Various dyes used in radiology
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Finding Sources
Loading Image
Searching Images
radiology contrast agents iodinated gadolinium barium classification
Loading Image
Loading Image
I now have all the information needed for a comprehensive answer. Here is the complete overview:
Contrast Agents (Dyes) Used in Radiology
Radiology uses several classes of contrast agents, each matched to a specific imaging modality. There are three types in common clinical use: iodinated agents (X-ray/CT/fluoroscopy), gadolinium-based agents (MRI), and ultrasound microbubble agents. Barium sulfate and CO₂ are additional special-purpose agents.
1. Iodinated Contrast Agents
Modality: Plain X-ray, CT, Fluoroscopy, Angiography
Iodine's high atomic number strongly attenuates X-rays, making iodinated compounds the standard contrast agent for CT and fluoroscopic studies.
Classification by Osmolality
| Type | Osmolality | Examples |
|---|---|---|
| High-osmolar (HOCM) | ~2000 mOsm/kg | Diatrizoate (Gastrografin), Iothalamate |
| Low-osmolar (LOCM) | 600–800 mOsm/kg | Iohexol (Omnipaque), Iopamidol, Iopromide |
| Iso-osmolar (IOCM) | ~290 mOsm/kg | Iodixanol (Visipaque) |
Classification by Ionicity
- Ionic (older): Dissociate in solution; more adverse reactions
- Non-ionic (modern): Do not dissociate; lower osmolality, fewer reactions; now preferred
Uses
- CT angiography (CTA), CT urogram, IV pyelogram
- Contrast-enhanced CT (thorax, abdomen, pelvis)
- Fluoroscopic angiography (intra-arterial administration)
- Gastrointestinal studies (water-soluble agents like Gastrografin)
Key Adverse Effects
- Nephrotoxicity (Post-Contrast AKI / contrast-induced nephropathy): Risk increases with eGFR <30 mL/min, age >60, diabetes, heart failure. IV hydration is the most protective measure; sodium bicarbonate and N-acetylcysteine show minimal benefit.
- Hypersensitivity reactions: Range from mild urticaria to anaphylaxis. Premedication with steroids ± diphenhydramine is used in at-risk patients.
- Thyrotoxicosis: In patients with hyperthyroidism exposed to iodinated contrast.
- Metformin: Should be held after contrast in patients with renal impairment.
— National Kidney Foundation Primer on Kidney Diseases, 8e
2. Gadolinium-Based Contrast Agents (GBCAs)
Modality: Magnetic Resonance Imaging (MRI)
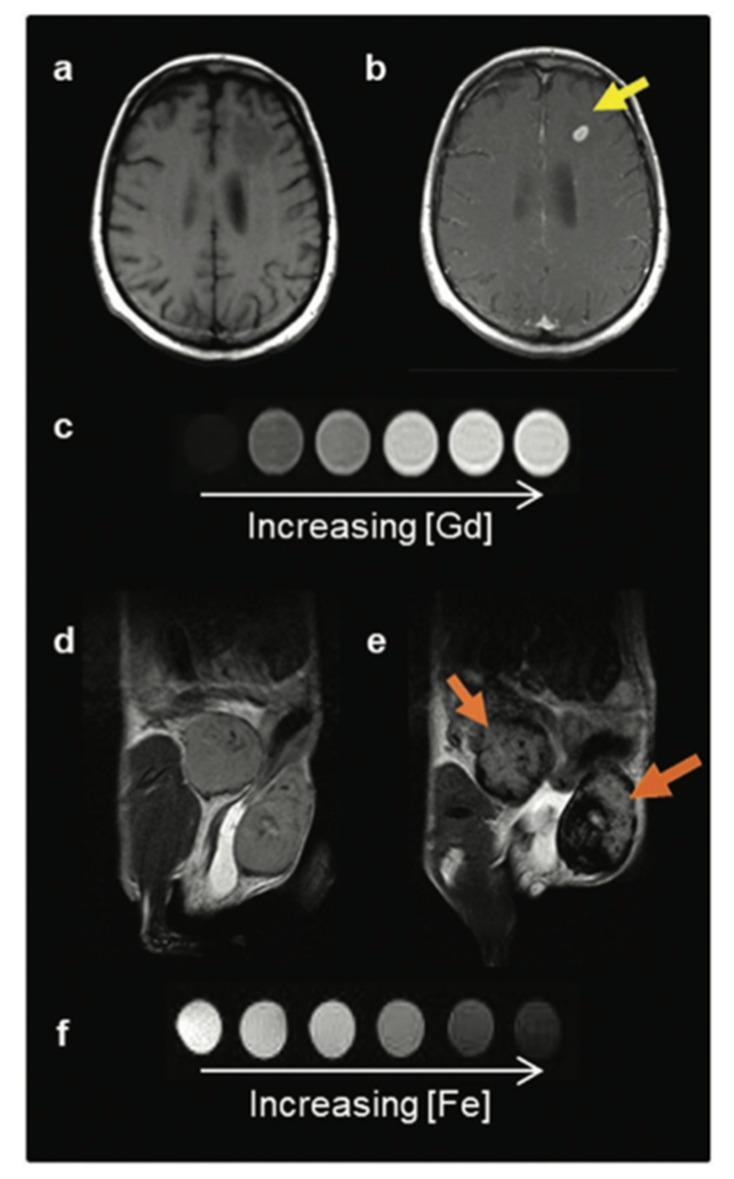
