A 55 years old male with history of falling two years ago feel pain in left shoulder region now on again fall pain increase in shoulder region also feel stiffness of neck muscle say feel like stretching of left eye sometime and now headache head stiffness pain increase on lifting arm upward pain increase on shoulder region when he keep arm straight there is no previous history of any medical condition kindly suggest what will be diagnosis any medicine?
Reading File
Finding Sources
Finding Sources
Finding Sources
Searching PubMed
cervical spondylosis shoulder pain radiculopathy
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Loading Image
Reading File
I now have comprehensive information to provide a thorough clinical assessment. Let me compile the full answer.
Clinical Assessment
⚠️ Important Disclaimer: This is educational information only. The patient must be evaluated in person by a qualified physician — no diagnosis should be made or treatment started without proper clinical examination, neurological assessment, and imaging.
Most Likely Diagnosis: Cervical Spondylosis with Left C5 Radiculopathy (possibly compounded by a Rotator Cuff Pathology)
This 55-year-old male's symptom complex — left shoulder pain since a fall 2 years ago, worsening after a second fall, neck stiffness, pain radiating to the left eye/head region, pain aggravated by lifting the arm upward and keeping the arm straight — is a classic presentation of cervical spondylotic radiculopathy, most likely at the C4–C5 level compressing the C5 nerve root.
Understanding the Anatomy
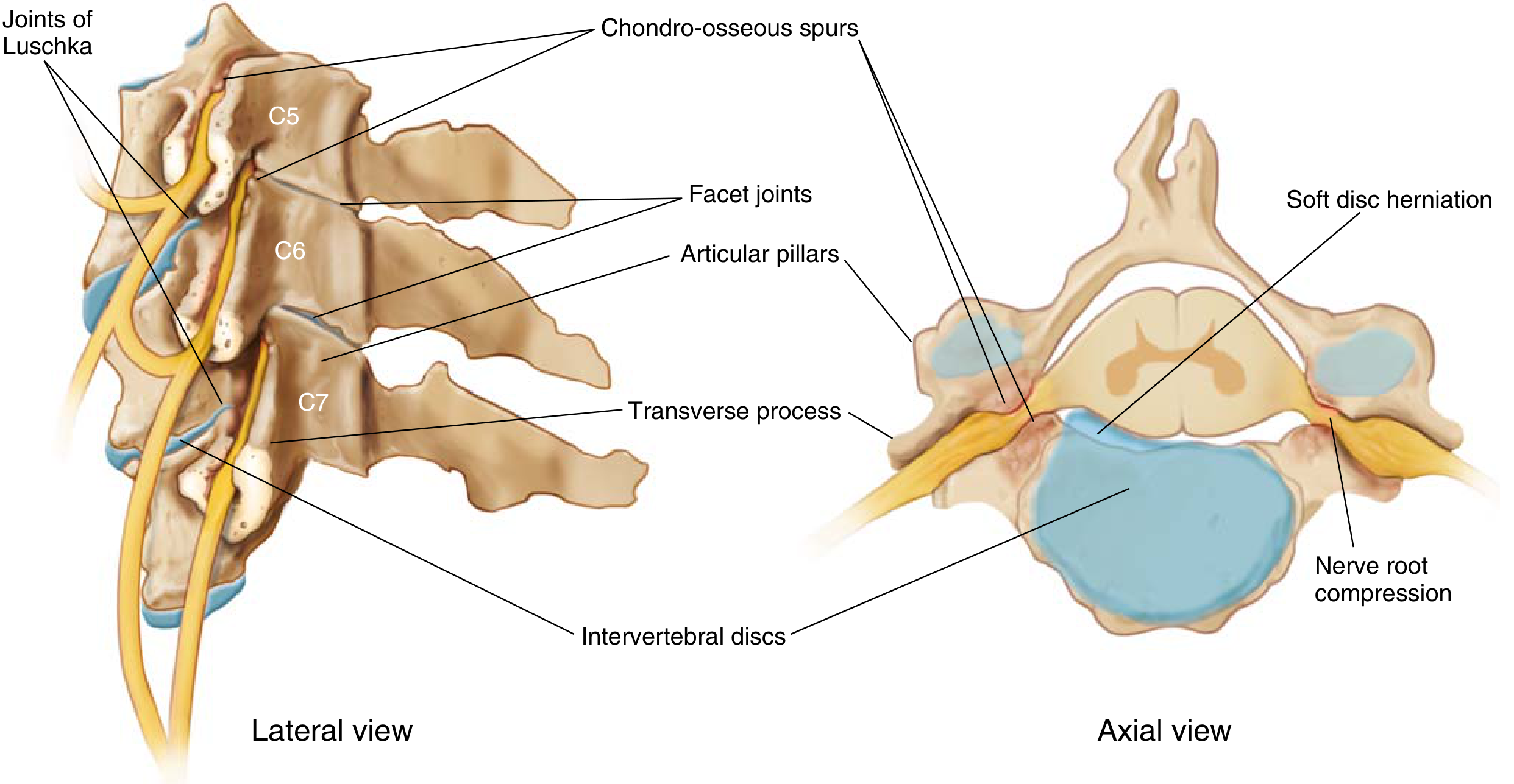
Cervical root compression — from Miller's Review of Orthopaedics
Symptom-by-Symptom Analysis
| Patient's Symptom | Clinical Explanation |
|---|---|
| Left shoulder pain (2 years) | C5 root compression: C4–C5 spondylosis causes pain, paresthesias, and sensory loss over the shoulder region |
| Pain worsens with arm raised upward | Abduction/elevation of the arm stretches the C5 root — classic radicular aggravation; also possible rotator cuff impingement |
| Pain worsens with arm held straight (extended) | Brachial stretch sign — stretching the compressed nerve root increases pain |
| Neck stiffness | Loss of cervical flexibility due to disc degeneration, osteophyte formation, and facet arthropathy |
| Headache + head stiffness | Cervical spondylosis causes occipital neuralgia and referred headache — extremely common |
| "Stretching" sensation in the left eye | Referred pain from upper cervical (C2–C3) involvement or occipital nerve irritation radiating to the periorbital/eye region |
| History of falls (triggering/worsening) | Trauma (even minor) can precipitate acute disc herniation or exacerbate existing spondylotic nerve root compression |
| Age 55, male | Peak incidence of cervical spondylosis is 40–50 years, males more affected than females |
As noted in Tintinalli's Emergency Medicine: "The symptoms of an acute cervical disk prolapse include neck pain, headache, pain distributed to the shoulder and along the medial scapular border, dermatome pain, and dysesthesia in the spinal root distribution to the shoulder and arm."
