Mitral stenosis medicine notes along with the homeopathic approach.
Reading File
Finding Sources
Searching the Web
mitral stenosis homeopathic treatment remedies
Searching PubMed
"mitral stenosis"[MeSH Terms] AND management
Reading File
Reading File
Reading Web Page
mitral stenosis homeopathic remedies treatment
Finding Sources
Searching Images
mitral stenosis echocardiography chest X-ray diagram
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
I now have comprehensive information from Harrison's, Braunwald's, and Fuster & Hurst's, along with homeopathic sources. Let me compile the complete notes.
Mitral Stenosis — Complete Medicine Notes with Homeopathic Approach
OVERVIEW
Mitral stenosis (MS) is a narrowing of the mitral valve orifice that obstructs blood flow from the left atrium (LA) to the left ventricle (LV) during diastole. Normal mitral valve area (MVA) is 4–6 cm². Symptoms typically appear when MVA falls below 2 cm², and severe obstruction exists at <1.5 cm² (critical: <1.0 cm²).
ETIOLOGY
| Cause | Notes |
|---|---|
| Rheumatic fever (most common) | ~90% of cases; group A β-hemolytic streptococcal infection triggers autoimmune valve damage; 3:1 female preponderance |
| Degenerative (Mitral Annular Calcification) | Increasing in developed nations; age-related; more in older women |
| Congenital MS | Rare; parachute mitral valve, supravalvular ring |
| Infective endocarditis | Vegetation rarely causing obstruction |
| Radiotherapy-induced MS | Fibrotic commissural fusion post-thoracic radiation |
Epidemiology: ~39 million cases of rheumatic heart disease worldwide; MS prevalent in developing nations (20–30/1000 school children on echo screening). In developed nations, prevalence is 0.02% due to antibiotic prophylaxis and improved socioeconomic conditions. — Fuster & Hurst's The Heart, 15th Ed.
PATHOPHYSIOLOGY
The sequence of hemodynamic events:
- Commissural fusion, leaflet thickening & calcification → ↓ MVA
- Persistent diastolic pressure gradient across the mitral valve (LA > LV)
- Left atrial enlargement and elevated LA pressure
- Pulmonary venous hypertension → pulmonary edema (dyspnea)
- Reactive pulmonary arterial hypertension (PAH) → RV hypertrophy and failure
- LA dilation + stasis → atrial fibrillation (AF) and thromboembolism (stroke)
Key hemodynamic formulae:
- Transmitral gradient increases with tachycardia (less diastolic filling time)
- CO can be normal at rest but fails to increase with exercise
- MVA by pressure half-time (PHT): MVA = 220 / PHT
