I need to make a presentation on anatomy of pelvic organs based on Telinde surgical gynaecology
Reading File
search_medical_text
pelvic organ anatomy surgical gynecology TeLinde
search_medical_text
pelvic floor muscles ligaments supports uterus bladder rectum anatomy
search_medical_image
pelvic organ anatomy female pelvis uterus bladder rectum
GradeResponse
GradeResponse
GradeResponse
search_medical_text
uterus anatomy structure cervix uterine body ligaments blood supply
search_medical_text
pelvic retroperitoneal spaces paravesical pararectal ureter anatomy gynecology
search_medical_image
pelvic floor levator ani muscles anatomy diagram
GradeResponse
Here is a comprehensive, presentation-ready outline on Anatomy of Pelvic Organs based on TeLinde's Operative Gynecology (with supplementary detail from standard references). You can use this as a slide-by-slide framework.
🎯 Anatomy of Pelvic Organs
Based on TeLinde's Operative Gynecology
Slide 1 — Introduction & Clinical Relevance
- Precise knowledge of pelvic anatomy is the cornerstone of safe gynecologic surgery
- The pelvis contains organs of the urinary, reproductive, and gastrointestinal systems — all in close proximity
- Surgical errors (ureteric injury, bladder entry, rectal injury) arise directly from failure to appreciate these relationships
- TeLinde's approach: anatomy as it is encountered during surgery, not just descriptively
Slide 2 — Bony Pelvis
| Structure | Surgical Relevance |
|---|---|
| Sacrum & coccyx | Posterior boundary; sacrospinous fixation point |
| Ilium, ischium, pubis | Pelvic sidewall landmarks |
| Pubic symphysis | Anterior boundary; space of Retzius lies behind it |
| Pelvic inlet/outlet | Determines axis of surgical access |
| Ischial spine | Key landmark for pudendal nerve block, sacrospinous ligament |
- True pelvis (below pelvic inlet) — contains the pelvic organs
- False pelvis (above inlet) — contains bowel loops
Slide 3 — Pelvic Floor
Muscles of the Pelvic Floor (Levator Ani Group)
| Muscle | Origin | Insertion | Function |
|---|---|---|---|
| Pubococcygeus | Pubic body | Anococcygeal raphe | Urethral & vaginal support |
| Puborectalis | Pubic body | Forms U-sling around rectum | Fecal continence |
| Iliococcygeus | Arcus tendineus | Anococcygeal raphe | Pelvic diaphragm |
| Coccygeus (ischiococcygeus) | Ischial spine | Coccyx/sacrum | Closes posterior pelvis |
- Covered by endopelvic fascia
- Lateral thickening = Arcus Tendineus Fascia Pelvis (ATFP) — lies medial to obturator internus; critical landmark for anti-prolapse sutures (Bailey & Love, p. 1507)
- The pelvic floor muscles support all three compartments: bladder/urethra (anterior), uterus/vagina (middle), rectum (posterior)
Slide 4 — Pelvic Peritoneum & Pouches
- Peritoneum drapes over pelvic organs, forming important surgical landmarks
| Structure | Location | Significance |
|---|---|---|
| Vesicouterine pouch | Between bladder & uterus anteriorly | Dissection plane for hysterectomy |
| Rectouterine pouch (Pouch of Douglas) | Between uterus & rectum posteriorly | Deepest peritoneal recess; endometriosis site |
