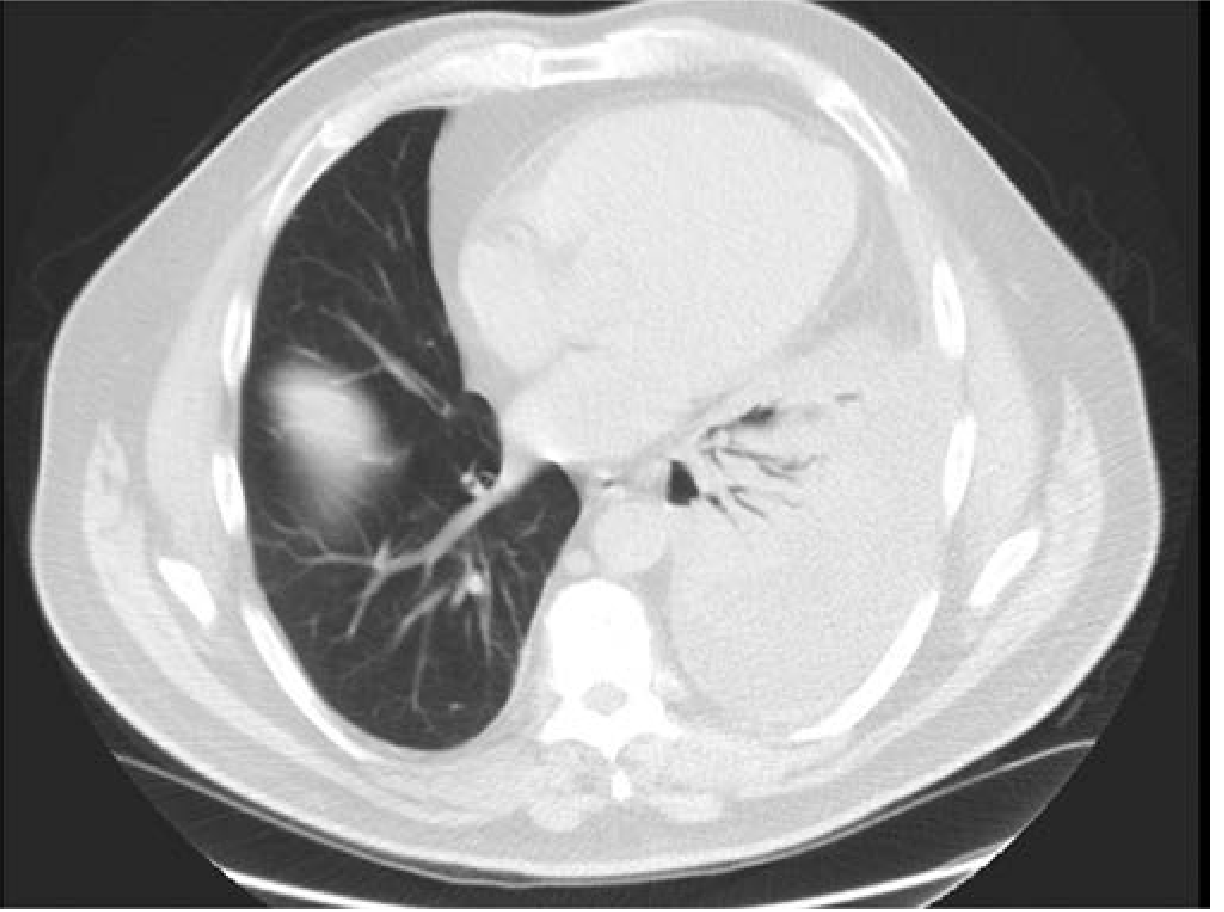
Imaging features
- Lobar air-space consolidation on chest imaging
- Air bronchograms are a classic clue (air-filled bronchi outlined by surrounding alveolar opacification)
- Pleural effusion may accompany severe bacterial cases
(Fishman’s Pulmonary Diseases and Disorders, p. 1640)
Complications
Possible complications include:
- Lung tissue necrosis/abscess
- Parapneumonic effusion or empyema
- Pleuritis with adhesions
- Bacteremic spread causing meningitis, endocarditis, pericarditis, septic arthritis, etc.
(Robbins & Kumar Basic Pathology, p. 470; Robbins, Cotran & Kumar Pathologic Basis of Disease, p. 662)
Clinical diagnosis and treatment principles
- Diagnosis is clinical plus radiographic infiltrate (history/exam + chest imaging).
- Identify severe disease and need for hospitalization.
- Start empiric antibiotics targeting common CAP pathogens, then narrow if microbiology identifies an organism.