The "fish mouth" appearance of the stenotic valve on gross pathology is characteristic (shown in Fuster & Hurst below).
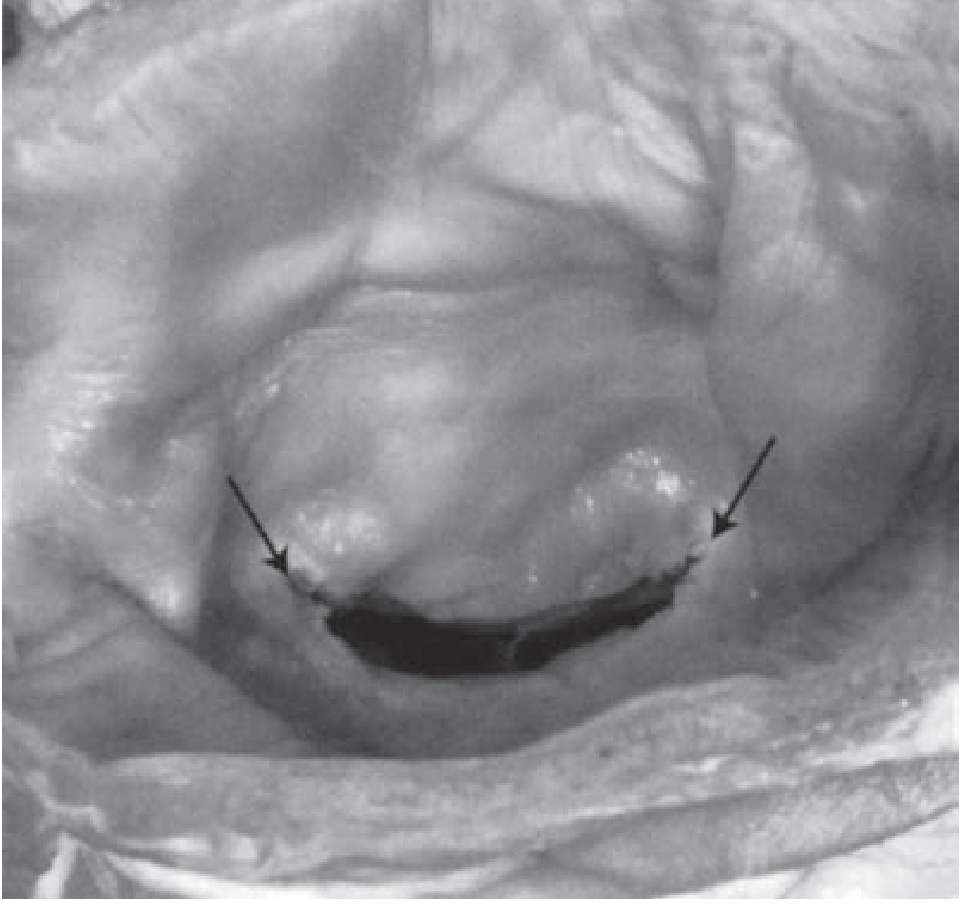
SEVERITY GRADING (AHA/ACC)
| Severity | MVA (cm²) | Mean Gradient (mmHg) | PASP (mmHg) |
|---|---|---|---|
| Mild | >1.5 | <5 | <30 |
| Moderate | 1.0–1.5 | 5–10 | 30–50 |
| Severe | <1.0 | >10 | >50 |
CLINICAL FEATURES
Symptoms
- Dyspnea on exertion → orthopnea → PND (earliest and most common)
- Hemoptysis — due to rupture of pulmonary-bronchial venous anastomoses
- Palpitations — AF is the most common arrhythmia
- Systemic embolism — stroke, TIA (especially with AF)
- Hoarseness — Ortner's syndrome: LA enlargement compressing recurrent laryngeal nerve
- Chest pain — uncommon; due to PAH or coexistent CAD
- Fatigue — low cardiac output state
- Recurrent bronchitis
Signs
- Malar flush ("mitral facies") — dilated capillaries in the cheeks due to low CO
- Tapping apex — palpable loud S1
- Parasternal heave — RV enlargement (sign of PAH)
- Diastolic thrill (rare)
Auscultation (Classic Triad)
- Loud S1 — due to abrupt tensing of stiffened mitral leaflets
- Opening Snap (OS) — follows A2 by 0.05–0.12 s; shorter A2–OS interval = more severe MS
- Low-pitched mid-diastolic rumbling murmur — best heard at apex with bell, patient in left lateral decubitus, accentuated by mild exercise; presystolic accentuation in sinus rhythm
Other sounds:
- Loud P2, closely split S2 (PAH)
- Graham Steell murmur — high-pitched, early diastolic decrescendo along left sternal border (pulmonary regurgitation due to PAH)
- Functional TR murmur (pansystolic, louder on inspiration — Carvallo's sign)
Note: In severe MS with very low CO, the murmur may become inaudible ("silent MS"). — Harrison's Principles of Internal Medicine, 22nd Ed.
INVESTIGATIONS
ECG
- P-mitrale (bifid P in lead II, width >0.12 s) — LA enlargement in sinus rhythm
- Tall, peaked P in lead V1 (negative terminal deflection)
- AF — most common arrhythmia in established MS
- RV hypertrophy pattern (right axis deviation, dominant R in V1) if PAH
Chest X-Ray
- LA enlargement — double shadow at right heart border, elevated left main bronchus, left atrial appendage prominence (straightening of left heart border)
- Pulmonary venous hypertension — upper lobe diversion, Kerley B lines, interstitial edema
- Mitral valve calcification
- RV enlargement (loss of retrosternal airspace on lateral)
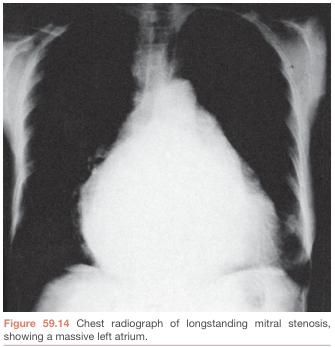
