Tell me about perineum
Reading File
Finding Sources
Searching the Web
perineum anatomy clinical significance
Reading File
Reading File
Searching Images
perineum anatomy triangles muscles
Reading File
Reading File
Reading File
Loading Image
Here is a comprehensive overview of the perineum based on Gray's Anatomy for Students and Campbell-Walsh-Wein Urology.
The Perineum
Definition & Location
The perineum is a diamond-shaped region positioned inferiorly to the pelvic floor, between the thighs. Its peripheral boundary is the pelvic outlet; its ceiling is the pelvic diaphragm (levator ani and coccygeus muscles). — Gray's Anatomy for Students
Bony Boundaries
The corners of the diamond are defined by palpable landmarks:
- Anterior: inferior border of the pubic symphysis
- Posterior: tip of the coccyx
- Lateral (×2): ischial tuberosities
The lateral margins are formed by the ischiopubic rami anteriorly and the sacrotuberous ligaments posteriorly.
Division into Two Triangles
An imaginary transverse line between the two ischial tuberosities divides the perineum into two triangles. Importantly, these triangles are not coplanar — the urogenital triangle lies in a more horizontal plane, while the anal triangle tilts upward to face more posteriorly.
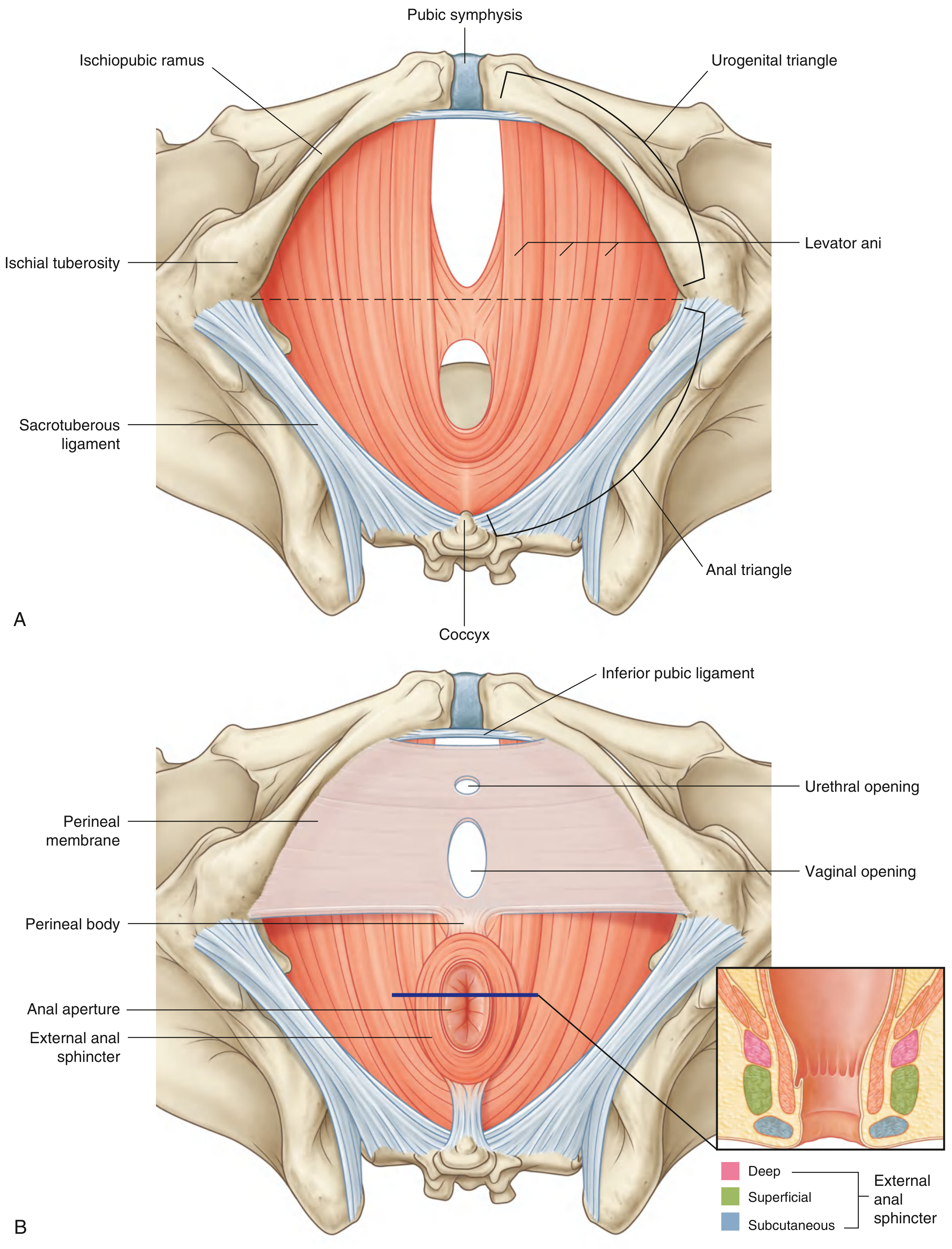
1. Urogenital Triangle (Anterior)
- Function: Anchors the external genitalia; contains openings of the urinary and reproductive tracts
- Subdivided by the perineal membrane into:
| Space | Contents |
|---|---|
| Deep perineal pouch (superior to membrane) | External urethral sphincter, deep transverse perineal muscles, bulbourethral glands (males), urethrovaginalis (females) |
| Superficial perineal pouch (inferior to membrane) | Ischiocavernosus, bulbospongiosus, superficial transverse perineal muscles; roots of external genitalia; vestibular bulbs + Bartholin's glands (females) |
The perineal membrane is a thick fibrous sheet spanning the urogenital triangle, anchored posteriorly to the perineal body.
