Cutaneous tb Full details for md exam
Reading File
search_medical_text
cutaneous tuberculosis classification types lupus vulgaris scrofuloderma
search_medical_text
cutaneous tuberculosis pathogenesis clinical features diagnosis histopathology
search_medical_image
cutaneous tuberculosis lupus vulgaris scrofuloderma skin lesion
GradeResponse
GradeResponse
GradeResponse
search_medical_text
tuberculids erythema induratum lichen scrofulosorum papulonecrotic treatment antitubercular
I have sufficient retrieved content and my own knowledge to deliver a comprehensive MD-exam level answer. Here is the full coverage:
Cutaneous Tuberculosis (Cutaneous TB) — Complete MD Exam Notes
1. Introduction
Cutaneous tuberculosis (CTB) refers to skin lesions caused by Mycobacterium tuberculosis, M. bovis, or the BCG bacillus. It accounts for ~1–2% of all TB cases and ~2% of all dermatological conditions in endemic regions. The skin may be infected via exogenous inoculation, endogenous spread (hematogenous, lymphatic, contiguous), or hypersensitivity reactions (tuberculids).
2. Pathogen
- Mycobacterium tuberculosis — aerobic, acid-fast bacillus (AFB)
- M. bovis — from infected animals/unpasteurized milk
- BCG strain — following BCG vaccination (rare, mostly in immunocompromised)
3. Pathogenesis / Routes of Infection
| Route | Type |
|---|---|
| Exogenous inoculation | Primary inoculation TB, Tuberculosis verrucosa cutis |
| Endogenous — hematogenous | Lupus vulgaris, Acute miliary TB, Metastatic tuberculous abscess |
| Endogenous — direct/lymphatic extension | Scrofuloderma, Orificial TB |
| Immunological reaction (tuberculids) | Lichen scrofulosorum, Papulonecrotic tuberculid, Erythema induratum of Bazin |
4. Classification
A. TRUE CUTANEOUS TB (Organisms Present in Skin)
1. Primary Inoculation Tuberculosis (Tuberculous Chancre)
- Occurs in: Previously uninfected individuals (primary infection)
- Route: Direct inoculation (cuts, abrasions — laboratory workers, pathologists, medical personnel)
- Features:
- Chancre: Painless, indurated papule → ulcer at inoculation site (face, hands, feet)
- After 3–8 weeks: Regional lymphadenopathy ("Primary complex" = chancre + lymphadenopathy)
- Heals spontaneously in most, may disseminate
- Histology: Initially non-specific inflammation → later caseating granulomas
- AFB: Sometimes positive in lesion, usually positive in nodes
2. Tuberculosis Verrucosa Cutis (Warty TB)
- Occurs in: Previously sensitized individuals (re-infection)
- Route: Exogenous inoculation
- At risk: Pathologists, butchers, laboratory workers, children (playing barefoot in endemic areas)
- Features:
- Begins as small, painless, hyperkeratotic papule
- Evolves into verrucous (warty), irregular plaque with a "pebbly" or papillomatous surface
- Site: dorsum of hands, fingers, feet, ankles
- No lymphadenopathy (sensitized host)
- Indolent; may persist for years
- Old names: Prosector's wart, Butcher's wart, Anatomist's wart
- Histology: Pseudoepitheliomatous hyperplasia, caseating granulomas in dermis, AFB rare
- Mantoux: Strongly positive
3. Lupus Vulgaris
- Most common form of CTB in India
- Occurs in: Previously sensitized, high-immunity individuals
- Route: Hematogenous spread; also direct extension from lymph nodes/bones; or post-primary inoculation
- Features:
- Most commonly on head and neck (nose, cheek — "butterfly" distribution), also extremities
- Begins as soft, reddish-brown papules → coalesce into plaques
- Pathognomonic sign — Apple-jelly (Lupoid) nodules: Yellowish-brown translucent nodules visible on diascopy (pressing glass slide on skin)
- Central scarring with active spreading periphery
- Active edge + healing periphery can coexist (see image below)
- Slow, relentlessly progressive — can persist for decades
- Complications: Destruction of nasal cartilage, ectropion; squamous cell carcinoma can develop in scars (Marjolin's ulcer)
- Histology: Non-caseating or minimally caseating tuberculoid granulomas; Langerhans giant cells; AFB very rare
- Mantoux: Strongly positive
According to Harrison's Principles of Internal Medicine, 21st Ed. (p. 1605): "Lesions occur primarily in the head and neck region and are red-brown plaques with a yellow-brown color on diascopy. Secondary scarring can develop within the central portion of the plaques. Cultures or PCR analysis of the lesions should be performed, along with an interferon γ release assay of peripheral blood, because it is rare for the acid-fast stain to show bacilli within the dermal granulomas."
