Explain the clicnial examination of respirator6 system in detail Inspection palpation auscultation percussion all their components in detail refer gold standard textbooks
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Searching Images
respiratory system clinical examination chest inspection palpation percussion auscultation
I now have all the content needed to deliver a comprehensive, textbook-referenced answer. Let me compose it fully.
Clinical Examination of the Respiratory System
References: Fishman's Pulmonary Diseases and Disorders (2-Volume Set), Murray & Nadel's Textbook of Respiratory Medicine, Harrison's Principles of Internal Medicine 22e, Goldman-Cecil Medicine
Overview & Patient Positioning
The patient should be seated upright (45°), adequately exposed from the waist up. Examination follows the classical sequence: General Inspection → Hands & Periphery → Face & Neck → Inspection of Chest → Palpation → Percussion → Auscultation.
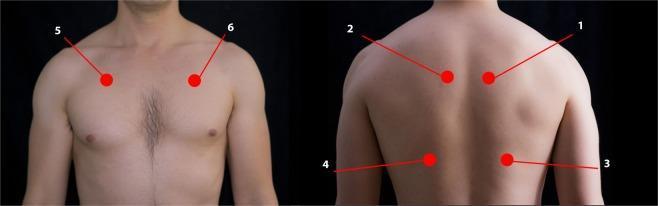
I. INSPECTION
A. General Inspection (from the end of the bed)
Observation from the foot of the bed before touching the patient is a hallmark of expert clinical method.
1. General appearance
- Distress, tachypnoea, use of accessory muscles (sternocleidomastoid, scalenes, trapezius)
- Inability to complete a full sentence in one breath (severe obstruction)
- Cachectic habitus — suggests malignancy or COPD
2. Respiratory pattern
| Pattern | Characteristics | Causes |
|---|---|---|
| Normal | 12–20 breaths/min, regular | — |
| Tachypnoea | >20/min, shallow | Pneumonia, pulmonary embolism, pleural effusion |
| Bradypnoea | <12/min | Sedation, raised ICP |
| Kussmaul | Deep, rapid, regular (air hunger) | Metabolic acidosis (DKA, uraemia) |
| Cheyne-Stokes | Waxing-waning cycles with apnoea | Heart failure, uraemia, CNS lesions |
| Biot's | Irregular rate & depth with sudden apnoea | Medullary lesions, raised ICP |
| Slow, deep | Prolonged expiration | Severe airflow obstruction (COPD, asthma) |
| Rapid, shallow | Low tidal volumes | Interstitial lung disease, kyphoscoliosis, neuromuscular disease |
Fishman's: "Patients with severe airflow obstruction often take slow, deep breaths, whereas rapid and shallow breaths are often seen with restrictive processes, such as interstitial lung disease or kyphoscoliosis."
3. Paradoxical breathing
In the supine position, inward movement of the abdomen on inspiration (instead of outward) indicates respiratory muscle weakness or diaphragmatic paralysis.
B. Inspection of the Hands & Periphery
1. Clubbing
- Grade I: Loss of angle between nail and nailbed (Lovibond angle >180°)
- Grade II: Increased curvature of nail
- Grade III: Drumstick appearance
- Grade IV: Hypertrophic pulmonary osteoarthropathy (periosteal new bone, wrist/ankle pain)
Respiratory causes: bronchogenic carcinoma, bronchiectasis, lung abscess, empyema, fibrosing alveolitis, mesothelioma, cystic fibrosis. (Not a feature of COPD or asthma.)
2. Peripheral cyanosis
Blue discolouration of fingertips/nailbeds; can occur with low cardiac output + peripheral vasoconstriction without hypoxaemia.
3. Fine tremor / flap (asterixis)
Irregular, coarse flapping tremor of outstretched hands = CO₂ retention (type II respiratory failure, PaCO₂ >6 kPa). Best elicited with wrists cocked back, eyes closed, for 15 seconds.
4. Tobacco staining
Yellow-brown staining of fingers/nails.
5. Pulse
- Tachycardia → infection, PE, hypoxia
- Pulsus paradoxus (>10 mmHg drop in systolic BP on inspiration) → severe asthma, cardiac tamponade. Palpated as apparent disappearance of radial pulse on deep inspiration.
6. Bounding pulse + warm peripheries
Suggests CO₂ retention causing peripheral vasodilation.
C. Inspection of the Face
1. Central cyanosis — Examine mucous membranes (lips, tongue, sublingual area). Requires ≥5 g/dL reduced haemoglobin in capillaries.
Fishman's: "The discoloration is most apparent in the lobes of the ears, the cutaneous surfaces of the lips, and the nail beds. In patients with dark skin, the mucus membranes and the retina are important sites to examine for cyanosis."
2. Pursed-lip breathing — characteristic of COPD (maintains intrinsic PEEP, prevents small airway collapse)
3. Nasal flaring — accessory muscle use; prominent in children
4. Plethoric face — polycythaemia (chronic hypoxia), SVC obstruction
5. Horner syndrome (enophthalmos, ptosis, miosis, anhidrosis) — Pancoast tumour invading stellate ganglion
6. Conjunctival pallor — anaemia contributing to dyspnoea
D. Inspection of the Neck
1. Jugular venous pressure (JVP)
- Elevated JVP → cor pulmonale, right heart failure from chronic lung disease
- Non-pulsatile, non-compressible distension → SVC obstruction (malignancy)
2. Tracheal position — visually assessed first; midline vs. deviated. More accurately assessed by palpation (see below).
3. Lymphadenopathy — cervical nodes enlargement suggests malignancy, sarcoidosis, TB, lymphoma
4. Accessory muscle use — sternocleidomastoids visibly contracting during quiet respiration = significant respiratory distress
E. Inspection of the Chest Wall
1. Shape & symmetry
| Deformity | Description | Cause/Significance |
|---|---|---|
| Barrel chest | Increased AP diameter; horizontal ribs; thoracic kyphosis | Chronic hyperinflation (COPD, severe asthma) |
| Pectus excavatum | Depressed sternum ("funnel chest") | Congenital; can compress heart rightward |
| Pectus carinatum | Protruding sternum ("pigeon chest") | Childhood chronic respiratory disease; rickets |
| Kyphosis | Posterior curvature of spine | Restrictive ventilatory defect |
| Scoliosis | Lateral spinal curvature | Restrictive ventilatory defect; can cause respiratory failure |
| Harrison's sulci | Bilateral horizontal grooves at diaphragm insertion level | Childhood respiratory disease with increased inspiratory effort |
2. Chest expansion
- Bilateral reduction: COPD, bilateral pleural disease
- Unilateral reduction (lag): pneumothorax, pleural effusion, pneumonia, phrenic nerve palsy, fibrosis
Fishman's: "A visible lag in expansion of one side of the thorax localizes a pleural effusion, pulmonary infection, or paralyzed diaphragm."
