Hiii,.I've just started surgery posting today
Welcome to your surgery posting! It's a big day. Here are a few things that'll help you hit the ground running:
On the ward
- Always know your patients before rounds — vitals, overnight events, pending investigations, drain outputs
- Carry a small notebook or use your phone for patient lists
- Learn to present concisely: "Mr. X, Day 2 post-op lap chole, afebrile, vitals stable, tolerating diet, drains nil, plan for discharge"
In the OT (Operating Theatre)
- Arrive early, scrub properly (watch a scrub technique video if you haven't)
- Stand where you don't block the light, and don't touch anything blue (sterile field)
- If you're unsure whether something is sterile — assume it's not
- Ask questions between cases, not during critical steps
Basics to know from Day 1
- Surgical knot tying (start practicing!)
- Basic instruments: scalpel, Kocher, Allis, retractors, needle holders
- Surgical site infection (SSI) prevention principles
- Pre-op, intra-op, and post-op roles
Mindset
- Be enthusiastic and proactive — volunteer to help with dressings, sutures, IV lines
- Residents remember students who show up early and stay engaged
- It's okay not to know — it's not okay not to try
Is there a specific topic you want to read up on, or something you'll be seeing today that I can help you prepare for?
Hemorrhage and shock 101 please
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Finding Sources
Reading File
Excellent — I now have comprehensive material from Guyton & Hall (physiology), Harrison's (stages/evaluation), Miller's Orthopaedics (ATLS classification table), Washington Manual (hemodynamic patterns), and Quick Compendium of Clinical Pathology. Here's your Surgery 101 guide on hemorrhage and shock:
Hemorrhage & Shock — Surgery 101
What Is Shock?
Shock is inadequate oxygen delivery to tissues relative to their metabolic needs. The result: cells switch to anaerobic metabolism → lactic acidosis → organ dysfunction → death if untreated.
Types of Shock (The Big 4)
| Type | Mechanism | Classic Example | Key Feature |
|---|---|---|---|
| Hypovolemic | ↓ intravascular volume | Trauma, GI bleed, burns | Cold, clammy, tachycardic |
| Distributive | ↓ SVR / vasodilation | Sepsis, anaphylaxis, neurogenic | Warm skin (early sepsis) |
| Cardiogenic | Pump failure | MI, myocarditis | Pulmonary edema |
| Obstructive | Outflow obstruction | Tension pneumo, tamponade, PE | Raised JVP |
In surgery, hypovolemic (hemorrhagic) shock is what you'll encounter most — especially in trauma and post-op patients.
Hemorrhagic Shock: The Physiology
When you bleed, the body fights back via sympathetic reflexes triggered by baroreceptors:
- Arteriolar vasoconstriction → ↑ Total Peripheral Resistance
- Venous constriction → maintains venous return
- Tachycardia → HR can rise to 160–180 bpm
Key insight: Cardiac output falls before arterial pressure does. The body sacrifices perfusion to maintain BP — so a normal BP does NOT mean the patient is fine.