- Supportive care: oxygen (if hypoxemic), fluids, antipyretics, monitoring for complications.
(Tintinalli’s Emergency Medicine, p. 505)
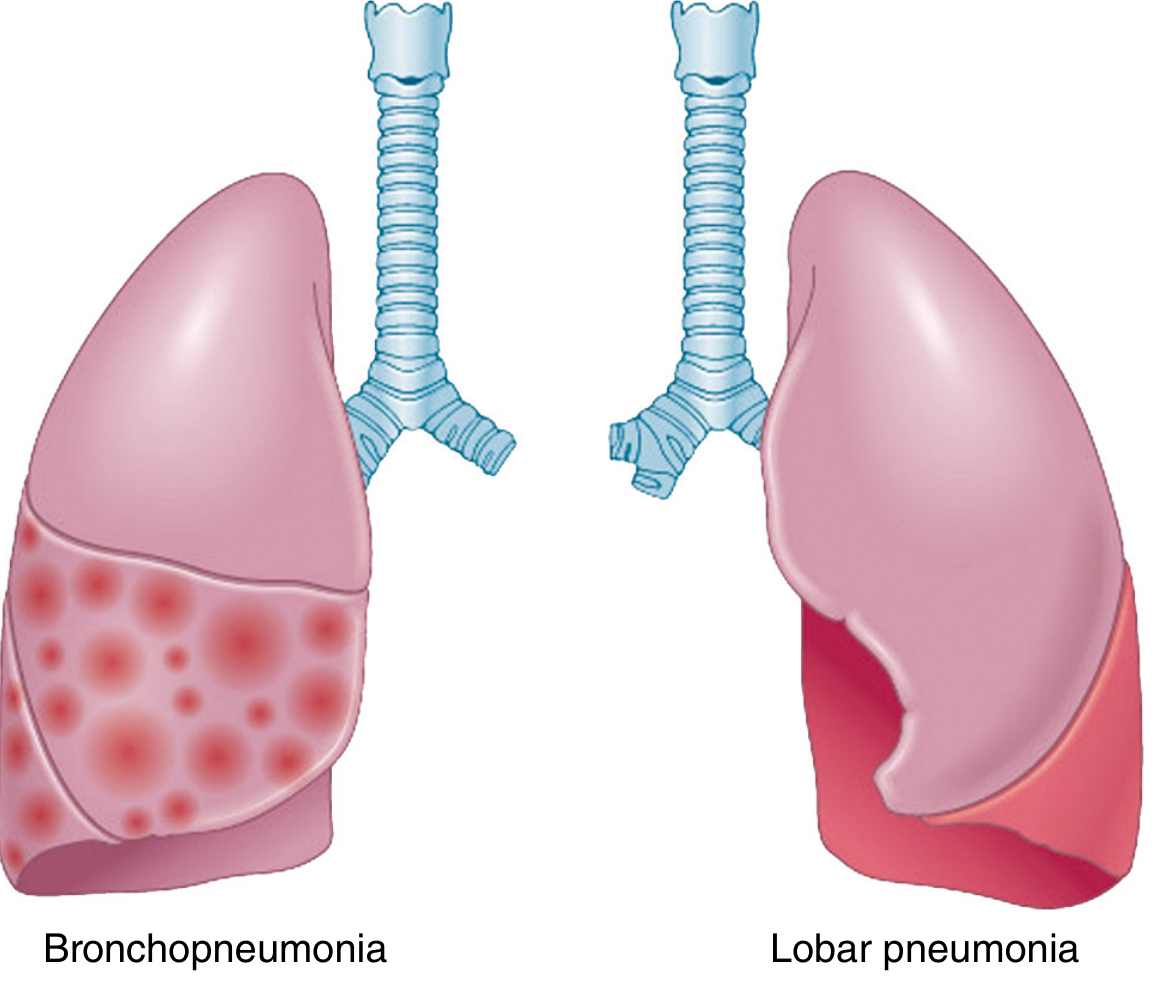
Lobar vs bronchopneumonia (quick distinction)
- Lobar pneumonia: confluent involvement of large part/all of a lobe
- Bronchopneumonia: patchy, often multilobar/basal foci centered around bronchi/bronchioles
Recent evidence check (last 2 years): no direct meta-analysis focused only on “lobar pneumonia” pattern, but newer CAP systematic reviews suggest updates in antibiotic strategy/risk stratification may affect management pathways (PMIDs: 40107661, 39243792, 39427174).
This is a shared conversation. Sign in to Orris to start your own chat.