Pathology at the C4–C5 level compresses the C5 root, causing pain, paresthesias, and sometimes loss of sensation over the shoulder, with potential weakness of the deltoid and biceps muscles — Bradley and Daroff's Neurology in Clinical Practice.
Differential Diagnoses to Consider
- Cervical spondylotic radiculopathy (C5) — Most likely ✅
- Cervical disc herniation (C4–C5 or C5–C6) — Often coexists
- Rotator cuff tear / impingement syndrome — Pain on arm elevation; could be a co-existing shoulder pathology worsened by the fall
- Adhesive capsulitis (frozen shoulder) — Shoulder pain with restricted movement; however, stiffness here appears to be primarily cervical
- Cervical myelopathy — If cord is compressed (check for gait problems, hand clumsiness, bladder symptoms)
- Brachial plexopathy — Less likely without trauma to the brachial region
- Referred cardiac pain — Must exclude in a 55-year-old male with left-sided arm/shoulder pain (check for exertional chest pain, ECG)
Key Clinical Tests to Perform
- Spurling's Test: Neck extension + lateral flexion to the left + axial compression → reproduces left shoulder/arm pain = positive for C5 radiculopathy
- Cervical distraction test: Manual traction of the neck → if it relieves pain, confirms root compression
- Shoulder abduction relief sign: Placing the arm on top of the head relieves radicular pain
- Neurological exam: Test deltoid (C5), biceps reflex (C5–C6), sensation over lateral shoulder
Investigations Required
- MRI cervical spine — Gold standard; identifies nerve root compression, disc herniation, osteophytes, canal stenosis
- X-ray cervical spine (AP + lateral) — Shows disc space narrowing, osteophytes, loss of lordosis
- Shoulder X-ray — Rule out rotator cuff calcification or glenohumeral arthritis
- ECG + cardiac workup — Essential in a 55-year-old male with left arm symptoms
- EMG/NCS — If diagnosis remains unclear; loss of CMAP amplitude with preserved SNAP suggests radiculopathy
- MRI shoulder — If rotator cuff tear suspected
Management
Conservative (First Line — Effective in Most Cases)
Per Bradley and Daroff's Neurology: "The mainstay of treatment is conservative management — a combination of a period of reduced physical activity with use of a soft cervical collar, physiotherapy, and anti-inflammatory and analgesic agents. Most patients improve, even those with mild to moderate motor deficits."
Medications:
| Drug | Dose | Purpose |
|---|---|---|
| Diclofenac sodium (NSAID) | 50 mg twice daily with food | Anti-inflammatory, pain relief |
| Methocarbamol or Cyclobenzaprine | 500 mg TDS or 5 mg TDS | Muscle relaxant for neck stiffness |
| Pregabalin or Gabapentin | 75–150 mg BD or 300 mg BD | Neuropathic/radicular pain |
| Pantoprazole | 40 mg once daily | GI protection with NSAIDs |
| Vitamin B12 + B complex | Once daily | Nerve support |
Note: These medications must be prescribed by a licensed physician after proper clinical evaluation. Dosing must be individualized.