Echocardiography (Investigation of Choice)
- 2D echo: Doming ("hockey stick") of anterior mitral leaflet; restricted posterior leaflet; commissural fusion; calcification; Wilkins score
- Doppler: Mean transmitral gradient, PHT-derived MVA; assess PAH (TR jet velocity)
- Planimetry: Direct MVA measurement
- TEE: Exclude LA appendage thrombus before valvuloplasty or cardioversion
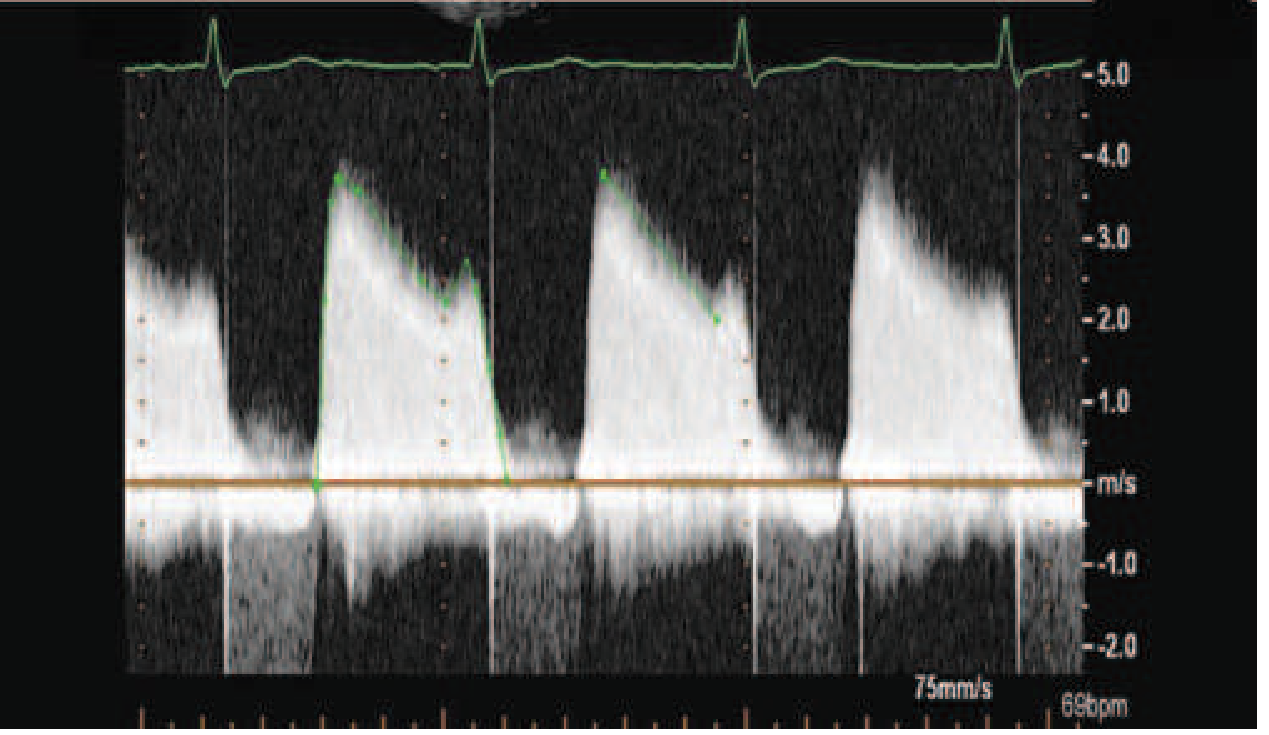
Wilkins Echocardiographic Score (each criterion scored 0–4, max 16):
- Leaflet mobility
- Leaflet thickening
- Subvalvular thickening
- Calcification
Score ≤8: favorable for Balloon Mitral Valvotomy (BMV)
Cardiac Catheterization
- Reserved when echo inconclusive or discordant with symptoms
- Pre-op coronary angiography in those with risk factors or age >40
NATURAL HISTORY
- Long asymptomatic latent period (20–40 years in developed nations; can be as short as 5 years in developing nations)
- Once symptoms develop, untreated prognosis is poor:
- NYHA II: 10-year survival 69%
- NYHA III: 10-year survival 33%
- NYHA IV: 10-year survival 0%
- MVA declines ~0.09 cm²/year on average
- Complications: AF (~30–40%), systemic embolism, pulmonary hypertension, RV failure
MANAGEMENT
A. Medical Management
1. Prevention (Primary & Secondary)
- Penicillin prophylaxis against Group A Strep (rheumatic fever secondary prevention) — lifelong in at-risk patients
- Infective endocarditis prophylaxis in high-risk patients
2. Symptom Relief
- Salt restriction + oral diuretics (loop diuretics: furosemide; thiazides) — reduce pulmonary congestion, relieve dyspnea
- Avoid strenuous exertion
3. Rate Control in AF (critical — tachycardia worsens hemodynamics)
- Beta-blockers (metoprolol, bisoprolol) — first line; also useful during pregnancy
- Non-DHP calcium channel blockers — verapamil, diltiazem
- Digoxin — useful in AF with heart failure, less effective for exercise-induced tachycardia
4. Rhythm Control
- Cardioversion (electrical or pharmacological) in recent-onset AF
- Requires ≥3 weeks of therapeutic anticoagulation (INR 2–3) OR TEE to exclude LA thrombus before cardioversion
- Less successful if LA markedly enlarged or AF >1 year
5. Anticoagulation
- Warfarin (Vitamin K antagonist), target INR 2–3 — indicated in:
- MS + AF (paroxysmal or permanent)
- Prior thromboembolism
- LA thrombus on echo
- ⚠️ NOACs (e.g., rivaroxaban) are NOT recommended in rheumatic MS with AF — a randomized trial showed significantly higher mortality compared to warfarin (Harrison's 22nd Ed.)
