Vasculotoxic snake bite treatment
Reading File
search_medical_text
vasculotoxic snake bite treatment management antivenom
search_medical_text
snake bite coagulopathy DIC bleeding management
search_medical_image
vasculotoxic snake bite clinical features local tissue necrosis
GradeResponse
GradeResponse
GradeResponse
search_medical_text
hemotoxic viper snakebite venom coagulopathy fibrinogen depletion treatment
search_medical_text
snake bite antivenom dose administration local wound care necrosis
Vasculotoxic Snakebite: Treatment
Overview
Vasculotoxic (hemotoxic) snakes include vipers (Russell's viper, saw-scaled viper, green pit viper), some rattlesnakes, and Bothrops species. Their venom contains metalloproteinases, phospholipases A2, serine proteases, and hyaluronidase, causing:
- Local tissue destruction, edema, and necrosis
- Venom-induced consumption coagulopathy (VICC) / DIC
- Thrombocytopenia
- Hemolysis and hemoglobinuria
- Acute kidney injury (AKI)
Clinical Features
| System | Manifestations |
|---|---|
| Local | Fang marks, pain, swelling, bruising, blistering, necrosis |
| Hematologic | Spontaneous bleeding (gums, IV sites), hemoptysis, hematuria |
| Renal | Oliguria, dark urine, AKI (from hemolysis + direct toxicity) |
| Cardiovascular | Hypotension, shock (venom vasodilation + fluid loss) |
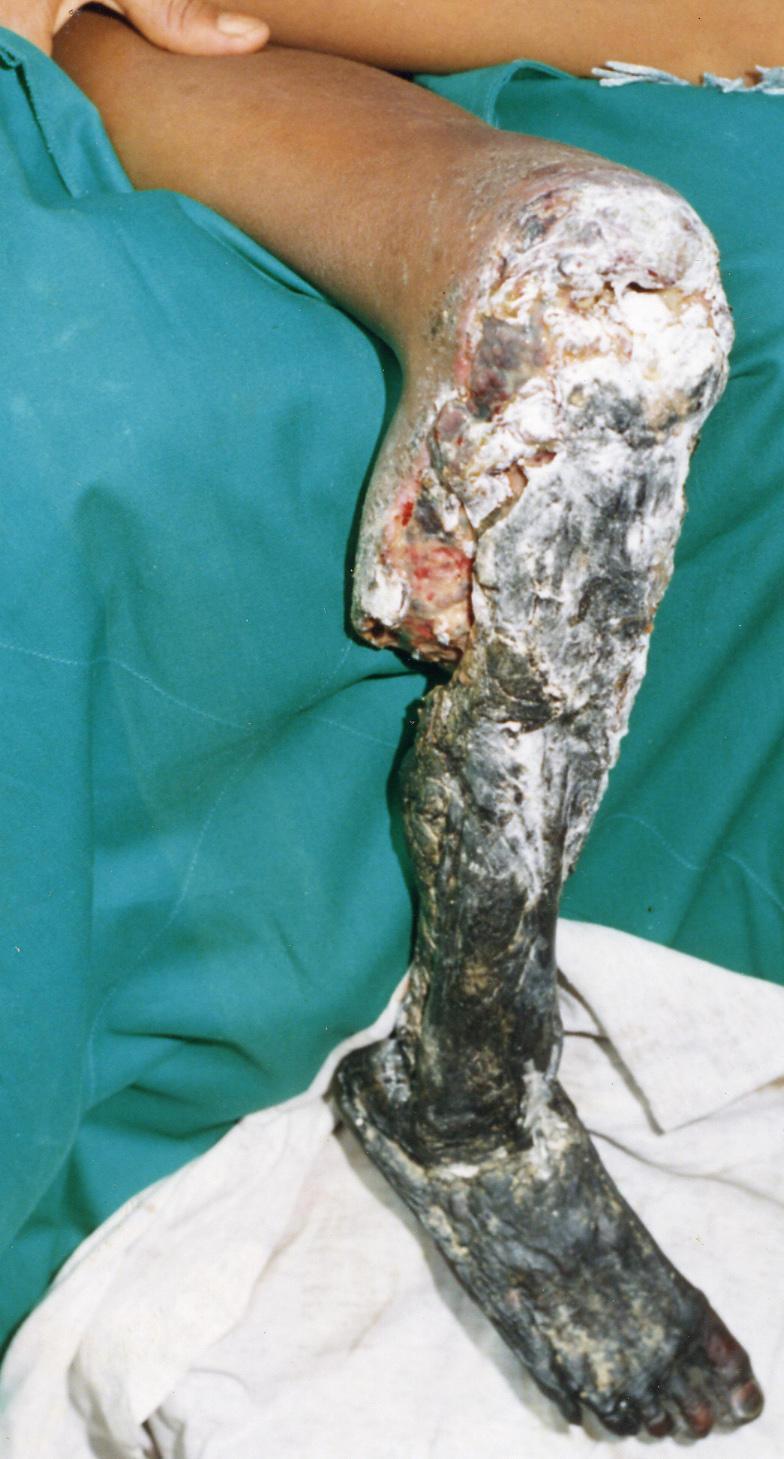
First Aid (Pre-hospital)
- Immobilize the bitten limb below heart level (reduces venom spread)
- Remove rings, watches, tight clothing
- Do NOT: cut/suck the wound, apply tourniquet, apply ice, give aspirin/NSAIDs
- Transport urgently to a hospital with antivenom
Hospital Management
1. Antivenom (Cornerstone of Treatment)
According to Harrison's Principles of Internal Medicine (p. 13049), antivenom is the mainstay of treatment for significant envenomation. The goal is to allow antibodies (or antibody fragments) to bind and neutralize circulating venom components before they attach to target tissues.