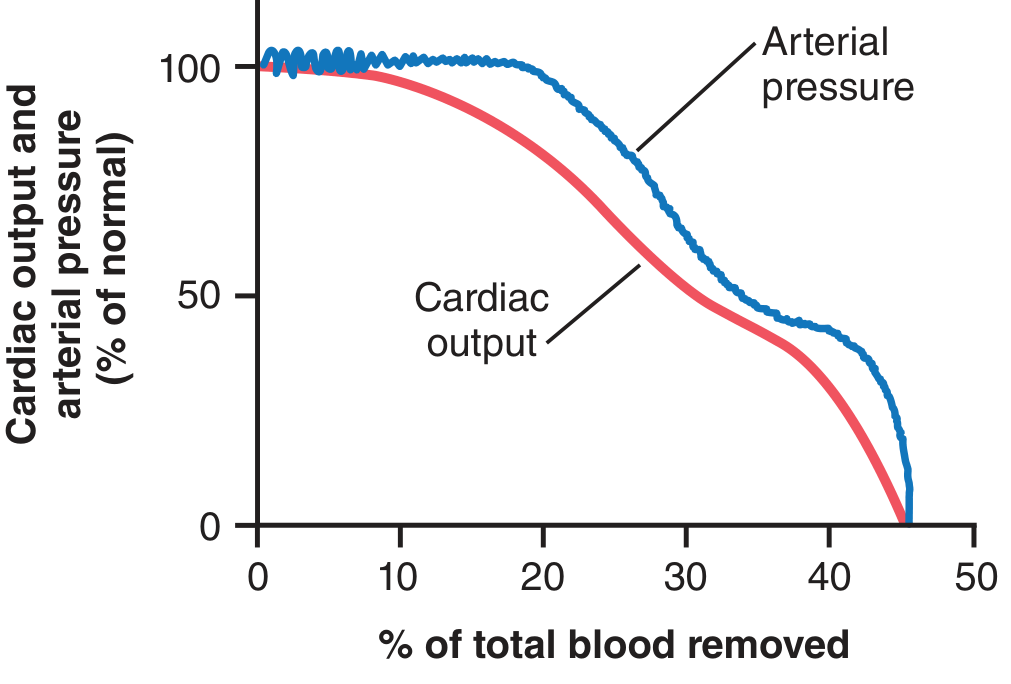
Up to 10% blood loss → almost no change in BP or cardiac output.
At 40–45% blood loss → both fall to zero. Death imminent.
— Guyton and Hall Textbook of Medical Physiology
ATLS Classification of Hemorrhagic Shock
This is the table you MUST know. Total blood volume ≈ 5L in a 70 kg adult.
| Class | Blood Loss | HR | BP | Urine Output | Mental Status | Treatment |
|---|---|---|---|---|---|---|
| I | <15% (<750 mL) | <100 | Normal | >30 mL/h | Normal | IV fluids |
| II | 15–30% (750–1500 mL) | >100 | ↓ | 20–30 mL/h | Anxious | IV fluids |
| III | 30–40% (1500–2000 mL) | >120 | ↓↓ | 5–15 mL/h | Confused | Fluids + blood |
| IV | >40% (>2000 mL) | >140 | ↓↓↓ | Negligible | Lethargic/unconscious | Fluids + blood (emergency) |
Memory trick: Class I = you're fine. Class II = worried. Class III = blood now. Class IV = dying.
— Miller's Review of Orthopaedics / ATLS
3 Stages of Shock (Harrison's)
-
Compensated (preshock): Body compensates — HR rises, SVR rises, BP maintained. Mild lactate elevation. Organs still okay. Reversible if caught here.
-
Decompensated (true shock): Compensatory mechanisms overwhelmed. Hypotension, organ dysfunction (↑ creatinine, altered consciousness, oliguria). Still reversible with aggressive treatment.
-
Irreversible shock: Permanent organ damage. Multiorgan failure. Even with treatment, death is likely.
⚠️ The goal is to catch shock at Stage 1 or 2 — never let it reach Stage 3.
Progressive Deterioration in Untreated Shock
If shock is not treated, a vicious cycle begins:
- ↓ perfusion → ischemic tissues → release of histamine, serotonin, cytokines
- Capillary permeability ↑ → fluid leaks into interstitium → further ↓ volume
- Lactic/carbonic acid → blood "sludging" in microvasculature → microthrombi
- CNS ischemia → vasomotor centre fails → complete cardiovascular collapse
— Guyton and Hall
Management: The Surgical Approach
Immediate steps (think ABCDE + hemorrhage control)
- Stop the bleeding — pressure, tourniquet, surgical control. "Stop the bleeding first" is the golden rule.
- Two large-bore IV lines (antecubital, 16G or larger)
- Send bloods: FBC, U&E, coagulation, cross-match, ABG (lactate!)