- Controversial in sinus rhythm with LA >5.5 cm
Medical therapy relieves symptoms but does NOT correct the underlying mechanical obstruction. Definitive treatment requires intervention. — Fuster & Hurst's The Heart, 15th Ed.
B. Interventional / Surgical Management
Indications for intervention (AHA/ACC):
- Symptomatic (NYHA II–IV) severe MS (MVA <1.5 cm²)
- Asymptomal severe MS with new-onset AF, PAH (PASP >50 mmHg), or desire for pregnancy
1. Percutaneous Mitral Balloon Commissurotomy (PMBC) / Balloon Mitral Valvotomy (BMV)
- Procedure of choice when anatomy is favorable
- Technique: Inoue balloon inflated across mitral valve via transseptal puncture
- Contraindications: MVA >1.5 cm², LA thrombus, MR >grade 2, severe calcification (Wilkins score >8), significant commissural calcification
- Results: MVA doubles, mean gradient halves
- Complications: MR (~3%), tamponade (~1%), embolism (~1%), mortality (<1%)
- Long-term: 80–90% event-free survival at 5–7 years with favorable anatomy
2. Surgical Mitral Commissurotomy (Closed / Open)
- Open commissurotomy: direct visualization on cardiopulmonary bypass
- Preferred when BMV contraindicated but valve not too diseased for repair
3. Mitral Valve Replacement (MVR)
- Indicated when leaflets too calcified/distorted for commissurotomy
- Options: mechanical valve (lifelong anticoagulation) vs. bioprosthetic valve
- Perioperative mortality: 1–3% (higher in older patients with PAH or LV dysfunction)
- Transcatheter mitral replacement (TMVR) under evaluation for degenerative MS/MAC
Management Flowchart (Harrison's 22nd Ed.):
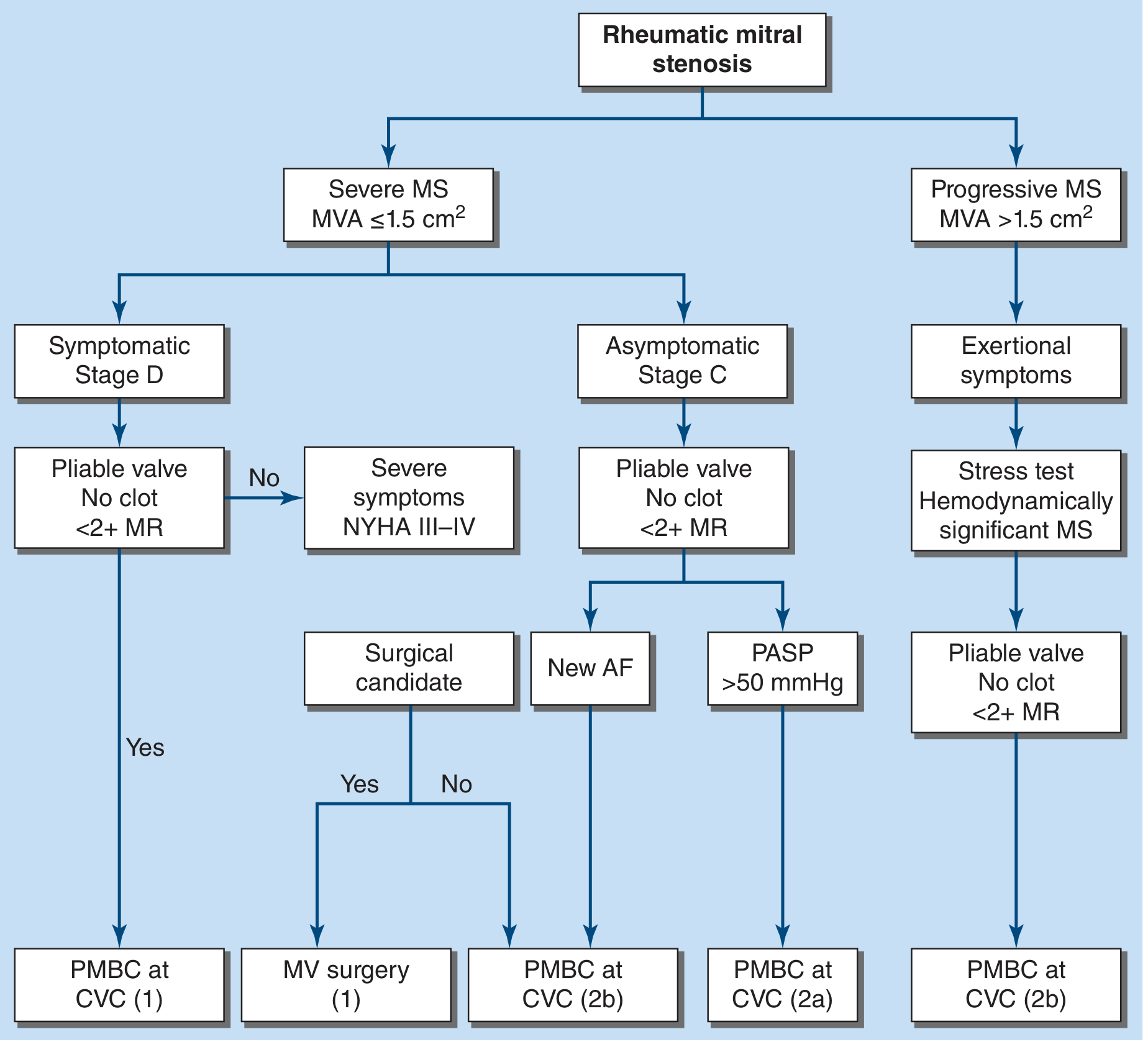 Rheumatic MS management flowchart per ACC/AHA 2021 guidelines — Harrison's 22nd Ed.