| Consideration | Details |
|---|---|
| Selection | Species-specific (monospecific) or polyspecific (regional coverage) |
| Timing | Give as soon as significant envenomation is confirmed — delays worsen coagulopathy and necrosis |
| Route | IV infusion (never IM for systemic envenomation) |
| Dose | Repeat doses if coagulopathy/bleeding fails to resolve within 6 hours |
| Cross-protection | Antivenoms rarely cross-protect between species unless venoms are homologous |
Indications for antivenom:
- Coagulopathy (elevated PT/aPTT, low fibrinogen, thrombocytopenia)
- Active hemorrhage
- Progressive local swelling beyond the bitten limb
- Hemodynamic instability
- Hemolysis or hemoglobinuria
Premedication: Subcutaneous epinephrine (0.25 mg) before antivenom infusion reduces anaphylaxis risk (controversial but practiced widely in South/Southeast Asia).
2. Coagulopathy Management
- Baseline labs: PT, aPTT, fibrinogen, platelet count, D-dimer, CBC, blood group
- Antivenom is the definitive treatment for VICC — not FFP alone
- Fresh Frozen Plasma (FFP) or cryoprecipitate: indicated for active bleeding with coagulopathy; do NOT give prophylactically without antivenom (replenished clotting factors are quickly consumed)
- Platelet transfusion: if platelets <20,000 with active bleeding
- Avoid: heparin (worsens bleeding), aspirin, NSAIDs
3. Fluid Resuscitation
- IV crystalloids (0.9% NaCl or Ringer's lactate) for hypotension/shock
- Urine output monitoring (target ≥0.5 mL/kg/hr) to prevent oliguric AKI
4. Renal Protection
- Aggressive hydration to prevent myoglobin/hemoglobin cast nephropathy
- Urinary alkalinization (sodium bicarbonate) if hemoglobinuria is present
- Dialysis (hemodialysis) if AKI with oliguria/hyperkalemia/uremia occurs
5. Local Wound Care
- Elevate the limb
- Monitor for compartment syndrome (tense compartments, pain on passive stretch) — requires fasciotomy (though debated; antivenom is preferred first)
- Debridement of necrotic tissue after stabilization
- Tetanus prophylaxis
- Antibiotics: only if secondary infection is confirmed (prophylactic antibiotics are not routinely recommended)
- Surgical amputation may be required in cases of extensive necrosis/gangrene (as illustrated above)
6. Monitoring
| Parameter | Frequency |
|---|---|
| Coagulation profile (PT, fibrinogen) | Every 6 hours until normalizing |
| Urine output | Hourly |
| Platelet count | Every 6–12 hours |
| Local wound circumference | Every 2–4 hours |
| Vital signs | Continuous initially |
Special Situations
| Situation | Approach |
|---|---|
| Anaphylaxis to antivenom | Stop infusion; give epinephrine 0.5 mg IM, antihistamines, steroids; restart at slower rate |
| Pregnancy | Antivenom is not contraindicated; fetal monitoring mandatory |
| Pediatric | Same antivenom dose as adults (dose is based on venom amount, not body weight) |
| Delayed presentation (>24h) | Antivenom still indicated if coagulopathy persists |
Common Vasculotoxic Snakes by Region
| Region | Snake |
|---|---|
| South Asia | Russell's viper (Daboia russelii), Saw-scaled viper (Echis carinatus) |
| Southeast Asia | Green pit viper, Malayan pit viper |
| Americas | Rattlesnakes (Crotalus spp.), Fer-de-lance (Bothrops asper) |
| Africa | Puff adder (Bitis arietans), Gaboon viper |
Key principle: Antivenom neutralizes the venom source — all other treatments are supportive. Early administration prevents coagulopathy progression, AKI, and local tissue loss. (Harrison's Principles of Internal Medicine, 21st Ed., p. 13049)
Anti snake venom dosing and duration
Reading File
search_medical_text
anti snake venom dosing number of vials initial dose repeat dose
search_medical_text
antivenom administration duration endpoint treatment snakebite coagulopathy resolution
GradeResponse
GradeResponse
Anti-Snake Venom (ASV): Dosing & Duration
General Principles
- Dose is based on venom load, not patient body weight — children receive the same dose as adults
- The goal is to neutralize all circulating venom; undertreating is more dangerous than overtreating
- Antivenom should be species-specific (monospecific) or regionally appropriate (polyspecific)
- The treating physician at bedside must be present during infusion for early detection of anaphylaxis
(Harrison's Principles of Internal Medicine, 21st Ed., p. 13049)
Indian Polyvalent ASV (Most Widely Used in South Asia)
Covers the "Big Four": Russell's viper, Saw-scaled viper, Common cobra, Common krait.
