Iron deficiency anemia 15 marks long and questions for mbbs University exam
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have all the content needed to compose a comprehensive 15-mark MBBS university exam answer. Let me compile it.
Iron Deficiency Anemia — 15 Marks (MBBS University Exam)
Definition
Iron deficiency anemia (IDA) is a hypochromic microcytic anemia resulting from inadequate iron supply to the bone marrow erythroid precursors, most often due to depletion of total body iron stores. It is the most common nutritional deficiency worldwide, affecting approximately 1.2 billion individuals — roughly half of all anemic persons globally.
(Harrison's Principles of Internal Medicine 22e, p. 807; Robbins & Kumar Pathologic Basis of Disease, p. 612)
Iron Metabolism (Normal)
Understanding IDA requires a grasp of normal iron physiology:
| Parameter | Value |
|---|---|
| Total body iron (male) | ~3.5 g |
| Total body iron (female) | ~2.5 g |
| Iron in hemoglobin | ~2100 mg (male), 1750 mg (female) |
| Storage iron (ferritin + hemosiderin) | ~1000 mg (male), 400 mg (female) |
| Daily dietary iron | 10–20 mg |
| Daily loss | 1–2 mg (shed epithelial/skin cells) |
| Serum iron (male/female) | ~120 / 100 μg/dL |
| Transferrin saturation | ~33% normally; TIBC = 300–350 μg/dL |
- Absorption occurs in the proximal duodenum: Fe³⁺ is reduced to Fe²⁺ by ferrireductases (duodenal cytochrome B), transported across the apical membrane by DMT-1 (divalent metal transporter-1), then moved to plasma via ferroportin, re-oxidized by hephaestin/ceruloplasmin, and bound to transferrin
- ~20% of heme iron is absorbable vs. only 1–2% of non-heme iron
- Hepcidin (liver-derived peptide) is the master regulator: it downregulates ferroportin, reducing iron absorption. In iron deficiency, hepcidin falls, allowing maximum intestinal absorption
Etiology / Causes
Causes are best classified by mechanism (Harrison's, Table 102-2):
1. Increased Iron Demand
- Infants, toddlers, adolescents (growth spurt)
- Pregnancy (demand rises to 4–5 mg/day in third trimester)
- Breastfeeding
- Treatment with erythropoiesis-stimulating agents (ESAs)
2. Inadequate Intake
- Vegan/vegetarian diet (only non-heme iron available)
- Malnutrition, poverty
- Prolonged exclusive breastfeeding
3. Decreased Absorption
- Celiac disease (duodenal mucosal damage)
- Atrophic/autoimmune gastritis; H. pylori gastritis
- Post-gastrectomy / bariatric surgery
- Proton pump inhibitor use (reduces gastric acidity needed for Fe³⁺ → Fe²⁺ conversion)
- Hereditary iron-refractory IDA (IRIDA — TMPRSS6 mutations)
4. Chronic Blood Loss (most important cause in adults)
| Source | Examples |
|---|---|
| Gastrointestinal | Peptic ulcer, esophagitis, angiodysplasia, hookworm, colorectal carcinoma (esp. right-sided), IBD, large hemorrhoids |
| Gynecological | Heavy menstrual bleeding, fibroids, uterine cancer |
| Urinary | Intravascular hemolysis (PNH), schistosomiasis, bladder/renal cancer |
| Iatrogenic | Hemodialysis, frequent phlebotomy |
Key point for exams: In males and postmenopausal females, GI blood loss (especially colorectal carcinoma) must always be excluded.
Stages of Iron Deficiency
| Stage | Iron Stores | Serum Ferritin | Transferrin Sat. | Hemoglobin | RBC Morphology |
|---|---|---|---|---|---|
| Pre-latent (depletion) | ↓ | ↓ (<30 μg/L) | Normal | Normal | Normal |
| Latent (iron-deficient erythropoiesis) | Absent | Very low | <20% | Normal | Normal/mildly abnormal |
| Manifest IDA | Absent | Very low | <15% | ↓ | Hypochromic, microcytic |
Pathophysiology
- Iron stores become depleted → serum ferritin falls
- Hepcidin decreases (positive feedback to maximise absorption)
- Transferrin saturation falls below 15–20% → iron-restricted erythropoiesis
- Erythroid precursors in bone marrow cannot synthesise adequate hemoglobin → smaller, paler red cells
- Non-erythroid tissues also suffer: heart muscle, skeletal muscle, brain may be iron-depleted before severe anemia develops → fatigue, poor concentration, restless legs even before Hb falls
Clinical Features
General Symptoms of Anemia
- Pallor, fatigue, dyspnoea on exertion, palpitations, headache, dizziness
- Anemia often remains undetected until Hb < 8 g/dL due to slow progression
Features Specific to Iron Deficiency
| Feature | Description |
|---|---|
| Pica | Craving for non-nutritive substances — ice (pagophagia), clay, dirt, paper |
| Koilonychia | Spoon-shaped (concave) nails |
| Angular cheilosis | Fissuring at corners of mouth |
| Atrophic glossitis | Smooth, sore tongue with papillary atrophy |
| Alopecia | Hair thinning/loss |
| Dysphagia | Due to esophageal webs (Plummer-Vinson syndrome — see below) |
| Fatigue, irritability, poor concentration | Due to iron depletion in brain/muscle |
Plummer-Vinson Syndrome (Patterson-Kelly Syndrome)
Classic triad: microcytic hypochromic anemia + atrophic glossitis + dysphagia (from esophageal webs). Predisposes to postcricoid carcinoma.