2. Anal Triangle (Posterior)
- Contains the anus and external anal sphincter
- On either side of the anus lies an ischio-anal fossa — a fat-filled, wedge-shaped space that permits movement of the pelvic diaphragm during defecation
- The external anal sphincter has three parts: deep, superficial, and subcutaneous
The Perineal Body (Central Tendon)
A critical fibromuscular node at the midline, located between the vagina (or root of penis) and the anus. Multiple muscles converge here:
- Bulbospongiosus
- External anal sphincter
- Superficial and deep transverse perineal muscles
- Contributions from levator ani
Clinical importance: Damage during vaginal delivery can disrupt the external anal sphincter fibers → fecal incontinence. Episiotomy is deliberately angled laterally to avoid these fibers. — Campbell-Walsh-Wein Urology
Superficial Perineal Muscles
| Muscle | Attachments/Function |
|---|---|
| Ischiocavernosus | Covers the crura of clitoris/penis; maintains erection by compressing the crus |
| Bulbospongiosus | In females: surrounds vaginal orifice, covers vestibular bulbs, expresses Bartholin's gland secretions. In males: wraps the bulb and corpus spongiosum |
| Superficial transverse perineal | Runs transversely from ischial tuberosity to perineal body; stabilizes the perineal body |
Ischio-Anal Fossae
Inverted wedge-shaped fat-filled spaces flanking the anal canal. Their anterior recesses extend forward into the urogenital triangle above the deep perineal pouch. These spaces communicate across the midline behind the anal canal (important for spread of infection).
Clinical note: Anal mucosa is vulnerable to tears from hard feces. Infection can track laterally into the ischio-anal fossae, producing ischio-anal abscesses or intersphincteric fistulas. — Gray's Anatomy for Students
Neurovascular Supply
| Structure | Detail |
|---|---|
| Primary nerve | Pudendal nerve (S2–S4) — enters via lesser sciatic foramen, travels in Alcock's canal |
| Primary artery | Internal pudendal artery (branch of internal iliac) |
| Sensory | Pudendal nerve branches carry sensation from external genitalia |
| Erection | Parasympathetic fibers from pelvic splanchnic nerves (S2–S4) → relaxation of arteries → engorgement of erectile tissues |
Sex Differences
| Feature | Female | Male |
|---|---|---|
| Urogenital hiatus | Transmits urethra and vagina | Transmits urethra only |
| External genitalia | Clitoris, labia, vestibular bulbs, Bartholin's glands | Penis, scrotum, bulbourethral glands in deep pouch |
| Perineal body | Posterior to vaginal opening | Between bulb of penis and anus |
| Bulbospongiosus | Splits to surround introitus | Encircles corpus spongiosum |
Key Clinical Correlations
- Perineal tears / episiotomy during childbirth — most common cause of perineal body damage → pelvic organ prolapse, urinary/fecal incontinence
- Pudendal nerve block — injected near the ischial spine; anesthetizes most of the perineum for obstetric and anorectal procedures
- Ischio-anal abscess / fistula-in-ano — infection spreads through the ischio-anal fat; may cross to the contralateral side (horseshoe abscess)
- Urethral injuries — straddle injuries or pelvic fractures can rupture the urethra in the deep perineal pouch; extravasation of urine is contained by Colles' fascia (spreads into scrotum/labia, penis, lower anterior abdominal wall — but not thighs or buttocks due to fascial attachments)
- Bartholin's gland cysts/abscesses — arise from blocked ducts in the superficial perineal pouch; treated by marsupialization
Sources: Gray's Anatomy for Students; Campbell-Walsh-Wein Urology, 12th ed.; Berek & Novak's Gynecology
This is a shared conversation. Sign in to Orris to start your own chat.