How to assess glenohumeral bone loss
Reading File
Finding Sources
Finding Sources
Searching PubMed
"glenohumeral bone loss" AND assessment
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
Loading Image
I now have all the information needed to provide a comprehensive answer. Here is a structured, evidence-based overview:
Assessment of Glenohumeral Bone Loss
Glenohumeral bone loss occurs on both sides of the joint — the glenoid (anteroinferior) and the humerus (posterosuperior Hill-Sachs lesion). Accurate pre-operative assessment of both is essential because significant bone loss predicts failure of soft-tissue stabilization and dictates the need for bony augmentation.
1. Clinical Context
- Some degree of glenoid bone loss is present in 40% of first-time dislocations and 85% of recurrent dislocations.
- A Hill-Sachs lesion is seen in 40% of patients with recurrent subluxation, 90% after first dislocation, and approaching 100% with recurrent dislocations.
- Bipolar lesions (combined glenoid + Hill-Sachs) occur in 33% of primary instability and 62% of recurrent instability cases.
2. Imaging Modalities
Plain Radiography
Several special views improve sensitivity:
| View | Technique | Purpose |
|---|---|---|
| Stryker Notch | Supine, arm over head, beam 10° cephalad | Detects Hill-Sachs lesion |
| West Point | Prone, forearm hanging, beam 25° downward + 25° medial | Detects anteroinferior glenoid rim (bony Bankart) |
| Bernageau (Glenoid Profile) | Arm flexed, beam along scapular spine at 30-40° | Glenoid profile, anterior rim loss |
| True AP (Grashey) | Standard shoulder series | Overall joint assessment |
CT Scan (Primary Modality)
CT is the standard for evaluating bone loss. High-resolution thin-slice acquisition with 3D volume-rendered reconstructions and digital subtraction of the humeral head provides the best visualization.
- Identifies smallest osseous fragments and glenoid asymmetry
- 3D CT with humeral subtraction: gold standard for glenoid bone loss quantification
- Also detects Hill-Sachs lesions with accuracy comparable to arthroscopy
- Essential when bipolar lesions are suspected
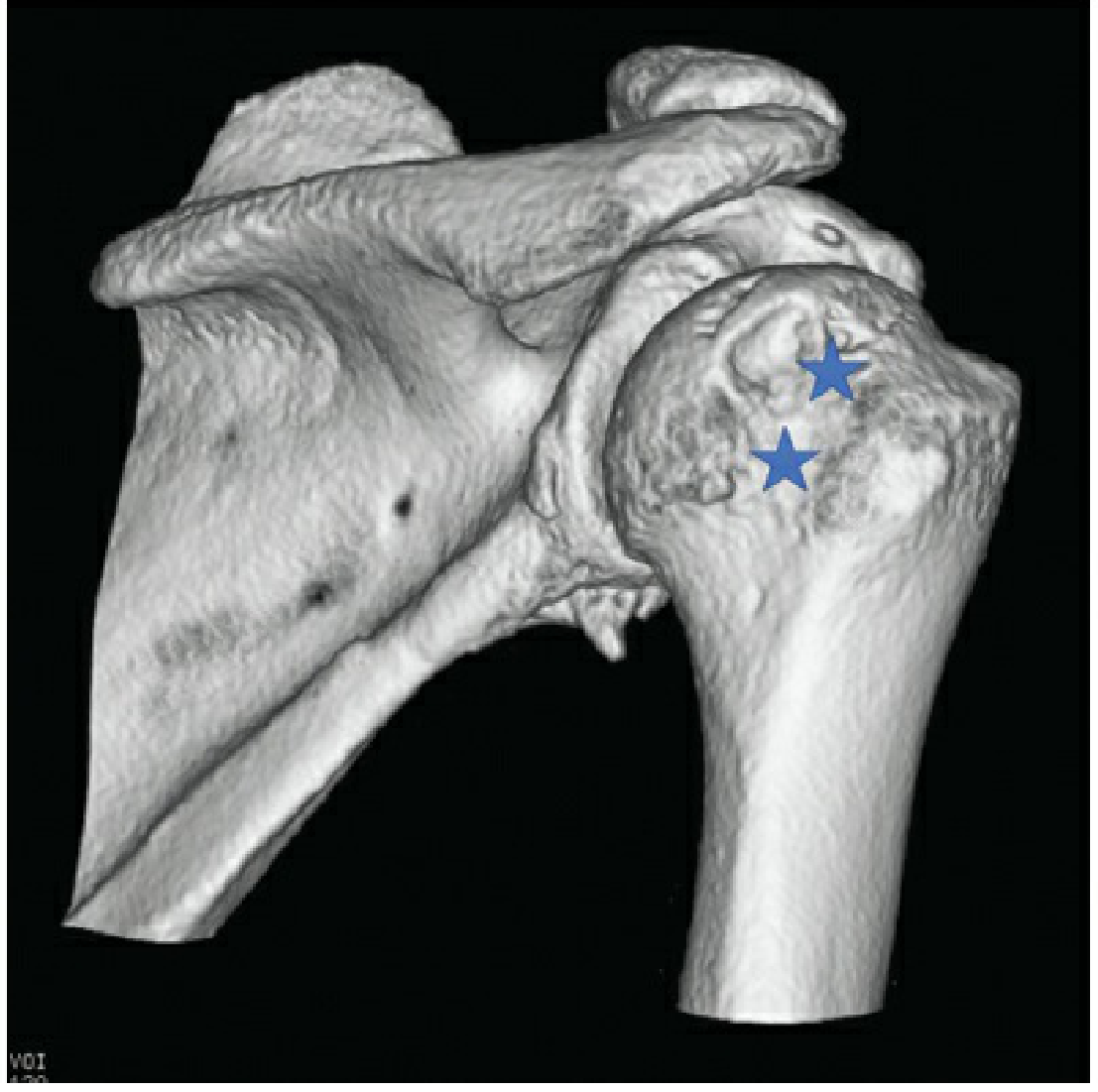
3D CT reconstruction showing Hill-Sachs lesions (★) on the posterolateral humeral head — Rockwood & Green's Fractures in Adults, 10th ed.
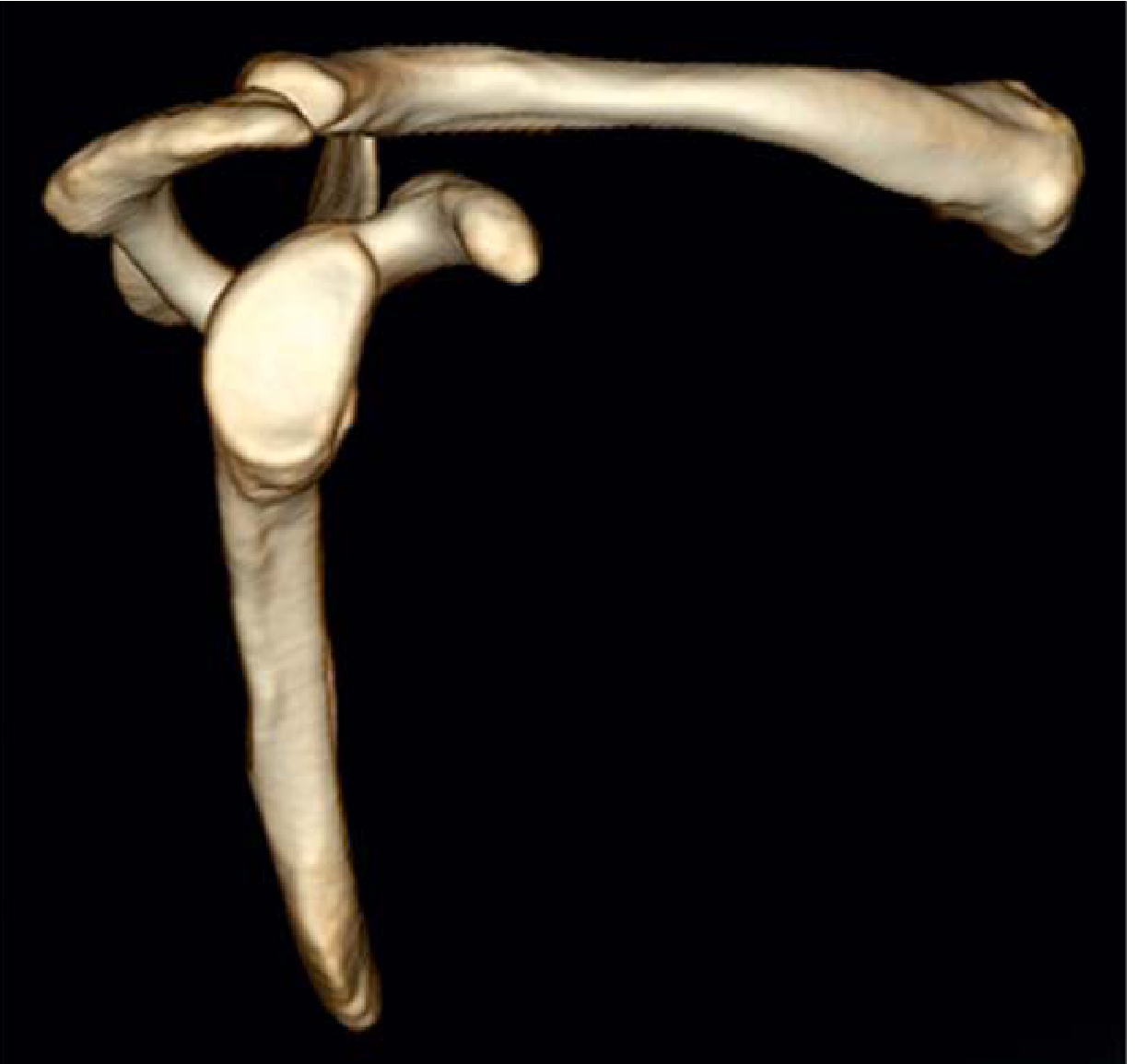
3D CT reconstruction of the glenoid and scapula demonstrating approximately 20% anterior glenoid bone loss — Miller's Review of Orthopaedics, 9th ed.