3. Scars & deformities
- Thoracotomy scar, VATS ports, drain sites, radiotherapy tattoo marks
- Subcutaneous emphysema (crepitus on inspection/palpation)
4. Chest wall veins
- Distended collateral veins flowing upwards → SVC obstruction
- Flowing downwards → IVC obstruction
5. Respiratory muscle use
- Intercostal recession (indrawing): increased work of breathing
- Subcostal/supraclavicular recession: severe distress
II. PALPATION
A. Tracheal Position
Technique: With the patient's neck slightly flexed, the examiner's middle finger is placed into the suprasternal notch and pressure applied gently into each side of the trachea. Equal distances on each side = midline.
Interpretation:
| Finding | Cause |
|---|---|
| Trachea pulled toward abnormal side | Pulmonary fibrosis, lung collapse, pneumonectomy, fibrothorax |
| Trachea pushed away from abnormal side | Tension pneumothorax, large pleural effusion, mediastinal mass |
| Tracheal tug (downward movement on inspiration) | Severe airflow obstruction (COPD) |
Fishman's: "The position of the trachea determined by palpation in the suprasternal notch may be helpful in detecting a lateral displacement of the upper mediastinum."
B. Lymph Nodes
Systematically palpate: submental, submandibular, anterior cervical chain, posterior cervical chain, supraclavicular fossae, axillae. Supraclavicular nodes (especially left — Virchow's/Troisier's node) suggest thoracic or upper GI malignancy.
C. Chest Expansion (Quantitative)
Upper lobe (anterior): Examiner's hands placed on anterior upper chest, thumbs meeting in the midline at the clavicular level. Patient takes a deep breath. Thumb separation is measured.
Lower lobe (posterior): Examiner's hands placed symmetrically over the posterior lower chest, thumbs meeting at the midline (T10 level). Normal excursion: 5–8 cm bilaterally and equal.
Unilateral reduction indicates ipsilateral disease. Bilateral reduction indicates bilateral lung disease.
D. Vocal Fremitus (Tactile Fremitus)
Technique: Place the ulnar border of both hands simultaneously on symmetric areas of the chest; ask patient to say "ninety-nine" repeatedly. Compare side to side systematically — posterior, lateral, anterior chest.
| Finding | Mechanism | Cause |
|---|---|---|
| Increased TVF | Sound transmits better through consolidated (solid) lung | Consolidation (lobar pneumonia) |
| Decreased TVF | Sound blocked or attenuated | Pleural effusion (fluid blocks), pleural thickening, pneumothorax (no conducting medium), COPD (hyperinflated) |
| Absent TVF | No transmission | Large effusion, complete pneumothorax |
E. Pleural Rub (Palpable)
A palpable friction rub (leathery, grating sensation) felt over inflamed pleura.
F. Subcutaneous Emphysema
Crepitus on palpation of the chest wall (crackling like bubble-wrap); indicates air in subcutaneous tissues — suggests pneumothorax, tracheobronchial injury, or surgical emphysema.
G. Apex Beat & Cardiac Shift
- Apex displaced laterally/inferiorly → cor pulmonale, right ventricular dilatation
- Right ventricular heave palpated in parasternal region → pulmonary hypertension
H. Hoover Sign (Palpation)
Examiner places both hands lightly over the lower hemithorax with thumbs touching below the xiphoid. On deep inspiration, instead of normal outward/upward movement, the lower ribs move inward — indicates severe hyperinflation and diaphragm flattening (COPD).
Fishman's: "Hoover sign may be useful in disclosing a unilateral lag in motion of one side of the chest due to pleuritis or a pleural effusion... elicited by comparing the displacement from the midline during a patient's deep inspiration of the examiner's hands, each placed lightly over one hemithorax, with thumbs touching beneath the xiphoid."
III. PERCUSSION
Technique (Mediate Percussion)
The middle finger of the non-dominant hand (pleximeter) is pressed firmly flat against the chest wall in the intercostal space (not over a rib). The tip of the dominant middle finger (plexor) strikes the middle phalanx of the pleximeter with a quick, sharp, wrist-flexion movement. Compare side to side, systematically.
Percussion Notes — Spectrum
| Note | Quality | Normal site | Pathological cause |
|---|---|---|---|
| Resonant | Low-pitched, hollow | Normal lung | Normal |
| Hyperresonant | Booming, drum-like | Gastric bubble | Pneumothorax, emphysema (bilateral) |
| Tympanitic | Drum-like, musical | Gastric air | Pneumothorax (very large) |
| Dull | Higher-pitched, shorter, thud | Liver, heart, consolidated lung | Consolidation, lung collapse |
| Stony dull | Extremely dull, no resonance at all | Never normal | Pleural effusion, haemothorax, empyema |
Memory aide: Stony dull = fluid (the stone sinks in water); Hyper-resonant = air.
Sites to Percuss
Anterior: Start at the clavicle (direct percussion), then in each intercostal space from 2nd downward; identify:
- Right heart border (3rd–5th ICS parastemal)
- Liver dullness (5th ICS right MCL, normally)
- Left cardiac dullness
- Traube's space (normally tympanic — LLQ costal margin; dull if effusion or splenomegaly)
Posterior: From apex of scapula down to 11th rib; percuss 2.5 cm lateral to spinous processes; compare bilaterally.
Axillary (lateral): 4th–8th ICS in the mid-axillary line; particularly important to outline upper border of a pleural effusion.
Special Tests
1. Shifting dullness (pleural effusion)
Percuss from resonant to dull (supine, moving laterally); mark the line of dullness. Roll patient 45° toward you — if the dull note shifts superiorly (fluid moves by gravity), this is a pleural effusion. >300–500 mL usually needed to detect.
2. Level of diaphragm / diaphragmatic excursion
Find the lower border of lung resonance on full inspiration, then on full expiration posteriorly. Normal excursion: 4–6 cm. Reduced in phrenic nerve palsy, COPD, subphrenic collection. High hemidiaphragm: phrenic nerve palsy, hepatomegaly (right), atelectasis.
3. Kronig's isthmus
A band of resonance over the apex (~5–6 cm width); narrows in apical fibrosis (old TB) or consolidation.
4. Obliteration of cardiac and hepatic dullness
Bilateral hyperresonance obscuring liver dullness → severe emphysema.
