Nephrotic syndrome
Reading File
search_medical_text
nephrotic syndrome etiology pathophysiology clinical features diagnosis
search_medical_text
nephrotic syndrome management treatment complications
search_medical_image
nephrotic syndrome histology biopsy glomerular pathology
GradeResponse
GradeResponse
GradeResponse
Nephrotic Syndrome
Definition
Nephrotic syndrome is defined by three cardinal features (Harrison's, p. 8392):
| Feature | Threshold |
|---|---|
| Proteinuria | > 3.5 g/day |
| Hypoalbuminemia | < 3.5 g/dL |
| Edema | Periorbital, peripheral, ascites |
Additional findings include hyperlipidemia (high LDL, low HDL), lipiduria, oval fat bodies, fatty casts, and Maltese cross-shaped cholesterol crystals under polarized light.
Pathophysiology
The primary defect is increased glomerular permeability to plasma proteins, particularly albumin. This leads to:
- Proteinuria → loss of oncotic pressure → hypoalbuminemia
- Reduced plasma oncotic pressure → fluid shifts to interstitium → edema
- Compensatory hepatic lipoprotein synthesis + reduced lipoprotein lipase activity → hyperlipidemia
- Loss of anticoagulant proteins (antithrombin III, proteins C and S) → hypercoagulable state
- Loss of immunoglobulins → increased infection susceptibility
Causes
Primary (Glomerular)
| Disease | Population | Key Features |
|---|---|---|
| Minimal Change Disease (MCD) | Children (#1), young adults | Abrupt onset, steroid-responsive, normal LM |
| Focal Segmental Glomerulosclerosis (FSGS) | Adults, African Americans | Focal/segmental scarring, higher resistance to therapy |
| Membranous Nephropathy | Adults (#1 cause in adults) | Spike-and-dome on EM, anti-PLA2R antibody |
| Membranoproliferative GN (MPGN) | Any age | Low complement, tram-track pattern |
| IgA Nephropathy | Young adults | Mesangial IgA deposits |
Secondary Causes
- Diabetes mellitus (most common secondary cause worldwide — diabetic nephropathy)
- Systemic lupus erythematosus (lupus nephritis class V)
- Amyloidosis (AA or AL)
- Infections: Hepatitis B/C, HIV, malaria, syphilis
- Drugs: NSAIDs, gold, penicillamine, heroin
- Malignancy: Hodgkin lymphoma (MCD), solid tumors (membranous)
- Preeclampsia
Clinical Features
- Edema: Periorbital (especially morning), dependent edema, anasarca in severe cases
- Frothy urine (heavy proteinuria)
- Ascites and pleural effusions
- Xanthelasma (chronic hyperlipidemia)
- Increased thrombosis risk: Deep vein thrombosis, renal vein thrombosis, pulmonary embolism
- Increased infection risk: Spontaneous bacterial peritonitis, cellulitis, pneumonia (encapsulated organisms)
Diagnosis
Initial Workup
- Urinalysis: Proteinuria, lipiduria, oval fat bodies, fatty casts
- Urine protein-to-creatinine ratio (spot) or 24-hour urine protein (> 3.5 g/day)
- Serum albumin (< 3.5 g/dL)
- Lipid panel: Elevated total cholesterol, LDL; low HDL
- BMP/CMP: Assess renal function
- CBC, coagulation studies
Secondary Cause Workup
- ANA, anti-dsDNA, complement (C3/C4) — for lupus
- Anti-PLA2R antibody — for membranous nephropathy
- Serum/urine protein electrophoresis — for amyloidosis/myeloma
- Hepatitis B/C serology, HIV
- Blood glucose, HbA1c — for diabetes
- Age-appropriate cancer screening
Kidney Biopsy
Indicated in adults with nephrotic syndrome (except presumed diabetic nephropathy). Generally deferred in children with initial presentation (empirically treated as MCD).