MRI / MR Arthrogram (MRA)
- MRA preferred over plain MRI for greater sensitivity for labral and ligamentous lesions
- ABER position (abduction-external rotation) increases sensitivity for anteroinferior labral injuries
- Circle method on MRI is accurate to within 1.3% of 3D CT for measuring glenoid bone loss
- Demonstrates capsular volume, glenoid version, and associated soft-tissue pathology
3. Quantifying Glenoid Bone Loss
A. Circle Method (most widely used)
A best-fit circle is drawn over the intact posterior glenoid on the en face view (CT or sagittal MRI). The missing segment anteriorly represents the bone loss.
% Bone loss = (diameter of best-fit circle − remaining anterior-posterior width) / diameter × 100
B. Burkhart Bare-Spot Arthroscopic Method
Arthroscopic measurement using a calibrated probe:
- Distance from bare spot to posterior glenoid margin = Dp
- Distance from bare spot to anterior glenoid margin = Da
- % Bone loss = (Dp − Da) / (2 × Dp) × 100
C. Width-Based Formula (Owens et al.)
Predicts normal glenoid width from height measurements on MRI:
- Males: Normal glenoid width = ⅓ height + 15 mm
- Females: Normal glenoid width = ⅓ height + 13 mm
4. Critical Thresholds
| Threshold | Significance |
|---|---|
| ≥20–25% glenoid bone loss (≈6–8 mm) | "Critical" defect → recurrence rate after arthroscopic Bankart repair rises to 67%; bony augmentation (Latarjet, bone graft) required |
| >21% of glenoid length | Biomechanically causes instability and ROM limitation after Bankart repair |
| Inverted-pear glenoid morphology | Corresponds to ~25–27% anteroinferior width loss |
5. Hill-Sachs Lesion Assessment and the Glenoid Track Concept
A Hill-Sachs lesion is not just quantified by size but by whether it is on-track or off-track — whether it will engage the anterior glenoid rim in functional positions.
Glenoid Track Calculation
Glenoid Track (GT) = 0.84 × actual glenoid width
(The 84% factor accounts for the medial glenoid insertion of the inferior glenohumeral ligament, which limits how far laterally the humeral head can translate.)
Hill-Sachs Interval (HSI)
Measured on coronal MRI as the distance from the rotator cuff footprint to the medial margin of the Hill-Sachs lesion.
