Ashu Vrikka-Nishkriyata (Acute Renal Failure / AKI) & Chirakaari Vrikka-Nishkriyata (Chronic Renal Failure / CKD)
PART I — ASHU VRIKKA-NISHKRIYATA (Acute Renal Failure / Acute Kidney Injury)
1. DEFINITION
Acute Kidney Injury (AKI) — formerly "Acute Renal Failure" — is a rapid decline in the kidney's ability to clear waste products and maintain fluid-electrolyte homeostasis, occurring over hours to days.
KDIGO 2012 Diagnostic Criteria (current gold standard)
| Criterion | Threshold |
|---|
| Rise in serum creatinine | ≥ 0.3 mg/dL within 48 hours OR |
| Rise in serum creatinine | ≥ 1.5× baseline within prior 7 days OR |
| Urine output | < 0.5 mL/kg/h for ≥ 6 hours |
STAGING (KDIGO)
| Stage | Serum Creatinine | Urine Output |
|---|
| 1 | 1.5–1.9× baseline or ≥0.3 mg/dL rise | <0.5 mL/kg/h × 6–12 h |
| 2 | 2.0–2.9× baseline | <0.5 mL/kg/h × ≥12 h |
| 3 | ≥3× baseline OR ≥4.0 mg/dL OR RRT initiated | <0.3 mL/kg/h × ≥24 h OR anuria ≥12 h |
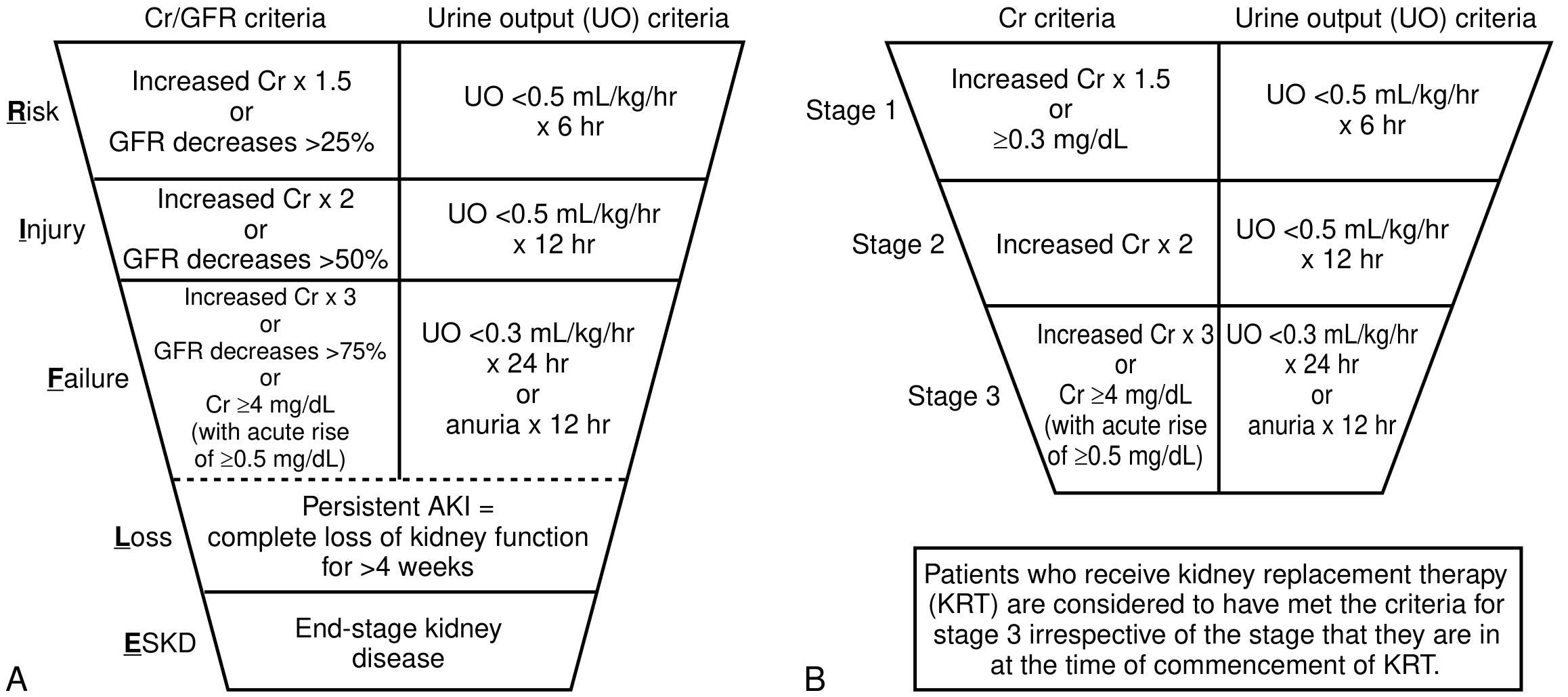
RIFLE Classification (older, still used):
- Risk → Injury → Failure → Loss (complete loss >4 weeks) → ESKD
RIFLE (A) and KDIGO (B) staging — National Kidney Foundation Primer on Kidney Diseases, 8e
2. ETIOPATHOGENESIS — CHART
Etiological Classification
ACUTE KIDNEY INJURY (AKI)
│
├── PRE-RENAL (most common ~55–60%)
│ ├── Hypovolemia: hemorrhage, burns, vomiting, diarrhea, dehydration
│ ├── Low cardiac output: heart failure, cardiogenic shock, cardiac tamponade
│ ├── Systemic vasodilation: sepsis, anaphylaxis, hepatorenal syndrome