- Fluid resuscitation:
- Class I–II: Crystalloid (Normal saline or Lactated Ringer's)
- Class III–IV: Blood products. Rule of thumb — start pRBCs once crystalloids exceed 30 mL/kg (~2L)
- Target MAP ≥ 60–65 mmHg
- Monitor urine output (catheterise) — aim >0.5 mL/kg/h
- Warm the patient — hypothermia worsens coagulopathy
The Lethal Triad (avoid at all costs in trauma)
Hypothermia + Acidosis + Coagulopathy — each worsens the others. Breaking this cycle is the core of damage control surgery.
Quick Summary Card
Shock = ↓ O₂ delivery to tissues
Hemorrhagic shock = most common in surgery
Signs: tachycardia > hypotension (BP is a late sign!)
ATLS Class I→IV based on blood loss %
3 stages: Compensated → Decompensated → Irreversible
Treatment: Stop bleeding + Fluids + Blood products + Monitor UO
Avoid: Lethal triad (hypothermia + acidosis + coagulopathy)
Want me to go deeper on any part of this — fluid resuscitation choices, massive transfusion protocols, specific shock types like septic or neurogenic, or how to present a shocked patient on rounds?
General Examination and specific thyroid Examination
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Searching Images
thyroid goiter examination neck swelling
Loading Image
Searching Images
Graves disease exophthalmos proptosis hyperthyroidism clinical signs
Loading Image
I now have comprehensive material. Here's your complete guide:
General Examination + Thyroid Examination
PART 1: General Examination
This is the first thing you do after introducing yourself to the patient. It takes 30 seconds but tells you a lot. Think of it as reading the patient at a glance.
The 10 Components of General Examination
| Parameter | What to Look For |
|---|---|
| Build & Nutrition | Obese / average / thin / cachectic / wasted |
| Pallor | Conjunctival pallor (pull lower lid) → anaemia |
| Jaundice | Sclerae (yellow tinge) → liver/haemolysis |
| Cyanosis | Central (tongue) or peripheral (fingertips) |
| Clubbing | Grades 1–4; causes: lung, heart, liver, IBD |
| Lymphadenopathy | Cervical, axillary, inguinal nodes |
| Oedema | Pitting (press shin for 5s) vs non-pitting |
| Dehydration | Skin turgor (pinch abdomen), dry tongue, sunken eyes |
| Pulse | Rate, rhythm, volume, character |
| Temperature | Febrile / afebrile |
Surgery tip: Always add vitals (BP, HR, RR, SpO₂, temp) and urine output in surgical patients.
Presenting General Examination
"The patient is conscious, oriented, and cooperative. She is moderately built and nourished. She has no pallor, jaundice, cyanosis, or clubbing. There is no significant lymphadenopathy or pedal oedema."
PART 2: Thyroid Examination
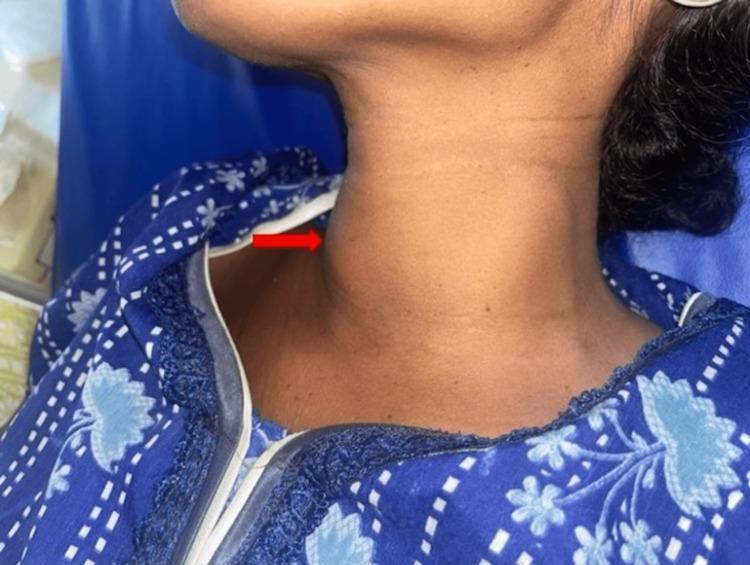
The thyroid is a butterfly-shaped gland sitting in the anterior neck, below the thyroid cartilage. Any swelling of the thyroid = a goitre.
