Oral Submucous Fibrosis
Reading File
Finding Sources
Searching PubMed
"oral submucous fibrosis"[MeSH Terms]
Reading File
Reading File
Finding Sources
Reading File
Reading File
Searching Images
oral submucous fibrosis clinical features fibrous bands
Here is a comprehensive overview of Oral Submucous Fibrosis (OSMF):
Oral Submucous Fibrosis (OSMF)
Definition
OSMF is a chronic, progressive, premalignant condition of the oral mucosa characterized by failure of collagen remodeling, leading to submucosal fibrosis, restricted mouth opening, and significant malignant potential. It is most prevalent in South and Southeast Asia and the western Pacific basin.
Etiology & Pathogenesis
The primary etiologic factor is habitual use of areca (betel) nut — consumed by:
- Chewing betel quid (areca nut + betel leaf + slaked lime)
- Placing paan masala in the buccal/labial sulcus
- Using powdered/packaged forms (guthka)
Pathogenic mechanism:
- Failure of collagen remodeling with altered epithelial-mesenchymal interactions
- Formation of collagenous bands and aggregates within the submucosa and lamina propria
- Diminished functional collagenase levels → increased collagen accumulation
- Elevated inducible nitric oxide synthetase (iNOS) in early erythematous phase
Diet heavily seasoned with chili also plays a contributing role — Andrews' Diseases of the Skin, p. 709
Clinical Features
Sequential progression:
| Stage | Features |
|---|---|
| Early | Oral dysesthesia (burning sensation), erythema ± vesiculation |
| Intermediate | Progressive pallor/blanching of mucosa ("marble-white"), palpable vertical fibrous bands in buccal soft tissues |
| Advanced | Restricted jaw opening (trismus), limited tongue mobility, difficulty eating, swallowing, and speech |
| Late | Ulceration, leukoplakic areas, verrucous surface changes → risk of SCC |
Sites involved: Buccal mucosa, soft palate, faucial pillars, tonsillar pillars, lips, tongue
- Characteristic inverted/shrunken uvula and sunken cheeks in advanced cases
Clinical Images
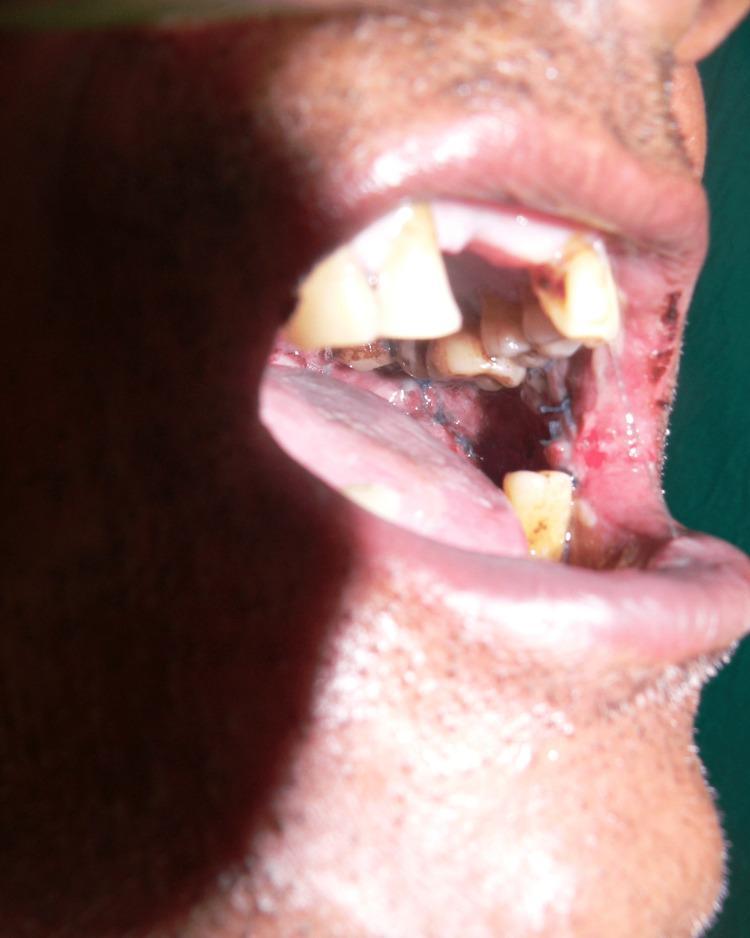
Blanched, marble-white buccal mucosa with vertical fibrous bands — a hallmark of OSMF
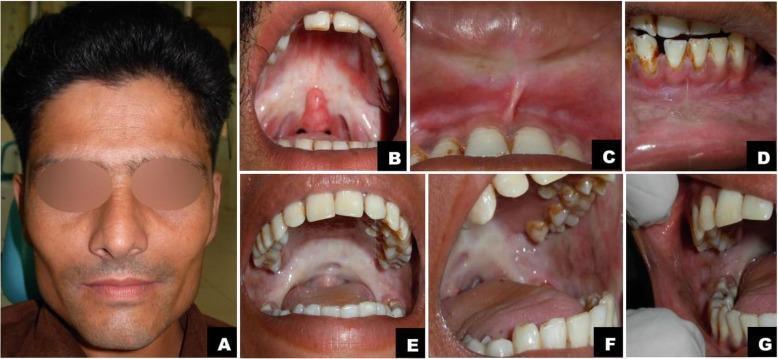
Composite showing sunken cheeks, mucosal blanching, shrunken uvula, fibrous bands, and hyperpigmentation at different stages
