Hi
Hi! How can I help you today?
Alcoholic cirrhosis morphology flow chart pathology pov
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Searching Images
alcoholic cirrhosis liver gross morphology micronodular
Reading File
Searching Images
alcoholic hepatitis Mallory bodies ballooning degeneration histology
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
Loading Image
I now have all the content needed. Here is a comprehensive pathology-focused morphology flow chart of alcoholic cirrhosis:
Alcoholic Cirrhosis — Morphology Flow Chart (Pathology POV)
Source: Robbins, Cotran & Kumar — Pathologic Basis of Disease; Sleisenger & Fordtran's GI and Liver Disease; Harrison's Principles of Internal Medicine
Master Flow Diagram
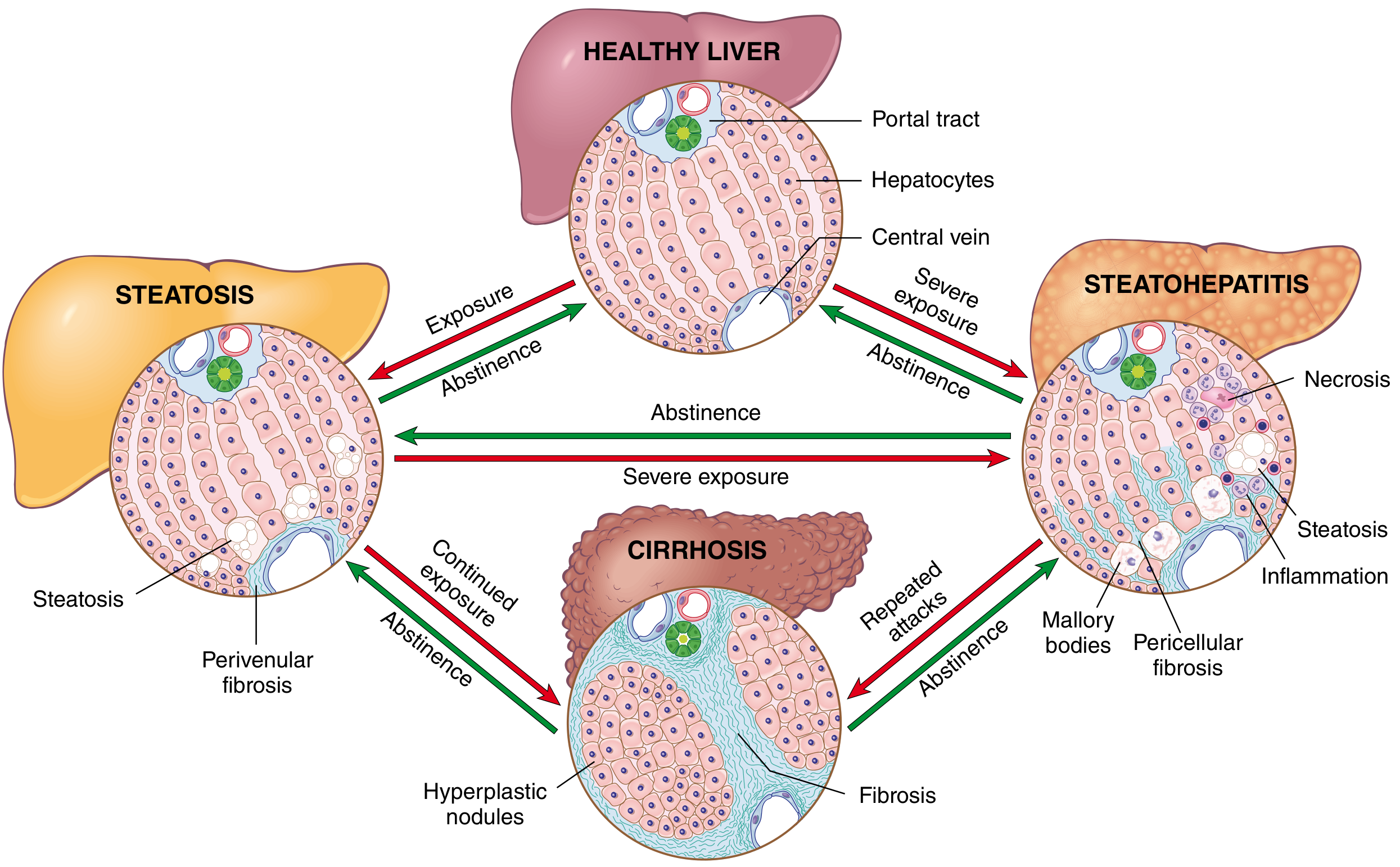
Robbins Fig. 18.18 — Shows the interrelationships among steatosis, steatohepatitis, and cirrhosis with key morphologic features at each stage.