Classification
- On-track (safe): HSI < GT → no engagement risk → arthroscopic Bankart repair alone is appropriate
- Off-track (high risk): HSI ≥ GT → engagement occurs → requires remplissage or Latarjet in addition
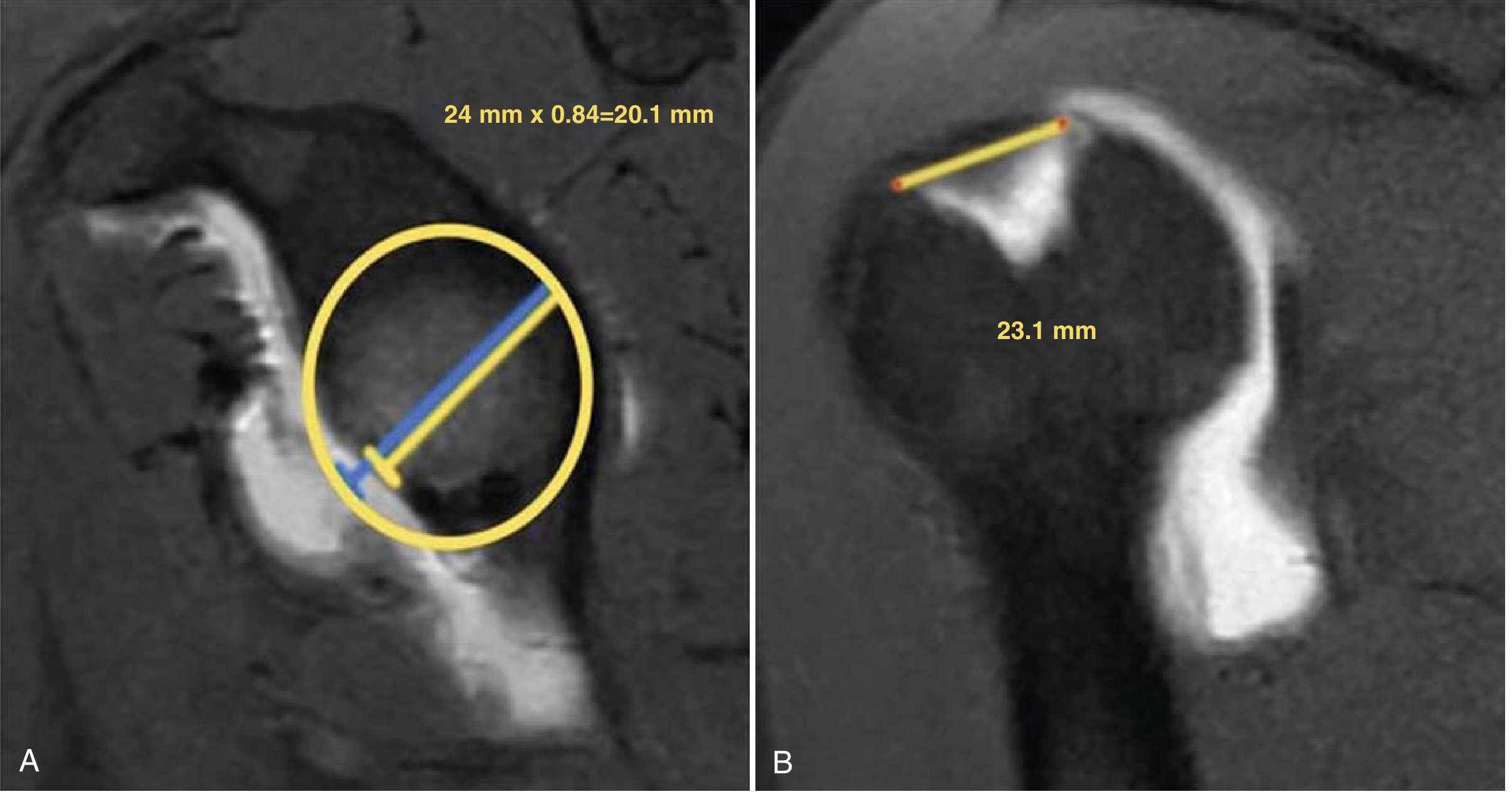
(A) Sagittal oblique MRI: best-fit circle on glenoid; glenoid track = 24 mm × 0.84 = 20.1 mm with 17% bone loss. (B) Coronal MRI: Hill-Sachs interval = 23.1 mm. Since HSI (23.1 mm) > GT (20.1 mm) → off-track lesion at high risk for engaging. (Miller's Review of Orthopaedics, 9th ed.)
6. Summary Algorithm
Plain XR (Stryker Notch, West Point, Bernageau)
↓
Suspected bone loss?
↓
3D CT with humeral subtraction ← primary quantification
+/- MRI/MRA (soft tissue, labrum, version)
↓
Measure glenoid bone loss (circle method)
↓
< 20% 20–25% > 25%
↓ ↓ ↓
Arthroscopic Borderline: Bony augmentation
Bankart repair glenoid track (Latarjet / bone graft)
analysis
↓
On-track → ABR
Off-track → ABR + remplissage or Latarjet
Sources:
- Rockwood and Green's Fractures in Adults, 10th ed., 2025 — Chapter 35
- Miller's Review of Orthopaedics, 9th ed. — Chapter 4, Anterior Instability
This is a shared conversation. Sign in to Orris to start your own chat.