Percussion Findings in Common Conditions
| Condition | Percussion note | Expansion | TVF |
|---|---|---|---|
| Consolidation (pneumonia) | Dull | Reduced ipsilateral | Increased |
| Pleural effusion | Stony dull | Reduced ipsilateral | Absent/decreased |
| Pneumothorax | Hyper-resonant | Reduced ipsilateral | Absent |
| COPD/emphysema | Hyper-resonant | Reduced bilateral | Decreased bilateral |
| Pulmonary fibrosis | Dull | Reduced bilateral | Increased |
| Lung collapse (proximal obstruction) | Dull | Reduced ipsilateral | Absent/reduced |
IV. AUSCULTATION
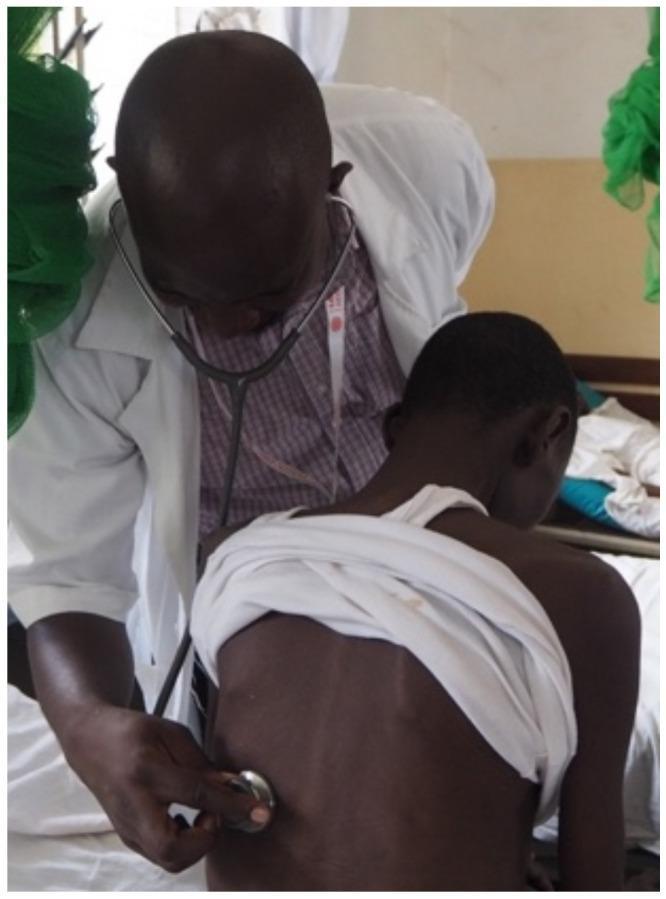
Technique
Use the diaphragm of the stethoscope (firm contact). Ask patient to breathe deeply through an open mouth. Auscultate systematically from apex to base, comparing sides simultaneously or alternating between symmetric points. Cover: posterior (most useful), lateral, and anterior chest.
Auscultation sites — posterior: upper zones (above T3), mid-zones (T3–T5), lower zones (T5–T10); lateral: mid-axillary line; anterior: clavicle, 2nd ICS, 4th ICS.
A. Breath Sounds
1. Vesicular breath sounds (normal)
- Soft, low-pitched, rustling (like wind in trees)
- Inspiration > expiration; no silent interval
- Heard over most of the normal lung
- Generated by turbulent airflow in larger airways, transmitted to periphery through lung parenchyma
2. Bronchial breath sounds (abnormal in the periphery)
- Loud, high-pitched, tubular/hollow quality (like blowing air through a tube)
- Expiration ≥ inspiration; distinct silent gap between I and E phases
- Heard normally only over the trachea/large airways
- In the periphery, they indicate transmission of tracheal sounds through consolidated (solid) lung
- Causes: lobar pneumonia (consolidation), large pulmonary infarction, fibrosing alveolitis (sometimes), cavities with pneumonia around them
3. Bronchovesicular sounds
- Intermediate quality; I = E; no silent gap
- Normal over right 1st–2nd ICS anteriorly (near right main bronchus) and between scapulae posteriorly
- Abnormal elsewhere
4. Diminished/absent breath sounds
- Pneumothorax (no conducting medium)
- Pleural effusion (fluid attenuates sound)
- COPD/emphysema (reduced airflow + hyperinflation)
- Obesity, muscular chest wall
- Complete bronchial obstruction (collapse behind)
B. Added Sounds (Adventitious Sounds)
1. Crackles (Crepitations, Rales)
Fine crackles:
- High-pitched, brief, non-musical
- Like Velcro tearing or rubbing hair between fingers near the ear
- Heard in: end-inspiratory phase
- Mechanism: sudden opening of previously collapsed small airways/alveoli (alveolar recruitment)
- Causes: pulmonary fibrosis (fine, end-inspiratory, bibasal, "Velcro crackles"), pulmonary oedema (early), pneumonia
Coarse crackles:
- Low-pitched, bubbling, longer duration
- Early inspiratory or pan-inspiratory
- Mechanism: air moving through secretions in large airways
- Causes: bronchiectasis, COPD with mucus, resolving pneumonia, pulmonary oedema (late/severe)
Post-tussive crackles (clearing with cough) suggest secretions in airways (bronchiectasis, infection). Crackles that persist after coughing suggest parenchymal disease.
2. Wheeze (Rhonchi)
- Musical, high-pitched (or low-pitched) sounds, predominantly expiratory (may be biphasic)
- Mechanism: rapid airflow through a narrowed airway creating oscillation of airway walls
- Types:
- Polyphonic wheeze (multiple tones simultaneously): diffuse airway narrowing → asthma, COPD
- Monophonic fixed wheeze (single tone, same character throughout cycle): single large airway obstruction → bronchial carcinoma, foreign body
- Inspiratory wheeze = stridor when heard without stethoscope (see below)
- Absent wheeze in severe asthma = silent chest (ominous sign — insufficient airflow to generate wheeze)
3. Stridor
- High-pitched, inspiratory (predominantly) monophonic sound
- Audible without a stethoscope, louder on inspiration
- Indicates upper airway or large central airway obstruction
- Causes: laryngeal oedema (anaphylaxis, croup), epiglottitis, foreign body, tracheal compression (goitre, mediastinal mass), tracheal stenosis, bilateral vocal cord palsy
4. Pleural Friction Rub
- Creaking, grating, or leather-rubbing sound (like new shoe leather)
- Heard in both inspiration and expiration, does not change with coughing
- Localised (in one area of the chest)
- Mechanism: roughened inflamed visceral and parietal pleurae rubbing together
- Causes: pleurisy (viral, bacterial), pulmonary infarction, mesothelioma, adjacent pneumonia
- Disappears if effusion develops (separates the pleural surfaces)
C. Vocal Resonance
Patient says "ninety-nine" while you auscultate. Normal: low-pitched, muffled sound.