Peripheral Blood Smear Findings
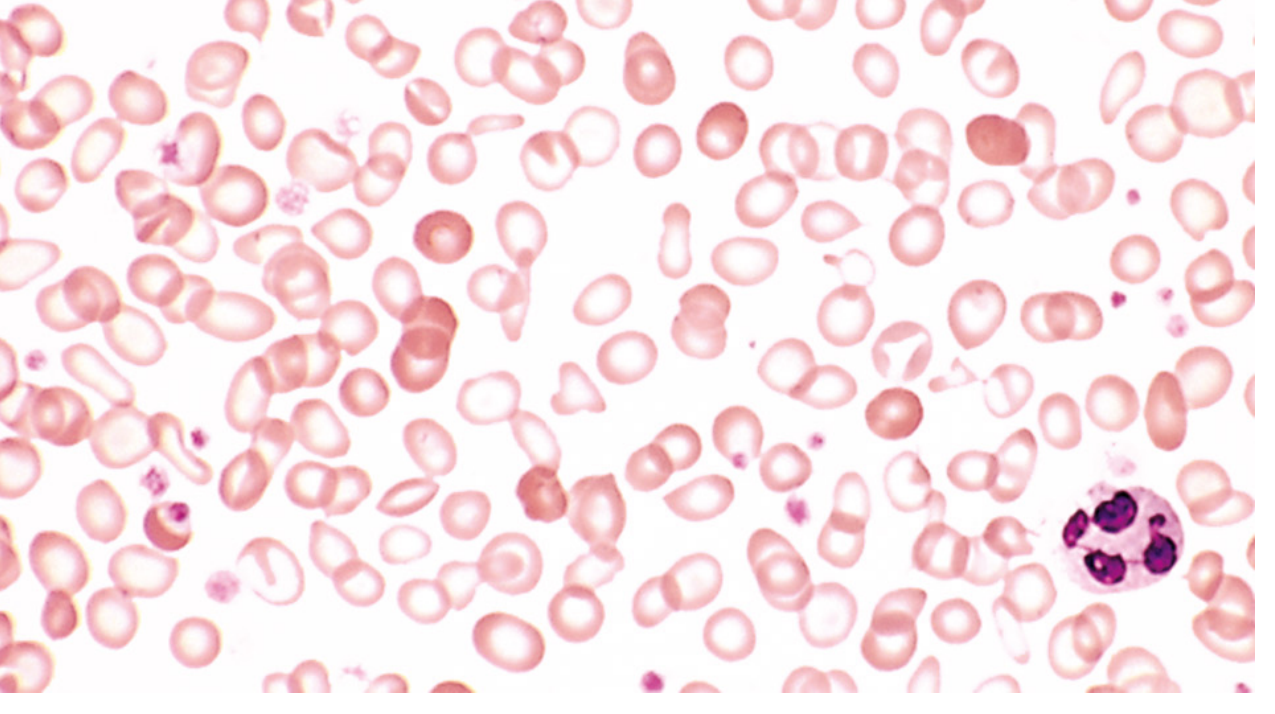
Fig. Iron deficiency anemia — peripheral blood smear. Note hypochromic microcytic RBCs with narrow rim of peripheral hemoglobin, anisocytosis, and poikilocytosis. (Robbins & Kumar Pathologic Basis of Disease)
- Microcytic (MCV < 80 fL)
- Hypochromic — pale RBCs, central pallor >1/3 diameter
- Anisocytosis (variable size) — elevated RDW (>15%)
- Poikilocytosis — pencil cells (elliptocytes), target cells
- Thrombocytosis may occur (reactive)
- Bone marrow: absent stainable iron (Prussian blue stain negative) — the gold standard for diagnosis
Laboratory Findings
| Investigation | Iron Deficiency Anemia | Normal |
|---|---|---|
| Hemoglobin | ↓ | 13.5–17.5 g/dL (M); 12–16 g/dL (F) |
| MCV | ↓ (<80 fL) | 80–100 fL |
| MCH | ↓ (<27 pg) | 27–32 pg |
| MCHC | ↓ (<32 g/dL) | 32–36 g/dL |
| RDW | ↑ (>15%) | 11.5–14.5% |
| Serum iron | ↓ (<60 μg/dL) | 80–150 μg/dL |
| TIBC | ↑ (>400 μg/dL) | 250–370 μg/dL |
| Serum ferritin | ↓ (<12–30 μg/L) | 20–200 μg/L |
| Transferrin saturation | ↓ (<15%) | 25–50% |
| Serum hepcidin | ↓ | Normal |
| Reticulocyte count | ↓ or normal | 0.5–2.5% |
| Bone marrow iron | Absent | Present |
Serum ferritin <30 μg/L has sensitivity 92% and specificity 98% — it is the single best test for diagnosing iron deficiency.