│ ├── Renal afferent arteriolar constriction: NSAIDs, contrast agents
│ └── Efferent arteriolar dilation: ACE inhibitors, ARBs
│
├── INTRA-RENAL / RENAL (~35–40%)
│ ├── Tubular (ATN — most common intrinsic cause)
│ │ ├── Ischemic ATN (prolonged prerenal → tubular necrosis)
│ │ └── Nephrotoxic ATN
│ │ ├── Exogenous: aminoglycosides, amphotericin B, contrast dye,
│ │ │ cisplatin, cyclosporine
│ │ └── Endogenous: myoglobin (rhabdomyolysis), hemoglobin (hemolysis),
│ │ uric acid (tumor lysis), myeloma proteins
│ ├── Glomerular: rapidly progressive GN, SLE, vasculitis
│ ├── Interstitial: acute interstitial nephritis (drugs, infections)
│ └── Vascular: renal artery/vein thrombosis, malignant hypertension,
│ thrombotic microangiopathy (HUS/TTP)
│
└── POST-RENAL / OBSTRUCTIVE (~5%)
├── Ureteral: calculi, strictures, retroperitoneal fibrosis
├── Bladder: BPH, neurogenic bladder, clot retention, bladder carcinoma
└── Urethral: strictures, phimosis
Pathogenetic Mechanism of Ischemic ATN
↓ Renal Perfusion
↓
Tubular cell ischemia → ATP depletion
↓
↑ Intracellular Ca²⁺ + reactive oxygen species
↓
Cell swelling, brush border loss, cytoskeleton disruption
↓
Cell death (necrosis/apoptosis) → tubular obstruction by casts
↓
Backleak of glomerular filtrate → ↓ effective GFR
↓
Oliguria / Anuria → AKI
Key mediators: Loss of polarity, Na⁺-K⁺-ATPase mislocalization, tubuloglomerular feedback activation, afferent arteriolar vasoconstriction (endothelin, thromboxane A₂), neutrophil/macrophage infiltration.