1. Increased vocal resonance
Clearer, louder transmission of voice → consolidation (same mechanism as bronchial breathing)
2. Whispering pectoriloquy
Ask patient to whisper "one-two-three." Normally whispers are barely audible. If clearly heard through the stethoscope → consolidation (sound transmitted clearly through solid lung to chest wall)
3. Aegophony (Egophony)
Voice takes on a nasal, bleating, "E-to-A" quality. When patient says "E", you hear "A" through the stethoscope. Found at the upper border of a pleural effusion (where lung is partially collapsed but still in contact with chest wall). Also present in consolidation.
4. Decreased vocal resonance
Pleural effusion, pneumothorax, COPD.
Summary Comparison Table — Bedside Findings
| Consolidation | Pleural Effusion | Pneumothorax | COPD | Fibrosis | Collapse | |
|---|---|---|---|---|---|---|
| Trachea | Central | Pushed away (large) | Pushed away (tension) | Central | Pulled toward | Pulled toward |
| Expansion | ↓ ipsilateral | ↓ ipsilateral | ↓ ipsilateral | ↓ bilateral | ↓ bilateral | ↓ ipsilateral |
| TVF/VR | ↑ | ↓/absent | Absent | ↓ bilateral | ↑ | ↓/absent |
| Percussion | Dull | Stony dull | Hyper-resonant | Hyper-resonant | Dull | Dull |
| Breath sounds | Bronchial | Absent/↓ | Absent | Vesicular ↓ | Vesicular ↓ | Absent/bronchial |
| Added sounds | Fine crackles | Rub (if pleuritis) | None | Wheeze, coarse crackles | Fine bibasal crackles | None |
| Aegophony | + | + (at upper border) | − | − | − | − |
V. COMPLETE SEQUENCE — SYSTEMATIC APPROACH
- Wash hands, introduce, consent, position patient at 45°
- End-of-bed inspection: general, respiratory pattern, distress
- Hands: clubbing, cyanosis, tremor/flap, pulse, staining
- Arms/face: BP (paradoxus if suspected), eyes (Horner, pallor), mouth (central cyanosis, voice quality), JVP
- Neck: trachea position (look → palpate), lymph nodes, accessory muscles
- Chest inspection: shape, scars, veins, chest wall movement, symmetry
- Palpation: trachea (confirm), expansion (anterior upper + posterior lower), TVF (compare sides)
- Percussion: systematically anterior → lateral → posterior; diaphragm level; shifting dullness if relevant
- Auscultation: breath sounds, added sounds, vocal resonance; anterior → lateral → posterior
- Complete: check ankles for oedema (cor pulmonale), examine sputum if available, temperature chart
Key Eponyms & Signs
| Sign | Description | Meaning |
|---|---|---|
| Hoover sign | Inward movement of lower ribs on inspiration | Severe COPD, diaphragm hyperinflation |
| Hamman's sign | Crunching sound synchronous with heartbeat | Pneumomediastinum |
| Pemberton's sign | Facial plethora, JVP rise on raising arms | SVC compression (retrosternal goitre, mediastinal mass) |
| Troisier's sign | Left supraclavicular lymphadenopathy | Intrathoracic/abdominal malignancy |
| Pancoast syndrome | Shoulder/arm pain + Horner's + wasting | Apical lung tumour |
| Ewart's sign | Dull percussion + bronchial breathing below left scapula | Large pericardial effusion (compression of left lower lobe) |
| Traube's space | Normally resonant left costal LLQ | Dull = left pleural effusion, splenomegaly |
Sources: Fishman's Pulmonary Diseases and Disorders, 5e (Grippi et al.); Murray & Nadel's Textbook of Respiratory Medicine, 7e; Harrison's Principles of Internal Medicine, 22e; Goldman-Cecil Medicine, International Edition.
Complete it
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Searching Images
clubbing fingers grading respiratory disease
Searching Images
barrel chest hyperinflation COPD inspection kyphosis pectus excavatum deformity
Searching Images
percussion technique chest mediate pleximeter plexor
I now have all the additional content needed. Here is the complete continuation and expansion of the previous answer — filling in all remaining components:
Clinical Examination of the Respiratory System — Complete Reference
Continued from previous response. References: Fishman's Pulmonary Diseases and Disorders 5e; Harrison's Principles of Internal Medicine 22e; Murray & Nadel's Textbook of Respiratory Medicine 7e; Washington Manual of Medical Therapeutics; Goldman-Cecil Medicine; Textbook of Family Medicine 9e
ADDITIONS & COMPLETIONS TO INSPECTION
Clubbing — Expanded Grading
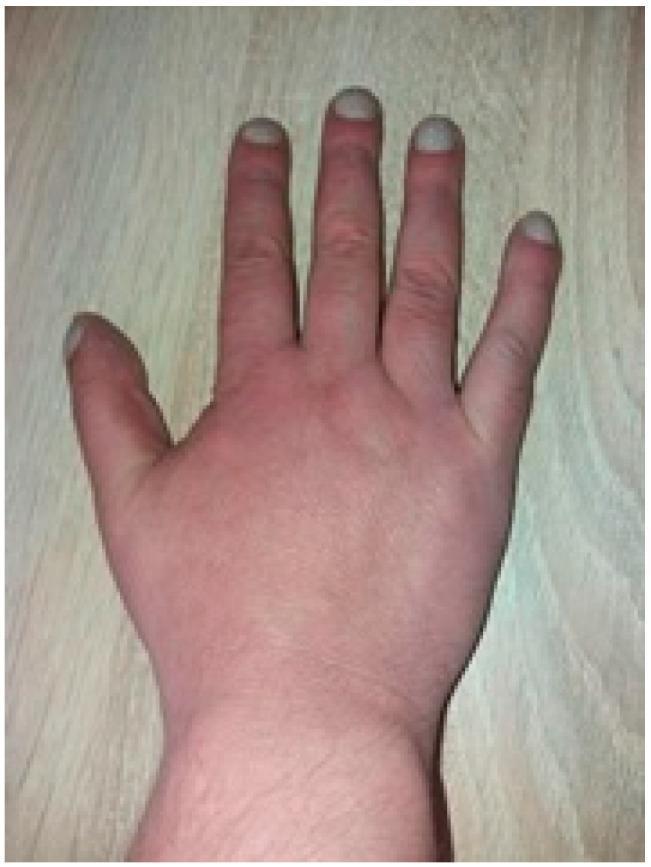
Schamroth's window test (bedside sign):
Place the dorsal surfaces of the terminal phalanges of the same finger of both hands together (fingernail to fingernail). Normally a diamond-shaped window is visible at the nail bases. In clubbing, this window is obliterated.