Non-pharmacological:
- Soft cervical collar — Short-term immobilization to reduce root tension
- Physiotherapy / cervical traction — Reduces foraminal pressure on the nerve root
- Heat therapy to neck and shoulder for muscle stiffness
- Postural correction — Avoid prolonged neck flexion (phones, screens)
- Rotator cuff strengthening exercises (after acute pain subsides)
If Conservative Fails (After 6–8 Weeks)
- Epidural corticosteroid injection (cervical transforaminal steroid injection) — Good for radicular pain
- Surgery (ACDF — Anterior Cervical Discectomy and Fusion) — Reserved for:
- Unrelenting pain despite adequate conservative treatment
- Progressive weakness in the C5 territory (deltoid, biceps)
- Signs of myelopathy (cord compression)
Red Flags — Seek Urgent Evaluation If:
- 🚨 Progressive weakness or paralysis of the arm
- 🚨 Loss of bladder/bowel control (suggests myelopathy)
- 🚨 Bilateral arm/leg symptoms
- 🚨 Chest pain, breathlessness, jaw pain (cardiac cause must be excluded urgently in a 55-year-old male)
- 🚨 Night sweats, unexplained weight loss (rule out malignancy)
Summary
This patient most likely has cervical spondylosis with C5 nerve root radiculopathy, likely triggered/worsened by his two falls. The combination of left shoulder pain, neck stiffness, headache, periorbital "stretching" sensation, and pain aggravated by arm elevation and extension all fit the C5 dermatome and referred pain pattern of cervical disc disease at C4–C5 or C5–C6. An MRI cervical spine is the most important next investigation. A cardiac cause must also be excluded given his age and left-sided presentation.
Sources: Bradley and Daroff's Neurology in Clinical Practice; Tintinalli's Emergency Medicine; Miller's Review of Orthopaedics; Goldman-Cecil Medicine.
psa normal ramge
Finding Sources
Reading File
Finding Sources
Finding Sources
I have enough information from the textbooks to give a complete, authoritative answer.
PSA (Prostate-Specific Antigen) — Normal Range
General Reference Range
| PSA Level | Interpretation |
|---|---|
| 0 – 4.0 ng/mL | Normal (standard cutoff) |
| 4.0 – 10.0 ng/mL | "Grey zone" — suspicious, biopsy may be needed |
| > 10.0 ng/mL | High — significant risk of prostate cancer |
The normal reference range is 0 to 4 ng/mL — Henry's Clinical Diagnosis and Management by Laboratory Methods
Age-Specific PSA Reference Ranges
(More clinically relevant — PSA normally rises with age due to prostate enlargement)
| Age Group | Normal PSA Upper Limit |
|---|---|
| 40–49 years | ≤ 2.5 ng/mL |
| 50–59 years | ≤ 3.5 ng/mL |
| 60–69 years | ≤ 4.5 ng/mL |
| 70–79 years | ≤ 6.5 ng/mL |
Age-specific ranges help detect cancer earlier in younger men and avoid unnecessary biopsies in older men with mildly elevated PSA.
PSA Velocity (Rate of Rise)
- A PSA rise of > 0.75 ng/mL per year is considered suspicious for prostate cancer, even if the absolute value is within normal range.
Important Caveats
PSA can be elevated without cancer (not cancer-specific):
- ✅ BPH (Benign Prostatic Hyperplasia) — most common cause
- ✅ Acute prostatitis (infection/inflammation)
- ✅ Prostate biopsy or instrumentation — causes transient spike
- ✅ Digital rectal examination (DRE) — mild transient rise
- ✅ Ejaculation — can slightly raise PSA (check after 48 hrs abstinence)
- ✅ Urinary tract infection
PSA can be normal despite cancer:
- 15% of men with PSA < 4.0 ng/mL still have prostate cancer on biopsy (Textbook of Family Medicine)
- PSA is a screening tool, not a definitive diagnostic test
Free vs. Total PSA Ratio
When PSA is in the grey zone (4–10 ng/mL):
| Free/Total PSA Ratio | Cancer Risk |
|---|---|
| > 25% | Low risk |
| 10–25% | Intermediate |
| < 10% | High risk — biopsy strongly recommended |
Screening Recommendations
- Age 50 — Routine PSA screening for average-risk men
- Age 40–45 — Earlier screening for high-risk men (family history of prostate cancer, African-American men)
Source: Henry's Clinical Diagnosis and Management by Laboratory Methods; Robbins & Kumar Basic Pathology; Textbook of Family Medicine
This is a shared conversation. Sign in to Orris to start your own chat.