Abscess
Reading File
Asking for Preferences
Finding Sources
Searching PubMed
abscess management incision drainage
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have comprehensive content to deliver a thorough, well-organized answer.
Abscess
Definition
An abscess is a focal accumulation of pus within body tissues, representing the end result of tissue destruction by a pyogenic infection. The surrounding tissue undergoes liquefactive necrosis, forming a walled-off cavity filled with dead cells, bacteria, and inflammatory exudate. — Rosen's Emergency Medicine, p. 1250
Pathophysiology
Bacteria breach the skin or mucosal barrier (usually via trauma, follicular invasion, or haematogenous seeding) and trigger an acute inflammatory response. Polymorphonuclear neutrophils migrate to the site, attempt phagocytosis, and die, releasing proteases. The resulting liquefied material (pus) accumulates under pressure, creating the characteristic fluctuant cavity enclosed by a pyogenic membrane.
Common Types
| Type | Key Features |
|---|---|
| Furuncle | Staphylococcal infection of a hair follicle + surrounding tissue; localized fluctuant nodule |
| Carbuncle | Multiple confluent furuncles in thick skin (nape of neck, back, thigh); severe pain, fever; risk of septicaemia |
| Hidradenitis suppurativa | Recurrent apocrine gland abscesses in axillae/groin; often resistant to therapy |
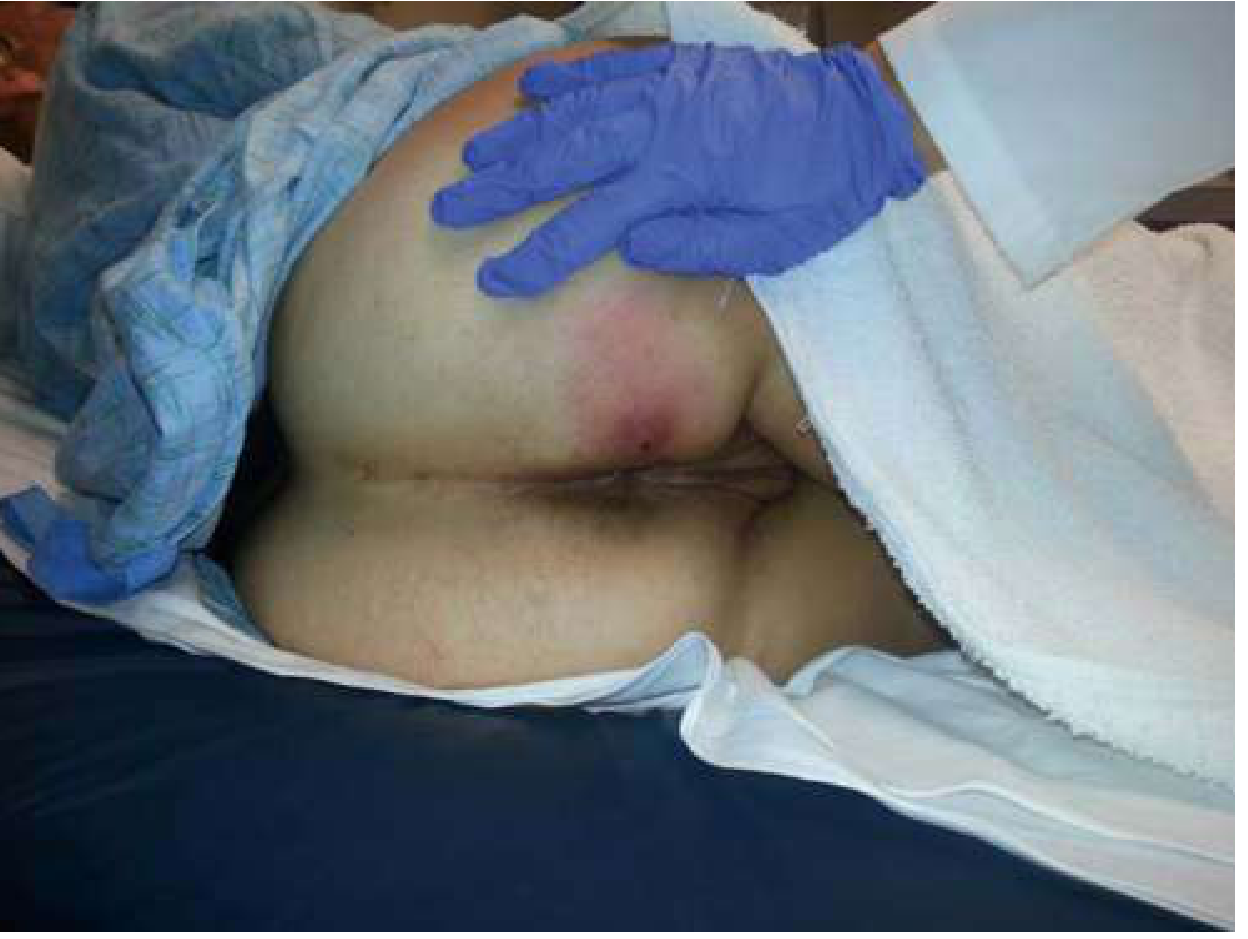
| Perianal/perirectal | May indicate fistula-in-ano; requires surgical referral |
| Collar-button (web space) | Subfascial hand infection; palmar + dorsal swelling, fingers held in abduction |
| Peritonsillar | Deep neck space; risk of airway compromise |
| Intra-abdominal | Hepatic, subphrenic, pelvic; usually post-operative or complicating visceral perforation |
| Brain abscess | Neurosurgical emergency; headache, focal deficit, fever triad |
| Epidural | Spinal emergency; back pain + neurological signs |
Clinical Features
- Local: Erythema, warmth, swelling, tenderness, central fluctuance (the hallmark distinguishing it from cellulitis)
- Systemic: Fever, malaise, leukocytosis (more common in carbuncles or deep abscesses)
- MRSA lesions often show central necrosis and are frequently mistaken by patients for spider bites
- Adjacent fingers held in abduction suggests collar-button (web space) abscess
Diagnosis
Clinical Examination
Fluctuance on palpation is the key distinguishing feature from cellulitis, which lacks a drainable fluid collection.