Grading of Clubbing (Cyanotic/Respiratory Scale):
| Grade | Finding |
|---|---|
| 1 | Fluctuation of nailbed (spongy feel on pressing) + loss of Lovibond angle (normally 160°, now ≥180°) |
| 2 | Grade 1 + increased convexity of nail (watch-glass nail) |
| 3 | Grade 2 + drumstick swelling of distal phalanx |
| 4 | Grade 3 + hypertrophic pulmonary osteoarthropathy (periosteal bone formation; wrist/ankle pain, joint swelling) |
Respiratory causes of clubbing:
| Category | Specific conditions |
|---|---|
| Malignancy | Bronchogenic carcinoma (most common adult cause), mesothelioma, lymphoma of mediastinum |
| Suppurative lung disease | Bronchiectasis, lung abscess, empyema, cystic fibrosis |
| Diffuse pulmonary fibrosis | Idiopathic pulmonary fibrosis (IPF), asbestosis |
| Chronic hypoxia | Cyanotic congenital heart disease |
| Not a feature of | COPD, asthma, simple pleural effusion, sarcoidosis without fibrosis |
Washington Manual: "Clubbing is not a feature of COPD alone, so its presence should prompt an evaluation for other conditions, especially lung cancer."
Chest Deformities — Images
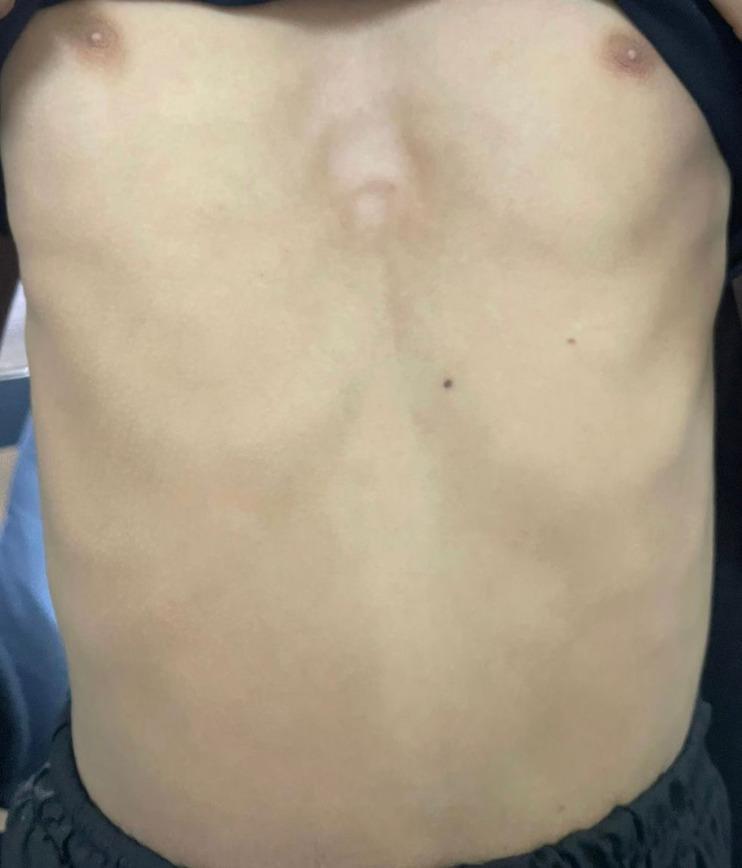
Respiratory Pattern — Additional Types
Apneustic breathing: Prolonged inspiratory pause before exhalation; caused by pontine lesions (stroke, encephalitis).
Ataxic (Biot's) breathing: Completely irregular, no pattern, random deep and shallow breaths interspersed with apnoea; caused by medullary lesions (compression, Arnold-Chiari malformation, opioid overdose).
Orthopnoea: Dyspnoea on lying flat (lying down increases venous return → worsens pulmonary oedema); quantified by number of pillows required.
Platypnoea: Dyspnoea worse on sitting up, relieved by lying flat (rare; hepatopulmonary syndrome, atrial septal defect in upright position).
Trepopnoea: Dyspnoea worse when lying on one side; massive unilateral pleural effusion.
ADDITIONS TO PALPATION
Tracheal Deviation — Expanded
Away from lesion (pushed):
- Tension pneumothorax (emergency — trachea + mediastinum pushed; hypotension + absent breath sounds)
- Large pleural effusion (>1000 mL usually required for detectable shift)
- Large mediastinal mass
Toward lesion (pulled/sucked):
- Lung fibrosis (ipsilateral volume loss pulls trachea)
- Complete lung collapse (atelectasis) — ipsilateral pull
- Pneumonectomy — trachea pulled toward the operated side
- Fibrothorax
Special tracheal signs:
- Tracheal tug (Oliver's sign): Downward tug of larynx/trachea synchronous with heartbeat; aortic aneurysm. Also used to mean downward tug on inspiration in severe COPD hyperinflation.
- Fixed midline trachea despite large effusion → suggests malignant fixation of mediastinum (e.g., malignant mesothelioma, lymphoma).
Chest Expansion — Detailed Measurement
Upper zone (anterior):
- Hands placed on anterior chest, thumbs at sternal angle (angle of Louis, 2nd rib junction)
- Examiner's fingers curved around the upper ribs laterally
- Normal: 3–5 cm separation of thumbs
Lower zone (posterior):
- Most important and most sensitive
- Hands on posterior lower chest at T10; thumbs lifted off the skin (do not press), meeting at midline
- Patient takes full breath in — thumbs diverge symmetrically
- Normal: 5–8 cm; record as "5 cm bilaterally equal" or note asymmetry
Reduced expansion causes (asymmetric/unilateral):
Pleural effusion, pneumothorax, consolidation, collapse, fibrosis, pleural thickening
Reduced expansion (bilateral):
COPD, bilateral fibrosis, neuromuscular weakness (Guillain-Barré, motor neurone disease, myasthenia gravis), kyphoscoliosis, ankylosing spondylitis
Vocal Fremitus — Complete Method
Technique:
Use the ulnar border (hypothenar eminence) or flat of the hand — NOT the fingertips — as the bony structures transmit vibration better. Apply to the chest wall while patient says "ninety-nine" or "one-one-one." Work systematically comparing both sides — start at the apices and progress downward. Avoid the scapulae.
Why ulnar border? The ulnar border (8th cranial and ulnar nerve supply) is more sensitive to vibration than the fingertips.
| Anatomical zone | Side compared |
|---|---|
| Above scapular spines (upper zone) | Left vs right |
| Between scapulae (mid-zone) | Left vs right |
| Below scapulae (lower zone) | Left vs right |
| Axillary lines | Left vs right |
| Anterior: 1st–4th ICS | Left vs right |
PERCUSSION — EXPANDED
Kronig's Isthmus (Apical Percussion)
Percuss from the midline of the neck along the top of the trapezius laterally. A band of resonance (~5–6 cm wide) bridges the clavicle and the neck = Kronig's isthmus. Narrowing or dullness indicates apical pathology: old TB, apical fibrosis, Pancoast tumour.