3. DIAGNOSIS
A. CLINICAL FEATURES
Symptoms (develop as azotemia worsens):
- Oliguria (<400 mL/day) or anuria (<100 mL/day)
- Nausea, vomiting, anorexia
- Fatigue, lethargy, confusion (uremic encephalopathy)
- Asterixis, myoclonus (severe uremia)
- Pericardial friction rub (uremic pericarditis)
- Abnormal bleeding (platelet dysfunction)
Signs of volume overload:
- Peripheral oedema
- Raised JVP
- Pulmonary oedema (dyspnoea, basal crepitations)
- Hypertension
Signs pointing to etiology:
- Hypotension + skin turgor ↓ → prerenal
- Palpable bladder / suprapubic fullness → obstructive (post-renal)
- Purpuric rash → vasculitis/HUS
- Livedo reticularis → cholesterol emboli
Phases of AKI (particularly ATN):
| Phase | Duration | Key Feature |
|---|
| Initiation | Hours–days | Injury occurring; creatinine rising |
| Oliguric | 1–3 weeks (avg 10–14 days) | UO <400 mL/day; ↑ BUN, creatinine; hyperkalaemia, acidosis |
| Diuretic | Days–weeks | UO 3–5 L/day; risk of dehydration, hyponatraemia |
| Recovery | Weeks–months | GFR gradually returns; may be incomplete |
B. INVESTIGATIONS
Urinalysis & Microscopy:
| Finding | Suggests |
|---|
| Specific gravity >1.020; urine Na <20 mEq/L; FENa <1% | Prerenal |
| Granular "muddy brown" casts; renal tubular epithelial cells; urine Na >50 mEq/L; FENa >3% | ATN (intrinsic) |
| RBC casts, dysmorphic RBCs; proteinuria | Glomerulonephritis |
| WBC casts, eosinophiluria | Acute interstitial nephritis |
| No casts; dilute urine | Obstructive (post-renal) |
FENa (Fractional Excretion of Sodium) = (Urine Na × Plasma Cr) / (Plasma Na × Urine Cr) × 100
Serum Biochemistry:
- Serum creatinine & BUN (rising)
- Electrolytes: Hyperkalaemia, Hyponatraemia, Hyperphosphataemia, Hypocalcaemia
- Arterial blood gas: metabolic acidosis (↓ pH, ↓ HCO₃⁻, ↑ anion gap)
- CBC: anaemia (dilutional), eosinophilia (AIN), thrombocytopenia (HUS/TTP)
- Complement (C3/C4), ANA, ANCA, anti-GBM antibodies (if glomerular cause suspected)
Imaging:
- Ultrasound kidneys: first-line — bilateral enlarged/normal kidneys (AKI); small kidneys (CKD); hydronephrosis (obstructive)
- Doppler: renal artery/vein thrombosis
- CT abdomen/pelvis (non-contrast): calculi, retroperitoneal pathology
- Chest X-ray: pulmonary oedema
Renal Biopsy: Indicated when cause is unclear after initial workup, especially when glomerulonephritis or vasculitis is suspected.
Novel Biomarkers (early AKI detection):
- NGAL (neutrophil gelatinase-associated lipocalin)
- KIM-1 (kidney injury molecule-1)
- Cystatin C
- IL-18
- TIMP-2 × IGFBP7 (NephroCheck®)
4. PRINCIPLES OF MANAGEMENT
A. NON-PHARMACOLOGICAL
- Fluid management: Aggressive IV fluid resuscitation for hypovolaemia (isotonic saline or balanced crystalloids); avoid fluid overload. Fluid balance strictly monitored.
- Dietary modification:
- Restrict protein (0.6–0.8 g/kg/day in non-dialysis AKI to reduce urea generation)
- Restrict potassium, phosphorus, sodium
- Adequate calories (25–35 kcal/kg/day) — enteral nutrition preferred
- Avoidance of nephrotoxins: Withhold NSAIDs, aminoglycosides, contrast agents, ACE inhibitors/ARBs in the acute setting; dose-adjust all renally cleared drugs.
- Monitoring: Strict intake/output, daily weights, cardiac monitoring (hyperkalaemia), blood pressure control.
- Treat underlying cause: Relieve obstruction (catheterisation, nephrostomy), treat sepsis, remove nephrotoxic agents.
- Renal Replacement Therapy (RRT) — non-pharmacological intervention:
- Indications (AEIOU): Acidosis, Electrolyte disturbance (refractory hyperkalaemia), Ingestion/toxin, Overload (pulmonary oedema), Uraemia (symptomatic — pericarditis, encephalopathy)
- Modalities: Intermittent Haemodialysis (IHD) or Continuous Renal Replacement Therapy (CRRT — preferred in haemodynamically unstable patients)
B. PHARMACOLOGICAL
| Indication | Drug/Intervention |
|---|
| Prerenal hypotension | IV isotonic saline / balanced crystalloids; vasopressors (norepinephrine) in septic shock |
| Hyperkalaemia | IV calcium gluconate (membrane stabilisation); IV insulin + dextrose; sodium bicarbonate; calcium resonium/patiromer (exchange resins); dialysis for refractory cases |
| Metabolic acidosis | IV sodium bicarbonate (pH <7.1 or HCO₃⁻ <12 mEq/L) |
| Pulmonary oedema (volume overload) | IV furosemide (loop diuretic — converts oliguria, facilitates fluid management but does NOT improve outcome) |
| Sepsis-AKI | Broad-spectrum antibiotics; early goal-directed therapy |
| Contrast-induced AKI prophylaxis | IV N-acetylcysteine; adequate pre- and post-hydration; use iso-osmolar contrast |
| Hyperuricaemia (tumour lysis) | Rasburicase / allopurinol + aggressive hydration |
| Uremic bleeding | Desmopressin (DDAVP); dialysis |
| Anaemia | Erythropoiesis-stimulating agents (ESA) if prolonged; transfusion if severe |
Note: Dopamine ("renal dose") is NOT recommended — no proven benefit in AKI.
