foreign body in child nostril
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
Here is a comprehensive clinical overview of nasal foreign bodies in children, drawn from Tintinalli's Emergency Medicine and The Harriet Lane Handbook.
Nasal Foreign Body in Children
Epidemiology & Common Objects
- Nasal foreign bodies are almost exclusively a pediatric problem; children who insert nasal objects tend to be younger than those with ear foreign bodies.
- Common objects: beads, paper, rocks, toy parts, and organic material (peas, corn, seeds, nuts, legumes).
- Most children are asymptomatic at presentation.
Clinical Features
| Feature | Frequency |
|---|---|
| Local pain | 23–55% |
| Nasal discharge | 7–36% |
| Epistaxis | Variable |
| Parent witnessed insertion | Variable |
Key diagnostic clue: Persistent, unilateral, purulent, foul-smelling nasal discharge in a child of appropriate age — maintain a high index of suspicion for a retained foreign body.
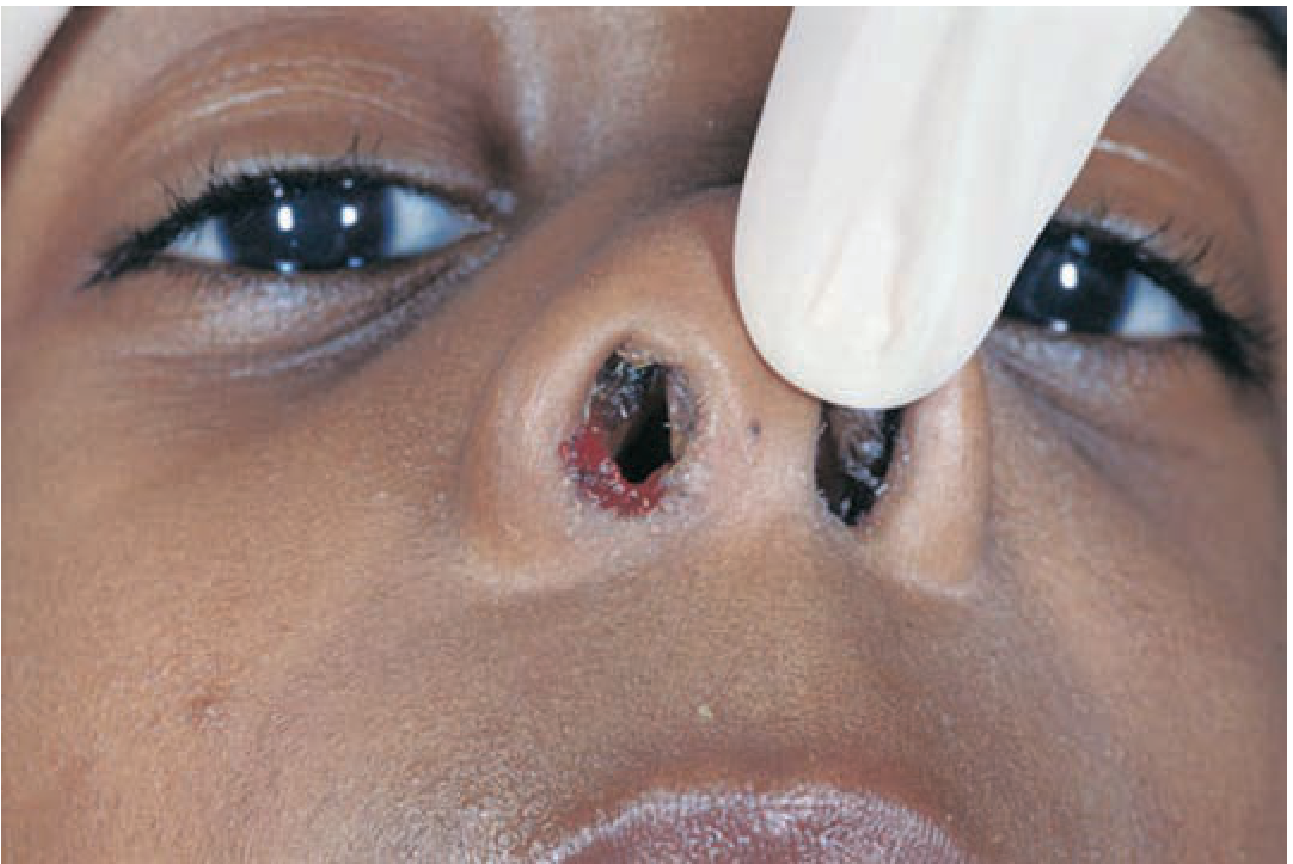
A 6-year-old presenting with serosanguineous nasal discharge from a retained button (inserted ~1 week prior). — Tintinalli's Emergency Medicine
Diagnosis
- Most foreign bodies can be directly visualized.
