Causes of postcoital p/v bleeding
Causes of Postcoital (Per Vaginal) Bleeding
1. Cervical Causes (most common overall)
| Cause | Notes |
|---|---|
| Cervical ectropion (erosion) | Eversion of fragile columnar endocervical epithelium onto the ectocervix; bleeds on contact. Common in OCP users and pregnancy. |
| Cervical polyp | Pedunculated benign growths from the endocervical canal; bleed easily on contact |
| Cervicitis | Inflammation from STIs — Chlamydia trachomatis (most common), Neisseria gonorrhoeae, Trichomonas vaginalis, HSV; manifests as cervical friability |
| Cervical intraepithelial neoplasia (CIN) / Cervical carcinoma | PCB is a hallmark symptom; must be excluded regardless of Pap smear status — colposcopy is indicated for any unexplained PCB |
| Condylomata acuminata (HPV) | Friable lesions on the cervix or vaginal walls |
| Nabothian cysts | Usually innocent; rarely bleed |
2. Vaginal Causes
| Cause | Notes |
|---|---|
| Atrophic vaginitis | Postmenopausal hypoestrogenic mucosa is fragile and tears easily during intercourse |
| Vaginal lacerations / trauma | The most common mechanism of genital injury in adult women is coitus itself; ranges from minor contusions to deep lacerations |
| Vaginal candidiasis / trichomoniasis | Inflamed, friable vaginal epithelium |
| Vaginal carcinoma | Rare but important to exclude |
| Foreign body | May cause inflammation and contact bleeding |
3. Uterine / Endometrial Causes
| Cause | Notes |
|---|---|
| Endocervical / endometrial polyps | Polyps prolapsing through the os can bleed post-coitally |
| Endometrial carcinoma | Less commonly presents as PCB; more typical of postmenopausal bleeding |
| Submucosal fibroids | May cause irregular and contact bleeding |
4. Pregnancy-Related Causes
| Cause | Notes |
|---|---|
| Physiological (increased cervical vascularity) | PCB is more common in pregnancy due to increased cervical blood flow |
| Threatened / inevitable abortion | Any trimester |
| Ectopic pregnancy | First trimester; associated with pain |
| Cervical carcinoma in pregnancy | Must be excluded |
| Placenta previa | Second/third trimester — do NOT perform digital exam without USS |
5. Iatrogenic / Other
| Cause | Notes |
|---|---|
| IUD (intrauterine device) | Copper IUD especially can increase bleeding; misplaced string |
| Exogenous hormones / OCP | Breakthrough bleeding; missed doses |
| Tamoxifen use | Associated with endometrial polyps; must sample |
| Coagulopathy | von Willebrand disease, thrombocytopenia; predispose to abnormal bleeding at any site |
| Schistosomiasis haematobium | Genitourinary granulomas causing contact bleeding (in endemic areas) |
Key Clinical Pearls
- Abnormal PCB should always prompt colposcopy, regardless of a normal Pap smear — cervical cancer must be excluded — Pfenninger & Fowler's Procedures for Primary Care
- In postmenopausal women, any PCB warrants endometrial sampling to exclude malignancy — Berek & Novak's Gynecology
- Chlamydial cervicitis is an important and often missed cause, particularly in adolescents and young women — Berek & Novak's Gynecology
- In pregnancy, PCB with cervical motion tenderness/discharge suggests PID or STI — Rosen's Emergency Medicine
Vaginal lacerations / trauma post coitus causes of heavy bleeding
Causes of Heavy Bleeding from Vaginal/Coital Trauma
Why Coital Lacerations Can Bleed Heavily
Predisposing Factors for Heavy Coital Bleeding
1. Anatomical / Site-Related
| Factor | Mechanism |
|---|---|
| Posterior fornix laceration | Most common site of serious coital injury; thin wall adjacent to pouch of Douglas; vessels close to surface |
| Vaginal vault laceration | Following hysterectomy, the vault suture line is a weak point susceptible to penetrative injury |
| Hymenal tears (first intercourse) | Minor but occasionally bleeds significantly; rarely severe unless underlying coagulopathy |