PART II — CHIRAKAARI VRIKKA-NISHKRIYATA (Chronic Renal Failure / Chronic Kidney Disease)
1. DEFINITION
Chronic Kidney Disease (CKD) is defined as abnormalities of kidney structure or function, present for >3 months, with implications for health.
Diagnostic criteria (either one for >3 months):
- GFR < 60 mL/min/1.73 m²
- Markers of kidney damage: albuminuria (≥30 mg/24h), abnormal urinary sediment, electrolyte abnormalities due to tubular disorders, structural abnormality on imaging, history of kidney transplantation
KDIGO Staging of CKD
| Stage | GFR (mL/min/1.73 m²) | Description |
|---|
| G1 | ≥90 | Normal/High (with markers of damage) |
| G2 | 60–89 | Mildly decreased |
| G3a | 45–59 | Mildly–moderately decreased |
| G3b | 30–44 | Moderately–severely decreased |
| G4 | 15–29 | Severely decreased |
| G5 | <15 | Kidney failure (ESKD); dialysis/transplant |
Albuminuria categories (A1: <30, A2: 30–300, A3: >300 mg/g) further risk-stratify.
2. ETIOPATHOGENESIS — CHART
Common Causes
CAUSES OF CKD (Global)
│
├── DIABETES MELLITUS (most common worldwide — ~40%)
│ └── Diabetic nephropathy: glomerulosclerosis (Kimmelstiel-Wilson lesion)
│ microalbuminuria → proteinuria → GFR decline
│
├── HYPERTENSION (~25–30%)
│ └── Hypertensive nephrosclerosis: afferent arteriolar thickening,
│ glomerular ischaemia, tubular atrophy, interstitial fibrosis
│
├── GLOMERULONEPHRITIS (~10–15%)
│ ├── IgA nephropathy, Focal segmental glomerulosclerosis (FSGS)
│ ├── Membranous nephropathy, Lupus nephritis
│ └── ANCA-associated vasculitis
│
├── HEREDITARY / GENETIC
│ ├── ADPKD (Autosomal Dominant Polycystic Kidney Disease)
│ └── Alport syndrome, Fabry disease
│
├── OBSTRUCTIVE NEPHROPATHY
│ └── Chronic BPH, renal calculi, posterior urethral valves
│
├── CHRONIC TUBULOINTERSTITIAL NEPHRITIS
│ └── Chronic analgesic use, heavy metals (lead, cadmium), sickle cell
│
└── RECURRENT AKI → progressive CKD
Pathogenetic Mechanism (Common Final Pathway)
Any Initiating Injury (DM, HTN, GN, etc.)
↓
Nephron loss → Compensatory hyperfiltration in remaining nephrons
↓
Intraglomerular hypertension → Glomerular hypertrophy
↓
Proteinuria → Tubulo-interstitial inflammation
↓
TGF-β activation → Fibroblast proliferation
↓
Glomerulosclerosis + Tubular atrophy + Interstitial fibrosis
↓
Further nephron loss → Self-perpetuating cycle
↓
End-Stage Kidney Disease (ESKD)
Key mediators of progression: Angiotensin II (intrarenal), TGF-β1, RAAS activation, oxidative stress, proteinuria itself (tubular toxicity), systemic and intraglomerular hypertension.
3. DIAGNOSIS
A. CLINICAL FEATURES
Early CKD (Stages 1–3): Usually asymptomatic; detected on screening (incidental lab findings).