- If not visible (e.g., obscured by mucopurulent discharge/edema), consider a plain radiograph to characterize the object — especially if a button battery is suspected.
Treatment
Step 1 — Positive Pressure Techniques (First Line)
Try these before any instrumentation. Successful in >50% of cases.
| Technique | Details |
|---|---|
| Self-removal (nose blowing) | Effective in children >3 years; occlude unaffected nostril and blow |
| Parent kiss | Up to 60% success rate. Caregiver covers child's mouth, occludes unaffected nostril with one finger, delivers a single forceful puff of air |
| Bag-valve mask | Used similarly to the parent kiss |
| High-flow oxygen | Best for objects that completely occlude the anterior nasal cavity; 10–15 L/min through suction tubing placed in the unobstructed nostril |
Step 2 — Pretreatment Before Instrumentation
- Topical 1% lidocaine + 0.5% phenylephrine (vasoconstrictor) to reduce mucosal edema and minimize bleeding.
- Note: Phenylephrine should be avoided topically in children < 6 years old unless bleeding is refractory to other measures.
- Immobilization is critical — ~20% of children require procedural sedation (most commonly ketamine).
Step 3 — Instrumentation (for non-occlusive or non-expellable objects)
| Tool | Best for |
|---|---|
| Alligator forceps | Compressible, rough-surfaced, anteriorly located objects |
| Right-angle hook | Smooth objects that cannot be easily grasped |
| Foley catheter (5–8 Fr) | Small, round objects (e.g., marble); advance past object, inflate balloon, withdraw |
| Suction catheter | Soft or friable objects |
⚠️ If the object is friable, pulling with forceps risks leaving fragments behind. ⚠️ Do not irrigate if the object is organic/expandable (rice, sponge, vegetable matter) — swelling will impede removal.
Special Considerations
🔴 Button Batteries — EMERGENT
- Can cause liquefactive necrosis and septal perforation in as little as 7 hours.
- Do NOT instill any nasal drops before removal — electrolyte-rich fluid causes electrolysis → severe alkaline burn.
- Remove immediately; refer to ENT if not visible or initial attempt fails.
Magnets
- Magnets attached to the nasal septum also require emergent removal.
Live Insects
- Kill first with 2% lidocaine or mineral oil, then attempt removal.
Complications
- Epistaxis
- Mucosal laceration
- Septal perforation (rare)
- Aspiration (rare)
- Retained foreign object → rhinosinusitis, mucosal/septal necrosis
- Cribriform plate perforation (rare, with deep probing)
When to Refer to ENT (Otolaryngology)
- Posterior objects not reachable anteriorly
- Button batteries or penetrating injuries
- Unsuccessful initial attempt(s)
- Anatomic abnormalities
Sources: Tintinalli's Emergency Medicine: A Comprehensive Study Guide; The Harriet Lane Handbook, 23rd ed. (Johns Hopkins Hospital)
This is a shared conversation. Sign in to Orris to start your own chat.