2. Tissue Fragility
| Condition | Mechanism |
|---|---|
| Atrophic vaginitis (postmenopausal) | Hypoestrogenic mucosa is thin, inelastic, poorly lubricated — tears at minimal force |
| Post-radiation vaginitis | Radiation-induced fibrosis and poor vascularity paradoxically causes fragility and impaired healing |
| Lichen sclerosus | Pale, atrophic, friable epithelium; splits easily |
| Lichen planus / erosive vulvovaginitis | Ulcerated and inflamed surfaces |
| Inflammatory vaginitis | Inflamed mucosa is hyperaemic and bleeds more readily |
3. Mechanical / Situational Factors
| Factor | Mechanism |
|---|---|
| Inadequate lubrication / arousal | Friction injury to urothelium |
| Unusual/forceful coital positions | Increased shearing force on posterior fornix |
| Foreign object penetration | Irregular objects cause deeper or wider lacerations |
| Sexual assault / rape | Non-consensual intercourse with struggling — higher force, unprepared tissues |
| First coitus (defloration) | Hymenal and introital tears |
4. Underlying Bleeding Diatheses
| Condition | Notes |
|---|---|
| Von Willebrand disease | Most common inherited coagulopathy; minor trauma → disproportionate bleeding |
| Thrombocytopenia | ITP, haematological malignancy, medication-induced |
| Anticoagulant therapy | Warfarin, DOACs, heparin |
| Liver disease | Coagulopathy from reduced clotting factor synthesis |
| DIC | Consumption of clotting factors |
5. Vascular Abnormalities
| Condition | Notes |
|---|---|
| Arteriovenous malformation (AVM) of vagina/uterus | Rare; can cause catastrophic haemorrhage from minor trauma |
| Varicosities | Pelvic or vulvovaginal varices (seen in pregnancy, portal hypertension) |
| Pregnancy-related hypervascularity | Markedly increased blood flow to cervix and vagina in pregnancy — any laceration bleeds heavily |
AAST Vaginal Injury Scale (severity grading)
| Grade | Injury |
|---|---|
| I | Contusion or haematoma |
| II | Laceration — superficial (mucosa only) |
| III | Laceration — deep (into fat or muscle) |
| IV | Laceration — complex, into cervix or peritoneum |
| V | Injury into adjacent organs (anus, rectum, urethra, bladder) |
Red Flags Warranting Urgent Surgical Evaluation
- Haemodynamic instability after coital trauma
- Bleeding not controlled by direct pressure
- Suspected posterior fornix / peritoneal extension
- Expanding pelvic haematoma
- Post-hysterectomy vault laceration
- Injury following assault with foreign object
Posterior fornix laceration Most common site of serious coital injury; thin wall adjacent to pouch of Douglas; vessels close to surface.
posterior fornix vagina anatomy pouch of Douglas sagittal
Posterior Fornix Laceration — Anatomy & Why It Causes Heavy Bleeding
Anatomical Basis
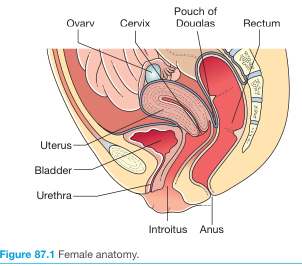
"The posterior vaginal fornix is separated from the posterior cul-de-sac and peritoneal cavity by the vaginal wall and peritoneum." — Berek & Novak's Gynecology
- Anteriorly: posterior surface of uterus, cervix, and posterior vaginal fornix
- Posteriorly: anterior wall of rectum
- Laterally: uterosacral ligaments
Why the Posterior Fornix Bleeds So Heavily
1. Thin wall — only two layers between vaginal lumen and peritoneum
- The thin vaginal wall (mucosa + submucosa + a thin muscularis)
- A layer of peritoneum
2. Rich vascular supply immediately adjacent
- Vaginal artery (branch of internal iliac artery)
- Descending branch of the uterine artery — runs laterally at 3 o'clock and 9 o'clock at the cervix, with anastomoses extending into the fornix
- Anastomotic plexus with middle rectal and internal pudendal arteries
3. Intraperitoneal haemorrhage — "hidden" bleeding
- Blood can pour freely into the abdomen without proportionate external PV bleeding
- The patient may present with haemodynamic shock with surprisingly little visible blood