| Broad ligament | Bilateral peritoneal fold over uterus/tube | Contains uterine vessels, ureter, round & ovarian ligaments |
| Round ligament | From uterine cornua through inguinal canal | Marks anterior leaf of broad ligament |
| Infundibulopelvic (IP) ligament | Suspends ovary, contains ovarian vessels | Must be ligated in salpingo-oophorectomy |
Slide 5 — Uterus
Anatomy
- Position: Anteverted, anteflexed (normal); retroversion in ~20% of women
- Size: ~7.5 × 5 × 2.5 cm (nulliparous); larger after pregnancies
- Parts: Fundus → Body → Isthmus → Cervix (supravaginal + vaginal portions)
Layers
| Layer | Description |
|---|---|
| Perimetrium | Outer peritoneum |
| Myometrium | Thick smooth muscle; contracts during labor |
| Endometrium | Inner mucosa; functional + basal layers |
Blood Supply
- Uterine artery (from internal iliac) — crosses ureter 1.5–2 cm lateral to cervix ("water under the bridge")
- Anastomoses with ovarian artery superiorly
- Venous drainage: Uterine venous plexus → internal iliac veins
Ligamentous Supports
| Ligament | Attachment | Role |
|---|---|---|
| Cardinal (Mackenrodt's) | Cervix → pelvic sidewall | Primary lateral support against prolapse |
| Uterosacral | Cervix/upper vagina → sacrum | Posterior support; contains sympathetic nerves |
| Round | Cornua → labia majora | Maintains anteversion (limited structural role) |
| Broad | Lateral uterus → pelvic sidewall | Contains vessels and ureter |
Slide 6 — Fallopian Tubes & Ovaries
Fallopian Tube
- Parts: Interstitial → Isthmus → Ampulla → Infundibulum (with fimbriae)
- Ampulla = most common site of ectopic pregnancy and fertilization
- Blood supply: branches of uterine and ovarian arteries in the mesosalpinx
Ovary
- Attachments: Suspensory (IP) ligament superiorly, ovarian (utero-ovarian) ligament medially, mesovarium
- Blood supply: Ovarian artery (directly from aorta at L2)
- Venous drainage: Right ovarian vein → IVC; Left → left renal vein
- Surgical note: IP ligament must be clamped high to avoid ureteric injury during oophorectomy
Slide 7 — Urinary Bladder & Urethra
Bladder
- Lies posterior to pubic symphysis, anterior to uterus and vagina
- Detrusor muscle: three layers of smooth muscle
- Trigone: between two ureteric orifices and internal urethral meatus — landmark for cystoscopy
- Pubovesical/pubourethral ligaments: anterior supports of bladder neck
Urethra
- Female urethra: 3.5–5 cm long
- Passes through urogenital diaphragm, opens at external urethral meatus anterior to vaginal introitus
- Supported by pubourethral ligaments and pelvic floor (pubococcygeus)
Surgical Vulnerability
- Bladder injury most common during entry into vesicouterine space in hysterectomy
- Urethral injury rare but occurs in anterior colporrhaphy
Slide 8 — Ureter
"The ureter is the most important structure in gynecologic surgery" — TeLinde's
Course
- Abdominal ureter: Descends over psoas, crosses pelvic brim at bifurcation of common iliac
- Pelvic ureter: Enters pelvis crossing external/internal iliac vessels → runs in medial leaf of broad ligament