Clinical photograph — Lupus Vulgaris:
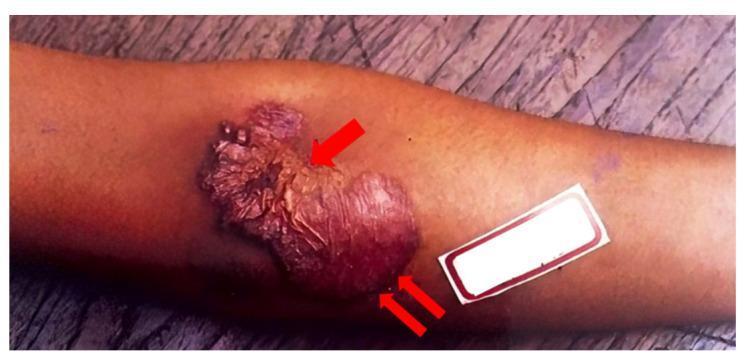
4. Scrofuloderma
- Occurs in: Children and young adults
- Route: Contiguous spread from underlying infected lymph node (cervical most common), bone, or joint
- Features:
- Initially: Firm, painless, non-tender subcutaneous nodule overlying infected node (usually cervical, axillary, or inguinal)
- Nodule softens → skin becomes bluish-red, adherent, fluctuant
- Breaks down to form irregular ulcers with undermined, "collar-stud" edges, and sinuses discharging watery pus/caseous material
- Heals with cord-like, bridge scars (pathognomonic)
- Histology: Caseating necrosis, granulomas; AFB often found
- Mantoux: Usually positive
- DDx: Actinomycosis, atypical mycobacteriosis, syphilitic gumma, hidradenitis suppurativa
5. Orificial Tuberculosis (Tuberculosis Cutis Orificialis)
- Rarest and most severe form
- Occurs in: Severely immunocompromised with advanced internal TB
- Route: Autoinoculation — organisms from internal lesions (pulmonary, GI, genitourinary TB) shed into body orifices
- Features:
- Sites: Around oral cavity (tongue, soft palate — from pulmonary TB), perianal region (from GI/GU TB), genitalia
- Painful, punched-out ulcers with undermined edges, yellowish base; may have "soft palate perforations"
- Poor prognosis; indicates terminal disease
- Histology: Caseating granulomas; AFB readily found
- Mantoux: May be negative (anergy due to severe immunosuppression)
6. Acute Miliary Tuberculosis Cutis
- Occurs in: Severely immunocompromised (infants, HIV, post-measles)
- Route: Hematogenous dissemination from primary focus
- Features: Multiple tiny papules, vesicles, or pustules — widespread over trunk; poor prognosis
- Histology: Non-specific initially; AFB may be found; granulomas form later
7. Metastatic Tuberculous Abscess (Tuberculous Gumma)
- Occurs in: Immunocompromised (poor host immunity)
- Route: Hematogenous spread from primary focus (often during latent TB reactivation)
- Features:
- Cold, painless, fluctuant subcutaneous abscess without signs of acute inflammation
- "Cold abscess" — may be single or multiple
- Spontaneously ruptures → sinus formation
- Sites: Trunk, extremities
- AFB: Usually found in aspirate
B. TUBERCULIDS (Immunological / Hypersensitivity Reactions)
Tuberculids are hypersensitivity reactions to M. tuberculosis antigens in a host with high immunity but no organisms in the skin. AFB are absent (or very rarely found by PCR). They resolve with anti-TB treatment.
1. Lichen Scrofulosorum
- Most common tuberculid
- Age: Children and adolescents
- Features:
- Asymptomatic, lichenoid, minute (1–3 mm) perifollicular or periductal papules
- Grouped in discoid or annular plaques
- Sites: Trunk (especially chest, abdomen)
- Spontaneously resolves
- Histology: Superficial perifollicular/periductal granulomas; no caseation; no AFB
- Mantoux: Strongly positive
- Association: Usually with underlying lymph node or bone TB
2. Papulonecrotic Tuberculid
- Features:
- Recurrent, symmetrical, necrotic papules and pustules
- Heal with depressed, "punched-out" scars
- Sites: Extensor surfaces of extremities (elbows, knees, buttocks)
- Histology: Obliterative vasculitis, wedge-shaped necrosis; no AFB
- Mantoux: Positive
- DDx: Pityriasis lichenoides, leukocytoclastic vasculitis
3. Erythema Induratum of Bazin
- Features:
- Recurrent, tender, indurated erythematous nodules and plaques
- Ulcerate and leave atrophic scars
- Sites: Posterior calves (calves of legs — "stockings area")
- Predominantly in middle-aged women
- Associated with cold weather (cold panniculitis)
- Pathology: Lobular panniculitis with vasculitis and granulomas
- Note: When no TB link found → called "Nodular vasculitis"
- Mantoux: Positive; MTB-PCR may be positive in lesion
4. Rosai-Dorfman Disease (associated in some classifications)
(Less commonly listed but some classify here)
5. Summary Comparison Table
| Feature | Primary Inoculation TB | TB Verrucosa Cutis | Lupus Vulgaris | Scrofuloderma | Orificial TB | Tuberculids |
|---|---|---|---|---|---|---|
| Immunity | None (primary) | Sensitized (high) | Sensitized (high) | Variable | Low | Very high |
| AFB in skin | +/- | Rare | Very rare | Often + | Readily + | Absent |
