Macular hole
Reading File
Finding Sources
Searching PubMed
"macular hole"[MeSH Terms] AND treatment
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
A macular hole is a full-thickness defect at the fovea (center of the macula) that causes central vision loss and distortion.
Key points
- Most often affects women age 60 to 70
- Usually idiopathic and related to vitreomacular traction (VMT) during posterior vitreous detachment
- Can also occur with high myopia or blunt trauma
- Bilateral involvement risk is clinically relevant (about 10% to 30% reported depending on cohort/setting)
Typical symptoms
- Blurred central vision in one eye
- Metamorphopsia (straight lines look wavy)
- Central scotoma
- Early/impending stages may be minimally symptomatic
Diagnosis
- OCT is the key test for confirmation and staging
- Fundus exam may show a round red foveal lesion with a cuff/halo
- Watzke-Allen slit-beam test may show a perceived break in the beam over a true full-thickness hole
- Differentiate from:
- Lamellar macular hole
- Macular pseudohole from epiretinal membrane
- Chronic CME-related cystic changes
- Solar retinopathy
Staging
Classic Gass staging:
- Stage 1: impending hole
- Stage 2: small full-thickness hole
- Stage 3: full-thickness hole, no complete PVD
- Stage 4: full-thickness hole with complete PVD
Modern OCT-based classification also uses:
- Hole size (small, medium, large)
- Presence/absence of VMT
- Etiology (primary vs secondary)
Management
- Stage 1: often observation (many resolve spontaneously)
- Symptomatic full-thickness holes (especially stage 2+): pars plana vitrectomy with ILM peel and gas tamponade is standard of care
- Better outcomes when treated earlier, especially within about 6 months
- Post-op face-down positioning may be used (shorter protocols common with modern techniques)
- Ocriplasmin may be considered in selected early small VMT-related cases, but use is limited by variable efficacy and side effects
- Cataract progression after vitrectomy in phakic patients is very common
Prognosis
- Anatomical closure rates are high after surgery
- Vision often improves over months
- Smaller holes and shorter duration generally have better visual outcomes
- Some full-thickness holes can close spontaneously
Example images
Fundus stages of macular hole:
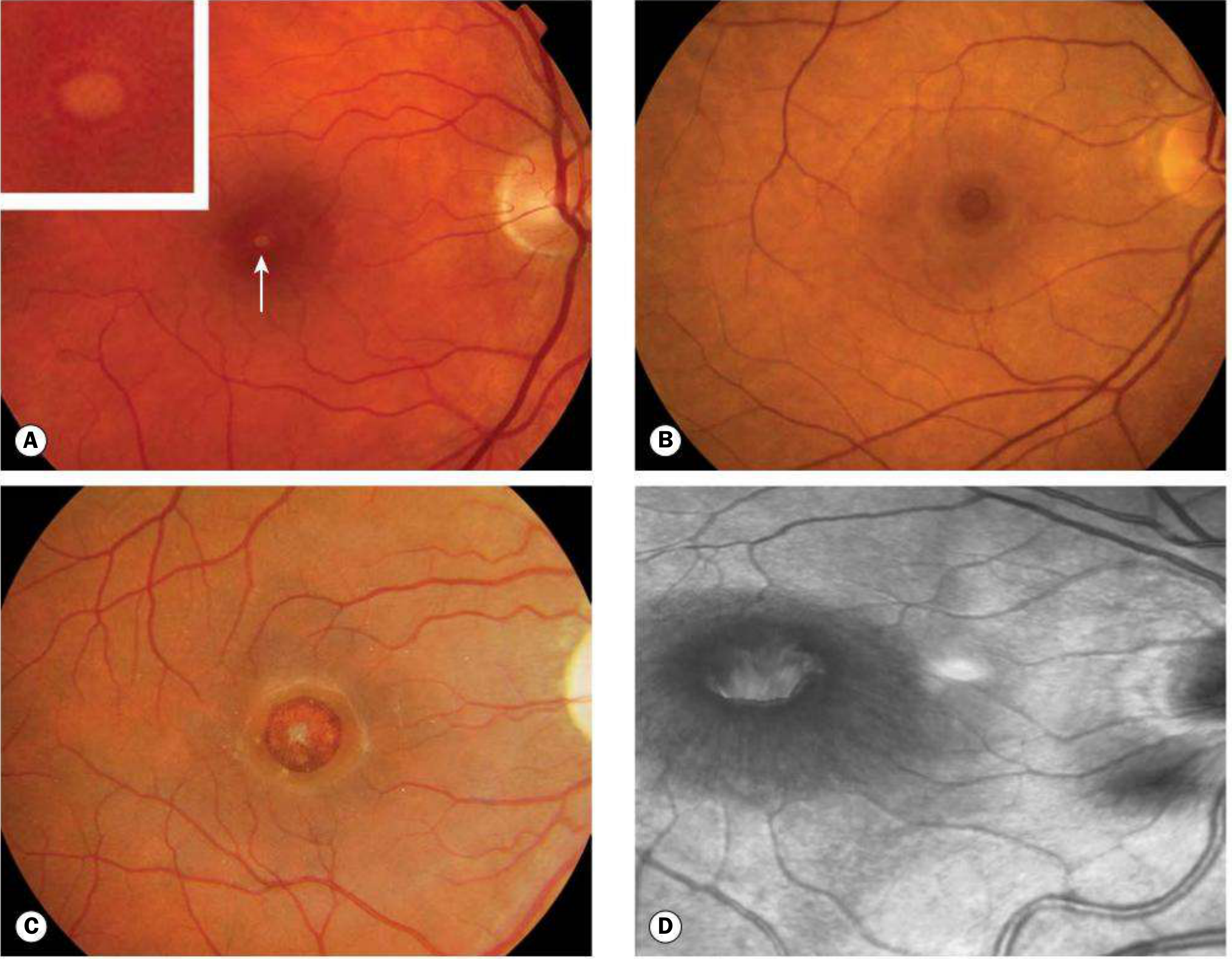

OCT appearance of macular hole:
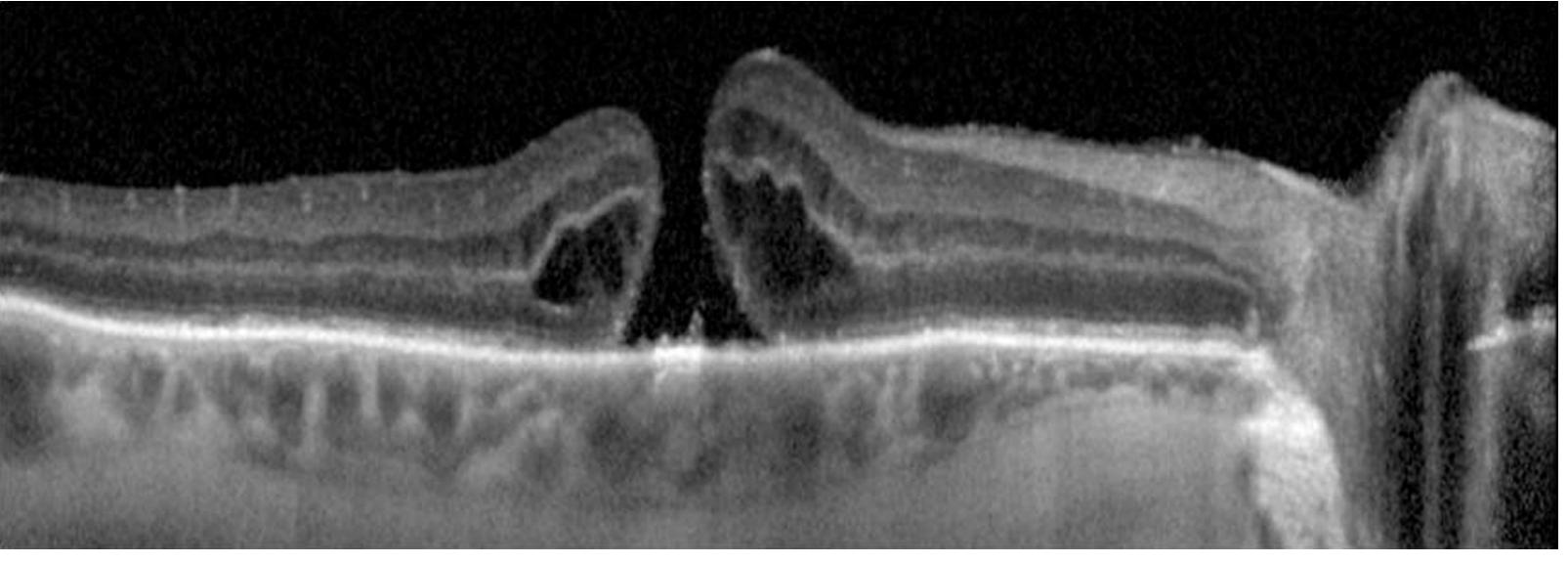

Recent evidence check:
- A quick PubMed search limited to the last 2 years for systematic reviews/meta-analyses on “macular hole treatment” returned no hits, so no immediate high-level contradiction signal was identified from that narrow filter.