- Critical point: Passes 1.5–2 cm lateral to the cervix, under the uterine artery
- Passes near vaginal fornix, then enters trigone of bladder
Danger Zones in Surgery
| Procedure | Danger Zone |
|---|---|
| Hysterectomy | Uterine artery ligation, paracervical clamp |
| Salpingo-oophorectomy | IP ligament clamping |
| Pelvic lymph node dissection | Along iliac vessels |
| Sacrocolpopexy | Sacral promontory dissection |
Slide 9 — Rectum & Sigmoid Colon
- Rectum: ~12–15 cm; begins at S3, ends at anorectal junction
- Lies posterior to uterus/vagina, anterior to sacrum
- Rectovaginal septum (Denonvilliers' fascia): thin fascial plane between posterior vaginal wall and rectum
- Posterior to the rectum: pararectal space → important for rectal mobilization in radical hysterectomy
Surgical Relevance
- Entry into rectovaginal space is essential for posterior colporrhaphy and sacrocolpopexy
- Rectal injury most common at rectouterine pouch in cases of endometriosis/adhesions
Slide 10 — Retroperitoneal Spaces
These spaces are key to safe radical gynecologic surgery (Bailey & Love, p. 1598):
| Space | Boundaries | Clinical Use |
|---|---|---|
| Space of Retzius (retropubic) | Pubic symphysis anteriorly, bladder posteriorly | Retropubic continence procedures (Burch) |
| Paravesical space | Medial: bladder; Lateral: obturator fascia | Exposes lateral bladder, cardinal ligament |
| Pararectal space | Medial: rectum; Lateral: internal iliac artery | Ureter identification, rectal mobilization |
| — Medial pararectal (Okabayashi space) | Ureter medially | Radical hysterectomy |
| — Lateral pararectal (Latzko space) | Ureter laterally | Rectal dissection |
| Rectovaginal space | Anterior: vagina; Posterior: rectum | Posterior dissection, endometriosis surgery |
| Retrorectal (presacral) space | Anterior: rectum; Posterior: sacrum | Presacral neurectomy, sacrocolpopexy |
- Pararectal space: floor = levator ani, roof = posterior leaf of broad ligament, cranial border = uterine artery (Bailey & Love, p. 1598)
Slide 11 — Vascular Anatomy
Internal Iliac Artery (Hypogastric)
- Anterior division supplies pelvic organs:
- Uterine artery
- Vaginal artery
- Internal pudendal artery
- Obturator artery
- Inferior vesical artery
- Posterior division: iliolumbar, lateral sacral, superior gluteal (exits pelvis)
Key Points
- Internal iliac artery ligation (bilateral): used to control catastrophic pelvic hemorrhage
- Ovarian arteries arise directly from aorta (L1–L2 level)
Slide 12 — Pelvic Lymphatics
| Nodal Group | Drains |
|---|---|
| External iliac nodes | Bladder, upper vagina, cervix, vulva (via inguinal) |
| Internal iliac (hypogastric) nodes | Uterus, cervix, upper vagina, bladder base |
| Obturator nodes | Cervix, bladder, vulva — first echelon in cervical cancer |
| Common iliac nodes | Receive drainage from above |
| Para-aortic nodes | Ovaries, uterine fundus, tubes |
| Inguinal nodes | Vulva, lower vagina, perianal skin |
Slide 13 — Pelvic Nerve Supply
| Nerve | Origin | Supplies |
|---|---|---|