Advanced CKD (Stages 4–5) — Uraemic Syndrome:
| System | Manifestations |
|---|
| General | Fatigue, anorexia, nausea, weight loss, pruritis |
| CVS | Hypertension, LVH, pericarditis, accelerated atherosclerosis, arrhythmias |
| CNS | Lethargy, cognitive impairment, peripheral neuropathy, restless leg syndrome, uraemic encephalopathy |
| GIT | Anorexia, nausea, vomiting, peptic ulceration, GI bleeding (platelet dysfunction) |
| Haematological | Normochromic normocytic anaemia (↓ EPO), bleeding tendency, thrombocytopenia |
| Musculoskeletal | Renal osteodystrophy (osteoporosis, osteomalacia, osteitis fibrosa cystica), fractures, myopathy |
| Endocrine | Hyperparathyroidism (secondary → tertiary), hypogonadism, amenorrhoea, impotence, hypothyroidism |
| Fluid/Electrolyte | Oedema, hyperkalaemia, hyperphosphataemia, hypocalcaemia, hypermagnesaemia, metabolic acidosis |
| Skin | Pallor (anaemia), uraemic frost (severe), pruritus, hyperpigmentation |
| Immune | Immunosuppression → susceptibility to infections |
B. INVESTIGATIONS
Blood Tests:
- Serum creatinine + eGFR (CKD-EPI or MDRD equation)
- BUN, electrolytes (K⁺ ↑, Na⁺ variable, phosphate ↑, calcium ↓)
- Bicarbonate ↓ (metabolic acidosis)
- CBC: normochromic normocytic anaemia; ↓ reticulocytes
- Serum PTH ↑ (secondary hyperparathyroidism), Vitamin D ↓
- Fasting lipids, blood glucose / HbA1c
- Serum albumin (marker of nutritional status/inflammation)
Urine Tests:
- Spot urine albumin:creatinine ratio (ACR) or protein:creatinine ratio (PCR) — performed twice
- Urinalysis: proteinuria, haematuria, casts
- 24-hour urine collection (when needed for GFR estimation)
Imaging:
- Renal ultrasound: bilateral small, echogenic kidneys (most CKD); loss of corticomedullary differentiation; exceptions: DM (kidneys may be normal/large early), ADPKD (markedly enlarged, cystic)
- DMSA scan: differential renal function, scarring
- CT KUB: structural anomalies, obstruction, calculi
Renal Biopsy: Indicated in CKD with suspected glomerular cause, unexplained rapid progression, or when nephrotic syndrome is present; generally avoided when kidneys are small.
ECG: Hyperkalaemic changes (peaked T waves, widened QRS, sine wave pattern).
4. PRINCIPLES OF MANAGEMENT
A. NON-PHARMACOLOGICAL
-
Dietary modification:
- Low protein diet (0.6–0.8 g/kg/day) — reduces uraemia and slows progression
- Sodium restriction (<2 g/day) — BP control, oedema
- Potassium restriction (if hyperkalaemic)
- Phosphate restriction (<800 mg/day); avoid phosphate-rich foods (dairy, nuts, processed food)
- Adequate caloric intake (35 kcal/kg/day)
- Fluid restriction (in advanced CKD)
-
Lifestyle modifications:
- Smoking cessation (independent risk factor for progression)
- Regular moderate exercise
- Weight reduction (BMI <25)
- Alcohol moderation
-
BP control target: <130/80 mmHg (or <125/75 if proteinuria >1 g/day)
-
Avoidance of nephrotoxins: NSAIDs, contrast dye, herbal nephrotoxins, aminoglycosides
-
Patient education & self-management: Home BP monitoring, understanding signs of decompensation, fluid balance logs
-
Renal Replacement Therapy (RRT) — when GFR <15 or symptomatic uraemia:
- Haemodialysis (HD): 3× weekly, 3–4 hours; requires arteriovenous fistula
- Peritoneal Dialysis (PD): CAPD or APD; home-based; better for residual renal function preservation
- Renal Transplantation: Treatment of choice for ESKD; best long-term outcomes
B. PHARMACOLOGICAL
| Problem | Drug / Strategy |
|---|
| Slow progression | ACE inhibitors / ARBs — reduce intraglomerular pressure, reduce proteinuria (first-line in DM-CKD and proteinuric CKD) |
| SGLT2 inhibitors (empagliflozin, dapagliflozin) — reduce CKD progression and cardiovascular events (now guideline-recommended) |
| Finerenone (non-steroidal MRA) — reduce CKD progression in DM |
| Hypertension | ACE inhibitors/ARBs (first-line); CCBs, beta-blockers as add-on |
| Anaemia | Erythropoiesis-stimulating agents (ESA — darbepoetin, epoetin); IV iron (if ferritin <200 µg/L or TSAT <20%) — target Hb 10–12 g/dL |
| Hyperphosphataemia | Calcium carbonate (calcium-based binders); Sevelamer (non-calcium); lanthanum carbonate; iron-based binders |
| Secondary HPT | Calcitriol (activated Vit D) or analogues (paricalcitol); Cinacalcet (calcimimetic — for tertiary HPT) |