Liver Dullness & Traube's Space
Liver dullness:
Percuss down the right MCL — normally changes from resonant to dull at the 5th ICS on full expiration (can be at 4th in expiration, up to 6th ICS in inspiration). Upper border of liver:
- Raised → hepatomegaly, right lower lobe collapse, right phrenic nerve palsy, subphrenic abscess
- Low → emphysema (hyperinflation pushes diaphragm down)
Traube's space:
Left lower chest bounded by the left costal margin (inferiorly), left mid-axillary line (laterally), left heart border (medially), and splenic dullness (superiorly). Normally tympanitic (gastric air bubble).
- Dull → left pleural effusion (most common clinical use), splenomegaly, gastric outlet obstruction
Diaphragmatic Excursion — Technique in Detail
- Patient seated or standing; ask to breathe in fully and hold
- Percuss down posteriorly (paravertebral line) until dullness begins — mark this point
- Ask patient to breathe out fully and hold
- Percuss upward until resonance changes back to dullness — mark again
- Measure the distance between the two marks
- Repeat on the other side
Normal: 4–6 cm bilaterally; right slightly higher than left (liver effect).
Reduced (<2 cm): COPD (bilateral), phrenic nerve palsy (unilateral), subphrenic abscess, diaphragmatic splinting from pain (pleuritis), ascites.
Elevated hemidiaphragm:
- Right side: hepatomegaly, right lower lobe collapse, right phrenic nerve palsy, right-sided subphrenic abscess
- Left side: left phrenic nerve palsy (Pancoast, aortic aneurysm, mediastinal tumour), gastric distension
Percussion in Pleural Effusion — Key Signs
- Stony dullness (dullest note in medicine) over the effusion
- Upper border is concave (Ellis-Damoiseau line): dullness highest in the axilla, lower medially and laterally → creates a curved upper border
- Shifting dullness (>300–500 mL)
- Aegophony at the upper border of the effusion
- Traube's space obliterated for a left effusion
- Tracheal and mediastinal shift away (large effusion >1000 mL)
Skodaic resonance: Paradoxical increased resonance just above an effusion — compressed atelectatic lung above the fluid creates a more resonant note than expected.
AUSCULTATION — EXPANDED
Systematic Auscultation Map

Posterior (most important — maximises contact with lung bases):
Zones 1–2: above scapular spines (apices — TB, Pancoast)
Zones 3–4: between scapular spines (mid-zones)
Zones 5–6: below inferior angle of scapula (bases — pulmonary oedema, fibrosis, effusion)
Lateral axillary lines: bilateral middle lobes/lingula
Anterior:
Supraclavicular: apices
2nd ICS MCL: upper lobes
4th–5th ICS MCL: right middle lobe (right) / lingula (left)
Bases: pulmonary oedema, consolidation
Harrison's 22e: "Areas of alveolar filling have increased whispered pectoriloquy as well as transmission of larger-airway sounds (i.e., bronchial breath sounds in a lung zone where vesicular breath sounds are expected)."
Rhonchi vs Wheeze — Clarification
| Term | Definition | Cause |
|---|---|---|
| Wheeze (sibilant rhonchi) | High-pitched, musical, predominantly expiratory | Small airway obstruction — asthma, COPD |
| Rhonchi (sonorous) | Low-pitched, snoring/moaning, may clear with cough | Secretions in medium/large airways — bronchitis, bronchiectasis, COPD |
| Stridor | High-pitched inspiratory wheeze, heard without stethoscope | Upper airway/tracheal obstruction |
Harrison's 22e: "Wheezes can be polyphonic, involving multiple different size airways (e.g., asthma), or monophonic, involving one size airway (e.g., bronchogenic carcinoma)."
Harrison's 22e: "Rhonchi are a manifestation of obstruction of medium-sized airways, most often with secretions... Chronic rhonchi suggest bronchiectasis or COPD."
Crackles — Detailed Classification
| Feature | Fine crackles | Coarse crackles |
|---|---|---|
| Pitch | High-pitched | Low-pitched |
| Duration | Very brief, discontinuous | Longer, bubbling |
| Timing | End-inspiratory (late) | Early inspiratory or pan-inspiratory |
| Sound | Velcro tearing | Bubbling/gurgling through fluid |
| Clear with cough? | No | Partially |
| Mechanism | Opening of collapsed alveoli/small airways | Air through secretions in large airways |
| Causes | IPF (bibasal, fine, Velcro), early pulmonary oedema, pneumonia | Bronchiectasis, COPD with secretions, late pulmonary oedema |
| Distribution | Bibasal (pulm oedema, IPF), localised (pneumonia) | Bilateral or localised |
Harrison's 22e: "Crackles in pulmonary edema are generally more prominent at the bases. Interestingly, diseases that result in fibrosis of the interstitium (e.g., IPF) also result in crackles that sound like Velcro being ripped apart."
Harrison's 22e: "Although some clinicians make a distinction between 'wet' and 'dry' crackles, this distinction has not been shown to be a reliable way to differentiate among etiologies."
Vocal Resonance — Complete Assessment
Standard vocal resonance:
Patient says "ninety-nine" while you listen. Normal = low, muffled sound. Increased (louder, clearer) = consolidation. Decreased = effusion, pneumothorax.
Whispering pectoriloquy:
Patient whispers "1-2-3." Normally barely audible. If clearly audible = consolidation. One of the most sensitive signs of alveolar filling.
Aegophony (egophony):
Ask patient to say "EEEE." Normal = muffled "ee" sound. In consolidation or at upper border of effusion = nasal, bleating "AY" sound. Called the E-to-A change.
Harrison's 22e: "Egophony is the auscultation of the sound 'AH' instead of 'EEE' when a patient phonates 'EEE.' This change in note is due to abnormal sound transmission through consolidated parenchyma and is present in pneumonia but not in IPF."
DISEASE-SPECIFIC EXAMINATION FINDINGS — DETAILED
1. COPD / Emphysema
| Step | Finding |
|---|---|
| Inspection | Barrel chest; pursed-lip breathing; use of accessory muscles; tripod position (leaning forward on outstretched arms); prolonged expiratory phase; central cyanosis (severe); peripheral oedema (cor pulmonale) |
| Palpation | Reduced bilateral expansion; tracheal tug; cardiac apex may be impalpable; Hoover's sign positive; reduced TVF |
| Percussion | Bilateral hyperresonance; loss of cardiac dullness; loss of hepatic dullness (pushed down); reduced diaphragmatic excursion |
| Auscultation | Globally reduced breath sounds; prolonged expiration (>6 s forced expiratory time); expiratory wheeze; scattered rhonchi; heart sounds muffled by hyperinflated lungs |
Washington Manual: "On inspection, pursed lip breathing, barrel chest secondary to hyperinflation, use of accessory muscles of respiration, and central and peripheral cyanosis can be present... Auscultation in severe COPD may expose prolonged (i.e., >6 seconds) breath sounds on a maximal forced exhalation and decreased breath sounds."