Initial Dose
| Envenomation Severity | IV Dose (Vials) | Route | Infusion |
|---|---|---|---|
| Mild (local swelling only, no systemic features) | 8–10 vials | IV | Dilute in 100–200 mL NS; infuse over 30–60 min |
| Moderate (coagulopathy, mild bleeding) | 10–15 vials | IV | Dilute in 250–500 mL NS; infuse over 1 hour |
| Severe (active hemorrhage, shock, neuro features) | 15–20 vials | IV | Start slow (1 mL/min × 10 min), then faster under observation |
WHO recommendation: Initial dose of 10 vials IV for systemic envenomation; reassess at 6 hours.
Repeat Dosing Criteria
Repeat ASV if any of the following persist or recur at 6 hours:
- Coagulopathy not correcting (20-minute Whole Blood Clotting Test [20WBCT] still non-clotting)
- Ongoing active bleeding
- Progressive local swelling
- Worsening neurological signs
- Persistent hypotension/shock
Repeat dose: 8–10 vials IV, re-evaluate every 6 hours.
20-Minute Whole Blood Clotting Test (20WBCT)
A simple bedside test to guide ASV dosing for vasculotoxic bites:
- Place 2 mL of fresh venous blood in a clean, dry glass tube
- Leave undisturbed at room temperature for 20 minutes
- Tilt the tube:
- Clot formed → coagulopathy resolved, no further ASV needed
- No clot (non-clotting blood) → active VICC, repeat ASV dose
Repeat 20WBCT every 6 hours after each antivenom dose.
Crotalidae Polyvalent Immune Fab — CroFab (North American Pit Vipers)
(Harrison's, p. 13051)
| Phase | Dose | Details |
|---|---|---|
| Initial | 4–6 vials IV | Dilute in 250 mL NS; infuse over 1 hour |
| If progression | Repeat 4–6 vials | Until initial control achieved |
| Maintenance | 2 vials every 6 hours × 3 doses | To prevent recurrence of coagulopathy |
North American Coral Snake Antivenom
(Harrison's, p. 13051)
- Dilute 3–5 reconstituted vials in 250–500 mL normal saline
- Infuse IV over 1 hour (provider must remain at bedside)
- If signs of envenomation progress despite initial dosing: repeat starting dose
- Up to 10 vials total may be required
Duration of ASV Treatment
| Situation | Duration |
|---|---|
| Single dose, resolving coagulopathy | Stop after 20WBCT normalizes (usually within 6–24 h) |
| Persistent coagulopathy | Continue 6-hourly reassessment; repeat ASV until 20WBCT clots |
| Maximum recommended (Indian polyvalent) | Up to 100 vials reported in severe Russell's viper bites, though 20–30 vials covers most cases |
| Neurological envenomation (krait/cobra) | May need antivenom for longer; neostigmine adjunct for post-synaptic blockade |
| Late recurrence of coagulopathy (CroFab) | Can occur 2–3 days after initial treatment; maintenance dosing protocol addresses this |
Administration Protocol Summary
1. Pre-medicate: Adrenaline 0.25 mg SC (optional but widely practiced)
2. Dilute ASV in NS (250–500 mL)
3. Start infusion slowly (1 mL/min × 10 min)
4. Observe for anaphylaxis: urticaria, hypotension, bronchospasm
5. If no reaction → increase to full infusion rate over 60 min
6. Reassess at 6 hours with 20WBCT + clinical exam
7. Repeat dose if criteria met (see above)
8. Continue 6-hourly reassessment until stable
Anaphylaxis During Infusion
| Action | Details |
|---|---|
| Stop infusion immediately | — |
| Epinephrine | 0.5 mg IM (anterolateral thigh) |
| Antihistamine | Chlorphenamine 10 mg IV |
| Hydrocortisone | 200 mg IV |
| Restart | At slower rate once stabilized; do not abandon antivenom |
Key Points
- Never give ASV IM for systemic envenomation (absorption is unreliable)
- Pediatric dose = adult dose (same venom load regardless of body weight)
- FFP/cryoprecipitate should be given only after antivenom (otherwise clotting factors are rapidly consumed by residual venom)
- No upper limit is absolute — continue until clinical and laboratory endpoints are met
This is a shared conversation. Sign in to Orris to start your own chat.