| Lumbosacral trunk | L4–L5 | Lower limb motor |
| Obturator nerve | L2–L4 (lumbar plexus) | Medial thigh; at risk in lymphadenectomy |
| Femoral nerve | L2–L4 | Anterior thigh; lithotomy position palsy |
| Genitofemoral nerve | L1–L2 | Inguinal/labial sensation |
| Superior hypogastric plexus | T10–L2 (sympathetic) | Uterus, bladder, rectum |
| Inferior hypogastric plexus | S2–S4 (parasympathetic) | Bladder detrusor, rectum, sexual function |
| Pudendal nerve | S2–S4 | External sphincters, vulva, clitoris |
- Uterosacral ligaments carry autonomic nerves → nerve-sparing radical hysterectomy preserves bladder function
Slide 14 — Key Images
Sagittal View of Female Pelvis
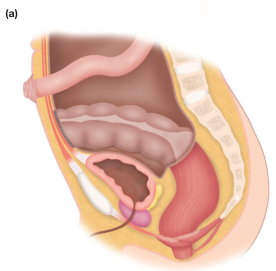
Sagittal section showing spatial relationships: sigmoid colon (superior/posterior) → rectum (posterior to uterus and vagina) → uterus (central) → bladder (anterior) → vagina (between bladder and rectum). The proximity of these structures explains common intraoperative injuries. (Bailey & Love, p. 1344)
Pelvic Floor — Levator Ani
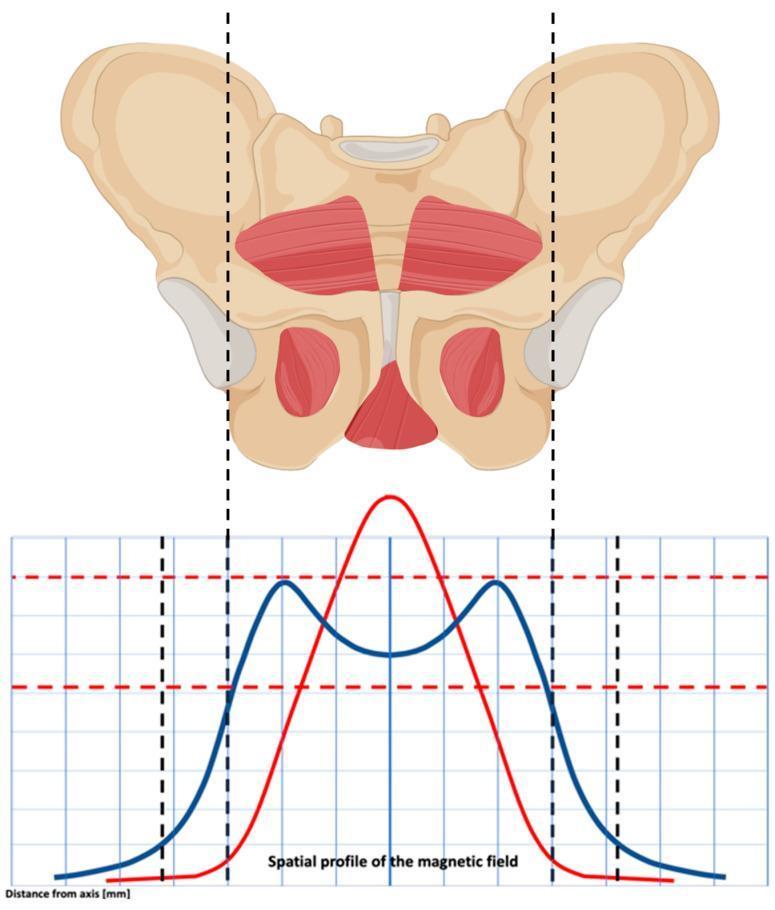
Anterior view of the pelvic girdle showing levator ani and pelvic floor muscles highlighted. These muscles form the pelvic diaphragm and support all three compartments.
Slide 15 — Summary: Surgical Danger Zones
| Structure at Risk | Operation | Prevention |
|---|---|---|
| Ureter | Hysterectomy, oophorectomy | Open retroperitoneum, identify ureter throughout |
| Bladder | Hysterectomy, anterior repair | Develop vesicouterine space sharply |
| Rectum | Posterior repair, endometriosis surgery | Identify rectovaginal space early |
| Obturator nerve | Pelvic lymphadenectomy | Identify nerve before node dissection |
| Iliac vessels | Para-aortic dissection | Gentle traction, sharp dissection |
| Pudendal nerve/vessels | Sacrospinous fixation | Stay medial to ischial spine |
Slide 16 — Key Takeaways
- The ureter is the most surgically critical structure — always identify before clamping
- Uterine artery crosses the ureter 1.5–2 cm lateral to cervix ("water under the bridge")
- Cardinal and uterosacral ligaments are primary supports against uterine prolapse
- Retroperitoneal spaces (paravesical, pararectal) are the safety corridors of radical pelvic surgery
- Arcus tendineus fascia pelvis (ATFP) is the key lateral anchor for pelvic floor repair
- Autonomic nerves in uterosacral ligaments must be preserved in nerve-sparing procedures
Sources: TeLinde's Operative Gynecology (12th Ed.) | Bailey & Love's Short Practice of Surgery, 28th Ed. (pp. 1344, 1507, 1598)
This framework gives you 16 slides covering all major anatomical regions. You can expand any slide with more detail or ask me to generate anatomical diagrams for any specific structure (uterine ligaments, ureter course, retroperitoneal spaces, vascular anatomy, etc.).
Can u make it into a presentation (ppt) format
Reading File
Finding Files
Browsing Directory
Browsing Directory
Browsing Directory
Model call limits exceeded: run limit (5/5)
This is a shared conversation. Sign in to Orris to start your own chat.