Stage-by-Stage Morphology
① STEATOSIS (Fatty Liver) — Earliest / Reversible
| Feature | Detail |
|---|---|
| Gross | Enlarged liver (up to 4–6 kg), soft, yellow, greasy |
| Micro — onset | Small lipid droplets → coalesce into large macrovesicular droplets displacing the nucleus |
| Predominant form | Macrovesicular steatosis (large droplet) |
| Distribution | Starts at centrilobular zone 3 (perivenular), extends outward |
| Reversibility | Completely reversible with abstinence |
| Exception | Alcoholic foamy degeneration = diffuse small-droplet (microvesicular) steatosis — associated with ER and mitochondrial damage |
② ALCOHOLIC STEATOHEPATITIS (ASH) — Inflammatory Stage
| Feature | Detail |
|---|---|
| Ballooned hepatocytes | Swollen, cleared-out cytoplasm; cytoskeletal damage; essential for diagnosis |
| Mallory-Denk (Mallory Hyaline) bodies | Skeins of intermediate filaments (keratin 8 & 18) — partially degraded, ubiquitinated; eosinophilic intracytoplasmic inclusions; confirmed by IHC (p62, ubiquitin, CK8/18) |
| Inflammation | Predominantly neutrophilic infiltrate surrounding/satelliting necrotic hepatocytes |
| Steatosis | Less prominent than pure steatosis; mixed micro/macrovesicular |
| Early fibrosis | Perisinusoidal/pericellular ("chicken-wire") fibrosis starting in zone 3 |
| Megamitochondria | Large, rounded cytoplasmic organelles (stain red on CAB; differ from Mallory bodies which stain blue) |
| Cholestasis | Canalicular bile plugging in severe cases |
| Sclerosing hyaline necrosis | Partial/complete obliteration of terminal hepatic venules |
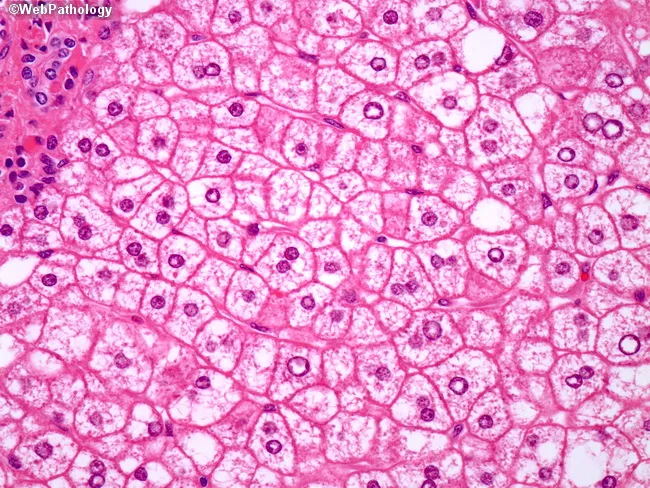
H&E showing ballooned hepatocytes with Mallory-Denk bodies and macrovesicular steatosis in alcoholic steatohepatitis
③ FIBROSIS — Bridging / Progressive
| Feature | Detail |
|---|---|
| Pattern | Zone 3 pericellular → portal/periportal → bridging fibrosis |
| Stain | Masson trichrome — blue collagen; "chicken-wire" perisinusoidal pattern |
| Perivenular fibrosis | Fibrous obliteration of central veins (phlebosclerosis, veno-occlusive lesions) |
| Progression | Continued alcohol exposure → bridging fibrosis → cirrhosis |
| Partial reversibility | Early fibrosis can regress with abstinence; once cirrhosis develops, regression is rare |
④ CIRRHOSIS ("Laennec Cirrhosis") — End-Stage / Irreversible
Gross Pathology
| Feature | Detail |
|---|---|
| Size | Initially enlarged → shrinks as disease progresses (hard, nodular) |
| Surface | Diffuse fine micronodularity < 3 mm — cobblestoned texture |
| Color | Mottled reddish-brown; greenish tint if cholestasis present |
| Consistency | Firm; distorted, loss of normal lobular architecture |