- This is the same reason culdocentesis (needle aspiration through the posterior fornix) is used to detect haemoperitoneum in ruptured ectopic pregnancy
4. Retroperitoneal extension
Clinical Presentations of Posterior Fornix Laceration
| Severity | Presentation |
|---|---|
| Minor | Superficial mucosal tear, controlled PV bleeding |
| Moderate | Deep laceration into fat/muscle, heavy PV bleeding, haematoma |
| Severe | Full-thickness breach into peritoneal cavity, haemoperitoneum, peritonitis, shock |
| Catastrophic | Vascular injury to uterine/vaginal artery branch — uncontrolled haemorrhage |
High-Risk Scenarios for Posterior Fornix Laceration
- Forceful or unusual coital positions (woman astride — penis directed toward posterior fornix)
- Atrophic postmenopausal vagina — thin walls, poor elasticity, inadequate lubrication
- First intercourse — unrelaxed introitus directs force posteriorly
- Sexual assault — non-consensual, struggle, unprepared tissues
- Post-hysterectomy vault — vault scar is relatively avascular and inelastic; vault dehiscence can occur with vigorous intercourse
- Foreign body penetration — irregular objects, deeper/wider trajectory
Management Principles
- Examination under anaesthesia (EUA) — mandatory if bleeding not adequately assessed in outpatient setting
- Suture repair under direct vision
- If peritoneal breach suspected → laparoscopy/laparotomy
- Uterine artery embolisation for uncontrolled haemorrhage
- Monitor for delayed haemoperitoneum
Guidelines for treatment of vaginal tear grade 4
vaginal laceration repair management guidelines
ACOG RCOG guidelines treatment grade 4 vaginal laceration coital tear management 2023 2024
Treatment of Grade 4 Vaginal/Perineal Tear — Clinical Guidelines
Classification First: Understanding "Grade 4"
| Grade | Extent |
|---|---|
| 1st degree | Perineal skin and vaginal mucosa only |
| 2nd degree | Perineal muscles (not anal sphincter) |
| 3rd degree (a/b/c) | External anal sphincter (EAS) ± internal anal sphincter (IAS) |
| 4th degree | Full thickness through EAS + IAS + rectal mucosa |
| Grade | Extent |
|---|---|
| I | Contusion/haematoma |
| II | Superficial laceration (mucosa only) |
| III | Deep laceration (into fat/muscle) |
| IV | Laceration complex — into cervix or peritoneum |
| V | Injury into adjacent organs (bladder, urethra, rectum) |
A. 4th Degree Perineal Tear (RCOG GTG-29 / ACOG PB-198 / SOGC Guideline 457)
Immediate Principles
- Recognised as an obstetric anal sphincter injury (OASIS)
- Repair must be performed in a well-lit environment (operating theatre preferred)
- Regional or general anaesthesia is mandatory — adequate relaxation is essential for proper repair
- Repair should not be delayed beyond 8–12 hours if an experienced surgeon is not immediately available — studies show equivalent outcomes if repaired within this window (Berek & Novak's Gynecology)
Step-by-Step Surgical Repair (RCOG GTG-29 / ACOG PB-198)
Step 1 — Rectal Mucosa Repair
- The torn rectal mucosa must be repaired first
- Interrupted or continuous sutures using 3-0 polyglactin (Vicryl) or 3-0 chromic catgut
- Sutures placed through the submucosal layer only — do not penetrate the rectal lumen (to reduce infection risk)
- Alternatively, a continuous submucosal suture is acceptable
Step 2 — Internal Anal Sphincter (IAS) Repair
- The IAS is the pale, white smooth muscle layer between rectal mucosa and EAS
- Repair with interrupted or mattress sutures using 3-0 PDS (polydioxanone) or 2-0 Vicryl
- The IAS is often not separately identified or repaired — this is a common error; separate IAS repair improves continence outcomes
Step 3 — External Anal Sphincter (EAS) Repair
| Method | Technique |
|---|---|
| Overlap repair | The two ends of EAS are overlapped and secured with mattress sutures — preferred if ends are long enough |