Sources:
- Kanski's Clinical Ophthalmology: A Systematic Approach, 10th ed, p. 626-629
- The Wills Eye Manual, p. 866-870
If you want, I can give you a one-page patient-friendly version or a retina-specialist-level surgical decision flowchart.
Need for 15 marks
Macular Hole (15-mark answer)
Definition
A macular hole is a full-thickness defect in the neurosensory retina at the fovea, causing central visual impairment.
Epidemiology
- Common in older adults, especially 60 to 70 years
- Female preponderance
- Usually unilateral at presentation, but fellow-eye risk exists (about 10% or more over time)
Etiology and Pathogenesis
- Idiopathic (most common)
Related to age-related vitreous changes and anomalous posterior vitreous detachment. - Vitreomacular traction (VMT)
Persistent vitreofoveal adhesion causes anteroposterior and tangential traction, leading to foveal dehiscence. - Secondary causes
- High myopia
- Blunt ocular trauma
- Less commonly cystoid macular edema-associated tractional changes
Classification
A. Gass Clinical Staging
- Stage 1: Impending hole (yellow spot/ring at fovea)
- Stage 2: Small full-thickness macular hole
- Stage 3: Full-thickness hole with cuff of subretinal fluid, without complete PVD
- Stage 4: Full-thickness hole with complete PVD
B. OCT-Based Classification (current practical approach)
- Based on:
- Hole size (small, medium, large)
- Presence/absence of vitreomacular traction
- Etiology (primary/secondary)
Clinical Features
Symptoms
- Painless diminution of central vision
- Metamorphopsia
- Central scotoma
- Reading difficulty
- Early stages may be minimally symptomatic
Signs
- Round red foveal lesion
- Gray cuff/halo (subretinal fluid) around full-thickness hole
- Possible operculum
- Loss of normal foveal contour in VMT stages
Investigations
- Optical Coherence Tomography (OCT)
Gold standard for diagnosis, staging, and follow-up. - Amsler grid
Detects central distortion. - Watzke-Allen test
Thinning/break in slit beam perception suggests true full-thickness hole. - Fundus biomicroscopy
For morphology and associated vitreoretinal interface abnormalities. - FA/FAF (selected cases)
Usually not required when OCT is diagnostic.
Differential Diagnosis
- Lamellar macular hole
- Macular pseudohole (epiretinal membrane)
- Chronic CME with central cystic change
- Solar retinopathy
- Other foveal lesions mimicking a hole
Management
1. Observation
- Stage 1 holes are often observed because spontaneous resolution can occur.
- Small spontaneous closure can also occur in some full-thickness holes.
2. Pharmacologic vitreolysis
- Ocriplasmin in selected VMT/small early holes
- Limited use due to variable efficacy and adverse effects
3. Surgical treatment (standard for symptomatic full-thickness holes)
- Pars plana vitrectomy + ILM peeling + gas tamponade
- Relieve traction, promote hole closure
- Better outcomes when operated early (preferably within ~6 months of onset)
- Postoperative prone positioning may be advised for selected duration
Prognosis
- High anatomical closure rates after surgery
- Visual recovery occurs over months
- Better visual outcomes with:
- Smaller hole size
- Shorter symptom duration
- Earlier surgery
- Cataract progression in phakic eyes after vitrectomy is common
Complications
- Persistent/recurrent hole
- Cataract progression
- Retinal detachment (uncommon but important)
- Other vitrectomy-related complications
Follow-up
- Monitor with serial OCT
- Counsel regarding symptoms of retinal detachment
- Periodic fellow-eye assessment due to bilateral risk
Short conclusion
Macular hole is an important treatable cause of central visual loss in older adults. OCT is central to diagnosis and staging, and modern vitrectomy with ILM peel and gas tamponade provides high closure rates and useful visual recovery, especially when intervention is early.