Rheumatic MS management flowchart per ACC/AHA 2021 guidelines — Harrison's 22nd Ed.

Special Situations
Pregnancy + MS
- Physiological increases in HR and blood volume → may precipitate acute decompensation
- Beta-blockers are the mainstay for symptom control
- BMV is preferred intervention if needed; preferably after 20 weeks, with fetal lead shielding
- MVR carries high fetal risk
COMPLICATIONS
| Complication | Mechanism |
|---|---|
| Atrial fibrillation | LA dilation → conduction remodeling |
| Systemic thromboembolism | LA stasis, especially in AF |
| Pulmonary arterial hypertension | Reactive pulmonary vasoconstriction |
| Right heart failure | Chronic PAH |
| Infective endocarditis | Turbulent flow, abnormal endothelium |
| Hemoptysis | Pulmonary venous hypertension |
| Ortner's syndrome | Hoarseness from LA compression of left RLN |
HOMEOPATHIC APPROACH TO MITRAL STENOSIS
Important clinical note: Homeopathy does not reverse structural valve stenosis or calcification. In the homeopathic framework, remedies are selected based on individualization — matching the totality of physical, mental, and general symptoms of the patient (not just the disease label). Homeopathic care is considered supportive/complementary; all patients with moderate-to-severe MS must receive conventional cardiological management.
Commonly Indicated Homeopathic Remedies
| Remedy | Key Indications in Cardiac/MS Context |
|---|---|
| Digitalis purpurea | Slow, very irregular, weak pulse; extreme exhaustion on slight motion; cardiac failure; cyanosis; patient fears heart will stop |
| Naja tripudians | Chronic valvular lesions; hypertrophied heart; oppression of chest; pulse irregular in force but regular in rhythm; sympathetic cough in rheumatic carditis; prostration; mental depression |
| Cactus grandiflorus | Constriction as of an iron band around chest; mitral insufficiency; cardiac incompetence; palpitations; precordial dullness; endocarditis |
| Spigelia anthelmia | Violent palpitation; trembling sensation in the chest; dyspnea; pain radiating to left arm; worse motion, left side; stitching pains in chest |
| Laurocerasus | Cyanosis; dyspnea with gasping; feeble, irregular pulse; cardiac failure; cold extremities; cold sweat |
| Kalmia latifolia | Cardiac symptoms after rheumatism; sharp pain in heart with extreme dyspnea and anguish; palpitation worse leaning forward; bradycardia (35–40 bpm) |
| Apis mellifica | Edema; anasarca; general fluid retention; oliguria; "feels each breath will be the last"; mitral insufficiency; organic heart disease |
| Aurum metallicum | Palpitation and cardiac hypertrophy; oppressive sensation; hypertension with heart disease; depression, tendency to despair |
| Adonis vernalis | Mitral and aortic regurgitation; rheumatic endocarditis; fatty heart; pericarditis; rapid irregular pulse; dyspnea; cardiac asthma |
| Arsenicum album | Prostration; anxiety and restlessness; dyspnea worse lying down; edema; palpitations with anxiety; worse at midnight |
| Spongia tosta | Dyspnea and wheezing (cardiac asthma); valvular disease; palpitation on ascending stairs |
| Lithium carbonicum | Rheumatic soreness in cardiac region; sudden shock in heart; throbbing and dull stitch in cardiac region; pains before urination |
| Rhus toxicodendron | Cardiac damage after rheumatic fever; palpitations; restlessness; valvular disease; worse cold and damp |
| Baryta carbonica | Elderly patients with hypertension and valve disease; palpitation; weakness |
| Crataegus oxyacantha | "Hawthorn" — cardiac tonic; strengthens heart muscle; used in cardiac failure, valvular disease; dyspnea on exertion |
Repertory References for Valvular Disease
From the Homoeopathic Repertory:
- Circulatory system – valvular disease: Acon., Adon. v., Apoc., Ars., Ars. iod., Aur. br., Aur. iod., Aur. m., Cact., Calc. fl., Camph., Conv., Crat., Dig., Ferr., Galanth., Glon., Iod., Kal., Lach., Laur., Lith. c., Lycop., Naja, Ox. ac., Phos., Plumb., Rhus. t., Sang., Serum ang., Spig., Spong., Stigm., Stroph., Thyr., Viscum.