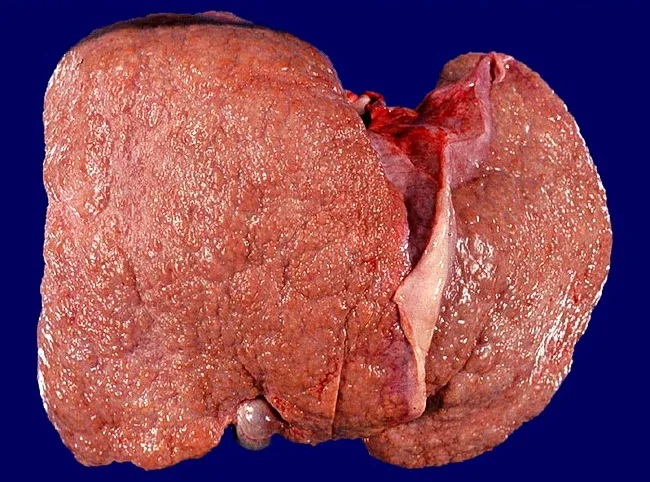
Gross pathology: Micronodular alcoholic cirrhosis — diffuse nodules <3 mm, firm liver with cobblestoned surface
Histology
| Feature | Detail |
|---|---|
| Nodule type | Micronodular (< 3 mm) = "Laennec cirrhosis"; mixed micro + macronodular with abstinence |
| Fibrous septa | Thick, collagen-rich bands completely surrounding each nodule (blue on trichrome) |
| Steatosis in cirrhosis | Often absent in "burned-out" cirrhosis (fat disappears late) |
| Mallory hyaline | Present when active steatohepatitis coexists; nearly universal in active disease |
| Regenerative nodules | Hyperplastic nodules replacing normal lobular architecture |
| Vascular distortion | Sinusoidal capillarization; loss of normal portal/hepatic venous landmarks |
Summary Flow Chart (Text)
Chronic Alcohol Exposure
↓
① STEATOSIS (Zone 3 macrovesicular fat)
↓ continued exposure ↑ abstinence → REVERSIBLE
② STEATOHEPATITIS
• Ballooned hepatocytes
• Mallory-Denk bodies (K8/K18)
• Neutrophilic satellitosis
• Pericellular "chicken-wire" fibrosis (zone 3)
• Sclerosing hyaline necrosis
↓ repeated attacks ↑ abstinence → partial reversal
③ BRIDGING FIBROSIS
• Portal-to-portal and portal-to-central bridges
• Trichrome: blue collagen bridges
↓ continued exposure
④ CIRRHOSIS ("Laennec")
• MICRONODULAR < 3 mm (active drinking)
• Gross: firm, green-brown, cobblestoned liver
• Micro: nodules in dense fibrous septa
• "Burned-out" = no steatosis, no Mallory bodies
• Abstinence → gradual → MACRONODULAR / MIXED
(indistinguishable from other etiologies)
Key Distinguishing Points (vs NASH/Other Cirrhoses)
| Feature | Alcoholic | MASH (NAFLD) |
|---|---|---|
| Steatosis | Less (especially in hepatitis stage) | More prominent |
| Ballooning | More severe | Present but less |
| Mallory-Denk bodies | More common, prominent | Present, less prominent |
| Neutrophilic infiltrate | Predominant | Mixed, less neutrophils |
| Cholestasis | More common | Less common |
| Obliterated central veins | Common | Less common |
| Nodule type | Micronodular → mixed | Macronodular |
| AST:ALT ratio | > 2 (due to pyridoxal-5-phosphate deficiency) | < 1 |
Trichrome Stain Pattern Summary
| Stage | Trichrome Finding |
|---|---|
| Steatosis | No/minimal fibrosis |
| Steatohepatitis | Perisinusoidal "chicken-wire" blue fibrosis, zone 3 |
| Bridging fibrosis | Blue bridges portal-to-portal, portal-to-central |
| Cirrhosis | Thick blue septa completely encircling nodules |
Sources: Robbins, Cotran & Kumar Pathologic Basis of Disease, p. 783–785; Sleisenger & Fordtran's GI and Liver Disease; Harrison's Principles of Internal Medicine 22E
This is a shared conversation. Sign in to Orris to start your own chat.