Payhogenesis of HTN
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
pathogenesis hypertension RAAS renin angiotensin sympathetic nervous system mechanism diagram
I have comprehensive content now. Let me compile the full answer.
Pathogenesis of Hypertension
Blood pressure (BP) = Cardiac Output (CO) × Systemic Vascular Resistance (SVR). Sustained hypertension arises when either — or both — are chronically elevated. Primary (essential) hypertension accounts for 90–95% of all cases and results from a complex interplay of genetic susceptibility and environmental factors; the remaining 5–10% are secondary to identifiable causes.
1. Fundamental Haemodynamic Framework
| Phase | Mechanism | Predominant Change |
|---|---|---|
| Early (young adults) | Sympathetic overactivity → ↑ CO | ↑ Cardiac output, labile BP, ↑ HR |
| Established | Total-body autoregulation → vasoconstriction | ↑ SVR, normal CO |
| Late/Elderly | Arterial stiffness → faster pulse-wave return | Isolated systolic HTN |
Increased cardiac output does not persist: each organ's intrinsic autoregulation translates excess flow into vasoconstriction over 5–15 days ("total-body autoregulation"), converting the haemodynamic abnormality into a structurally sustained rise in SVR.
2. Renal Sodium Handling — The Central Defect
The kidney is the pivotal long-term regulator of BP via pressure natriuresis: a rise of as little as 1–3 mmHg in mean arterial pressure normally triggers a sharp increase in urinary NaCl excretion, correcting volume and BP.
In hypertension this curve is reset/shifted rightward:
- The kidney retains more sodium at any given perfusion pressure
- Obligatory fluid retention → ↑ ECF volume → ↑ blood volume → ↑ CO → ↑ BP
- Eventually a new steady state is reached, but only at a higher BP
Two mechanisms of pressure natriuresis are impaired:
- Medullary pressure-flow pathway: ↑ perfusion pressure → ↑ medullary blood flow → ↑ interstitial hydrostatic pressure → ↓ proximal tubule reabsorption. Blunted in HTN.
- RAAS suppression: ↑ BP should suppress renin from the juxtaglomerular apparatus → ↓ Ang II → ↓ Na⁺ reabsorption. A normal or elevated PRA in a hypertensive patient is therefore "inappropriately" high and perpetuates the disorder.
Salt sensitivity (present in ~30% of normotensives, ~60% of hypertensives) is especially common in Black individuals, the elderly, and those with CKD. It correlates with low plasma renin activity.
3. Renin–Angiotensin–Aldosterone System (RAAS)
The RAAS is the master regulator of salt/volume homeostasis:
Renin (JGA) → cleaves Angiotensinogen → Angiotensin I
ACE (lung/endothelium) → Angiotensin II
Angiotensin II actions that raise BP:
- Potent vasoconstriction (AT₁ receptor → SVR ↑)
- Stimulates aldosterone → ENaC activation → Na⁺/water retention in collecting duct
- Stimulates ADH (vasopressin) release → water reabsorption
- Inhibits ANP → blunts natriuresis
- Stimulates thirst
- Promotes vascular smooth muscle cell (SMC) hypertrophy and fibrosis
Genetic polymorphisms in angiotensinogen, ACE, and AT₁ receptor genes contribute to interindividual variation in BP and population-level differences (e.g., lower-renin hypertension in Black individuals).
4. Sympathetic Nervous System (SNS)
- Many hypertensive patients show elevated plasma catecholamines, increased sympathetic nerve discharge, and elevated heart rate — despite the stimulus that should suppress sympathetic tone
- Baroreflex resetting: after 2–5 days of elevated BP, baroreceptors adapt to the new set-point and defend the higher BP rather than correcting it
- With aging and atherosclerosis, carotid sinus walls stiffen → reduced baroreceptor stretch sensitivity → further SNS over-activation
- SNS activation increases: CO (via ↑ HR, ↑ contractility), SVR (vasoconstriction), and renal Na⁺ retention (via direct tubular effects + renin release)
5. Endothelial Dysfunction and Vasomotor Imbalance
A balance between vasodilators and vasoconstrictors normally maintains vascular tone:
| Vasodilators | Vasoconstrictors |
|---|---|
| Nitric oxide (NO) | Angiotensin II |
| Prostacyclin (PGI₂) | Endothelin-1 (ET-1) |
| Bradykinin | Thromboxane A₂ |
| ANP/BNP | ROS-generated isoprostanes |
In hypertension:
- Nitric oxide (NO) synthesis (via eNOS) is reduced → loss of vasodilation + reduced renal Na⁺ excretion
- Reactive oxygen species (ROS), particularly superoxide (O₂⁻), scavenge NO, forming peroxynitrite (ONOO⁻) → oxidative stress → vasoconstriction, salt retention, platelet aggregation, LDL oxidation → accelerated atherosclerosis
- Endothelin-1 released by endothelial cells acts on ETA receptors → vasoconstriction; potentiates Ang II-mediated vasoconstriction
- NADPH oxidase–derived ROS are amplified by Ang II, further coupling the RAAS to endothelial dysfunction
6. Vascular Remodeling — Structural Perpetuation
Chronic vasoconstriction induces irreversible structural changes:
- Wall hypertrophy of resistance arterioles → fixed reduction in lumen-to-wall ratio → permanently elevated SVR
- Enhanced vascular reactivity: thickened walls produce greater luminal narrowing for any given vasoconstrictor stimulus
- Microvascular rarefaction: loss of arterioles and capillaries reduces the cross-sectional area available for flow
- Impaired myogenic response: blunts autoregulation of renal blood flow → barotrauma to glomeruli
- These changes blunt pressure natriuresis (juxtaglomerular apparatus hypertrophies → renin sensing impaired) → salt sensitivity worsens → hypertension self-perpetuates
This explains why antihypertensive therapy often takes weeks to reach maximal effect, and why vascular hypertrophy is only partially reversible.