2. Lobar Pneumonia (Consolidation)
| Step | Finding |
|---|---|
| Inspection | Rapid, shallow breathing; use of accessory muscles; tachycardia; high fever; pleuritic chest pain (splinting) |
| Palpation | Reduced expansion ipsilateral; trachea central (unless large); increased TVF ipsilateral |
| Percussion | Dull to percussion over affected lobe; normal elsewhere |
| Auscultation | Bronchial breath sounds; fine end-inspiratory crackles; increased VR; whispering pectoriloquy; aegophony; pleural rub (if pleurisy present) |
3. Pleural Effusion
| Step | Finding |
|---|---|
| Inspection | Reduced expansion on affected side; intercostal fullness (large effusion) |
| Palpation | Reduced expansion ipsilateral; trachea pushed away (large); stony dull/absent TVF |
| Percussion | Stony dull; Ellis-Damoiseau curved upper border; shifting dullness; Skodaic resonance above; Traube's obliterated (left) |
| Auscultation | Absent/reduced breath sounds; aegophony at upper border; reduced VR; pleural rub (if pleuritis before effusion fully forms) |
4. Pneumothorax
| Step | Finding |
|---|---|
| Inspection | Acute respiratory distress; tachycardia; reduced expansion ipsilateral; if tension → cyanosis, haemodynamic collapse |
| Palpation | Reduced expansion; trachea deviated away (tension); absent TVF ipsilateral |
| Percussion | Hyper-resonant (hollow drum-like sound) |
| Auscultation | Absent breath sounds; absent VR; no added sounds |
Tension pneumothorax (emergency): tracheal deviation + absent breath sounds + hypotension + raised JVP — do not wait for CXR.
5. Pulmonary Fibrosis (IPF/Fibrosing Alveolitis)
| Step | Finding |
|---|---|
| Inspection | Cyanosis; clubbing (Grade 3–4); cachexia; tachypnoea; finger clubbing prominent |
| Palpation | Reduced bilateral expansion; increased TVF (if fibrosis with volume loss) |
| Percussion | Dull to flat at bases bilaterally |
| Auscultation | Fine bibasal end-inspiratory "Velcro" crackles (classic); no wheeze; no VR change unless co-existent consolidation |
6. Bronchiectasis
| Step | Finding |
|---|---|
| Inspection | Clubbing (prominent); sputum pot nearby (large volumes of purulent sputum); cyanosis; weight loss |
| Palpation | Reduced expansion over affected areas; coarse TVF over areas of secretions |
| Percussion | May be dull (consolidation), normal, or hyperresonant |
| Auscultation | Coarse crackles (post-tussive — partially clearing with cough); rhonchi; wheeze |
7. Asthma (Acute)
| Step | Finding |
|---|---|
| Inspection | Tachypnoea; use of accessory muscles; intercostal recession; unable to complete sentences (severe); tachycardia; pulsus paradoxus (>25 mmHg = life-threatening) |
| Palpation | Reduced bilateral expansion; pulsus paradoxus on radial pulse (disappears on inspiration) |
| Percussion | Bilateral hyperresonance (hyperinflation during acute attack) |
| Auscultation | Polyphonic expiratory wheeze (bilateral, diffuse); prolonged expiration; silent chest = life-threatening (no wheeze = no airflow) |
8. Lung Carcinoma — Examination Findings
Primary tumour effects:
- Monophonic fixed wheeze or stridor (proximal airway involvement)
- Signs of lobar collapse (atelectasis distal to obstruction)
- Signs of consolidation (post-obstructive pneumonia)
Pleural/chest wall spread:
- Pleural effusion signs
- Pleuritic chest pain; pleural rub
Lymph node spread:
- Cervical/supraclavicular lymphadenopathy (Virchow's node — left)
- Superior vena cava obstruction: non-pulsatile JVP, facial plethora, cyanosis, distended chest veins, Pemberton's sign
Extrathoracic effects:
- Horner syndrome (Pancoast — stellate ganglion invasion)
- Wasting of small hand muscles (Pancoast — T1 root compression)
- Clubbing + hypertrophic pulmonary osteoarthropathy
- Signs of metastasis: hepatomegaly, bony tenderness, neurological signs (brain mets)
COMPLETE INTEGRATION TABLE — ALL FINDINGS
| Sign | Consolidation | Effusion | Pneumothorax | COPD | Fibrosis | Bronchiectasis | Asthma |
|---|---|---|---|---|---|---|---|
| Clubbing | − | − | − | − | ++ | ++ | − |
| Trachea | Central | Pushed away (large) | Away (tension) | Central | Toward | Variable | Central |
| Chest shape | Normal | Fullness | Normal | Barrel | Normal/reduced | Normal | Normal |
| Expansion | ↓ ipsilateral | ↓ ipsilateral | ↓ ipsilateral | ↓ bilateral | ↓ bilateral | Variable | ↓ bilateral |
| TVF | Increased | Absent | Absent | Decreased | Increased | Variable | Decreased |
| Percussion | Dull | Stony dull | Hyper-resonant | Hyper-resonant | Dull | Variable | Hyper-resonant |
| Breath sounds | Bronchial | Absent | Absent | ↓ vesicular | ↓ vesicular | Coarse crackles | Wheeze |
| Crackles | Fine (late insp) | None | None | Coarse | Fine bibasal | Coarse (post-tussive) | None |
| Wheeze | None | None | None | Expiratory | None | Sometimes | Polyphonic exp |
| VR/aegophony | ↑ / + | ↓ / + (upper border) | Absent | ↓ | Variable | Normal | ↓ |
| Pleural rub | ± (pleuritis) | ± (early) | − | − | − | − | − |
ADDITIONAL CLINICAL TESTS DURING EXAMINATION
Forced Expiratory Time (FET)
Ask patient to take a deep breath and exhale as forcefully as possible. Auscultate over the trachea and time the expiratory wheeze/sound:
- Normal: <3 seconds
-
6 seconds = significant airflow obstruction (COPD, severe asthma)
- Washington Manual: "Auscultation in severe COPD may expose prolonged (i.e., >6 seconds) breath sounds on a maximal forced exhalation."