| End-to-end (approximation) repair | Direct apposition of sphincter ends — used when muscle ends are short or retracted |
Step 4 — Vaginal Wall, Perineal Body, and Perineal Skin
- Perineal body (central tendon) reconstructed with interrupted sutures
- Vaginal mucosa closed with continuous unlocked 2-0 or 3-0 Vicryl
- Perineal skin — subcuticular suture preferred (less pain, fewer suture removal issues)
Postoperative Management (RCOG / ACOG / SOGC)
| Measure | Detail |
|---|---|
| Antibiotics | Single-dose IV cefuroxime + metronidazole intraoperatively (or oral prophylaxis for 5–7 days) — reduces wound infection and breakdown |
| Laxatives | Lactulose or Movicol (macrogol) — start immediately postoperatively; prevents constipation and straining at stool; continue for 10–14 days |
| Avoid enemas/suppositories acutely | Risk of disrupting repair |
| Analgesia | Regular NSAIDs + paracetamol; avoid constipating opioids where possible |
| Urinary catheter | Leave for minimum 24–48 hours (some centres 5 days) |
| Pelvic floor physiotherapy | Referral before discharge; commence pelvic floor exercises at 6 weeks |
| Follow-up | Clinic review at 6–12 weeks; assess wound healing, continence symptoms, sexual function |
| Endoanal ultrasound + anorectal manometry | If continence symptoms at follow-up — refer to urogynaecologist or colorectal surgeon |
Counselling for Future Pregnancies
- Women with previous OASIS should be counselled about mode of delivery
- Documented discussion in notes required (RCOG)
- Factors favouring elective caesarean section: persistent incontinence, manometry/USS defect, poor repair, patient preference
- No consensus on routine caesarean — individualise
B. AAST Grade IV Vaginal Laceration (Coital/Traumatic — into Cervix or Peritoneum)
Immediate Management
- Resuscitation first — IV access × 2, blood products, crossmatch, correct coagulopathy
- Examination under anaesthesia (EUA) in theatre — essential for adequate assessment
- Speculum examination — delineate extent; identify active bleeders
- Assess for peritoneal entry — if posterior fornix laceration extends into pouch of Douglas:
- Laparotomy / laparoscopy required to exclude visceral injury (bowel, bladder), haemoperitoneum, and to repair peritoneal defect
- Vaginal repair — layered closure:
- Deep layers: interrupted 0 Vicryl or PDS to achieve haemostasis
- Vaginal mucosa: continuous 2-0 Vicryl
- Haemostasis adjuncts if needed:
- Vaginal packing (temporary tamponade)
- Uterine/internal iliac artery embolisation (interventional radiology) for uncontrolled haemorrhage
- Internal iliac artery ligation (surgical last resort)
- Antibiotics — broad-spectrum cover (e.g., co-amoxiclav or cephalosporin + metronidazole)
- If vault dehiscence (post-hysterectomy) with eviseration — urgent laparotomy, reduce and repair vault with interrupted non-absorbable sutures
Key Points
- Diverting colostomy indicated if rectal injury accompanies vaginal injury — to protect repair and prevent faecal contamination (Schwartz's Principles of Surgery)
- Delayed repair (48–72 h) acceptable in haemodynamically unstable patients — damage control → stabilise → definitive repair
Explain the below with every possible outcomes and prognosis. AAST Grade IV Vaginal Laceration (Coital/Traumatic — into Cervix or Peritoneum) This is a surgical emergency and differs fundamentally from obstetric tears. Immediate Management Resuscitation first — IV access × 2, blood products, crossmatch, correct coagulopathy Examination under anaesthesia (EUA) in theatre — essential for adequate assessment. Speculum examination — delineate extent; identify active bleeders Assess for peritoneal entry — if posterior fornix laceration extends into pouch of Douglas: Laparotomy / laparoscopy required to exclude visceral injury (bowel, bladder), haemoperitoneum, and to repair peritoneal defect. Vaginal repair — layered closure: Deep layers: interrupted 0 Vicryl or PDS to achieve haemostasis Vaginal mucosa: continuous 2-0 Vicryl Haemostasis adjuncts if needed: Vaginal packing (temporary tamponade) Uterine/internal iliac artery embolisation (interventional radiology) for uncontrolled haemorrhage. Internal iliac artery ligation (surgical last resort)
