Causes of bradycardia
Reading File
Finding Sources
Finding Sources
Searching PubMed
bradycardia etiology causes
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Loading Image
Here is a comprehensive overview of the causes of bradycardia, synthesized from multiple authoritative sources.
Causes of Bradycardia
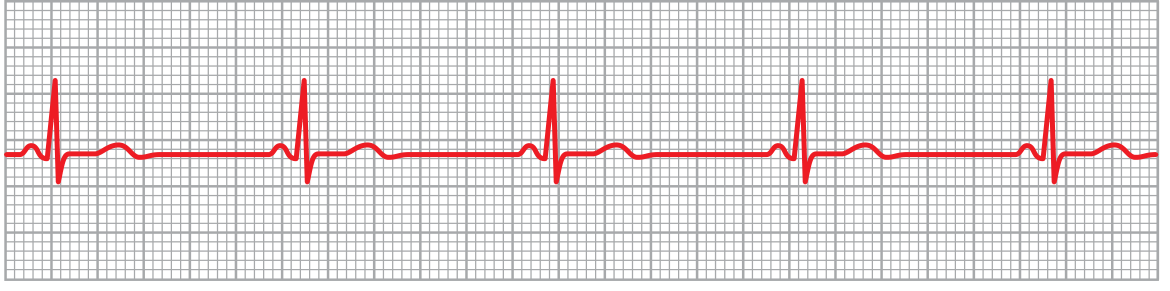
Definition: Heart rate < 60 beats/min. On ECG, sinus bradycardia shows normal P-wave morphology with a fixed P-P interval equal to the R-R interval and a ventricular rate below 60 bpm.
Figure: Sinus bradycardia (Lead III) — Guyton and Hall Textbook of Medical Physiology
1. Physiological (Normal) Causes
| Cause | Mechanism |
|---|---|
| Athletic training | Increased stroke volume triggers baroreceptor-mediated vagal reflexes; downregulation of If ("funny current") ion channels in the SA node reduces intrinsic pacemaker activity |
| Sleep | Dominant vagal tone at rest; sinus bradycardia and pauses during sleep are typically not an indication for pacing |
| High resting vagal tone in young adults | Normal variant |
— Guyton and Hall Textbook of Medical Physiology; Rosen's Emergency Medicine
2. Intrinsic (Structural/Cardiac) Causes
These reflect direct damage or disease of the SA node or conduction system:
| Cause | Notes |
|---|---|
| Idiopathic degeneration (aging) | Most common cause of sick sinus syndrome |
| Ischemia / Infarction | Particularly right coronary artery territory (supplies SA node); acute inferior MI |
| Cardiomyopathy | Dilated, hypertrophic |
| Infiltrative diseases | Sarcoidosis, amyloidosis, hemochromatosis |
| Collagen vascular diseases | SLE, rheumatoid arthritis, scleroderma |
| Infectious diseases | Endocarditis, Lyme disease, Chagas disease |
| Congenital disorders | May present later in life |
| Surgical trauma | Valve surgery, cardiac transplantation |
| Myocarditis | Inflammatory damage to SA node |
— The Washington Manual of Medical Therapeutics
3. Extrinsic / Autonomically Mediated Causes
Enhanced vagal tone suppresses SA node firing:
| Cause | Mechanism |
|---|---|
| Carotid sinus hypersensitivity | Hypersensitive baroreceptors; external neck pressure can cause profound bradycardia or even cardiac arrest and syncope |
| Neurocardiogenic (vasovagal) syncope | Reflex vagal surge |
| Valsalva maneuver / raised ICP | Cushing reflex (bradycardia + hypertension + irregular respiration) |
| Visceral reflexes | Coughing, vomiting, micturition, defecation, intubation, ocular pressure (oculocardiac reflex) |
| Acute inferior/posterior MI | Bezold-Jarisch reflex |
| Hemoperitoneum | Vagal stimulation |
4. Drug-Induced Causes
Among the most common, and importantly reversible:
| Drug Class | Examples |
|---|---|
| β-adrenergic blockers | Metoprolol, atenolol, propranolol |
| Non-dihydropyridine calcium channel blockers | Verapamil, diltiazem |
| Digoxin | Enhances vagal tone; slows AV conduction |
| Antiarrhythmics | Amiodarone, sotalol, flecainide |
| Dexmedetomidine | α2 agonist; especially problematic in children |
| Succinylcholine | Muscarinic activation; common in pediatric anesthesia |
| Sevoflurane / Halothane | Particularly problematic in trisomy 21 and CHD patients |
| Opioids | Vagotonic effect |
| Cholinesterase inhibitors | Neostigmine, physostigmine |
| SSRIs | Associated with minor sinoatrial node dysfunction |
— Washington Manual; Miller's Anesthesia; Barash Clinical Anesthesia; Kaplan & Sadock's Psychiatry
5. Metabolic / Systemic Causes
| Cause | Mechanism |
|---|---|
| Hypothyroidism | Reduces cardiac automaticity and conduction |
| Hypothermia | Slows all metabolic processes including SA node firing |
| Hyperkalemia | Depolarization block of cardiac membranes |
| Hypermagnesemia | Calcium channel antagonism |
| Hypoxia | Direct SA node depression |
| Hypercarbia | Elevated CO2 with autonomic effects |
| Obstructive sleep apnea (OSA) | High vagal tone during apneic events; a common reversible cause |
| Sepsis | Autonomic dysregulation |
6. Neurological Causes
| Cause | Notes |
|---|---|
| Raised intracranial pressure | Cushing reflex |
| Spinal cord injury (above T1–T6) | Loss of sympathetic outflow → unopposed vagal tone |
| Autonomic neuropathy | Diabetic or other causes |
Quick Reference: Intrinsic vs. Extrinsic
BRADYCARDIA
├── INTRINSIC (structural heart/conduction disease)
│ ├── Idiopathic degeneration
│ ├── Ischemia/infarction
│ ├── Infiltrative (sarcoid, amyloid, hemochromatosis)
│ ├── Collagen vascular disease
│ ├── Infectious (Lyme, Chagas, endocarditis)
│ └── Surgical/congenital
│
└── EXTRINSIC (reversible)
├── Drugs (β-blockers, CCBs, digoxin, antiarrhythmics)
├── Autonomic (vagal, neurocardiogenic, carotid sinus)
├── Metabolic (hypothyroidism, hypothermia, electrolytes)
├── Hypoxia / hypercarbia
└── Sleep apnea / neurological
Clinical Pearl: Always Rule Out Reversible Causes First
Before attributing bradycardia to intrinsic sinus node disease, reversible causes must be excluded — particularly hypothyroidism, rate-slowing medications, electrolyte disturbances, sleep apnea, and acute ischemia. — Harrison's Principles of Internal Medicine, 22nd Ed. (2025)
Recent literature note: A 2025 review in Am J Emerg Med (Tannenbaum & Long, PMID 40683036) confirms the same core etiologic framework, with emphasis on ECG-based diagnosis and systematic approach to reversible causes in the ED setting.
This is a shared conversation. Sign in to Orris to start your own chat.