Bimanual palpation
Reading File
Finding Sources
Finding Sources
Searching Images
bimanual palpation technique
Reading File
Reading File
Reading File
Finding Sources
Searching Images
bimanual pelvic examination uterus adnexa technique
Loading Image
Finding Sources
I now have comprehensive information to provide a detailed answer on bimanual palpation across all its clinical applications.
Bimanual Palpation
Bimanual palpation is a physical examination technique in which both hands are used simultaneously — one as an active palpating hand and one as a passive supporting or opposing hand — to assess underlying structures. It is applied in multiple clinical contexts.
1. Gynecologic Pelvic Examination
The most classic application. The examiner places one or two fingers into the vagina (the internal hand) and the other hand on the lower abdominal wall (external hand), coordinating both to outline the pelvic organs.
Technique (step-by-step)
- Insert the well-lubricated index finger (and middle finger if accommodated) into the vagina at the posterior aspect near the perineum. Test perineal strength by pressing downward and asking the patient to bear down — this can reveal a concealed cystocele, rectocele, or uterine descensus.
- Advance fingers along the posterior wall to the cervix. Note any structural abnormalities or tenderness.
- Apply external hand gently on the infraumbilical area, pressing downward to sweep pelvic structures toward the internal fingers. Evaluate the uterus for:
- Position (anteverted/retroverted)
- Architecture, size, shape, symmetry
- Consistency
- Tenderness
- Mobility
- Evaluate the cervix for position, consistency, and cervical motion tenderness (CMT). Assess anterior, posterior, and lateral fornices.
- Adnexal assessment: Place internal fingers in the right lateral fornix and the abdominal hand on the right lower quadrant. A normal tube is not palpable; a normal ovary (~4 × 2 × 3 cm) is often not palpable. If an adnexal mass is found, document its location relative to uterus, consistency, tenderness, and mobility. Repeat on the left.
- Rectovaginal examination: Index finger in vagina, middle finger in rectum — allows higher pelvic exploration beyond the cul-de-sac. Mandatory to complete the exam.
- Intact hymen: Use the rectal-abdominal technique instead.
The number of vaginal fingers should be based on patient comfort, vaginal pliability, and body habitus. Adolescent, slender, and older patients are often better examined with a single-finger technique.
— Berek & Novak's Gynecology
2. Spleen Palpation
For bimanual palpation of the spleen, the patient is supine with flexed knees:
- The left hand is placed on the lower left rib cage and pulls skin toward the costal margin
- The right hand fingertips feel the tip of the spleen as it descends during deep, slow inspiration
- Begin in the left lower quadrant and move gradually toward the left costal margin
- Record splenic tip as centimeters below the left costal margin (measured from umbilicus or xiphisternal junction) for serial comparisons
Bimanual palpation in the right lateral decubitus position adds nothing to the supine examination.
— Harrison's Principles of Internal Medicine, 22E
3. Oral Cavity / Floor of Mouth
One finger is placed intraorally and the opposing hand palpates externally through the cheek or submental region. Used to:
- Identify premalignant or malignant lesions of the cheeks and floor of mouth (especially in tobacco/smokeless tobacco users)
- Detect sialoliths in the submandibular (Wharton's) duct or parotid (Stensen's) duct
- Assess sublingual gland tumors for extent and fixation to the mandible
- Evaluate submandibular swellings for tenderness, consistency, and fluctuance
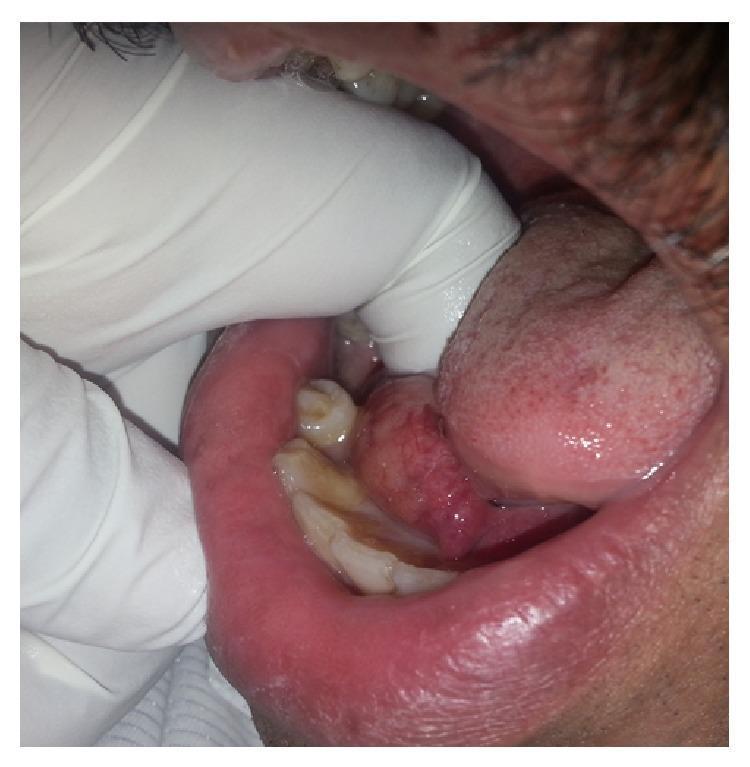
— Goldman-Cecil Medicine; Cummings Otolaryngology
4. Other Clinical Applications
| Site | Purpose |
|---|---|
| Pancreatic head | After Kocher maneuver during laparotomy — assess for masses prior to resection |
| Lungs (open thoracotomy) | Identify occult pulmonary metastases not visible on imaging (reason VATS was historically considered inferior to open thoracotomy for metastasectomy) |
| Neck lymph nodes | Mandatory in head and neck cancer to assess nodal status and potential regional metastasis |
| Oral cavity (head/neck SCC workup) | All subsites including oral tongue, floor of mouth, gingiva |
Key Principles
- Coordination between both hands is essential — one hand creates a platform or guides structures while the other actively palpates
- In pelvic examination, the internal hand guides while the external hand provides the primary diagnostic pressure
- Always start gently and increase pressure progressively
- Document findings in relation to fixed anatomical landmarks (e.g., costal margin, umbilicus, cervix) to allow reproducible comparison
This is a shared conversation. Sign in to Orris to start your own chat.