Homeopathic Principles Applied to MS
- Individualization — Remedy selection is based on the complete symptom picture (mental, general, local), not on the diagnosis alone
- Miasmatic understanding — Rheumatic MS is viewed through the Psora-Sycosis-Syphilis miasmatic framework; Sycotic and Syphilitic miasms often implicated in structural degeneration
- Constitutional remedies — A deep-acting constitutional remedy (e.g., Aurum met., Calc. carb., Lycopodium) may be indicated for the underlying predisposition
- Organotropic remedies — Naja, Digitalis, Cactus, Crataegus are considered specific to the heart
- Intercurrent / Anti-miasmatic remedies — Medorrhinum, Syphilinum, Tuberculinum may be needed intercurrently
SUMMARY TABLE
| Domain | Key Points |
|---|---|
| Most common cause | Rheumatic fever (Group A Strep) |
| Hallmark murmur | Low-pitched mid-diastolic rumble at apex + loud S1 + OS |
| Best investigation | 2D/Doppler echocardiography |
| Medical Rx: rate | Beta-blockers, verapamil, diltiazem, digoxin |
| Medical Rx: HF | Diuretics + salt restriction |
| Anticoagulation | Warfarin (INR 2–3) for AF/embolism; NOACs avoided |
| Intervention of choice | BMV/PMBC (if Wilkins score ≤8, no LA clot, MR ≤2+) |
| Surgery | MVR for unsuitable anatomy |
| Homeopathic pillars | Naja, Digitalis, Cactus, Spigelia, Crataegus, Aurum met. |
Sources:
- Harrison's Principles of Internal Medicine, 22nd Ed. (2025) — Management, physical findings, treatment algorithm
- Fuster & Hurst's The Heart, 15th Ed. — Etiology, pathophysiology, natural history, BMV
- Braunwald's Heart Disease, 10th Ed. — Pathology, diagnosis, treatment
- Homeobook.com / Hpathy.com — Homoeopathic management (Dr. Naziya G.M. Naik; Dr. Manisha Sachdeva)
Find me the flashcard of aortic regurgitation.
Reading File
Searching the Web
aortic regurgitation flashcard medical mnemonics key points
Finding Sources
Reading Web Page
aortic regurgitation signs mnemonics flashcard
Finding Sources
Searching Images
aortic regurgitation peripheral signs echocardiography diagnosis
Reading File
Reading File
Finding Sources
I now have all the key content needed. Here is the complete Aortic Regurgitation flashcard:
🃏 AORTIC REGURGITATION — FLASHCARD
CARD 1 — DEFINITION & BASICS
| Definition | Incompetence of the aortic valve → backflow of blood from aorta into LV during diastole |
| Also called | Aortic insufficiency (AI) |
| Prevalence | ~4.9% overall; moderate-severe ~0.5% (Framingham data) |
| Key haemodynamic lesion | Volume overload of the LV (± afterload excess) |
CARD 2 — ETIOLOGY
Mnemonic: "CREAM" for valve leaflet causes + aortic root causes
Valve Leaflet Causes
| Cause | Notes |
|---|---|
| Bicuspid aortic valve | Most common congenital cause |
| Infective endocarditis | Most common cause of acute AR |
| Rheumatic heart disease | Often with mitral disease |
| Calcific degeneration | Degenerative, elderly |
| Dopamine/serotonin agonists | Drug-induced |
Aortic Root Causes
| Cause | Notes |
|---|---|
| Marfan syndrome | Annuloaortic ectasia |
| Hypertension | Aortic root dilation |
| Aortic dissection | Acute AR → emergency |
| Syphilis | Obliterative endarteritis of vasa vasorum |
| Ankylosing spondylitis / Psoriatic arthritis | Seronegative arthropathy |
| Idiopathic root dilation | Most common cause in developed nations |
Acute AR causes: Endocarditis + Aortic Dissection (remember: "E-D")
CARD 3 — PATHOPHYSIOLOGY
Chronic AR (Compensated → Decompensated)
Incompetent aortic valve
↓
LV receives normal LA inflow + regurgitant volume