The Key Rule Before You Start
Ask the patient to swallow while you watch the neck from across the room. A thyroid swelling moves up with swallowing — this distinguishes it from other neck lumps. A thyroglossal cyst moves up with tongue protrusion.
Step-by-Step Thyroid Examination
1. INSPECTION (from front, patient seated)
- Inspect the anterior neck at rest
- Ask patient to swallow (offer a glass of water) — does the swelling move?
- Note:
- Size — localised or diffuse?
- Shape — single nodule / multinodular / diffuse?
- Symmetry — unilateral or bilateral?
- Surface — smooth / irregular / nodular
- Overlying skin — erythema, dilated veins, scar (previous surgery)
- Visible pulsation — seen in vascular goitres (hyperthyroidism)
2. PALPATION (stand behind the patient — the surgical way)
Stand behind seated patient, place both hands around the neck with fingertips on the gland.
For each lobe, assess:
- Site — which lobe? Isthmus?
- Size — approximate cm
- Shape — diffuse or nodular
- Surface — smooth / irregular
- Consistency — soft / firm / hard / rubbery
- Soft → colloid goitre
- Rubbery/firm → Hashimoto's
- Hard/stony → malignancy or Riedel's
- Tenderness — tender in thyroiditis; non-tender in most others
- Mobility — mobile in benign; fixed/tethered → malignancy
- Fixity to skin — pinch skin over the swelling
- Fluctuation — cysts may fluctuate
- Ask patient to swallow again — confirm movement
Also palpate:
- Cervical lymph nodes — central compartment (level VI), lateral (levels II–IV) — for malignancy
- Trachea — is it central or deviated? (large goitre can deviate it)
- Berry's sign — absence of carotid pulsation on the side of a malignant thyroid (carotid encasement)
3. PERCUSSION
- Percuss over the upper sternum (manubrium) from top downward
- Dullness on sternal percussion → retrosternal extension of goitre
- This is often missed but is a surgical red flag
4. AUSCULTATION
- Place the bell of the stethoscope over each lobe
- Listen for a bruit (continuous swooshing murmur) → indicates increased vascularity
- Bruit is a hallmark of Graves' disease (active hyperthyroidism)
- Ask the patient to hold their breath during auscultation (to eliminate tracheal breath sounds)
Special Tests in Thyroid Examination
| Test | How | Positive = |
|---|---|---|
| Kocher's test | Press laterally on the goitre | Stridor → tracheal compression |
| Pemberton's sign | Ask patient to raise both arms above head | Facial plethora, JVP rise, cyanosis → retrosternal goitre compressing superior vena cava |
| Berry's sign | Palpate carotid pulse medially | Absent pulsation on one side → malignant infiltration |
Pemberton's sign is one of those dramatic signs you'll love showing on rounds.