| Metabolic acidosis | Sodium bicarbonate supplementation (target HCO₃⁻ ≥22 mEq/L) |
| Hyperkalaemia | Dietary restriction; loop diuretics; sodium/potassium exchange resins (patiromer, sodium zirconium cyclosilicate) |
| Oedema / volume overload | Loop diuretics (furosemide — higher doses needed as GFR falls); thiazides lose efficacy when GFR <30 |
| Dyslipidaemia | Statins (atorvastatin, rosuvastatin) — reduce CV events in CKD |
| Diabetes control | Metformin (discontinue if GFR <30); SGLT2 inhibitors (adjust for GFR); insulin; avoid nephrotoxic oral hypoglycaemics |
| Infections | Vaccinations: Influenza (annual), Pneumococcal, Hepatitis B |
| Renal bone disease | Phosphate binders + Vitamin D analogues + Cinacalcet; bisphosphonates (use with caution in CKD) |
PART III — AYURVEDIC PERSPECTIVE
Conceptual Mapping
| Modern Term | Ayurvedic Equivalent |
|---|
| Kidney | Vrikka (a pair; embryologically derived from Rakta + Meda dhatu) |
| Acute Renal Failure | Ashu Vrikka-Nishkriyata (sudden / rapid cessation of kidney function) |
| Chronic Renal Failure | Chirakaari Vrikka-Nishkriyata (prolonged, gradual decline of kidney function) |
| Urine formation channels | Mutravaha Srotas |
| Urinary bladder | Basti (also the main seat of Vata) |
| Waste filtration | Kleda-vahana (kleda = excess fluid/moist waste) |
Dosha-Dushya Analysis
Pradhana Dosha: Tridosha derangement, with Vata-Kapha predominance (especially in CRF); Pitta involvement in inflammatory/haemorrhagic causes.
Dushya (affected tissues/channels):
- Rakta dhatu (blood tissue) — kidney's embryological origin
- Meda dhatu (fat/lipid tissue) — Vrikka moolasthana
- Mutravaha Srotas — channels of urine formation/excretion
Srotodushti (channel pathology): Primarily Sanga (obstruction) → Vimargagamana (misdirection of flow)
ASHU VRIKKA-NISHKRIYATA — Etiopathogenesis (Samprapti)
NIDANA (Causative Factors):
├── Ahara: Ati-ruksha (excessively dry food), Kshara (alkaline/caustic substances),
│ Ati-lavana (excessive salt), Viruddha ahara, dehydrating foods
├── Vihara: Trauma, excessive exertion, haemorrhage, suppression of natural urges (vegadharana)
└── Vyadhi: Infections (jwara), toxins (visha), haemolysis, post-surgical states
↓
PURVARUPA (Prodromal signs):
Reduced urine output, lower back discomfort, fatigue
↓
SAMPRAPTI (Pathogenesis):
Nidana Sevana
↓
Vata-Pitta vitiation
(Vata: governs urine flow / filtration; Pitta: metabolic fire)
↓
Mutravaha Srotas Dushti (obstruction/damage)
↓
Kleda (fluid waste) fails to be eliminated
↓
Toxin accumulation (Ama formation) → Srotosanga
↓
Agnimandya (impaired metabolic fire) → further Ama
↓
Rapid Vrikka Kshaya (acute kidney dysfunction)
↓
RUPA (Manifestations):
Anuria/Oliguria, Shotha (oedema), Aruchi, Chardi, Bhrama,
Klama, Sandhi shoola (uremic musculoskeletal pain)
CHIRAKAARI VRIKKA-NISHKRIYATA — Etiopathogenesis (Samprapti)
NIDANA:
├── Ahara: Guru-Snigdha-Sheeta-Abhisyandi (heavy, oily, cold, congestive) foods
│ → Kapha/Meda vitiation; Ati-lavana-amla-teekshna → Rakta-Pitta vitiation
├── Vihara: Sedentary lifestyle, day-sleep (Divaswapna → Kapha accumulation)
├── Vyadhi: Madhumeha (diabetes), Raktachapa (hypertension), Mutrashmari (calculi),
│ repeated AKI episodes, Beejadushti (genetic factors / ADPKD)
└── Manasika: Chronic stress → Vata derangement
↓
SAMPRAPTI:
Nidana Sevana
↓
Tridosha vitiation (Vata-Kapha predominant)
↓
Rakta + Meda Dushti (primary dhatu affected — kidney's origin)
↓
Medovaha + Mutravaha Sroto Dushti (Srotosanga + Srotodushti)
↓
Agnimandya → Ama Utpatti (toxic metabolic byproducts)
↓
Progressive Vrikka Kshaya (nephron loss / fibrosis)
↓
Kleda accumulation (uraemic toxins, fluid retention)
↓
RUPA: Pandu (anaemia), Shopha (oedema), Aruchi, Chardi,
Mootravaha srotas dushti (oliguria/polyuria), Sarvangavedana,
Twaka rukshata (dry skin), Hrudroga (cardiovascular), Daurbalya
↓
Yapya/Asadhya (incurable/palliable) stage = ESKD
AYURVEDIC TREATMENT PRINCIPLES
Chikitsa Sutra (Treatment Goals)
Break the Samprapti → Achieve: Ama pachana + Sroto shodhana + Rakta prasadana + Kleda-medososhana + Doshic balance + Rasayana chikitsa
SHODHANA CHIKITSA (Bio-Purification / Panchakarma)
Indicated when the patient has adequate bala (strength); best in early-to-moderate stages.