↓
Volume overload → Eccentric LV hypertrophy (LV dilates)
↓
↑ Stroke volume → ↑ Systolic BP → Wide pulse pressure
↓
Afterload excess → Concentric + eccentric hypertrophy
↓ (years later)
LV systolic dysfunction → Heart failure symptoms
Acute AR (Decompensated from the start)
- No time for LV compensation → sudden ↑ LVEDP
- ↓ Cardiac output + ↑ pulmonary pressure → Pulmonary oedema + shock
- Reflex vasoconstriction raises SVR (makes it worse)
- Medical emergency — early surgery needed
CARD 4 — SYMPTOMS
| Chronic AR | Acute AR |
|---|---|
| Long asymptomatic period | Sudden severe dyspnoea |
| Dyspnoea on exertion (first symptom) | Cardiogenic shock |
| Orthopnoea, PND | Pulmonary oedema |
| Fatigue | Tachycardia, hypotension |
| Angina (less common than AS) | Rapidly fatal if untreated |
| Palpitations (awareness of heartbeat) | |
| Carotid artery pain | |
| Neck pulsations |
CARD 5 — PERIPHERAL SIGNS (The Famous Eponyms)
Mnemonic: "WCDQ-MT" — Water hammer, Corrigan, De Musset, Quincke, Müller, Traube
| Sign | Description | How to Elicit |
|---|---|---|
| Corrigan's pulse (Water hammer pulse) | Rapid rise + sharp collapse of carotid/radial pulse | Feel the radial pulse with wrist elevated |
| De Musset's sign | Head nodding/bobbing with each heartbeat | Observe head at rest |
| Quincke's sign | Capillary pulsations at proximal nail bed | Press lightly on fingernail tip — alternating flush/blanch |
| Duroziez's sign | Systolic + diastolic bruit ("to-and-fro") over femoral artery | Press stethoscope on femoral artery |
| Traube's sign | Pistol-shot sound over the femoral artery | Auscultation over femoral |
| Müller's sign | Pulsation of the uvula | Inspect open mouth |
| Hill's sign | Popliteal BP > brachial BP by >20 mmHg (>60 mmHg = severe) | BP in arm and leg |
| Landolfi's sign | Alternating constriction and dilation of the pupil | Inspect pupils |
| Becker's sign | Visible pulsations of retinal arterioles | Fundoscopy |
| Lighthouse sign | Flushing and blanching of the forehead | Observe forehead |
| Mayne's sign | >15 mmHg drop in diastolic BP on raising arm | BP measurement |
| Rosenbach's sign | Pulsating liver | Palpate liver |
All these signs reflect the wide pulse pressure and hyperdynamic circulation from the high stroke volume.
CARD 6 — CARDIAC EXAMINATION
| Feature | Finding |
|---|---|
| Apex beat | Displaced downward & laterally; hyperdynamic, volume-overloaded character |
| S1 | Normal or soft |
| S2 | Soft A2 (leaflet not closing properly) |
| Murmur | High-pitched, blowing, early diastolic decrescendo murmur at left lower sternal border (LLSB) / 3rd ICS |
| Best heard | Patient sitting forward, breath held in expiration |
| Austin Flint murmur | Low-pitched mid-diastolic rumble at apex (regurgitant jet impinges on mitral valve causing it to vibrate — mimics mitral stenosis but no OS) |
| Systolic murmur | May be present (high flow ejection murmur across aortic valve — does NOT mean AS) |
In acute AR: murmur is short and soft (LV pressure rises rapidly, equalizes with aorta early in diastole) — easily missed!
CARD 7 — INVESTIGATIONS
ECG
- LV hypertrophy pattern (tall R in V5–V6, deep S in V1–V2)
- Left axis deviation
- ST-T changes (strain pattern)
- Normal in early/mild AR
Chest X-Ray
- Cardiomegaly — enlarged LV ("boot-shaped" or globular heart)
- Aortic root dilation (prominent aortic knuckle)
- In acute AR: pulmonary oedema with near-normal heart size
Echocardiography (Gold Standard)
- 2D: LV dilation, LV function, aortic root size, leaflet morphology, vegetations