CMV RETINITIS for 15 marks
CMV Retinitis (15-mark answer)
Definition
CMV retinitis is a necrotizing viral retinitis caused by cytomegalovirus, seen mainly in severely immunocompromised patients, classically advanced HIV/AIDS, but also transplant recipients and patients on strong immunosuppression.
Etiology and Risk Factors
- Causative agent: Human cytomegalovirus (HHV-5)
- Major risk groups:
- HIV with very low CD4 count (especially <50 cells/µL)
- Solid organ/hematopoietic stem cell transplant
- Prolonged corticosteroids, chemotherapy, biologics, immunosuppressants
- Hematologic malignancy, congenital immunodeficiency
Pathogenesis
- CMV reactivation occurs in profound immunosuppression
- Hematogenous spread to retina causes full-thickness retinal necrosis
- Associated occlusive vasculitis and hemorrhage
- Lesions spread centrifugally along vessels if untreated
- Healed lesions become atrophic scars, predisposing to retinal breaks and detachment
Clinical Features
Symptoms
- Floaters
- Blurred vision
- Scotoma
- Photopsia
- Painless progressive visual loss
(Early peripheral disease may be asymptomatic)
Signs (Fundus)
- Yellow-white granular retinal necrosis with retinal hemorrhages
classic “pizza pie” or “cottage cheese with ketchup” appearance - Perivascular whitening/sheathing
- Minimal anterior chamber/vitreous inflammation compared with lesion extent
- May be unilateral initially, with risk of fellow-eye involvement if untreated
Clinical Patterns
- Fulminant/edematous form
Dense hemorrhagic necrotizing lesions, often posterior pole - Indolent/granular form
Peripheral granular lesions with slower progression - Frosted branch angiitis-like vasculitis (less common)
Diagnosis
Primarily clinical in a high-risk patient:
- Dilated fundus examination (cornerstone)
- Wide-field fundus photography for documentation
- OCT for macular involvement/complications
- Aqueous/vitreous PCR (CMV DNA) when diagnosis is uncertain or atypical
- HIV testing/CD4 count and systemic immunologic workup where relevant
Differential Diagnosis
- Acute retinal necrosis (HSV/VZV)
- Progressive outer retinal necrosis
- Toxoplasma retinochoroiditis
- Syphilitic retinitis
- Candida endophthalmitis
- Intraocular lymphoma
Treatment
1) Anti-CMV induction therapy
- Valganciclovir (oral) commonly used if sight-threatening disease is absent
- IV ganciclovir for severe/bilateral/systemic disease
- Foscarnet (alternative or resistant/intolerant cases)
- Cidofovir less favored due to toxicity profile
2) Local therapy for sight-threatening lesions
(near macula/optic disc or rapidly progressive disease)
- Intravitreal ganciclovir or foscarnet, often combined with systemic therapy for rapid local control
3) Maintenance and immune restoration
- Continue maintenance therapy until immune recovery (in HIV, sustained CD4 improvement on ART)
- Start/optimize ART in HIV patients (timing individualized)
- Coordinate with physician/infectious disease specialist
Monitoring and Follow-up
- Frequent retinal exams during induction (often weekly initially)
- Watch for progression at lesion borders, new lesions, fellow-eye disease
- Hematologic and renal monitoring for drug toxicity
- Long-term follow-up for structural sequelae
Complications
- Rhegmatogenous retinal detachment (major cause of severe visual loss)
- Optic atrophy
- Macular scarring/edema
- Immune recovery uveitis after ART initiation
- Drug adverse effects:
- Ganciclovir/valganciclovir: neutropenia, thrombocytopenia
- Foscarnet: nephrotoxicity, electrolyte disturbances
- Cidofovir: nephrotoxicity, uveitis/hypotony
Prognosis
- Visual outcome depends on:
- Lesion location (macula/optic nerve involvement worse)
- Speed of diagnosis and treatment
- Degree of immune reconstitution
- Prognosis has improved markedly in the ART era, but relapse and late complications remain significant.
Prevention
- Early HIV diagnosis and effective ART
- In transplant and high-risk patients: virologic monitoring and pre-emptive CMV strategies
- Patient education to report new floaters, field defects, or blurred vision immediately
Short conclusion
CMV retinitis is an ophthalmic emergency in immunocompromised patients. Prompt recognition of characteristic necrotizing hemorrhagic retinitis, early anti-CMV induction (systemic ± intravitreal), and restoration of immune function are the keys to preventing irreversible blindness and reducing recurrence.
This is a shared conversation. Sign in to Orris to start your own chat.