coital vaginal laceration outcomes complications prognosis
vaginal laceration sexual intercourse treatment outcome
pelvic haemorrhage internal iliac ligation embolisation outcome
AAST Grade IV Vaginal Laceration (Coital/Traumatic) — Full Outcomes & Prognosis
Overview of the Clinical Spectrum
- Haemorrhagic shock from arterial/venous pelvic bleeding
- Haemoperitoneum or pneumoperitoneum from peritoneal breach
- Potential visceral injury to bowel, bladder, or ureter
Stage 1 — Resuscitation
What Is Done
- IV access × 2 (large bore, antecubital)
- Blood products: packed red cells, fresh frozen plasma (FFP), platelets in 1:1:1 ratio (massive transfusion protocol)
- Crossmatch, FBC, coagulation screen, U&E, LFTs, group & save
- Correct coagulopathy — FFP, cryoprecipitate, TXA (tranexamic acid) if within 3 hours of injury
- Urinary catheter — monitor output (target >0.5 mL/kg/hr)
Possible Outcomes at This Stage
| Scenario | Outcome |
|---|---|
| Prompt resuscitation, haemodynamically stable | Patient proceeds safely to EUA; optimal surgical outcome likely |
| Delayed presentation (>2–4 hours) | Progressive coagulopathy, hypothermia, acidosis — lethal triad of trauma |
| Failure to achieve haemostasis with resuscitation alone | Requires damage control surgery — morbidity rises significantly |
| Massive transfusion (>10 units pRBC in 24h) | Risk of transfusion-related acute lung injury (TRALI), TACO (transfusion-associated circulatory overload), hyperkalaemia, hypocalcaemia, dilutional coagulopathy |
| TXA given within 3 hours | Reduces mortality from haemorrhage by ~15% (CRASH-2 trial data) |
| Irreversible haemorrhagic shock before theatre | Cardiac arrest, death — rare if hospital reached promptly |
Prognostic Determinants
- Systolic BP on arrival: <70 mmHg = high-risk; >90 mmHg = favourable
- Lactate / base excess: lactate >4 mmol/L or BE worse than –6 = severe shock
- Time from injury to theatre: the single most important factor
Stage 2 — Examination Under Anaesthesia (EUA)
What Is Done
- Lithotomy position, good lighting, theatre environment
- Speculum examination with suction to delineate the full extent of the laceration
- Assessment of: depth, direction (anterior/posterior/lateral), involvement of fornix, cervix, vault
Possible Outcomes at This Stage
| Finding | Implication |
|---|---|
| Isolated deep vaginal laceration (no peritoneal breach) | Can be repaired vaginally — excellent prognosis |
| Posterior fornix laceration extending into pouch of Douglas | Peritoneal entry confirmed — laparoscopy/laparotomy mandatory |
| Active arterial spurting vessel identified | Suture ligation or diathermy at EUA — may resolve haemorrhage completely |
| Haematoma in broad ligament / paravaginal space | Risk of expansion and late haemorrhage; may need drainage and packing |
| Cervical laceration (lateral fornix) | Proximity to uterine artery at 3/9 o'clock — high-volume arterial bleeding likely |
| EUA inadequate (obese patient, uncooperative, poor view) | Underestimation of injury — risk of missed peritoneal entry or visceral damage |
Stage 3 — Vaginal Repair (Layered Closure)
What Is Done
- Deep layers: interrupted 0 Vicryl/PDS — achieves haemostasis, obliterates dead space
- Vaginal mucosa: continuous 2-0 Vicryl — restores epithelial integrity
Possible Outcomes
Favourable
- Complete haemostasis — bleeding stops; no further intervention needed
- Normal healing over 4–6 weeks; full mucosal re-epithelialisation
- Return to sexual function in 6–8 weeks if repair uncomplicated
Complications of Vaginal Repair
