immunologic raction as a cause of cell injury explain in short
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
I now have comprehensive content. Here is a concise, well-structured explanation:
Immunologic Reactions as a Cause of Cell Injury
Although the immune system's primary role is defense, immune reactions can themselves damage the body's own cells and tissues. This is one of the recognized causes of cell injury.
Mechanisms
1. Autoimmune Reactions
The immune system mounts a response against self-tissues. This leads to chronic inflammation and progressive tissue destruction. Examples include autoimmune hemolytic anemia, rheumatoid arthritis, and systemic lupus erythematosus (SLE).
2. Allergic (Hypersensitivity) Reactions
Exaggerated immune responses to environmental antigens (allergens, drugs, foreign proteins) cause tissue damage. These are classified into four types:
| Type | Mechanism | Example |
|---|---|---|
| Type I (Immediate) | IgE-mediated mast cell/basophil degranulation → release of histamine, leukotrienes | Anaphylaxis, allergic asthma |
| Type II (Cytotoxic) | IgG/IgM antibodies bind to cell-surface antigens → complement activation, opsonization, ADCC → cell lysis | Penicillin-induced hemolytic anemia, transfusion reactions |
| Type III (Immune complex) | Antigen-antibody complexes deposit in tissues → complement activation → neutrophil influx → tissue injury | Serum sickness, SLE vasculitis |
| Type IV (Delayed/Cell-mediated) | CD4⁺ T cells (Th1/Th17) and CD8⁺ cytotoxic T cells → cytokine release and direct cell killing | Tuberculin skin reaction, contact dermatitis, graft rejection |
3. Excessive or Chronic Immune Responses to Microbes
Even when directed at pathogens, a prolonged or exaggerated immune response can "overshoot" and destroy bystander healthy tissue. For example, chronic granulomatous inflammation in tuberculosis causes significant tissue damage.
Common Final Pathway
In all these situations, the immune response elicits inflammation, and it is the inflammatory reaction — via reactive oxygen species, proteolytic enzymes, complement proteins, and cytokines — that ultimately causes cell and tissue injury.
Key concept (Robbins): "Immune reactions can result in cell and tissue injury. Examples are autoimmune reactions against one's own tissues, allergic reactions against environmental substances, and excessive or chronic immune responses to microbes. In all these situations, the immune responses elicit inflammatory reactions, and inflammation is often the cause of damage to cells and tissues." — Robbins & Kumar Basic Pathology, Chapter 1
types of cell injury
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
I now have thorough content. Here is a complete, well-structured answer:
Types of Cell Injury
Cell injury is broadly divided into two main categories based on whether it is reversible or irreversible.
1. Reversible Cell Injury
The cell can recover completely if the injurious stimulus is removed before the "point of no return" is crossed.
Key Features:
- Cell swelling (water influx due to failure of Na⁺/K⁺ ATPase pump)
- Organelle swelling (mitochondria, ER)
- Plasma membrane blebbing
- Ribosome detachment from ER
- Clumping of nuclear chromatin
- Fatty change — lipid vacuoles in cytoplasm (especially liver)
- Also called hydropic change or vacuolar degeneration
Morphology:
- Cellular swelling → pallor, increased turgor and organ weight
- Increased eosinophilia of cytoplasm
- Myelin figures (phospholipid whorls from damaged membranes)
2. Irreversible Cell Injury → Cell Death
When injury is persistent or excessive, cells cross the point of no return and die. This occurs via two main pathways:
A. Necrosis
"Accidental" or uncontrolled cell death — always pathologic.
| Feature | Description |
|---|---|
| Cell size | Enlarged (swelling) |
| Nucleus | Pyknosis → karyorrhexis → karyolysis |
| Plasma membrane | Disrupted |
| Cell contents | Leak out (enzymatic digestion) |
| Inflammation | Always present |
| Cause | Ischemia, toxins, infection, trauma |
Types of Necrosis:
- Coagulative — most common; protein denaturation preserves cell outline (e.g., myocardial infarction)
- Liquefactive — enzymatic digestion liquefies tissue (e.g., brain infarct, abscess)
- Caseous — cheese-like, friable; seen in tuberculosis
- Fat necrosis — enzymatic (pancreatitis) or traumatic (breast)
- Fibrinoid — immune complex deposition in vessel walls
- Gangrenous — ischemic coagulative necrosis ± superimposed infection
B. Apoptosis
"Regulated" or programmed cell death — physiologic or pathologic.
