Everything in detail about varicose veins and management
Reading File
Finding Sources
Searching PubMed
"varicose veins"[MeSH Terms] AND management
Searching Images
varicose veins anatomy pathophysiology
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Loading Image
Loading Image
I now have comprehensive information from multiple authoritative textbooks. Let me compile the full detailed answer.
Varicose Veins — Comprehensive Overview
1. Definition & Epidemiology
Varicose veins are abnormally dilated, tortuous superficial veins produced by prolonged, increased intraluminal pressure resulting in vessel dilation and subsequent incompetence of the venous valves. The superficial veins of the lower extremity are most commonly involved because venous pressures at these sites can be markedly elevated — up to 10 times normal — by prolonged dependent posture.
Prevalence:
- Present in at least 10% of the general population
- Up to 20% of males and one-third of females develop lower extremity varicose veins
- By age 65, prevalence in the Western population exceeds 55% (Edinburgh Vein Study)
Risk Factors:
- Female sex (prolonged IVC compression from gravid uterus during pregnancy)
- Obesity
- Family history (faulty venous wall development — genetic predilection)
- Prolonged standing or inactivity
- Occupation (prolonged standing)
- Prior phlebitis destroying valve structure
- Congenital syndromes: Klippel-Trénaunay, Ehlers-Danlos, clonal trisomies
- Compressive syndromes: May-Thurner (iliac vein compression) and Nutcracker syndrome (left renal vein compression)
— Schwartz's Principles of Surgery, 11th Ed.; Robbins, Cotran & Kumar Pathologic Basis of Disease; Current Surgical Therapy, 14th Ed.
2. Anatomy & Pathophysiology
Venous Return Physiology
The lower limb veins carry blood against gravity by two principal mechanisms:
- Calf muscle pump: Contraction of calf muscles compresses the soleal sinuses and deep veins, generating pressures up to 300 cm H₂O, propelling blood proximally (the "ventricular" phase).
- Perforating vein valves: During relaxation, blood flows from the superficial system through perforators into the deep veins. The superficial venous system acts like an atrium, and the deep calf veins like a ventricle.
Standing pressure on the dorsum of the foot equals the hydrostatic column from foot to right heart — approximately 70–80 cm H₂O.
Sites of Valve Incompetence
The critical junctions where incompetent valves cause varicosities:
- Saphenofemoral junction (SFJ) — saphena varix where the great saphenous vein (GSV) joins the femoral vein
- Mid-thigh perforating vein — between GSV and femoral vein
- Calf perforating veins (Cockett's perforators) — at 5, 10, and 15 cm above the medial malleolus
- Saphenopopliteal junction (SPJ) — small saphenous vein (SSV) joining the popliteal vein
Mechanism of Varicosity Formation
Two proposed mechanisms:
- Valve-first theory: A malfunctioning valve allows retrograde flow → increased venous pressure → vein dilation → progressive incompetence of distal valves (a cascade effect).
- Wall-first theory (primary varicose veins): Intrinsic weakness of the vein wall causes primary dilation → valve leaflets separate and become incompetent → reflux develops.
When the SFJ valve becomes incompetent, blood flows from the common femoral vein back into the GSV, causing progressive dilation of the entire saphenous system.
Venous hypertension consequences: Ambulatory venous pressure (AVP) >35 mmHg begins causing cutaneous manifestations; AVP >90 mmHg almost certainly produces skin changes.
— Pfenninger & Fowler's Procedures for Primary Care, 3rd Ed.