| Complication | Timeframe | Details |
|---|---|---|
| Wound breakdown / dehiscence | Days 3–7 | Infection, poor tissue quality, tension on sutures; more common in atrophic/post-radiation tissue |
| Haematoma formation | Hours to days | Dead space not adequately closed; may expand and become infected; requires drainage |
| Infection / abscess | Days 5–14 | Bacterial contamination especially if bowel injured; presents as fever, purulent discharge, pelvic pain |
| Rectovaginal fistula | Weeks to months | If rectal wall involved but not recognised; presents as passing flatus/stool PV; requires staged surgical repair |
| Vesicovaginal fistula | Weeks | If bladder involved or suture placed through bladder; presents as continuous urinary incontinence |
| Vaginal stenosis | Months | Excessive fibrosis/scarring, especially if large area of mucosa lost; causes dyspareunia and difficulty with intercourse |
| Dyspareunia (painful intercourse) | Weeks to permanent | Scar tissue at repair site; more common with posterior fornix involvement; may require vaginal dilators or surgical revision |
| Psychological sequelae | Immediate to long-term | PTSD, sexual aversion, relationship difficulties — especially after assault; requires psychological support |
Long-term Prognosis of Uncomplicated Repair
- Good to excellent in young, otherwise healthy women
- Atrophic/postmenopausal tissue: higher complication rate — topical oestrogen aids healing pre- and post-operatively
- Post-hysterectomy vault: vault dehiscence repairs have higher re-dehiscence risk (~5–10%)
Stage 4 — Laparotomy / Laparoscopy for Peritoneal Entry
What Is Found and What Happens
A. Haemoperitoneum Without Visceral Injury
- Peritoneal cavity irrigated, bleeding source identified and controlled
- Peritoneal defect repaired (vaginal wall sutured from above if needed)
- Prognosis: Excellent if haemostasis achieved and no visceral injury
B. Small Bowel Injury
- Most common visceral injury in posterior fornix perforation (small bowel lies in the pouch of Douglas)
- Primary repair if clean laceration, minimal contamination, healthy bowel
- Resection + anastomosis if devascularised segment or large injury
- Diverting ileostomy if contamination heavy, patient unstable, or immunocompromised
- Risk of: anastomotic leak (3–8%), intra-abdominal abscess, ileus, adhesions, future bowel obstruction
- Systematic review (Stabile et al., 2021, PMID 34574671): in 16 cases of postcoital vaginal perforation with evisceration (1980–2020) in women with no prior surgery, all occurred at the posterior fornix; majority required laparotomy; no mortality reported in cases reaching surgical care — confirming that prompt diagnosis is the key determinant of survival
C. Rectal / Sigmoid Injury
- Requires diverting colostomy (Hartmann's procedure or loop colostomy) + distal washout
- Definitive rectal repair delayed until infection controlled
- Colostomy reversal 3–6 months later (second surgery)
- Risk of: anastomotic leak, wound infection, colostomy complications, adhesions
- Prognosis: Guarded — longer hospital stay, two-stage surgery, colostomy-related morbidity
D. Bladder Injury
- Primary repair in two layers (mucosa + seromuscular)
- Urinary catheter drainage for 7–14 days
- Risk of: vesicovaginal fistula (1–3%), urinary infection, urethral stricture
- Prognosis: Good with prompt repair
E. Ureteric Injury
- Rare; occurs with lateral fornix/parametrial extension
- Requires urological expertise: ureteric stenting or ureteroneocystostomy
- Missed injury → urinoma, hydronephrosis, renal impairment
- Prognosis: Good if identified intraoperatively; Poor if delayed >72h (stricture, loss of renal function)
F. Evisceration (Bowel Prolapsing Through Vaginal Defect)
- Dramatic presentation; bowel is usually viable if no prolonged exposure
- Reduction + vaginal/peritoneal repair ± bowel resection