Histopathology
Hallmark: Juxtaposition of atrophic epithelium overlying submucosal fibrosis
- Early: Delicate, loosely arranged collagen fibers; chronic inflammation (lymphocytes, plasma cells)
- Progressive: Increasing hyalinization of collagen
- Late: Complete hyalinization of supportive connective tissue
Dysplasia grading (one study):
- Mild dysplasia: 46%
- Moderate dysplasia: 52%
- Severe dysplasia: 2%
Malignant Potential
OSMF is classified as an oral potentially malignant disorder (OPMD):
- Transformation to squamous cell carcinoma (SCC): 7–30% (transformation rate of 7.6% over 17 years reported from India)
- SCC typically arises on the buccal mucosa, tongue, and labial mucosa
- 2.5% of cases demonstrate epithelial dysplasia on biopsy
Treatment
| Category | Options |
|---|---|
| Cessation | Stop areca/betel nut use (essential) |
| Medical (intralesional) | Triamcinolone or dexamethasone (alone or with hyaluronidase); antioxidant spirulina |
| Pharmacological | Collagenase injection; pentoxifylline |
| Physical therapy | Jaw-stretching exercises |
| Surgical | Scar band release (modest success), excision + grafting, laser ablation |
Management is problematic in advanced cases, especially when areca use continues. Surgical release has only modest success.
Epidemiology
- Predominantly affects South Asians (India, Pakistan, Bangladesh) and Southeast/Pacific populations
- Betel nut is one of the world's most widely used psychoactive substances
- Also classified as a premalignant lesion alongside leukoplakia, erythroplakia, and oral lichen planus
Recent Evidence (2024 Systematic Reviews)
- Prevalence meta-analysis (Wang M et al., 2024, PMID 39525471) — pooled prevalence data across diverse populations
- Mast cell role in pathogenesis (Bijai LK et al., 2024, PMID 39402549) — mast cells implicated in fibrotic progression
- Curcumin for OPMDs (Shi W et al., 2024, PMID 39559334) — curcumin shows some efficacy in management of oral potentially malignant disorders including OSMF
Sources: Cummings Otolaryngology Head and Neck Surgery, p. 1585 | Andrews' Diseases of the Skin, p. 709 | K.J. Lee's Essential Otolaryngology | Fitzpatrick's Dermatology, p. 1742
This is a shared conversation. Sign in to Orris to start your own chat.