3. Classification
Primary vs. Secondary
| Type | Mechanism |
|---|---|
| Primary | Intrinsic abnormalities of the venous wall (no underlying deep vein disease) |
| Secondary | Associated with deep and/or superficial venous insufficiency (e.g., post-DVT) |
CEAP Classification (2020 Revision)
The Clinical-Etiology-Anatomy-Pathophysiology (CEAP) system is the international standard:
| Class | Description |
|---|---|
| C0 | No visible or palpable signs |
| C1 | Telangiectasias or reticular veins |
| C2 | Varicose veins |
| C2r | Recurrent varicose veins |
| C3 | Edema |
| C4a | Pigmentation or eczema |
| C4b | Lipodermatosclerosis or atrophie blanche |
| C4c | Corona phlebectatica |
| C5 | Healed venous ulcer |
| C6 | Active venous ulcer |
| C6r | Recurrent active venous ulcer |
Morphological Classification by Vein Size (Dermatology 5e)
| Type | Description | Diameter | Color | Treatment |
|---|---|---|---|---|
| I — Telangiectasias | Spider veins / telangiectatic matting | 0.1–1 mm | Red | Microsclerotherapy, IPL, laser (pulsed dye, 1064 nm Nd:YAG) |
| II — Venulectasias | Small tortuous veins | 1–2 mm | Violaceous | Sclerotherapy, Nd:YAG laser |
| III — Reticular varicosities | Blue-green feeding veins | 2–4 mm | Cyanotic blue/green | Sclerotherapy, ambulatory phlebectomy |
| IV — Branch varicosities | Perforator-related | 3–8 mm | Blue/blue-green | Ambulatory phlebectomy, sclerotherapy |
| V — Saphenous varicosities | Truncal/axial (GSV, SSV) | ≥5 mm | Blue/green, may not be visible | Ambulatory phlebectomy, RFA, EVLA, sclerotherapy |
— Dermatology 2-Volume Set, 5th Ed.; Current Surgical Therapy, 14th Ed.
4. Clinical Features
Symptoms
- Unsightly cosmetic appearance
- Aching, heaviness, and fatigue in the affected leg
- Pruritus over varicosities
- Swelling (mild edema)
- Worsening with prolonged standing or sitting; relieved by leg elevation above heart level
Signs (Mild to Severe)
- Dilated, tortuous, visible subcutaneous veins
- Mild dependent edema
- Thrombophlebitis (superficial vein inflammation/thrombosis)
- Hyperpigmentation (stasis dermatitis / "brawny induration" — brownish discoloration from hemolysis of extravasated RBCs)
- Lipodermatosclerosis (fibrous thickening of subcutaneous fat)
- Venous ulceration — typically above medial malleolus; poor wound healing and superimposed infections are common
- Bleeding from attenuated vein clusters
- Stasis dermatitis ("brawny induration")
Important: Embolism from superficial varicose veins is very rare, unlike deep vein thrombosis which commonly leads to pulmonary embolism.
Pathology (Robbins)
Incompetence → stasis → congestion → edema → pain → thrombosis → secondary tissue ischemia from chronic venous congestion → stasis dermatitis and ulceration.
5. Diagnosis
Clinical Examination
Trendelenburg (tourniquet) test:
- Patient lies supine; leg is elevated to drain veins
- Tourniquet placed around upper thigh below SFJ
- Patient stands up
- No filling below tourniquet → SFJ incompetence (reflux from femoral into GSV)
- A second tourniquet below the knee tests the SPJ and calf perforators
Duplex Ultrasound (Gold Standard)
Essential for all patients. Protocol:
- Performed with patient standing or in steep reverse Trendelenburg to allow accurate assessment of valve competency
- Pathologic reflux defined as: reversal of flow for >500 ms in perforators and truncal superficial veins; >1000 ms in deep veins
- Vein diameters >5 mm (>3.5 mm for perforators) correlate with symptomatic reflux
- Must identify the most proximal/central source of reflux
- Correlate duplex findings with symptoms — mild or isolated segmental reflux in a small vein rarely warrants intervention
Additional Investigations
- Venous Clinical Severity Score (r-VCSS) — validated tool for outcomes and treatment planning
- Aberdeen Varicose Vein Score — QoL assessment; identifies patients most likely to benefit from intervention
- In complex cases: CT venography, MR venography (for pelvic vein/gonadal vein incompetence)
6. Management
Conservative (First-Line)
Elastic Compression Stockings:
- Cornerstone of conservative management
- Compression classes:
- 20–30 mmHg: mild symptoms, telangiectasias
- 30–40 mmHg: moderate varicosities, edema
- 40–50 mmHg: severe disease, venous ulcers
- Length: knee-high to waist-high, should cover symptomatic varices
- Provides sufficient symptom relief in many patients
- Lifestyle measures: weight loss, leg elevation, avoidance of prolonged standing
Interventional Management
Indicated when:
- Symptoms worsen or are unrelieved despite compression therapy
- Lipodermatosclerosis or venous ulceration present
- Patient desires treatment for cosmesis
Randomized trials demonstrate significantly improved quality of life with interventional treatment over compression alone.