Point-of-Care Ultrasound (POCUS)
Ultrasound is highly useful when clinical examination is equivocal:
- Abscess: discrete, focal, hypoechoic-to-anechoic fluid collection surrounded by thickened subcutaneous tissue; may contain internal echoes if debris-laden
- Cellulitis: "cobblestoning" — hypoechoic fluid interwoven in a reticular pattern between tissue planes, without a discrete cavity
- Ultrasound also determines depth and size, critical before I&D
- For peritonsillar abscess: intraoral probe shows rounded hypoechoic/anechoic collection; carotid artery location can be assessed
— Roberts & Hedges' Clinical Procedures in Emergency Medicine, p. 869
Microbiology
- Most common organism: Staphylococcus aureus (including MRSA in community settings)
- Perianal, intra-abdominal: mixed flora including anaerobes
- IV drug users: polymicrobial; Streptococcus spp.
- Send wound cultures in moderate–severe cases
Management
1. Incision & Drainage (I&D)
I&D is the definitive treatment — antibiotics alone are inadequate once pus has localized.
Key principles (Roberts & Hedges):
- Do not incise prematurely — incision before pus localizes is not curative and may spread infection or cause bacteraemia
- Apply warm compresses for up to 24–36 hours if fluctuance is not yet present, then reassess
- Incise at the point of maximum fluctuance; make the incision long enough to allow complete drainage and prevent premature closure
- Break up loculations with a haemostat or gloved finger
- Irrigate the cavity
- Pack the wound to prevent premature skin closure (remove packing at 12–24 hours; replace with warm soapy soaks)
- Most wounds heal by secondary intention; delayed primary closure only after repeat washouts in large wounds with confirmed infection control
— Schwartz's Principles of Surgery, p. 1976; Roberts & Hedges', p. 870
2. Antibiotics
Uncomplicated abscess in an immunocompetent host: I&D alone is typically curative. Routine post-procedural antibiotics are not standard.
Antibiotics ARE indicated when:
- Severe or extensive disease (multiple sites, rapid spread)
- Associated cellulitis with systemic signs
- Immunosuppression, extremes of age
- Comorbidities (diabetes, peripheral vascular disease)
- Difficult-to-drain location (face, hand, genitalia)
- Associated septic phlebitis
- Unresponsive to I&D alone
- IV drug user with fever (rule out endocarditis before discharge)
Antibiotic selection:
| Scenario | Agent |
|---|---|
| Mild outpatient, MRSA coverage | TMP-SMX or clindamycin (5–7 days) |
| Mild outpatient, non-MRSA | Dicloxacillin, cephalexin |
| Doxycycline/minocycline | Alternative for MRSA (oral) |
| Severe / hospitalised | Vancomycin, daptomycin, linezolid, telavancin, or ceftaroline IV |
| IVDU with major abscess | IV ampicillin/sulbactam (2g/1g q6h) |
- Duration: 3–5 days (uncomplicated outpatient); 7–14 days (complicated/hospitalised)
- Cephalosporins and macrolides are typically ineffective against MRSA
3. Bacteraemia Prophylaxis
- Transient bacteraemia can occur during I&D
- Patients at high risk for endocarditis should receive prophylactic antibiotics before the procedure
- Immunocompromised patients: IV broad-spectrum antistaphylococcal coverage (cefazolin 1g IV or vancomycin) 30 minutes before I&D
— Roberts & Hedges', pp. 870–872
Special Considerations
MRSA
- Community-associated MRSA is now the most common pathogen in ED skin/soft tissue infections in many US cities
- MRSA survives on surfaces for weeks and spreads via household contacts
- Recurrences are common; patients and contacts require hygiene education
- First-line: TMP-SMX, clindamycin, minocycline, or doxycycline
Hidradenitis Suppurativa
- Drain if fluctuant, painful, and large
- Mild: topical clindamycin × 3 months
- Moderate/severe: oral clindamycin + rifampicin × 3–6 months
- Antiandrogen therapy if antibiotics fail
- Recurrent/refractory: surgical referral
Recurrence Prevention
- Personal hygiene education (regular bathing, hand washing)
- Keep wounds covered with clean dry dressings
- Decolonisation (mupirocin nasal ointment, chlorhexidine body washes) for recurrent MRSA
When to Refer / Admit
- Deep-space infections (hand, neck, mediastinum)
- Brain or spinal epidural abscess
- Sepsis or septic shock
- Failed outpatient I&D
- Immunocompromised or systemically unwell patients
- Intra-abdominal or pelvic abscess (typically require CT-guided drainage or surgical intervention)
Sources: Rosen's Emergency Medicine 9e; Roberts & Hedges' Clinical Procedures in Emergency Medicine 7e; Schwartz's Principles of Surgery 11e
This is a shared conversation. Sign in to Orris to start your own chat.