Differential Diagnosis
Differentiation from other microcytic anemias is critical:
| Feature | IDA | Anemia of Chronic Disease | Thalassemia trait | Sideroblastic Anemia |
|---|---|---|---|---|
| Serum iron | ↓ | ↓ | Normal/↑ | ↑ |
| TIBC | ↑ | ↓ | Normal | Normal/↓ |
| Ferritin | ↓ | ↑ or Normal | Normal/↑ | ↑ |
| Transferrin Sat. | ↓ | ↓ | Normal/↑ | ↑ |
| RDW | ↑ | Normal | Normal (uniform microcytes) | ↑ |
| Bone marrow iron | Absent | ↑ (trapped in macrophages) | Present | Ring sideroblasts |
| Hb electrophoresis | Normal | Normal | Abnormal (↑HbA₂) | Normal |
(Robbins & Kumar, p. 614–615)
Diagnosis
Two-step approach (Harrison's, p. 808):
- Confirm iron deficiency — serum ferritin (<30 μg/L), serum iron ↓, TIBC ↑, transferrin saturation <15–20%, MCV <80 fL, RDW ↑
- Identify the cause — detailed history (menstrual, dietary, GI symptoms), stool occult blood, upper/lower GI endoscopy in men and postmenopausal women (to exclude malignancy), celiac serology, H. pylori testing
Treatment
1. Treat the Underlying Cause
Address bleeding sources, improve diet, treat malabsorption — most important step.
2. Oral Iron (First-Line)
- Ferrous sulfate 325 mg (65–105 mg elemental iron) once or twice daily — take on empty stomach with vitamin C to enhance absorption
- Alternate-day dosing is equally effective with fewer GI side effects
- Response: Reticulocytosis in 5–7 days → Hb rises by 1–2 g/dL per week
- Continue for 3–6 months after Hb normalises to replenish stores
- GI side effects (nausea, constipation) are common; ferrous gluconate or fumarate may be better tolerated
| Oral Preparation | Elemental Iron Content |
|---|---|
| Ferrous sulfate | 65–105 mg |
| Ferrous gluconate | 27–38 mg |
| Ferrous fumarate | 29–105 mg |
3. Parenteral (IV) Iron (When Oral Fails or Is Contraindicated)
Indications: malabsorption, intolerance to oral iron, inflammatory bowel disease, CKD on ESA therapy, second/third trimester pregnancy with severe anemia, preoperative anemia
| IV Preparation | Max Single Dose |
|---|---|
| Iron sucrose | 200–300 mg |
| Iron carboxymaltose | 750–1000 mg over 15 min |
| Low-MW iron dextran | 1000 mg over 1 h |
| Iron derisomaltose | Up to 20 mg/kg |
4. Blood Transfusion
Reserved for hemodynamic instability or rapid deterioration — not routine for IDA.
5. Prevention
- Dietary counselling — include iron-rich foods (red meat, legumes, fortified cereals) and avoid inhibitors (tea, calcium with meals)
- Iron fortification of food staples in high-burden regions
- Routine iron supplementation during pregnancy
Important Exam Points (Summary)
- Most common nutritional deficiency globally; most common cause of anemia worldwide
- Key clue: hypochromic microcytic anemia with ↓ ferritin, ↓ serum iron, ↑ TIBC, ↓ transferrin saturation
- Pica (especially pagophagia/craving for ice) is a hallmark
- Koilonychia is specific for IDA among the nutritional anemias
- Plummer-Vinson syndrome = IDA + glossitis + dysphagia (esophageal webs) → risk of postcricoid carcinoma
- Hepcidin is low in IDA (opposite of anemia of chronic disease where hepcidin is high)
- Serum ferritin is the single best test; bone marrow absent iron is gold standard
- IDA vs anemia of chronic disease: TIBC ↑ in IDA, ↓ in ACD; ferritin ↓ in IDA, ↑ in ACD
- Oral ferrous sulfate → reticulocytosis in 5–7 days → normalise Hb in 6–8 weeks → continue 3–6 months for store repletion
- In adults (especially males and postmenopausal women), always investigate for GI malignancy
Sources: Robbins & Kumar Pathologic Basis of Disease (10e), pp. 612–616 | Harrison's Principles of Internal Medicine (22e), pp. 807–811 | Robbins Basic Pathology (11e), p. 393–395
This is a shared conversation. Sign in to Orris to start your own chat.