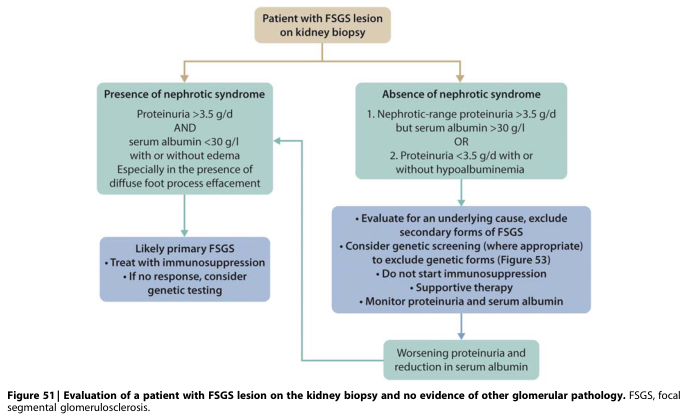
FSGS Evaluation (Management of Glomerular Diseases, p. 163)
When FSGS is found on biopsy, management depends on whether nephrotic syndrome is present:
- With nephrotic syndrome (proteinuria > 3.5 g/day + albumin < 30 g/L ± edema, especially with diffuse foot process effacement): Treat as primary FSGS with immunosuppression; consider genetic testing if non-responsive.
- Without nephrotic syndrome: Evaluate for secondary/genetic causes, provide supportive therapy, and monitor. Escalate to immunosuppression only if nephrotic syndrome develops.
Management
General Measures (Harrison's, p. 8592)
| Problem | Treatment |
|---|---|
| Edema | Loop diuretics (furosemide); avoid intravascular volume depletion |
| Hypercholesterolemia | Statins (all patients — increased CV risk) |
| Proteinuria | ACE inhibitors or ARBs (reduce proteinuria, slow progression) |
| Hypercoagulability | Anticoagulation if thromboembolism develops (some guidelines favor prophylactic anticoagulation if albumin < 2.5 g/dL) |
| Hypertension | ACE inhibitors/ARBs preferred |
| Infection risk | Pneumococcal vaccination; prompt antibiotic treatment |
Disease-Specific Treatment
| Cause | First-Line Treatment |
|---|---|
| MCD | Prednisone (high remission rate > 90%) |
| Primary FSGS | High-dose corticosteroids; calcineurin inhibitors (cyclosporine, tacrolimus) if steroid-resistant |
| Membranous Nephropathy | Spontaneous remission possible; rituximab (anti-CD20) now preferred; cyclophosphamide + steroids (Ponticelli protocol) |
| Lupus nephritis (class V) | Hydroxychloroquine; mycophenolate mofetil ± steroids |
| Diabetic nephropathy | Glycemic control, RAAS blockade, SGLT2 inhibitors (empagliflozin, dapagliflozin) |
Complications
| Complication | Mechanism |
|---|---|
| Thromboembolism | Loss of antithrombin III, proteins C/S; renal vein thrombosis is classic |
| Infections | Loss of IgG and opsonins; encapsulated organisms (Streptococcus pneumoniae) |
| AKI | Volume depletion, over-diuresis, renal vein thrombosis |
| CKD progression | Ongoing proteinuria is nephrotoxic |
| Hypothyroidism | Loss of thyroid-binding globulin (affects function tests) |
| Malnutrition | Protein loss, protein-energy wasting |
| Cardiovascular disease | Chronic hyperlipidemia accelerates atherosclerosis |
Prognosis
Prognosis depends heavily on the underlying cause:
- MCD: Excellent — most children and many adults achieve full remission with steroids; frequent relapsers exist
- Primary FSGS: Variable — up to 50% progress to ESRD within 10 years without treatment
- Membranous nephropathy: "Rule of thirds" — 1/3 spontaneous remission, 1/3 stable, 1/3 progressive
- Diabetic nephropathy: Progressive without aggressive management; SGLT2 inhibitors have improved outcomes
- Amyloidosis: Poor prognosis; depends on treatment of underlying disease
This is a shared conversation. Sign in to Orris to start your own chat.