General Examination in a Thyroid Patient
Don't forget to look beyond the neck. The general examination in thyroid disease is a goldmine:
In Hyperthyroidism (Graves' disease especially):
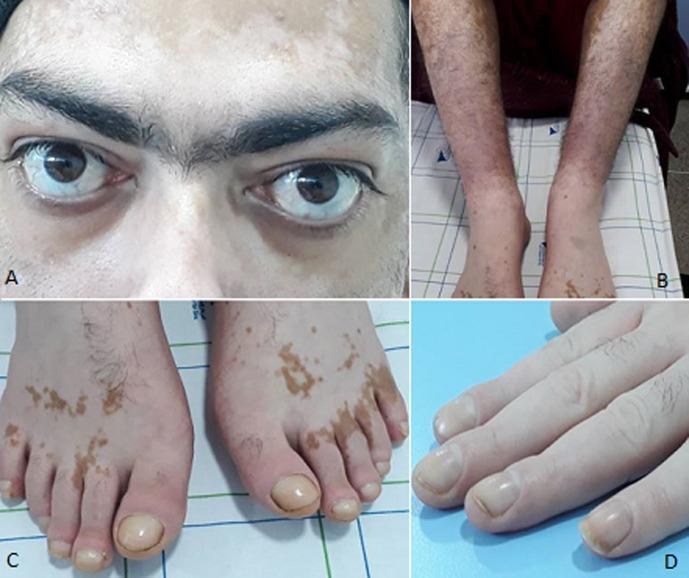
| System | Signs |
|---|---|
| Hands | Fine tremor (paper test), warm moist palms, thyroid acropathy (clubbing), onycholysis (Plummer's nails) |
| Pulse | Tachycardia, irregularly irregular (AF) |
| Eyes | Exophthalmos, lid lag (von Graefe's sign), lid retraction (Dalrymple's sign), chemosis, ophthalmoplegia |
| Skin | Pretibial myxedema (non-pitting, over shins), hyperpigmentation |
| Reflexes | Hyperreflexia |
In Hypothyroidism (Hashimoto's, post-surgery):
| System | Signs |
|---|---|
| Hands | Cold dry skin, nail brittleness |
| Face | Puffy, myxedematous face, loss of lateral eyebrow (Queen Anne's sign) |
| Hair | Dry, brittle, thinning; loss of outer third of eyebrows |
| Voice | Hoarse |
| Reflexes | Slow-relaxing reflexes (hung-up reflex) — a classic sign! |
| Pulse | Bradycardia |
How to Present Thyroid Examination
"On inspection, there is a diffuse smooth swelling in the anterior neck involving both lobes of the thyroid, which moves up with deglutition. On palpation from behind, the gland is diffusely enlarged, smooth, non-tender, firm, mobile, not fixed to skin or deep structures. Trachea is central. No cervical lymphadenopathy is palpable. On percussion, there is no retrosternal dullness. On auscultation, a bruit is present over both lobes. General examination reveals fine tremors, warm moist hands, and lid lag — consistent with hyperthyroidism."
Quick Summary Card
Thyroid swelling moves UP with swallowing ← key differentiator
Palpate from BEHIND (surgeon's approach)
Hard + fixed + LN → think malignancy
Bruit → Graves' disease (hyperthyroid)
Pemberton's sign → retrosternal extension
Tremor + tachycardia + exophthalmos → Graves' triad
Slow reflexes + puffy face + bradycardia → Hypothyroid
Sources: Harrison's Principles of Internal Medicine 22E; Guyton & Hall; Washington Manual of Medical Therapeutics
Want me to cover the investigations for a thyroid swelling next (USS, FNAC, TFTs, scintigraphy), or move on to another surgical examination topic?
Inguinal hernia 101
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
Hernias 101
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
Thyroid ca 101
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Searching Images
papillary thyroid carcinoma histology microscopy Orphan Annie eye nuclei
Loading Image
Finding Sources
Reading File
Finding Sources
Loading Image
Reading File
Loading Image
Reading File
I now have comprehensive material from Robbins Pathology, Robbins & Kumar Basic Pathology, Harrison's, and Cummings Otolaryngology. Here's your complete guide:
Thyroid Cancer — Surgery 101
Overview: The Big Picture
Thyroid cancer is the most common endocrine malignancy. The good news: most types are indolent and highly curable. The bad news: anaplastic thyroid cancer is one of the most lethal cancers known.
Mnemonic for the 4 types: "People Fear My Anger"
Papillary → Follicular → Medullary → Anaplastic
The 4 Types at a Glance
| Feature | Papillary | Follicular | Medullary | Anaplastic |
|---|---|---|---|---|
| Frequency | ~85% | 5–15% | <5% | ~1% |
| Cell of origin | Follicular cell | Follicular cell | C cells (parafollicular) | Follicular cell |
| Spread | Lymphatics | Blood (lungs, bone, liver) | Lymphatics + blood | Local invasion + blood |
| Marker | Thyroglobulin | Thyroglobulin | Calcitonin | None |
| Key mutation | BRAF V600E, RET fusion | RAS, PAX8/PPARG | RET point mutation | TP53 loss |
| Prognosis | Excellent (>95% 10-yr survival) | Good (minimally invasive) to moderate | Intermediate | Uniformly lethal |
| Radioiodine (RAI) sensitive? | Yes | Yes | No | No |
1. Papillary Thyroid Carcinoma (PTC)
The most common. Most are associated with radiation exposure (e.g., childhood RT to neck).