A. Sclerotherapy
Mechanism: Sclerosing agents destroy the venous endothelium → inflammatory adhesion and subsequent fibrosis/obliteration of the vein lumen.
Sclerosing Agents (concentration by vessel size):
| Agent | Small vessels (telangiectasias) | Larger varicosities |
|---|---|---|
| Hypertonic saline | 11.7–23.4% | 23.4% |
| Sodium tetradecyl sulfate (STS/Sotradecol) | 0.125–0.25% | 0.5–1% |
| Polidocanol (Aethoxysklerol) | 0.25–0.5% | 0.75–1.0% |
Post-injection protocol:
- Elastic bandages applied immediately after injection
- Worn continuously for 3–5 days to oppose inflamed vein walls and prevent thrombus
- Compression stockings for minimum 2 weeks after bandage removal
Complications: Allergic reaction, local hyperpigmentation, thrombophlebitis, DVT, skin necrosis, telangiectatic matting.
Foam Sclerotherapy:
- Foamed detergent (liquid:gas ratio 1:4) is more potent — the concentrated sclerosant is on the outer micelle of each bubble
- Fewer injections needed; treats larger segments
- Varithena® (polidocanol 1% injectable foam): FDA-approved for incompetent GSVs, accessory saphenous veins, and visible GSV system varicosities above and below the knee; uses patented O₂:CO₂ (65:35) gas mixture producing cohesive microfoam <100 micron bubbles; provides circumferential endothelial destruction
- A multicenter RCT confirmed significant symptom relief and improved cosmesis with foam sclerotherapy vs. placebo
Foam technique variants:
- Air bolus technique: Inject <0.5 mL air before sclerosant to displace blood and confirm intravascular needle position
- Multiple precannulation sites (MPS): Proximal and distal cannulation while patient stands (to distend veins), then veins treated in elevation
B. Endovenous Thermal Ablation
For patients with symptomatic GSV or SSV reflux.
Two main techniques:
| Feature | Endovenous Laser Ablation (EVLA) | Radiofrequency Ablation (RFA) |
|---|---|---|
| Energy | Laser (810–1470 nm) | Radiofrequency (RF waves) |
| Mechanism | Thermal destruction of vein wall | Resistive heating → collagen contraction |
| Access | 21-gauge needle under ultrasound → sheath → laser fiber advanced to SFJ | Same access; RFA catheter |
| Anesthesia | Tumescent anesthetic around GSV | Tumescent anesthetic around GSV |
| Efficacy | Durable GSV ablation; comparable to surgery | Comparable to EVLA and surgery |
| Recovery | More rapid than open surgical stripping | More rapid than open surgical stripping |
| Complications | DVT, ecchymosis, saphenous nerve injury | DVT, ecchymosis, saphenous nerve injury |
Procedure steps:
- Distal thigh or proximal calf GSV punctured with 21-gauge needle under US guidance
- Guidewire inserted → sheath placed
- Fiber/catheter advanced to just below (not at) SFJ
- Tumescent anesthetic infiltrated circumferentially around GSV (thermal protection and compression)
- Vein treated as catheter is withdrawn
Recent meta-analysis (Jiang et al., 2024, PMID 38316290): RFA and EVLA have comparable efficacy in lower extremity varicose veins, with RFA possibly associated with fewer complications.
C. Non-Thermal, Non-Sclerosant Ablation
Cyanoacrylate glue (VenaSeal):
- Proprietary adhesive closes the vein lumen without heat or sclerosant
- No tumescent anesthesia required
- Promising early results; no thermal injury risk to surrounding structures
Mechanochemical ablation (MOCA — ClariVein):
- Combines catheter-based mechanical endoluminal injury with simultaneous sclerosant injection
- No tumescent anesthesia required
- Lower risk of nerve injury or thermal damage
D. Surgical Treatment
1. Ambulatory Phlebectomy (Stab Avulsion)
- Best for large branch varicosities
- Technique: 2-mm incisions directly over varicosities → varicosity dissected from subcutaneous tissue proximally and distally → simple avulsion (no ligation needed in most cases)
- Bleeding controlled by leg elevation, manual compression, and pre-procedure tumescent anesthesia
2. Great Saphenous Vein (GSV) Stripping
- Preferred for GSVs of very large diameter (>2 cm) or when endovenous techniques are not feasible
- Technique: Small medial groin incision + incision below the knee → GSV removed using blunt tip catheter or invagination pin stripper
- GSV stripping → lower recurrence rate and better QoL than saphenofemoral junction ligation alone
- Complications: Ecchymosis, hematoma, lymphocele, DVT, infection, saphenous nerve injury
3. Saphenofemoral/Saphenopopliteal Junction Ligation
- Historically performed alone, but higher recurrence than stripping
- Popliteal fossa dissection carries risk of common fibular nerve injury → footdrop (nerve lies superficial to popliteal vein)
Anatomical Warning: In the popliteal fossa — popliteal artery is deepest, popliteal vein is intermediate, sciatic nerve/divisions are most superficial. The common fibular nerve is at risk during SSV/SPJ surgery.