- Prognosis: Good if bowel viable (no ischaemia); mortality approaches 0% in reported surgical cases
Stage 5 — Haemostasis Adjuncts
A. Vaginal Packing (Tamponade)
| Outcome | Details |
|---|---|
| Successful tamponade | Buys time for resuscitation and definitive repair; removed after 24–48 hours |
| Failure | Bleeding continues around pack; must escalate to embolisation or ligation |
| Complication | Retained pack (must document and remove at set time); pressure necrosis of vaginal epithelium with prolonged packing |
B. Uterine / Internal Iliac Artery Embolisation (UAE/IAE)
| Outcome | Rate / Details |
|---|---|
| Technical success (angiographic occlusion) | 85–95% |
| Clinical success (haemostasis achieved, surgery avoided) | 70–90% |
| Failure requiring surgery | 10–20%; escalate to ligation or hysterectomy |
| Recurrent haemorrhage | 5–10%; can re-embolise |
| Uterine ischaemia / necrosis | Rare (<1%); presents as sepsis, pain, foul discharge |
| Fertility preservation | UAE largely preserves fertility — menstruation typically resumes in 3–6 months; successful subsequent pregnancies documented |
| Ovarian failure | Rare (<5%) if non-target embolisation of ovarian artery |
| Post-embolisation syndrome | Fever, pain, leukocytosis in 30–50%; self-limiting, managed conservatively |
| Contrast nephropathy | 1–5%; risk higher in pre-existing renal impairment |
| Access site haematoma | 2–5% at femoral puncture site |
C. Internal Iliac (Hypogastric) Artery Ligation — Surgical Last Resort
| Outcome | Rate / Details |
|---|---|
| Haemostasis success rate | 40–75% (less reliable than embolisation in trauma) |
| Failure requiring hysterectomy | 25–50% if ligation alone insufficient |
| Uterine / pelvic organ necrosis | Rare — rich collateral circulation protects |
| Buttock claudication | Rare; due to reduced gluteal artery perfusion |
| Bladder / ureter injury (during ligation) | 1–3%; dissection near ureter and bladder at pelvic sidewall |
| Nerve injury | Obturator or lumbosacral nerve injury possible |
| Fertility | Reduced compared to UAE — subsequent pregnancies less likely; uterine blood flow permanently reduced |
| Future embolisation possible | Yes — ligation does not preclude subsequent radiological intervention |
Stage 6 — If All Else Fails: Hysterectomy
- Emergency hysterectomy (total or subtotal) is life-saving
- Prognosis: Life-saving but permanent loss of fertility
- Morbidity: haemorrhage, adjacent organ injury, adhesions
- Psychological impact of infertility — especially in young nulliparous patients; requires counselling
Overall Prognosis Summary
| Scenario | Prognosis |
|---|---|
| Isolated deep vaginal laceration, no peritoneal entry, haemostasis at EUA | Excellent — near-complete recovery |
| Peritoneal entry, small bowel injury, repaired within hours | Very good — mortality near zero with surgical care |
| Posterior fornix perforation with evisceration, bowel viable | Good — all 16 literature cases survived with surgery (Stabile et al., 2021) |
| Rectal injury requiring colostomy | Good but prolonged — 2-stage surgery, months of recovery |
| Bladder injury, repaired promptly | Good — low fistula risk |
| Ureteric injury, missed >72h | Guarded — risk of renal function loss |
| Massive haemorrhage, UAE/ligation successful | Good — fertility potentially preserved with UAE |
| Uncontrolled haemorrhage requiring hysterectomy | Survival good; permanent fertility loss |
| Delayed presentation (>6–12 hours) with peritonitis | Guarded to poor — septic shock, multi-organ dysfunction, ICU admission |
| Haemorrhagic shock with cardiac arrest before theatre | Poor — mortality high |
Key Prognostic Message
"Post-coital vaginal perforation and evisceration… is usually not a life-threatening condition, but a delay in diagnosis can lead to severe complications." — Stabile et al., 2021 (Systematic Review, PMID 34574671)