Key Histological Features (what the pathologist sees)
- Papillary architecture — finger-like projections with fibrovascular core
- "Orphan Annie eye" nuclei — optically clear, empty-looking nuclei
- Nuclear grooves and pseudo-inclusions
- Psammoma bodies — concentrically calcified concentric rings (almost pathognomonic for PTC)
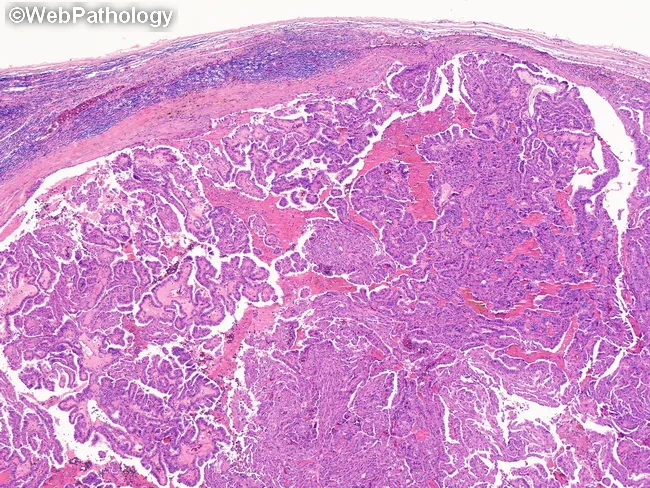
Key point: The nuclear features alone are diagnostic even WITHOUT papillary architecture.
Clinical Features
- Painless neck mass (within thyroid OR as a cervical lymph node metastasis)
- More common in women, peaks 30–50 years
- Can be multifocal within the thyroid
- FNAC (fine needle aspiration cytology) is usually diagnostic preoperatively
Spread & Prognosis
- Spreads via lymphatics → cervical lymph nodes (up to 50% of cases)
- Isolated nodal metastases do NOT worsen prognosis significantly in younger patients
- Rare haematogenous spread (lungs most common)
- 10-year survival >95% — one of the best prognoses of any cancer
2. Follicular Thyroid Carcinoma
More common in areas of iodine deficiency (important in India and South Asia).
Key Histological Features
- Uniform follicular cells resembling normal thyroid
- Diagnosis requires CAPSULAR ± VASCULAR INVASION — cannot be diagnosed on FNAC alone (this is why follicular lesions on FNAC need surgery)
- Distinguished from follicular adenoma only by invasion on histology
Clinical Features
- Presents as a solitary cold nodule
- More common in women, peak age 40–60 years
Spread & Prognosis
- Spreads via blood → lungs, bone, liver (haematogenous)
- Regional LN metastasis is uncommon
- Minimally invasive: <10% mortality at 10 years
- Widely invasive: ~50% mortality at 10 years
Surgeon's pearl: FNAC says "follicular lesion" → operate, because you cannot distinguish adenoma from carcinoma without the surgical specimen.
3. Medullary Thyroid Carcinoma (MTC)
Arises from parafollicular C cells, not follicular epithelium — so it does not respond to radioiodine.
Epidemiology
- 70% sporadic (solitary nodule, adults, peak 40s–50s)
- 30% familial — associated with MEN2A or MEN2B or Familial MTC
- All familial cases carry germline RET mutations
- Familial cases: bilateral, multifocal, younger patients
MEN Associations (must know)
| Syndrome | Components |
|---|---|
| MEN 2A | MTC + Phaeochromocytoma + Hyperparathyroidism |
| MEN 2B | MTC + Phaeochromocytoma + Mucosal neuromas + Marfanoid habitus |
| Familial MTC | MTC only (germline RET, no other MEN features) |
Any patient with MTC should be screened for phaeochromocytoma before surgery — operating on an undiagnosed phaco can kill the patient.