Gadolinium (a paramagnetic lanthanide element) shortens T1 relaxation time of nearby protons, producing bright (hyperintense) signal on T1-weighted sequences. Doses used in MRI are ~10× lower than iodinated contrast volumes.
Classification by NSF Risk (ACR Grouping)
| Group | NSF Risk | Agents |
|---|---|---|
| Group I | Highest — most NSF cases; no longer marketed in the US | Gadodiamide (Omniscan), Gadoversetamide (OptiMARK), Gadopentetate dimeglumine (Magnevist) |
| Group II | Lowest — few or no confirmed NSF cases; preferred in clinical use | Gadobutrol (Gadavist), Gadoteridol (ProHance), Gadobenate dimeglumine (MultiHance), Gadoterate meglumine (Dotarem) |
| Group III | Insufficient data; treated as Group I out of caution | Gadoxetate disodium (Eovist), Gadofosveset |
Structural Classification
- Linear agents: Less stable; release free Gd³⁺ more easily → higher NSF risk (Group I)
- Macrocyclic agents: Cage-like structure; more stable; lower NSF risk (Group II preferred)
Key Adverse Effects
- Nephrogenic Systemic Fibrosis (NSF): Rare but serious fibrosing disorder. Triggered when free gadolinium ions dissociate (in patients with eGFR <30 mL/min). Group I agents are contraindicated in severe renal impairment.
- Brain accumulation: Gadolinium can deposit in the dentate nuclei and globus pallidus after repeated doses; clinical significance under investigation.
- At standard doses, GBCAs are not nephrotoxic.
Special Use: Gadolinium as Alternative Angiography Agent
In patients with severe allergy to iodinated contrast, gadolinium-DTPA (0.5 mmol/mL) can be used for angiography at ≤0.3 mmol/kg. However, it should be avoided in CKD due to NSF risk.
— Grainger & Allison's Diagnostic Radiology; National Kidney Foundation Primer on Kidney Diseases, 8e
3. Barium Sulfate
Modality: Fluoroscopy / Plain X-ray (gastrointestinal studies)
Barium sulfate is an insoluble, inert heavy metal salt used exclusively for gastrointestinal tract opacification. It is not absorbed and passes through the GI tract unchanged.
| Study | Use |
|---|---|
| Barium swallow | Oropharynx, esophagus |
| Barium meal | Stomach, duodenum |
| Barium follow-through | Small intestine |
| Barium enema | Large intestine |
Contraindications: Suspected bowel perforation (barium leaking into the peritoneum causes severe chemical peritonitis). In these cases, water-soluble iodinated contrast (e.g., Gastrografin/diatrizoate) is used instead.