Management of Specific Complications
Chronic Venous Insufficiency (CVI)
- Affects ~600,000 people in the US; costs ~$1 billion/year in healthcare
- 2 million workdays lost per year
- Management: graduated compression, wound care, endovenous/surgical treatment of reflux
- Venous ulcers: multilayer compression bandaging (Unna boot), moist wound healing, treatment of underlying reflux
Superficial Thrombophlebitis
- Warm compresses, NSAIDs, compression
- If propagating toward SFJ: low molecular weight heparin or anticoagulation
Variceal Bleeding
- Leg elevation, direct pressure
- Followed by sclerotherapy or surgical treatment
7. Special Situations
Other Varicosities Sharing the Pathophysiology
| Site | Cause | Significance |
|---|---|---|
| Esophageal varices | Portal hypertension (cirrhosis, portal vein obstruction) | Most dangerous — rupture causes massive fatal GI hemorrhage |
| Hemorrhoids | Prolonged pelvic congestion (pregnancy, straining) | Bleeding, thrombosis, painful ulceration |
| Caput medusae | Portal hypertension → periumbilical vein dilation | Clinical sign of portal hypertension |
Pelvic Varicosities
- Dilated, tortuous gonadal/ovarian veins (typically left-sided) cause chronic pelvic pain
- Diagnosed by CT/MRI venography or pelvic duplex
- Treated by endovascular embolization
Recurrence Mechanisms
- Neovascularization at the SFJ after stripping/ablation
- Accessory lymph node vessels serving as reflux conduits
- Incomplete ablation of all tributaries
- New incompetence at other junctions
8. Recent Evidence Update (2024–2026)
- RFA vs. EVLA meta-analysis (PMID 38316290, 2024): Both techniques have comparable long-term ablation rates; RFA may have marginal safety advantages.
- Reflux patterns in primary CVD (PMID 39025298, 2024): Systematic review characterizing anatomical reflux patterns to guide treatment planning.
- Physiotherapy for venous ulcers (PMID 40504402, 2025): Exercise/physiotherapy interventions improve healing of chronic venous ulcers.
- Platelet-rich plasma for venous ulcers (PMID 41643347, 2026): Meta-analysis supports PRP as adjunct therapy improving venous ulcer healing rates.
- Restless legs syndrome and CVI (PMID 41306950, 2025): Systematic review confirms association — screening for CVI is warranted in RLS patients.
Summary Algorithm
Varicose Veins Suspected
↓
Clinical Examination + Duplex Ultrasound
↓
CEAP Classification
↓
C1–C2: Conservative (compression, lifestyle)
↓ if symptomatic/refractory
C2–C3: Sclerotherapy (liquid for small, foam for larger)
OR
Endovenous ablation (RFA/EVLA for truncal reflux)
OR
Ambulatory phlebectomy (branch varicosities)
↓
C4–C6 (skin changes, ulcers):
Aggressive treatment + wound care
Deep vein assessment before ablation
Multilayer compression for ulcers
GSV stripping if vein diameter >2 cm
Sources: Schwartz's Principles of Surgery, 11th Ed.; Current Surgical Therapy, 14th Ed.; Pfenninger & Fowler's Procedures for Primary Care, 3rd Ed.; Dermatology 2-Vol Set, 5th Ed.; Robbins, Cotran & Kumar Pathologic Basis of Disease; Gray's Anatomy for Students; PubMed systematic reviews 2024–2026.