- Colour Doppler: regurgitant jet width/area in LVOT
- Vena contracta ≥6 mm → severe AR
- Holodiastolic flow reversal in descending/abdominal aorta → severe AR
- Pressure half-time (PHT) <200 ms → severe AR (rapid equalization)
- LV dimensions: LVESD >50 mm or LVEDD >65 mm → surgical threshold
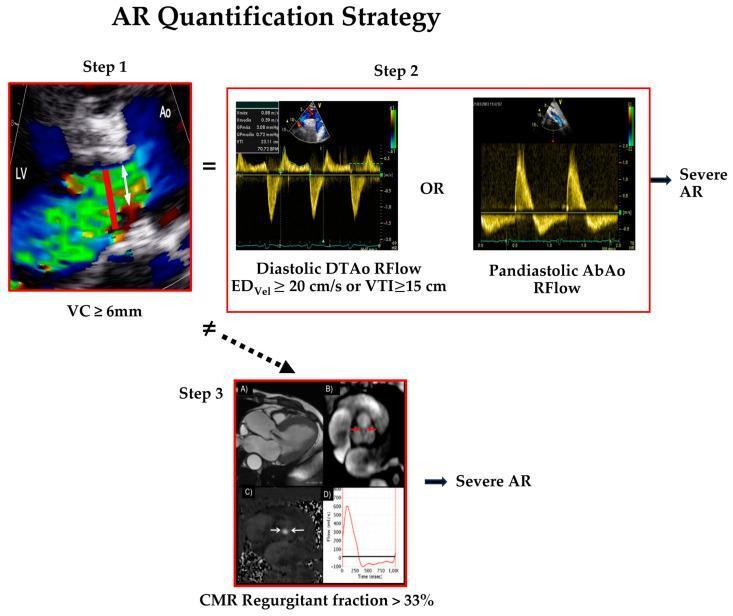
Cardiac Catheterization
- Aortography when echo is inconclusive
- Coronary angiography pre-op (age >40 or risk factors)
CARD 8 — SEVERITY GRADING
| Parameter | Mild | Moderate | Severe |
|---|---|---|---|
| Vena contracta (cm) | <0.3 | 0.3–0.6 | >0.6 |
| Regurgitant fraction | <30% | 30–50% | >50% |
| Regurgitant volume (mL/beat) | <30 | 30–60 | >60 |
| PHT (ms) | >500 | 200–500 | <200 |
| Holodiastolic reversal | Absent/brief | Present | Pandiastolic |
CARD 9 — MANAGEMENT
Acute AR — Emergency
- IV vasodilators (sodium nitroprusside) + inotropes (dobutamine)
- No IABP (contraindicated — worsens regurgitation in diastole)
- Urgent/Emergency aortic valve replacement (AVR) — medical management alone = high mortality
- Treat underlying cause (antibiotics for endocarditis, surgery for dissection)
Chronic AR — Medical
| Drug | Indication |
|---|---|
| Vasodilators (ACE inhibitors, nifedipine, hydralazine) | Symptomatic AR not yet ready for surgery; asymptomatic with LV dilation/hypertension |
| Beta-blockers | Avoid in pure AR (slow HR → longer diastole → more regurgitation time); used in Marfan syndrome for aortic root protection |
| Diuretics / Digoxin | Symptomatic heart failure relief |
| Penicillin prophylaxis | Secondary prevention of rheumatic fever |
| Endocarditis prophylaxis | High-risk patients per guidelines |
Note: Vasodilators reduce afterload, decrease regurgitant volume and are the cornerstone of medical management. — Goldman-Cecil Medicine
Chronic AR — Surgical: Indications for AVR (AHA/ACC)
| Indication | Class |
|---|---|
| Symptomatic severe AR (NYHA II–IV) | I |
| Asymptomatic severe AR + LVEF <55% | I |
| Asymptomatic severe AR + LVESD >50 mm or LVEDD >65 mm | IIa |
| Severe AR undergoing other cardiac surgery | I |
| Severe AR + aortic root ≥5.5 cm (Marfan: ≥5.0 cm) | I |
Valve replacement should occur before irreversible ventricular dysfunction — serial echo surveillance is key. — Fuster & Hurst's The Heart, 15th Ed.
CARD 10 — ACUTE vs. CHRONIC: QUICK COMPARISON
| Feature | Chronic AR | Acute AR |
|---|---|---|
| Onset | Gradual | Sudden |
| LV size | Enlarged | Normal |
| Pulse pressure | Wide | Normal/slightly wide |
| Murmur | Long, prominent | Short, soft (easily missed) |
| Apex | Displaced, hyperdynamic | Normal position |
| Compensation | Eccentric hypertrophy | None |
| Presentation | Exertional dyspnoea | Shock + pulmonary oedema |
| Urgency | Elective | Emergency |
CARD 11 — KEY MNEMONICS
Causes mnemonic: "CREAM + MHSAI"
- Congenital (bicuspid), Rheumatic, Endocarditis, Ankylosing spondylitis, Marfan's
- Marfan, Hypertension, Syphilis, Aortic dissection, Idiopathic
Peripheral signs mnemonic: "WCDQ + TMB"
- Water hammer, Corrigan, De Musset, Quincke, Traube, Müller, Becker
Austin Flint vs. MS:
Austin Flint = no Opening Snap, no LA enlargement, no P-mitrale on ECG
Murmur location memory:
AR = After S2 → At Left Lower Sternal Border = "A-LLSB"
Sources: Goldman-Cecil Medicine; Rosen's Emergency Medicine; Fuster & Hurst's The Heart, 15th Ed.; Morgan & Mikhail's Clinical Anaesthesiology, 7th Ed.; Braunwald's Heart Disease
This is a shared conversation. Sign in to Orris to start your own chat.