1. Purva Karma (Preparatory Procedures)
| Procedure | Detail |
|---|
| Snehana (Internal/External Oleation) | Medicated ghee/oil (e.g., Mahatiktaka ghrita, Dhanwantaram taila) — liquefies and mobilises Ama |
| Swedana (Sudation) | Avgaha Sweda (medicated sitz bath with Punarnava kwatha, dashamoola) — particularly suited to renal conditions; opens Srotas, promotes elimination through skin |
2. Pradhana Karma (Main Procedures)
| Panchakarma | Relevance to Vrikka-Nishkriyata |
|---|
| Virechana (Purgation) | For Pitta-predominant/inflammatory AKI; eliminates Ama, Pitta; uses Trivrut leha, Eranda taila; clears Mutravaha srotas indirectly via Pakwashaya shodhana |
| Basti (Medicated Enema) | MOST IMPORTANT — Vata's primary seat is Pakwashaya (colon); Basti pacifies Vata, the dominant dosha in both AKI/CRF; achieves systemic Shodhana without over-taxing kidneys |
| → Niruha Basti (Kashaya Basti) | Punarnava Kwatha Basti; Dashamoola Kwatha Basti — decoction enema for Srotoshodhana |
| → Anuvasana Basti (Sneha Basti) | Dhanwantaram oil; Ksheerabala oil — nourishes, lubricates, Vata-shamaka |
| Abhyanga (Medicated Oil Massage) | Dhanwantaram taila, Ksheerabala taila — promotes circulation, Vata pacification |
| Virechana + Basti (Yoga Basti cycle) | 8-day cycle: 3 Anuvasana + 5 Niruha Basti — standard protocol in CRF management |
Note: Vamana (emesis) is generally contraindicated in severe renal failure with hypovolaemia. Raktamokshana (bloodletting — jalauka/leech therapy) may be considered in Pitta-dominant/inflammatory cases.
SHAMANA CHIKITSA (Palliative / Conservative Treatment)
Used alone in debilitated patients; used after Shodhana as maintenance.
Key Therapeutic Strategies
| Goal | Intervention |
|---|
| Ama pachana (Digest toxins) | Ginger (Shunti), Pippali, Haritaki, Trikatu churna |
| Mutral (Diuretic) | Punarnava, Gokshura, Varuna (Crataeva nurvala), Pashanabheda (Bergenia ligulata) |
| Srotoshodhana (Channel cleansing) | Manjistha, Chandana, Ushira (Vetiver) |
| Rakta prasadana (Blood purification) | Manjistha, Neem, Guduchi (Tinospora cordifolia) |
| Vata-Kapha Shamana | Punarnava, Shilajatu, Gokshura |
| Anti-inflammatory / nephroprotective | Guduchi (Tinospora cordifolia), Amalaki, Bhumyamalaki (Phyllanthus niruri) |
| Rasayana (Regenerative/Tonic) | Shilajatu, Chyawanprash, Ashwagandha, Punarnava mandura (for anaemia) |
Key Ayurvedic Formulations
| Formulation | Composition / Use |
|---|
| Punarnavashtaka Kashaya | Punarnava, dashamoola, ginger etc. — diuretic, anti-oedematous, Vata-Kapha shamaka |
| Gokshuradi Guggulu | Gokshura, Guggulu, Trikatu — mutral, anti-inflammatory, breaks Srotosanga |
| Varuna / Varunadya Kashaya | Crataeva nurvala — mutra-shodaka (urine purifier), dissolves calculi |
| Chandraprabha Vati | Multi-herbal — urinary tonic, metabolic regulator |
| Punarnava Mandura | Punarnava + Mandura (iron) — anaemia of CKD (renal anaemia / Pandu) |
| Mutrakrichhantaka Rasa | Rasa preparation — acute urinary obstruction/AKI with dysuria |
| Shilajatu (Asphaltum) | Rasayana — improves glomerular function, anti-oxidant, adaptogen |