| Feature | Description |
|---|---|
| Cell size | Reduced (shrinkage) |
| Nucleus | Fragmented into nucleosome-sized pieces |
| Plasma membrane | Intact (altered lipid orientation) |
| Cell contents | Packaged into apoptotic bodies |
| Inflammation | Absent (clean death) |
| Role | Eliminates damaged, unnecessary, or unwanted cells |
Physiologic examples: embryogenesis, lymphocyte selection, endometrial shedding
Pathologic examples: DNA/protein damage beyond repair, viral infections, ischemia
Pathologic examples: DNA/protein damage beyond repair, viral infections, ischemia
C. Other (Newer) Forms of Cell Death
| Type | Key Feature |
|---|---|
| Necroptosis | Programmed necrosis; triggered by TNF/receptor signals; inflammatory |
| Pyroptosis | Caspase-1/11-mediated; releases IL-1β; seen in infections |
| Ferroptosis | Iron-dependent lipid peroxidation; seen in ischemia-reperfusion |
Summary Diagram (Concept)
Cell Injury
│
├── MILD / SHORT → Reversible Injury → Cell Swelling, Fatty Change → RECOVERY
│
└── SEVERE / PROLONGED → Irreversible Injury → CELL DEATH
├── Necrosis (pathologic, inflammatory)
├── Apoptosis (regulated, non-inflammatory)
├── Necroptosis
├── Pyroptosis
└── Ferroptosis
"Within limits, the cell can repair the alterations seen in reversible injury and, if the injurious stimulus abates, may return to normalcy. Persistent or excessive injury, however, causes cells to pass the rather nebulous 'point of no return' into irreversible injury and cell death." — Robbins & Kumar Basic Pathology
Fatty change — lipid vacuoles in cytoplasm (especially liver) what does it mean
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
I have all the content needed. Here is a clear explanation:
Fatty Change (Steatosis) — Explained
What is it?
Fatty change (steatosis) is the abnormal accumulation of triglycerides (fat droplets) inside parenchymal cells, appearing as clear vacuoles in the cytoplasm under the microscope.
It is a feature of reversible cell injury — meaning if the cause is removed early enough, the cell can recover.
Why does it happen in the liver especially?
The liver is the principal organ of fat metabolism. It:
- Receives fatty acids from the blood and diet
- Processes, packages, and exports them as lipoproteins
When the liver cell is injured or metabolically stressed, this normal fat-processing machinery is disrupted, causing triglycerides to pile up inside hepatocytes instead of being exported.
Causes (TODAN mnemonic)
| Cause | Example |
|---|---|
| Toxins | Alcohol (most common), CCl₄, drugs |
| Obesity | Non-alcoholic fatty liver disease (NAFLD) |
| Diabetes mellitus | Type 2 diabetes with insulin resistance |
| Anoxia / ischemia | Reduced oxygen supply to liver |
| Nutritional deficiency | Protein malnutrition |
In high-income countries, the two most common causes are alcohol abuse and obesity-associated diabetes (NAFLD).
What does it look like microscopically?