Complications
Finding Sources
Finding Sources
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Searching Images
venous stasis ulcer lipodermatosclerosis leg
I now have comprehensive data. Let me compile the full detailed answer on complications.
Complications of Varicose Veins
Complications can be divided into two major categories: disease complications (resulting from the underlying venous disease itself) and treatment complications (resulting from interventions).
A. Disease Complications
1. Chronic Venous Insufficiency (CVI)
The most important and common complication — a progressive syndrome of sustained venous hypertension affecting skin, subcutaneous tissue, and wound healing.
Pathophysiology: Sustained ambulatory venous pressure (AVP) → capillary wall distension → leakage of macromolecules, fibrin, and red cells into the interstitium → inflammatory cascade → tissue ischemia and fibrosis.
- AVP <35 mmHg: skin manifestations uncommon
- AVP >80 mmHg: 80% incidence of venous ulceration
Subtypes:
- Primary CVI: Intrinsic vein wall abnormalities
- Secondary CVI (Postthrombotic Syndrome / PTS): Follows DVT; valve destruction from thrombus organization leads to combined reflux + obstruction — usually the most severe form
Signs and symptoms:
- Leg fatigue, heaviness, discomfort
- Progressive edema (initially pitting, later non-pitting)
- Varicosities
Impact: 600,000 affected in the US; 2 million workdays lost per year; $1 billion/year in healthcare costs. Quality-of-life studies: 65% of patients with venous ulcers report severe pain, 81% have decreased mobility, 100% have impaired work capacity.
— Schwartz's Principles of Surgery, 11th Ed.
2. Edema
One of the earliest and most consistent complications. Sustained venous hypertension raises capillary hydrostatic pressure, driving fluid into the interstitium. Initially pitting (reducible by elevation), progresses to non-pitting with chronic protein accumulation. Uncontrolled edema creates a setup for poor wound healing.
3. Stasis Dermatitis (Venous Eczema)
- Mechanism: Chronic venous congestion → extravasation of RBCs → haemolysis → haemosiderin deposition → local inflammatory reaction
- Appearance: Brown-bronze "brawny" pigmentation of the lower leg (especially medial malleolus); associated with eczematous pruritic rash, erythema, scaling
- Also called "brawny induration" — the brawny colour comes directly from haemolysis of extravasated red cells
- In CEAP: C4a (pigmentation or eczema)
— Robbins, Cotran & Kumar Pathologic Basis of Disease
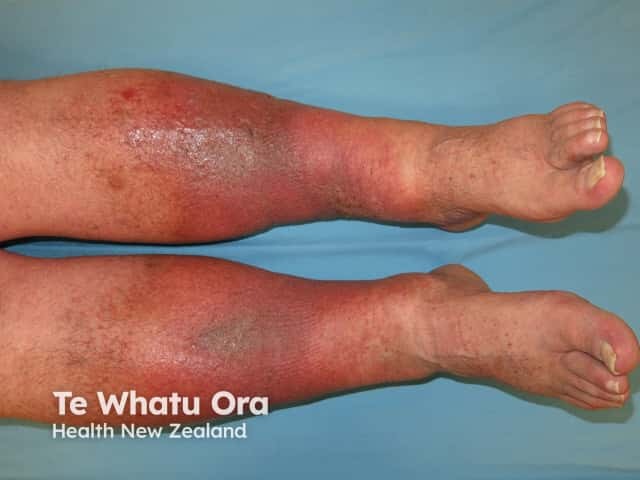
4. Lipodermatosclerosis
- Definition: Fibrotic thickening and induration of the subcutaneous fat of the lower leg, resulting from chronic venous hypertension and tissue ischaemia
- Appearance: Woody, board-like induration of the skin; often circumferential in the "gaiter zone" — classically giving an "inverted champagne bottle" or "champagne bottle" deformity of the lower leg
- In CEAP: C4b (lipodermatosclerosis or atrophie blanche)
- Predisposes to chronic non-healing ulcers and represents advanced CVI
5. Atrophie Blanche (Livedoid Vasculopathy)
- Focal white, ivory-coloured, atrophic, stellate scars surrounded by hyperpigmentation and telangiectasias
- Located in the "gaiter zone" (lower third of leg)
- Represents end-stage scarring from microthrombi in dermal capillaries in the setting of venous hypertension
- In CEAP: C4b — clinically significant because the skin is extremely fragile and prone to ulceration with minor trauma