| Route | Exogenous | Exogenous | Hematogenous | Contiguous | Autoinoculation | Hypersensitivity |
| Mantoux | + (late) | ++ | ++ | + | -/+ | +++ |
| Key feature | Chancre + LAP | Warty plaque | Apple-jelly nodules | Cold abscess + bridge scars | Painful ulcers at orifices | Sterile; respond to ATT |
6. Diagnosis
A. Clinical
- Site, morphology, epidemiology, contact history, BCG scar
B. Mantoux (Tuberculin Skin Test)
- Positive in most forms (strongly positive in tuberculids, lupus vulgaris, TB verrucosa)
- Negative (anergy) in orificial TB and miliary TB (immunocompromised)
C. Laboratory
| Test | Details |
|---|---|
| AFB smear | Low sensitivity in CTB (bacilli sparse) |
| Culture (Lowenstein-Jensen medium) | Gold standard — 6–8 weeks; low yield in paucibacillary forms |
| Histopathology | Caseating/non-caseating epithelioid granulomas with Langerhans giant cells (Bailey & Love, 28th Ed., p. 619) |
| PCR (IS6110 gene) | Rapid, sensitive; best for paucibacillary forms (lupus vulgaris, tuberculids) |
| IGRA (Interferon-γ Release Assay) | QuantiFERON-TB Gold / T-SPOT; confirms sensitization; unaffected by BCG |
| CBC, ESR | Non-specific; elevated ESR |
| Chest X-ray | Detect underlying pulmonary TB |
Harrison's (p. 1605): "Cultures or PCR analysis of the lesions should be performed, along with an interferon γ release assay of peripheral blood."
D. Histopathology (Key for Exam)
- Caseating granuloma: Epithelioid cells + Langerhans giant cells + lymphocytes surrounding central caseous necrosis
- Non-caseating granuloma: Seen in lupus vulgaris, tuberculids (high immunity)
- "Apple-jelly" correlate: Tuberculoid granulomas in upper dermis
7. Differential Diagnosis
| CTB Type | Key DDx |
|---|---|
| Lupus vulgaris | Sarcoidosis, lupus erythematosus, leishmaniasis, leprosy |
| TB verrucosa cutis | Verruca vulgaris, chromoblastomycosis, blastomycosis |
| Scrofuloderma | Actinomycosis, syphilitic gumma, hidradenitis suppurativa |
| Erythema induratum | Nodular vasculitis, erythema nodosum, polyarteritis nodosa |
| Orificial TB | Aphthous ulcers, Crohn's disease, SCC |
8. Treatment
Anti-Tubercular Therapy (ATT)
Standard regimen (same as pulmonary TB):
| Phase | Duration | Drugs |
|---|---|---|
| Intensive phase | 2 months | Isoniazid (H) + Rifampicin (R) + Pyrazinamide (Z) + Ethambutol (E) → 2HRZE |
| Continuation phase | 4 months | Isoniazid (H) + Rifampicin (R) → 4HR |
| Total | 6 months |
- In lupus vulgaris and severe/extensive disease: may extend continuation phase to 7 months (total 9 months)
- Tuberculids: Usually respond to 6-month regimen
Adjunctive / Surgical
- Surgical excision for localized TB verrucosa cutis (small lesions)
- Drainage for cold abscesses (scrofuloderma, tuberculous gumma)
- Reconstructive surgery for disfiguring scars (post-treatment)
Monitoring
- Clinical response in 4–8 weeks
- LFTs at baseline and monthly (rifampicin/INH hepatotoxicity)
- Visual acuity/color vision (ethambutol — optic neuritis)
9. Complications
| Complication | Form |
|---|---|
| Squamous cell carcinoma | Lupus vulgaris (Marjolin's ulcer) |
| Destruction of nasal cartilage, ectropion | Lupus vulgaris |
| Disfiguring bridge-like scars | Scrofuloderma |
| Drug resistance | MDR-TB (if irregular treatment) |
10. High-Yield Points for MD Exam
- Most common CTB in India = Lupus vulgaris
- Pathognomonic sign of LV = Apple-jelly nodules on diascopy
- Warty TB = TB verrucosa cutis (prosector's wart — occurs in sensitized)
- Bridge-like/cord scars = Scrofuloderma
- Mantoux negative in CTB = Orificial TB (anergy), Miliary TB
- No organisms in skin = Tuberculids
- Most severe form = Orificial TB (terminal disease)
- Cold abscess = Scrofuloderma or Tuberculous gumma
- Posterior calf ulcerating nodules in women = Erythema induratum of Bazin
- PCR target gene = IS6110 of M. tuberculosis
- Gold standard culture medium = Lowenstein-Jensen (L-J) medium
- Complication of LV = SCC in scar
- Treatment = 2HRZE + 4HR (6 months total)
- IGRA not affected by BCG vaccination (unlike Mantoux)
Sources: Harrison's Principles of Internal Medicine, 21st Ed. (p. 1605); Bailey & Love's Short Practice of Surgery, 28th Ed. (p. 619); supplemented from standard dermatology references (Rook's Textbook of Dermatology, IADVL Textbook of Dermatology)
This is a shared conversation. Sign in to Orris to start your own chat.