Peak Expiratory Flow Rate (PEFR)
Bedside assessment of airway obstruction (asthma monitoring). Normal: predicted by height, age, sex. <33% predicted = life-threatening asthma.
Pulsus Paradoxus (Measured)
Apply sphygmomanometer. Inflate above systolic. Deflate slowly — note when Korotkoff sounds first appear (expiration only). Continue deflating — note when sounds heard throughout cycle. Difference >10 mmHg = pulsus paradoxus.
Harrison's 22e: "Pulsus paradoxus is an ominous sign in a patient with obstructive lung disease, as it is associated with significant negative intrathoracic (pleural) pressures required for ventilation and impending respiratory failure."
Pemberton's Sign
Ask patient to raise both arms above their head for 1 minute. Positive if: facial plethora, cyanosis, and JVP elevation appear. Indicates superior vena cava obstruction from mediastinal mass (most commonly retrosternal goitre or lung tumour).
Six-Minute Walk Test (6MWT)
Functional assessment — measures oxygen desaturation on exertion; used in IPF, pulmonary hypertension, COPD. Desaturation >4% SpO₂ on walking = significant.
NORMAL ANATOMY OF LUNG LOBES — SURFACE MARKINGS
Knowing these allows precise localisation of signs:
Right lung (3 lobes):
- Upper lobe: above horizontal fissure (4th rib anteriorly, 4th ICS)
- Middle lobe: between horizontal and oblique fissures (4th–6th rib anteriorly; right axilla)
- Lower lobe: below oblique fissure (6th rib MCL to T10 posteriorly); dominates the posterior chest
Left lung (2 lobes + lingula):
- Upper lobe (+ lingula): above oblique fissure; dominates anterior chest
- Lower lobe: below oblique fissure; dominates posterior chest
- Lingula: equivalent of right middle lobe; 3rd–5th ribs anteriorly, left MCL
Clinical implication:
- Posteriorly, nearly all audible sounds below the scapulae = lower lobes
- Anteriorly above nipple = upper lobes (right) and upper + lingular (left)
- Right middle lobe and lingula best heard in the right and left axillae respectively
EXAMINATION OF SPECIAL SITUATIONS
Patient in Respiratory Distress (ABCDE Approach)
- Do not fully undress before calling for help
- Assess SpO₂ immediately (normal ≥94%, target 94–98%)
- Look for: stridor → upper airway; silent chest + wheeze history → severe asthma; absent unilateral breath sounds + haemodynamic instability → tension pneumothorax
Intensive Care / Ventilated Patient
- Chest inspection for asymmetric rise (mainstem intubation)
- Auscultate bilaterally immediately after intubation
- Percuss for pneumothorax (hyper-resonance) if acute deterioration
Paediatric Patient
- Respiratory rate faster (neonates 40–60/min; 2 years 25–35; 10 years 20–25)
- Subcostal recession more prominent (pliable chest wall)
- Grunting = alveolar atelectasis (intrinsic PEEP)
- Stridor more common (laryngomalacia, croup, epiglottitis)
FINAL SYSTEMATIC CHECKLIST
RESPIRATORY EXAMINATION — STRUCTURED SEQUENCE
1. PREPARATION
□ Wash hands, introduce, consent, chaperone if needed
□ Expose patient to waist; seated at 45° or upright
□ Adequate lighting
2. END-OF-BED INSPECTION
□ General appearance, distress, cachexy
□ Respiratory rate, pattern, depth
□ Accessory muscle use
□ Pursed-lip breathing, paradoxical breathing
□ Oxygen, nebulisers, inhalers, sputum pots
3. HANDS & ARMS
□ Clubbing (grade + Schamroth test)
□ Peripheral cyanosis
□ CO₂ flap (asterixis) — wrists extended 30 sec
□ Fine tremor
□ Tar staining
□ Radial pulse (rate, rhythm, character)
□ Bounding pulse (CO₂ retention)
□ Pulsus paradoxus (if indicated — >10 mmHg)
□ BP
4. FACE & NECK
□ Central cyanosis (lips, tongue)
□ Plethora vs pallor (conjunctivae)
□ Horner syndrome (ptosis, miosis, enophthalmos)
□ JVP (height, waveform)
□ Pemberton's sign (if mediastinal mass suspected)
□ Cervical/supraclavicular lymphadenopathy
5. TRACHEA
□ Visual midline assessment
□ Palpate tracheal position (suprasternal notch)
□ Tracheal tug (Oliver's sign if vascular cause)
6. CHEST INSPECTION
□ Shape: barrel, pectus, kyphoscoliosis, Harrison's sulci
□ Symmetry of chest wall
□ Scars (thoracotomy, VATS, chest drains, radiotherapy marks)
□ Dilated chest wall veins (direction of flow)
□ Chest wall movement — symmetry and degree
□ Intercostal recession
7. PALPATION
□ Upper zone expansion (anterior)
□ Lower zone expansion (posterior, most important)
□ Tactile vocal fremitus — all zones bilaterally
□ Subcutaneous emphysema
□ Apex beat position
□ Right ventricular heave (parasternal)
□ Pleural rub (palpable)
□ Hoover's sign
8. PERCUSSION
□ Apices (Kronig's isthmus)
□ Anterior: 2nd ICS downward bilaterally
□ Left → right comparison
□ Cardiac dullness boundaries
□ Posterior: systematic from apices to bases
□ Lateral axillary lines
□ Liver dullness (right MCL, 5th ICS)
□ Traube's space (left)
□ Diaphragmatic excursion (4–6 cm normal)
□ Shifting dullness (if effusion suspected)
9. AUSCULTATION
□ Breath sound character (vesicular vs bronchial vs ↓)
□ Inspiration: expiration ratio
□ Forced expiratory time (normal <3 s)
□ Added sounds: crackles (timing, type, distribution)
□ Wheeze (polyphonic vs monophonic, timing)
□ Stridor
□ Pleural rub
□ Vocal resonance (ninety-nine)
□ Whispering pectoriloquy
□ Aegophony (E→A change)
□ Anterior → lateral → posterior comparison
10. COMPLETION
□ Ankle oedema (cor pulmonale)
□ Temperature chart, SpO₂, PEFR if available
□ Sputum: colour, consistency, volume, odour
□ CXR if available — comment systematically
□ Thank patient, help redress
□ Summarise findings
Sources: Fishman's Pulmonary Diseases and Disorders 5e (Grippi); Harrison's Principles of Internal Medicine 22e (Levy); Washington Manual of Medical Therapeutics; Murray & Nadel's Textbook of Respiratory Medicine 7e; Goldman-Cecil Medicine; Textbook of Family Medicine 9e
This is a shared conversation. Sign in to Orris to start your own chat.