- Highly painful compared to standard venous ulcers
6. Corona Phlebectatica
- Fan-shaped network of intradermal telangiectasias at the medial or lateral ankle/foot
- Also called "ankle flare"
- Reflects underlying perforator incompetence and advanced ambulatory venous hypertension
- In CEAP: C4c
- A clinical warning sign that severe CVI is present
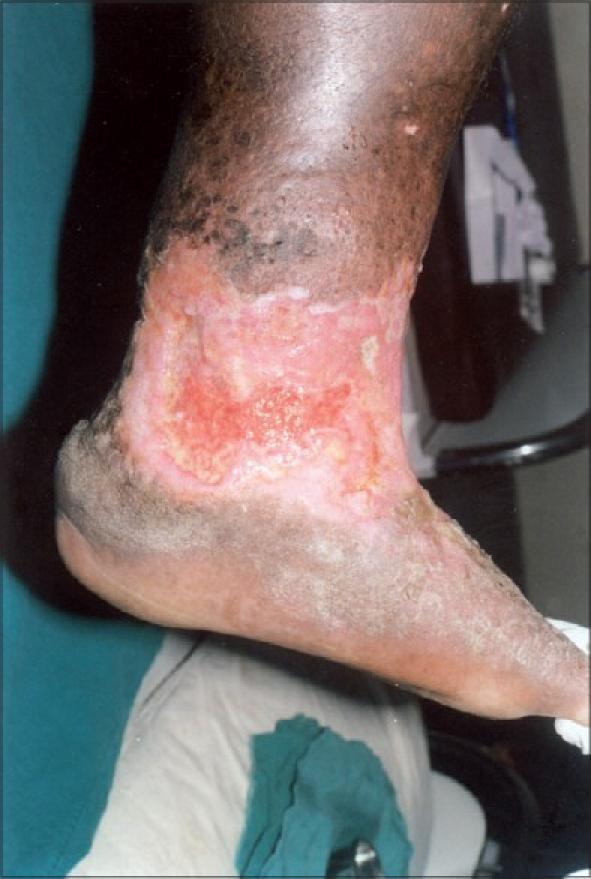
7. Venous Ulceration (Venous Stasis Ulcer)
The most severe complication of varicose veins and CVI. The most common type of chronic leg ulcer.
Pathophysiology: Incompetent venous valves + calf muscle pump failure → sustained venous hypertension → capillary wall distension + leakage of macromolecules (including fibrinogen, forming a "fibrin cuff" around capillaries) → limits oxygen and nutrient diffusion → tissue ischaemia → ulceration.
Characteristic features:
| Feature | Venous Ulcer |
|---|---|
| Location | Medial aspect of leg, above medial malleolus ("gaiter zone") |
| Shape | Irregular, shallow, round or oblong |
| Base | Beefy red granulation tissue; may have fibrinous slough |
| Pain | Variable — present but less severe than arterial or pyoderma gangrenosum ulcers |
| Surroundings | Stasis dermatitis, lipodermatosclerosis, haemosiderin pigmentation |
| Exudate | Moderate to heavy |
| CEAP | C6 (active); C5 (healed) |
Management of venous ulcers:
- Treat the underlying venous reflux (sclerotherapy/endovenous ablation)
- Compression therapy is the cornerstone: 30–40 mmHg below-knee elastic stockings
- 93% healing rate with compliant compression use
- Compliance is critical: ulcer recurrence 29% at 5 years (compliant) vs. 100% at 3 years (non-compliant)
- Unna's Boot: Three-layer dressing (zinc oxide impregnated gauze + elastic wrap + cohesive bandage); applied from forefoot to below knee; changed weekly
- Multilayer elastic wraps: Provide sustained compression; reduce inflammatory cytokines and matrix metalloproteins
- Pneumatic compression devices: For immobile patients or adjunct therapy
- Wound care: Moist wound environment; débridement of slough; antimicrobials for infected ulcers
- Rule out arterial insufficiency (ABI) before high-compression therapy
- Optimise systemic factors: diabetes, nutrition, immunosuppression, heart failure
— Schwartz's Principles of Surgery, 11th Ed.; Sabiston Textbook of Surgery
8. Superficial Thrombophlebitis
- Definition: Thrombosis and inflammation of a superficial varicose vein
- Presentation: Tender, red, warm, indurated cord along the course of a varicosity; overlying erythema and induration
- Mechanism: Stasis within the dilated varicosity → spontaneous thrombosis → inflammatory response
- Risk: Rare embolism from superficial veins (contrast with deep vein thrombosis which commonly embolises)
- Important exception: If thrombus propagates to within 3–5 cm of the SFJ (saphenofemoral junction), risk of extension into the deep system (DVT + pulmonary embolism) increases significantly → anticoagulation warranted
- Management:
- NSAIDs + warm compresses + compression
- Low-molecular-weight heparin if propagating toward SFJ or extensive
- Surgical drainage of large, tense thrombus for symptomatic relief
9. Deep Vein Thrombosis (DVT)
- CVI and venous stasis are independent risk factors for DVT
- Venous wall damage, venous hypertension, and turbulent flow promote thrombosis
- Conversely, DVT is also a cause of secondary CVI (postthrombotic syndrome) — a bidirectional relationship
- DVT carries risk of pulmonary embolism — the major life-threatening complication in the venous disease spectrum