Key Histological Feature
- Polygonal to spindle cells in nests/trabeculae
- Amyloid deposits in stroma (derived from calcitonin polypeptides) — characteristic!
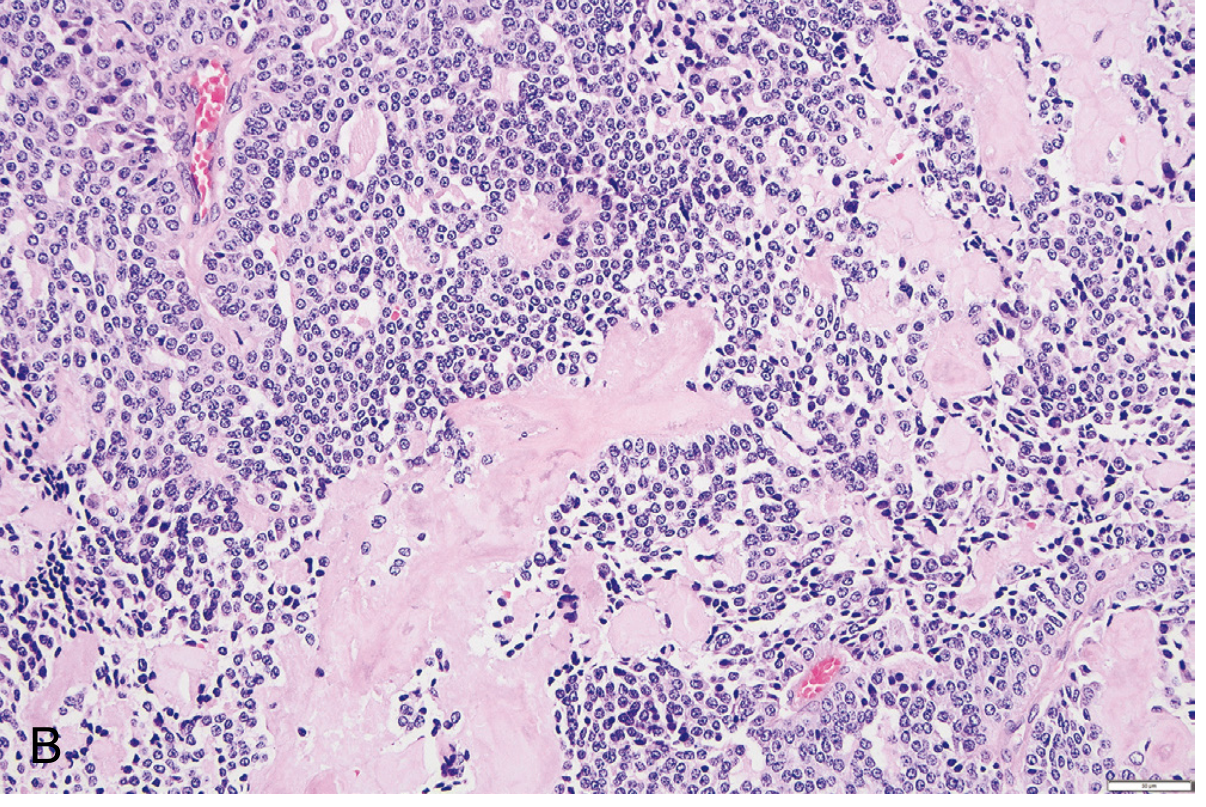
Tumour Marker
- Calcitonin — used for diagnosis AND follow-up (if calcitonin rises post-op → recurrence)
- Some also secrete serotonin, ACTH, VIP
Treatment
- Surgery (total thyroidectomy + central neck dissection)
- NOT radioiodine-sensitive
- Targeted therapy (vandetanib, cabozantinib) for metastatic disease
4. Anaplastic (Undifferentiated) Thyroid Carcinoma
The most aggressive thyroid cancer — and one of the most lethal cancers in oncology.