7. Genetic Factors
- Familial clustering and twin studies confirm a strong heritable component (estimated heritability ~30–60%)
- Most causative alleles are polygenic and small-effect (GWAS identifies >1000 loci)
- Known candidates: angiotensinogen gene variants, AT₁R polymorphisms, ENaC subunit mutations (Liddle syndrome — rare monogenic form), aldosterone synthase
- Monogenic forms (e.g., Liddle, Gordon, glucocorticoid-remediable aldosteronism) provide proof-of-concept for specific pathway derangements
8. Environmental / Modifiable Factors
| Factor | Mechanism |
|---|---|
| High dietary sodium | Overwhelms pressure natriuresis in salt-sensitive individuals |
| Obesity | Adipose-derived Ang II, leptin → SNS activation, insulin resistance → Na⁺ retention |
| Physical inactivity | Reduced vascular compliance, SNS over-activity |
| Smoking | ROS generation, endothelial injury, vasoconstriction |
| Chronic stress | Sustained SNS activation, cortisol |
| Alcohol excess | SNS activation, renin release |
9. Vascular Pathology (End-Organ Consequence)
| Lesion | Setting | Mechanism |
|---|---|---|
| Hyaline arteriolosclerosis | Benign/primary HTN | Plasma leakage across injured endothelium; SMC ECM deposition; → nephrosclerosis |
| Hyperplastic arteriolosclerosis | Malignant HTN (DBP >120 mmHg) | "Onion-skin" laminated SMC proliferation; fibrinoid necrosis → acute ischemia |
Integrated Pathogenetic Model
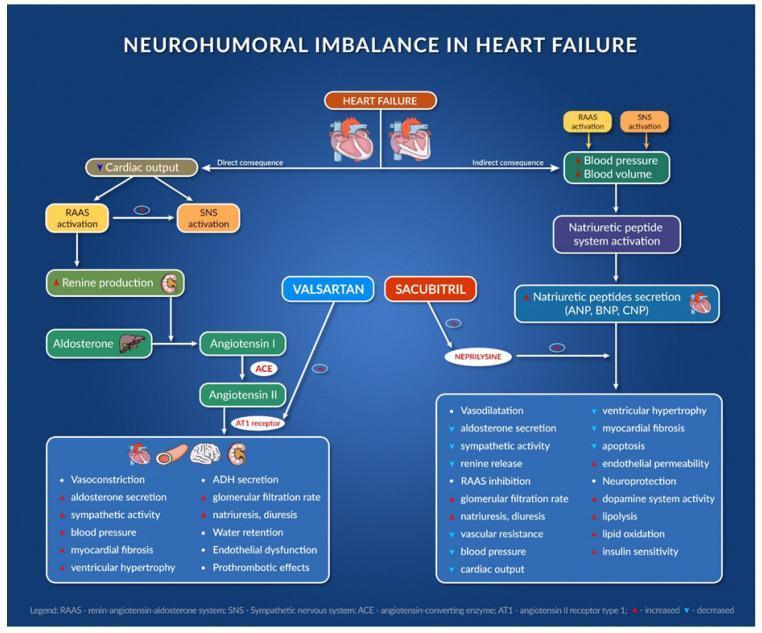
The pathogenesis can be synthesized as a self-reinforcing cycle:
Genetic predisposition + environmental triggers → impaired renal sodium handling → ↑ volume/CO → baroreceptor resetting → inappropriate SNS & RAAS activation → endothelial dysfunction + ↓ NO → vasoconstriction → ↑ SVR → vascular remodeling → structural HTN → further impairment of pressure natriuresis → cycle perpetuates
Sources:
- Robbins & Kumar Basic Pathology, Pathogenesis of Primary Hypertension, p. 278–311
- National Kidney Foundation Primer on Kidney Diseases, 8e, Pathophysiology of Hypertension, Ch. 63
This is a shared conversation. Sign in to Orris to start your own chat.