10. Variceal Haemorrhage
- Rupture of a large subcutaneous varicosity, either spontaneously or from minor trauma
- Blood loss can be profuse and alarming, particularly in elderly patients on anticoagulants
- Attenuated, thin-walled vein clusters are at highest risk
- Immediate management: Leg elevation + direct pressure → rapid cessation in most cases
- Definitive treatment: sclerotherapy or surgical avulsion
11. Secondary Infection / Cellulitis
- Chronic venous stasis and ulceration impair local immune defences
- The oedematous, poorly oxygenated skin is highly susceptible to bacterial invasion
- Cellulitis (most commonly Streptococcus pyogenes, Staphylococcus aureus) is a frequent complication of venous ulcers and stasis dermatitis
- Recurrent cellulitis can damage lymphatics → secondary lymphoedema — a devastating vicious cycle
12. Contact Dermatitis
- From chronic application of topical agents (antiseptics, wound dressings, lanolin, rubber in compression garments) to sensitised, compromised skin
- A frequent and often under-recognised complication of long-standing venous ulcer management
- Patch testing may be required
13. Restless Legs Syndrome (RLS)
A recently confirmed association: chronic venous insufficiency is significantly associated with RLS (systematic review, PMID 41306950, 2025). The mechanism may involve venous congestion causing sensory nerve irritation. Treatment of underlying venous insufficiency can improve RLS symptoms.
B. Complications of Treatment
Complications of Sclerotherapy
| Complication | Details |
|---|---|
| Hyperpigmentation | Most common local side effect (haemosiderin deposition); usually resolves over months but can persist. Reduced by post-injection compression |
| Telangiectatic matting | New fine telangiectasias appearing around injection sites; possibly from angiogenesis or opening of pre-existing subthreshold vessels. Treated with further sclerotherapy |
| Thrombophlebitis | Local inflammatory reaction in the treated vein; expected to some degree; excessive thrombus requires evacuation |
| DVT | Rare but serious; especially with foam sclerotherapy and large volumes; sclerosant can track into the deep system via perforators. Duplex surveillance is recommended |
| Allergic reaction / Anaphylaxis | More common with sodium tetradecyl sulfate; rare with hypertonic saline (no anaphylaxis risk with hypertonic saline — a major advantage) |
| Skin necrosis / Cutaneous ulceration | Perivenous extravasation of sclerosant destroys surrounding skin; sodium tetradecyl sulfate carries higher risk than polidocanol. Prevented by small volumes, correct needle placement, air-bolus technique |
| Visual disturbances / Migraine aura | Mostly with foam sclerotherapy; microfoam bubbles may enter arteriovenous connections or pass via PFO (patent foramen ovale) |
| Neurological complications | Rare — stroke, transient ischaemic attack reported with foam sclerotherapy, particularly in patients with cardiac shunts |
| Pulmonary microembolism | Microfoam particles reaching pulmonary circulation; usually clinically silent but chest tightness reported |
— Dermatology 5e (Dermatology 2-Volume Set); Schwartz's Principles of Surgery
Complications of Endovenous Thermal Ablation (EVLA/RFA)
| Complication | Details |
|---|---|
| DVT / VTE | Most clinically significant; incidence ~1–5%; extension of thrombus from the treated vein into the deep system (endovenous heat-induced thrombus — EHIT) |
| Ecchymosis | Very common; resolves within 2–3 weeks; reduced by adequate tumescent anesthesia |