Key Points
- Arises de novo or by dedifferentiation of a pre-existing PTC or follicular carcinoma (TP53 loss is the key step)
- Mean age at presentation: 65 years
- Up to 25% have a prior history of well-differentiated thyroid carcinoma
Clinical Presentation
- Rapidly enlarging, bulky, hard neck mass — this is the hallmark
- Symptoms of compression: dysphagia, dysphonia (hoarseness), dyspnea, stridor
- Most are already locally invasive or metastatic (lungs) at presentation
Prognosis
- Death in <1 year in most cases
- NOT radioiodine-sensitive
- Surgery rarely curative — palliative approach with external beam RT ± targeted therapy
Investigations for a Thyroid Nodule (Work-up)
Step 1: TSH (is it hyper/hypo/euthyroid?)
Step 2: Ultrasound (USS) — size, echogenicity, margins, calcifications, LN
Step 3: FNAC (fine needle aspiration cytology) → Bethesda system reporting
Step 4: If follicular lesion on FNAC → surgery (hemithyroidectomy)
Step 5: CT neck/chest if large, substernal, or suspected malignancy
Step 6: Calcitonin if MTC suspected
Step 7: Thyroglobulin post-thyroidectomy for follow-up
The Bethesda System (FNAC reporting for thyroid)
| Bethesda Category | Diagnosis | Malignancy Risk | Action |
|---|---|---|---|
| I | Non-diagnostic | — | Repeat FNAC |
| II | Benign | <3% | Observe |
| III | Atypia of undetermined significance | ~10–30% | Repeat / molecular testing |
| IV | Follicular neoplasm | 25–40% | Hemithyroidectomy |
| V | Suspicious for malignancy | 60–75% | Surgery |
| VI | Malignant | >97% | Surgery |
Treatment Summary
| Type | Surgery | Radioiodine (¹³¹I) | TSH Suppression | Monitoring |
|---|---|---|---|---|
| Papillary | Total thyroidectomy ± neck dissection | Yes (if high risk) | Yes | Thyroglobulin + USS |
| Follicular | Total thyroidectomy | Yes | Yes | Thyroglobulin + USS |
| Medullary | Total thyroid + central neck dissection | No | No | Calcitonin |
| Anaplastic | Palliative surgery/tracheostomy | No | No | CT imaging |
Red Flags on History/Exam Suggesting Malignancy
✗ Hard, firm, fixed, non-tender thyroid nodule
✗ Rapid growth
✗ Hoarseness (recurrent laryngeal nerve invasion)
✗ Dysphagia (oesophageal invasion)
✗ Cervical lymphadenopathy
✗ History of neck radiation
✗ Age extremes (<20 or >60)
✗ Male sex (more likely malignant than in females)
✗ Family history of MTC or MEN
Quick Summary Card
4 types: Papillary (85%) > Follicular > Medullary > Anaplastic
PTC: Orphan Annie nuclei + psammoma bodies, lymphatic spread, excellent prognosis
Follicular: Cannot diagnose by FNAC alone, haematogenous spread
Medullary: C cells, calcitonin marker, amyloid on histo, RET mutation, MEN2
Anaplastic: Rapidly enlarging hard mass, TP53 loss, uniformly lethal
Work-up: USS → FNAC (Bethesda) → Surgery
Radioiodine works: PTC and FTC only
Sources: Robbins & Kumar Basic Pathology; Robbins, Cotran & Kumar Pathologic Basis of Disease; Harrison's Principles of Internal Medicine 22E; Cummings Otolaryngology
Want me to cover the surgical complications of thyroidectomy (RLN injury, hypoparathyroidism, etc.) or move on to another surgery topic?
Acute cholecystitis
Reading File
Your credits are exhausted. Your daily credits reset tomorrow, or you can purchase a top-up for more.
This is a shared conversation. Sign in to Orris to start your own chat.