Poly angitis
Reading File
Finding Sources
Searching PubMed
"granulomatosis with polyangiitis" OR "microscopic polyangiitis" management
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Now I have comprehensive information from multiple textbooks. Let me compile a thorough answer on the polyangiitides.
Polyangiitis — Overview of the Three Major ANCA-Associated Vasculitides
"Polyangiitis" encompasses a spectrum of necrotizing vasculitic diseases. The three main forms are:
- Granulomatosis with Polyangiitis (GPA) — formerly Wegener granulomatosis
- Microscopic Polyangiitis (MPA)
- Eosinophilic Granulomatosis with Polyangiitis (EGPA) — formerly Churg-Strauss syndrome
All three are ANCA-associated vasculitides (AAV) involving small (and sometimes medium-sized) vessels with pauci-immune deposits.
1. Granulomatosis with Polyangiitis (GPA)
Pathology
A necrotizing granulomatous vasculitis of small and medium-sized vessels. GPA encompasses all features of MPA plus additional manifestations from necrotizing granulomatous inflammation.
— Goldman-Cecil Medicine, Chapter 249
Classic Triad
- Upper respiratory tract involvement (sinusitis, nasal ulceration, epistaxis, saddle-nose deformity)
- Lower respiratory tract (cavitary pulmonary nodules, hemoptysis)
- Renal disease (pauci-immune crescentic glomerulonephritis)
Other Features
- Subglottic stenosis (hoarseness, stridor)
- Orbital pseudotumor
- Scleritis/episcleritis (much more common than in MPA)
- Skin: palpable purpura, ulcers (Fig. 139-7), papules on extensor surfaces, subcutaneous nodules
- Peripheral neuropathy, CNS, cardiac involvement
ANCA
- C-ANCA / anti-PR3 (proteinase-3): present in ~70–90% of systemic disease; ~70% in disease restricted to upper airway
- P-ANCA/anti-MPO also possible but less common
Diagnosis
Three of six criteria in children: (1) renal involvement, (2) upper airway involvement, (3) pulmonary infiltrates/nodules/cavities, (4) laryngo-tracheobronchial stenosis, (5) granulomatous inflammation, (6) ANCA positivity.
— Brenner and Rector's The Kidney
2. Microscopic Polyangiitis (MPA)
Pathology
Nongranulomatous necrotizing vasculitis with few or no immune deposits, affecting small (and possibly medium-sized) vessels. Many cases previously diagnosed as polyarteritis nodosa are now properly reclassified as MPA.
Key Features
- Rapidly progressive glomerulonephritis (pauci-immune) — most common serious manifestation
- Pulmonary hemorrhage / diffuse alveolar hemorrhage
- Peripheral and cranial neuropathy
- Constitutional symptoms (fever, weight loss, arthralgia) — often a prolonged prodrome
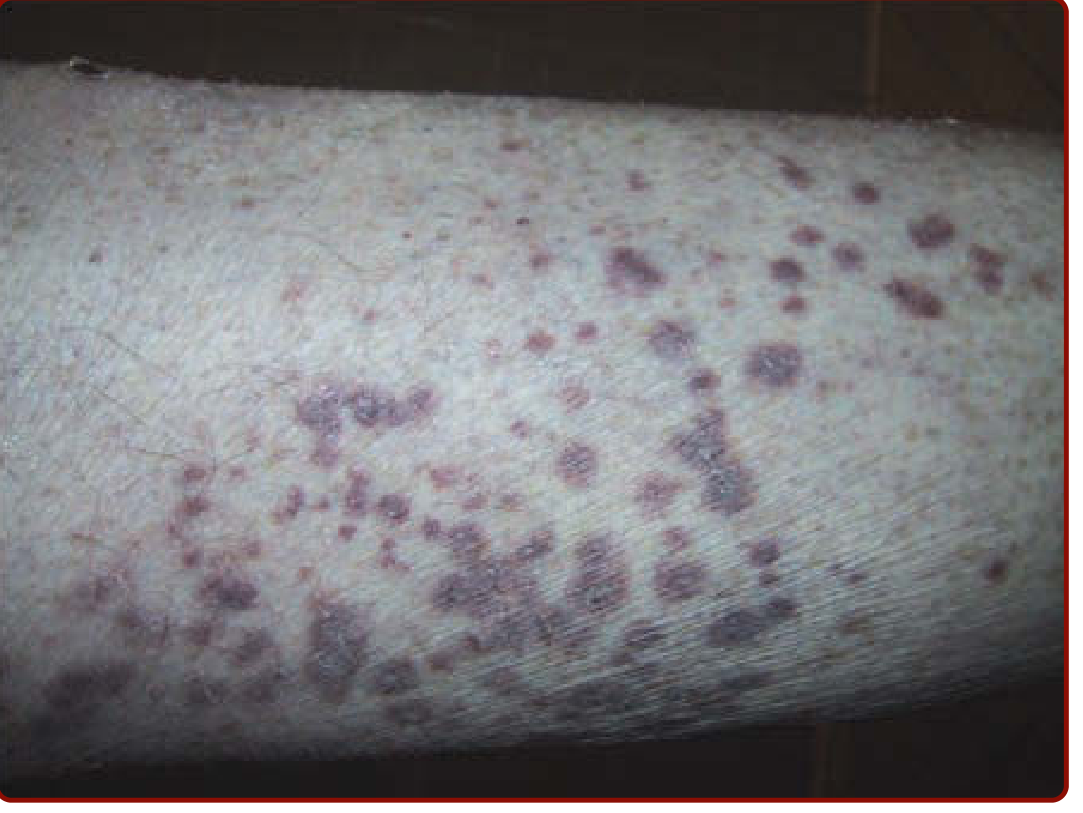
- Skin: palpable purpura (most common cutaneous lesion); rarely livedo reticularis, digital ischemia, deep ulcers from medium-vessel involvement
Differentiating MPA from GPA
| Feature | MPA | GPA |
|---|---|---|
| Granulomatous inflammation | Absent | Present |