| Saphenous nerve injury | Proximity of the saphenous nerve to the GSV in the calf; dysesthesia/numbness in the medial leg/foot; usually transient; reduced by tumescent anesthesia (acts as a thermal buffer) |
| Sural nerve injury | Risk during SSV ablation in the calf |
| Skin burns | Inadequate tumescent anesthesia; incorrect catheter placement too close to skin |
| Paraesthesias | Thermal nerve injury; usually transient |
| Thrombophlebitis | Treated vein or adjacent varicosities |
| Infection | Rare; access-site wound infection |
Complications of Surgical Treatment
GSV Stripping / Ligation
| Complication | Details |
|---|---|
| Saphenous nerve injury | Most common nerve complication; sensory deficit/dysesthesia along medial leg and foot; risk is higher if stripping is performed below the knee |
| Ecchymosis / Haematoma | Expected; large haematomas may require drainage |
| Lymphocele / Lymphorrhoea | Groin lymphatics disrupted at SFJ ligation; a tender fluctuant groin swelling may develop |
| DVT / Pulmonary embolism | Operative risk; appropriate VTE prophylaxis required |
| Wound infection | Groin incision is at particular risk (warm, moist, near inguinal crease) |
Popliteal Fossa Surgery (SSV/SPJ Ligation)
| Complication | Details |
|---|---|
| Common fibular (peroneal) nerve injury | The most feared complication — the nerve is the most superficial structure in the popliteal fossa (nerve > vein > artery from superficial to deep). Misidentification → ligation/damage → foot drop (absent dorsiflexion + eversion, lateral leg/dorsal foot sensory loss, wasting of fibular muscles) |
| Popliteal vein injury | Can cause DVT or significant haemorrhage |
The popliteal fossa anatomy (superficial to deep): sciatic nerve divisions > popliteal vein > popliteal artery. The common fibular nerve diverges laterally around the fibular head — extreme care is essential during SPJ surgery.
— Gray's Anatomy for Students; Schwartz's Principles of Surgery, 11th Ed.
Ambulatory Phlebectomy
- Complication rate is extremely low
- Minor haematoma, wound dehiscence, nerve injury (rare), infection, telangiectatic matting, hyperpigmentation
Summary Table
| Complication | Category | CEAP | Severity |
|---|---|---|---|
| Oedema | Disease | C3 | Mild–moderate |
| Stasis dermatitis / Pigmentation | Disease | C4a | Moderate |
| Lipodermatosclerosis | Disease | C4b | Moderate–severe |
| Atrophie blanche | Disease | C4b | Moderate–severe |
| Corona phlebectatica | Disease | C4c | Moderate |
| Healed venous ulcer | Disease | C5 | Severe |
| Active venous ulcer | Disease | C6 | Severe |
| Superficial thrombophlebitis | Disease | — | Mild–moderate |
| DVT / PE | Disease | — | Severe / Life-threatening |
| Variceal haemorrhage | Disease | — | Moderate–severe |
| Cellulitis / Infection | Disease | — | Variable |
| Sclerotherapy: skin necrosis | Treatment | — | Moderate |
| Sclerotherapy: DVT | Treatment | — | Severe |
| Sclerotherapy: neurological | Treatment | — | Severe (rare) |
| EVLA/RFA: EHIT/DVT | Treatment | — | Severe |
| EVLA/RFA: nerve injury | Treatment | — | Moderate |
| Popliteal surgery: foot drop | Treatment | — | Severe |
Sources: Schwartz's Principles of Surgery, 11th Ed.; Robbins, Cotran & Kumar Pathologic Basis of Disease; Dermatology 2-Volume Set, 5th Ed.; Current Surgical Therapy, 14th Ed.; Sabiston Textbook of Surgery; Gray's Anatomy for Students; PubMed PMID 41306950 (2025).
This is a shared conversation. Sign in to Orris to start your own chat.