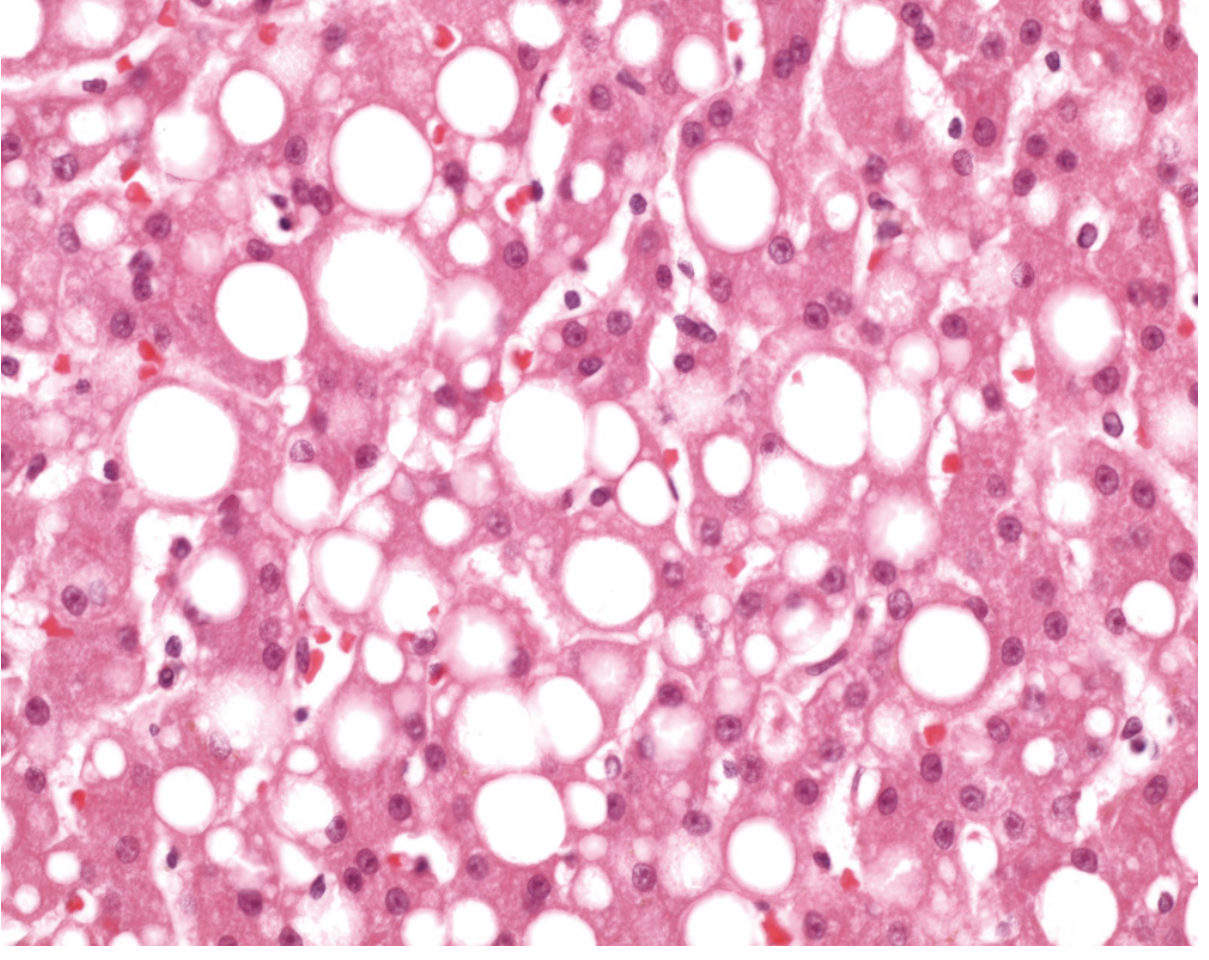
Two patterns:
| Pattern | Description | Example |
|---|---|---|
| Macrovesicular | One large fat droplet fills the cell, pushing the nucleus to the periphery | Alcohol, obesity, diabetes |
| Microvesicular | Many small fat droplets in cytoplasm; nucleus stays central; foamy appearance | Fatty liver of pregnancy, Reye syndrome, valproate toxicity |
What does it mean clinically?
- It is a marker of metabolic stress or toxic injury to the cell
- In the liver, it can be reversible if the cause (e.g., alcohol) is stopped early
- If the cause persists → steatohepatitis (inflammation + fat) → fibrosis → cirrhosis
- It can also occur in the heart (during severe anemia or diphtheria), kidney, and skeletal muscle
Simple analogy
Think of the liver cell as a factory that processes fat. Fatty change is like a factory breakdown — fat keeps coming in but cannot be packaged and shipped out, so it piles up inside the cell as visible droplets.
"Fatty change refers to an abnormal accumulation of triglycerides within parenchymal cells. It is most often seen in the liver, since this is the major organ involved in fat metabolism." — Robbins & Kumar Basic Pathology
consequences of cell injury
Finding Sources
Finding Sources
You've run out of free credits. Sign up for a free account to continue using Orris.
This is a shared conversation. Sign in to Orris to start your own chat.