| Upper airway disease | Mild/absent | Prominent (>90%) |
| ANCA positivity | ~70% | 70–90% |
| Predominant ANCA type | P-ANCA / MPO | C-ANCA / PR3 |
| Cavitary lung nodules | Rare | Common |
| Orbital pseudotumor | No | Yes |
ANCA
- P-ANCA / anti-MPO (myeloperoxidase) → perinuclear fluorescence pattern
3. Eosinophilic Granulomatosis with Polyangiitis (EGPA)
Pathology
An eosinophil-rich granulomatous inflammation of the respiratory tract with necrotizing vasculitis of small to medium-sized vessels.
Three Clinical Phases
| Phase | Features |
|---|---|
| Prodromal | Allergic asthma, allergic rhinitis (may last years) |
| Eosinophilic-tissue infiltration | High peripheral eosinophilia; eosinophilic infiltration of lung, GI tract, other organs |
| Vasculitic | Systemic necrotizing vasculitis — heart, lungs, peripheral nerves, skin |
Hallmarks
- Asthma (often severe, late-onset)
- Eosinophilia (markedly elevated)
- ~50% ANCA-positive (usually anti-MPO/P-ANCA)
Treatment
All three AAV forms share a common therapeutic framework:
Induction of Remission
| Agent | Role |
|---|---|
| Glucocorticoids | Cornerstone; initial high-dose (1–2 mg/kg/day oral or IV methylprednisolone boluses) |
| Rituximab (anti-CD20) | Preferred over cyclophosphamide for most patients; superior for relapsing disease |
| Cyclophosphamide | IV (500–750 mg/m²) or oral; used in severe/organ-threatening disease |
| Avacopan (C5a receptor blocker) | Glucocorticoid-sparing add-on to rituximab or cyclophosphamide |
| Methotrexate | Alternative induction in mild disease (no GN, Cr <150 µmol/L) |
| Plasmapheresis (PLEX) | Diffuse pulmonary hemorrhage or RPGN approaching dialysis |
Maintenance of Remission
- Gradual glucocorticoid taper
- Rituximab (500 mg or 1 g every 4–6 months) — now preferred maintenance
- Azathioprine or methotrexate as alternatives
EGPA-Specific
- Mepolizumab (anti-IL-5) 300 mg SC monthly — important glucocorticoid-sparing role
- Mild disease: prednisone alone
- Severe (cardiac, neuro, renal, GI involvement): add cyclophosphamide or rituximab
Treatment Principles
- Aim for remission rapidly, then switch to safer maintenance agents
- Monitor for glucocorticoid toxicity and opportunistic infections
- Pneumocystis pneumonia prophylaxis is an important part of many AAV regimens — Goldman-Cecil Medicine; Brenner and Rector's The Kidney
Prognosis
- GPA/MPA: Remission achieved in the majority; renal dysfunction may persist even after remission; ~25–50% relapse rate
- EGPA: >90% achieve clinical remission; majority cannot discontinue glucocorticoids entirely due to persistent asthma; ~25% relapse
Recent guideline update: The 2025 British Society for Rheumatology ANCA-associated vasculitis recommendations (PMID 40499922) provides the most current management guidance and may contain updates beyond the textbook content above.
This is a shared conversation. Sign in to Orris to start your own chat.