4. Carbon Dioxide (CO₂) Angiography
Modality: Digital Subtraction Angiography (DSA)
CO₂ was first used intra-arterially in the 1970s; became practical after DSA development in 1980. Unlike other agents, CO₂ displaces blood and creates negative contrast (darker than surrounding tissue). It is eliminated by the lungs in a single pass, so unlimited volumes can be used (with 2–3 minute intervals between injections).
Advantages:
- No nephrotoxicity
- No allergic reactions
- Inexpensive
Disadvantages:
- Cannot be used in the aortic arch or coronary arteries (risk of gas embolism)
- Requires special delivery system (to prevent air contamination)
- Special skills needed for interpretation
- Has never replaced iodinated contrast as the standard
— Grainger & Allison's Diagnostic Radiology
5. Ultrasound Contrast Agents (UCAs) / Microbubbles
Modality: Ultrasound
UCAs consist of a gas (sulfur hexafluoride, perflutren/perfluorocarbon, or air) enclosed within a shell of protein, lipid, or polymer. The ultrasound beam strongly reflects off the microbubbles, producing a bright signal. Enhancement patterns are similar to iodinated and gadolinium-based agents.
| Agent | Gas | Shell |
|---|---|---|
| SonoVue (Lumason) | Sulfur hexafluoride | Phospholipid |
| Definity | Perflutren | Lipid |
| Optison | Perflutren | Human albumin |
Key advantages:
- Not renally excreted — bubbles rupture and gas is exhaled; no nephrotoxicity
- No risk of NSF
- Minimal hypersensitivity reactions
- Useful when CT/MRI contrast is contraindicated
Limitations: Still constrained by standard ultrasound limitations (bowel gas, bone, obesity, metal implants).
— National Kidney Foundation Primer on Kidney Diseases, 8e
6. Iron Oxide Nanoparticles (Historical/Emerging)
Modality: MRI (T2/T2* agents)
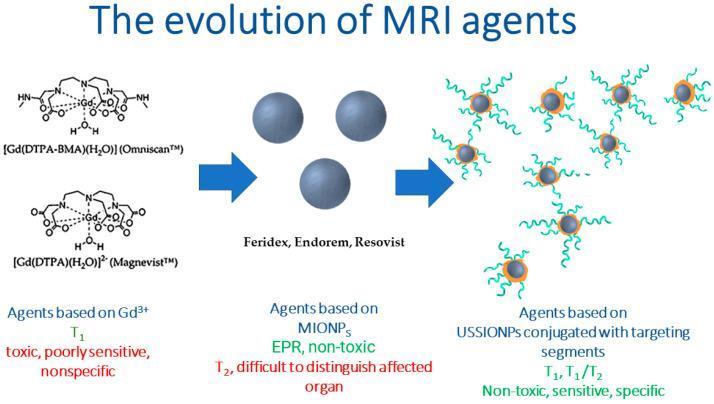
Iron oxide particles (SPIONs/USPIONs) create signal loss (hypointensity) on T2-weighted images, in contrast to gadolinium's signal enhancement on T1. Early products (Feridex, Endorem) were withdrawn from the market. Ultrasmall SPIONs (USPIONs) conjugated with targeting ligands are an active research area for tumor-specific MRI.
Summary Table
| Agent Class | Modality | Mechanism | Key Risk |
|---|---|---|---|
| Iodinated (LOCM/IOCM) | CT, fluoroscopy, angiography | X-ray attenuation | PC-AKI, hypersensitivity |
| Barium sulfate | GI fluoroscopy | X-ray attenuation | Peritonitis (if perforation) |
| Gadolinium (GBCA) | MRI | T1 shortening (positive contrast) | NSF (in renal failure), brain deposition |
| Iron oxide (SPION) | MRI | T2 shortening (negative contrast) | Largely withdrawn; research stage |
| CO₂ | DSA angiography | Negative contrast (displaces blood) | Gas embolism (arch/coronaries contraindicated) |
| Microbubbles | Ultrasound | Acoustic reflection | Minimal; not nephrotoxic |
This is a shared conversation. Sign in to Orris to start your own chat.