| Bhumyamalaki (Phyllanthus niruri) | Hepato-nephroprotective — reduces proteinuria, antiviral |
| Guduchi Satva | Tinospora cordifolia extract — immunomodulator, anti-uraemic |
Specific Treatment of Ashu Vrikka-Nishkriyata (AKI)
| Phase | Ayurvedic Approach |
|---|
| Acute phase (Initiation/Oliguric) | Shodhana deferred; focus on: Ama pachana (Ginger, Haritaki), Sroto unblocking (Punarnavashtaka), IV fluid equivalent = Yavagu (rice gruel), light easily digestible diet; Vastika dravyas (diuretics) cautiously |
| Diuretic phase | Rasayana + rehydration; Balya (strengthening) therapy begins |
| Recovery | Rasayana (Chyawanprash, Ashwagandha), dietary restoration, Yoga/Pranayama |
Specific Treatment of Chirakaari Vrikka-Nishkriyata (CRF/CKD)
| Stage | Ayurvedic Approach |
|---|
| Early (G1-G2) | Nidana Parivarjana (remove causative factors); Pathya Ahara-Vihara; Mutral + Rasayana; Shodhana (if bala adequate) |
| Moderate (G3) | Basti (Yoga basti), Virechana; Shamana — Punarnava, Gokshura, Guduchi, Chandraprabha; Manage Pandu with Punarnava Mandura |
| Advanced (G4-G5) | Primarily Shamana + Rasayana; Basti (Matra Basti with small quantities of medicated oil — safer); Ahara and Vihara adjustments; Integrate with dialysis if on RRT |
| ESKD | Palliative Ayurveda — symptom relief (pruritus: medicated oil massage; nausea: ginger; fatigue: Ashwagandha); supportive alongside RRT/transplant |
Pathya (Recommended Diet & Lifestyle)
- Light, warm, easily digestible food (Laghu, Ushna Ahara)
- Yava (barley), Old rice (Purana shali), Moong dal
- Bitter vegetables (karela/bitter gourd — Tikta rasa cleanses Rakta/Pitta)
- Avoid: Excess salt (Lavana), sour (Amla), heavy (Guru), cold, processed, dairy (Abhisyandi)
- Adequate hydration (unless oliguric)
- Mild Yoga: Pranayama (Anulom-Vilom), Bhujangasana, Setu Bandhasana
- Avoid: Divaswapna (day sleep), holding natural urges, excessive exertion
Summary Comparison Table
| Feature | Ashu Vrikka-Nishkriyata (ARF/AKI) | Chirakaari Vrikka-Nishkriyata (CRF/CKD) |
|---|
| Onset | Sudden (hours–days) | Gradual (>3 months) |
| Reversibility | Potentially reversible | Usually irreversible; progressive |
| Kidney size (USG) | Normal to enlarged | Small, echogenic |
| Creatinine | Rapidly rising | Chronically elevated |
| Anaemia | Mild/absent (acute) | Prominent (↓ EPO) |
| Osteodystrophy | Absent | Present (secondary HPT) |
| Ayurvedic predominant dosha | Vata-Pitta | Vata-Kapha |
| Primary Shodhana | Basti (Niruha + Anuvasana) | Basti (Yoga Basti) + Virechana |
| Key herbs | Punarnava, Varuna, Gokshura | Punarnava, Gokshura, Guduchi, Shilajatu |
| Rasayana | Post-recovery phase | Central to long-term management |
| RRT equivalent | Acute Basti + Virechana (elimination) | Dialysis + Basti (maintenance) |
Sources: Sabiston Textbook of Surgery 21e, National Kidney Foundation Primer on Kidney Diseases 8e, Brenner & Rector's The Kidney 2-Volume Set, KDIGO AKI Guidelines 2012; Ayurvedic content synthesized from IJCRT 2024 (Pathogenesis of CKD in Ayurveda), WJPLS 2025 (Vrikka Vikara management), DOAJ case reports on Shodhana-Shamana in CKD.