Scrofuloderma full details for md exams
Reading File
search_medical_text
Scrofuloderma tuberculosis skin clinical features diagnosis treatment
search_medical_image
Scrofuloderma skin lesion tuberculosis cutaneous
GradeResponse
GradeResponse
Here is a comprehensive exam-oriented breakdown of Scrofuloderma for MD examinations:
Scrofuloderma
Definition
Scrofuloderma (also called tuberculosis colliquativa cutis) is a form of cutaneous tuberculosis (TB) caused by direct extension of a tuberculous focus in an underlying structure (lymph node, bone, joint, epididymis) to the overlying skin, resulting in cold abscess formation, ulceration, and sinus tract/fistula development.
Key High-Yield Points at a Glance
| Feature | Detail |
|---|---|
| Causative organism | Mycobacterium tuberculosis (occasionally M. bovis) |
| Type | True cutaneous TB (reactivation/direct extension) |
| Pathogenesis | Per continuitatem spread from underlying focus |
| Most common underlying focus | Cervical lymph nodes |
| Most common site | Neck / submandibular / parotid region |
| Tuberculin/Mantoux test | Strongly positive |
| Lepromin test | Negative |
| Histology | Caseating granuloma |
| Treatment | Standard anti-TB regimen (2HRZE + 4HR) |
Etiology & Pathogenesis
- Causative agent: Mycobacterium tuberculosis (acid-fast bacillus)
- Route: NOT from external inoculation. The bacilli spread per continuitatem (by direct continuity) from an underlying infected focus through the dermis to the skin surface
- Underlying foci (in order of frequency):
- Cervical lymph nodes (most common) — classical "scrofula"
- Parotid and submandibular lymph nodes
- Infected bones/joints (especially sternoclavicular, sternal)
- Epididymis, testis
- Lacrimal glands
- Salivary glands
Clinical Features
Sites
- Neck (most common — overlying cervical lymph nodes) — submandibular, parotid, supraclavicular regions
- Axilla, groin (overlying axillary/inguinal nodes)
- Chest wall (overlying infected ribs/sternum)
Stages of Lesion Progression
- Stage 1 — Subcutaneous nodule: Firm, painless, skin-colored or bluish subcutaneous nodule; overlying skin initially normal
- Stage 2 — Softening (fluctuant): Nodule becomes fluctuant (cold abscess) — no warmth, no redness = "cold abscess" (key exam point)
- Stage 3 — Ulceration: Skin breaks down → irregular, undermined, ragged, violaceous ulcer with bluish-red overhanging edges
- Stage 4 — Sinus/fistula formation: Multiple discharging sinuses and fistulous tracts with thin, seropurulent or caseous discharge
- Stage 5 — Healing: Characteristic cord-like, bridge scars (pathognomonic — "bridging scars" or papillomatous scarring)
Exam-Relevant Clinical Points
- Painless (unless secondary bacterial infection)
- Cold abscess (no signs of acute inflammation)
- Undermined/overhanging edges of ulcer
- Bluish-red to violaceous skin discoloration over the lesion
- Characteristic bridging/cord scars on healing — pathognomonic
- Associated systemic TB signs: fever, night sweats, weight loss, malaise
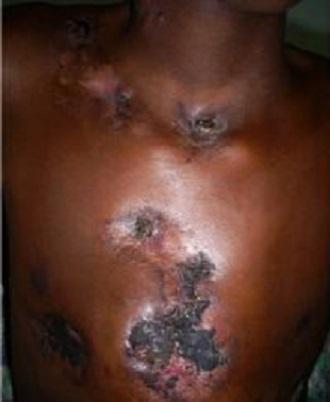
Classification of Cutaneous TB (Exam Context)
Scrofuloderma fits into this framework:
| Type | Pathogenesis | Example |
|---|---|---|
| Primary inoculation TB (chancre) | External inoculation, no prior immunity | Tuberculous chancre |
| Lupus vulgaris | Hematogenous/lymphatic spread | Most common cutaneous TB in India |
| Scrofuloderma | Direct extension from underlying focus | Cold abscess, sinus tracts |
| Warty TB (TB verrucosa cutis) | Exogenous re-inoculation, high immunity | Verrucous plaques on hands/feet |
| Miliary TB | Hematogenous spread (severe immunosuppression) | Disseminated papules |
| Tuberculids | Hypersensitivity reaction (not direct infection) | Erythema induratum, PNT |
Diagnosis
1. Mantoux (Tuberculin Skin Test / PPD)
- Strongly positive (>10 mm in immunocompetent; >5 mm in immunocompromised)
- High-grade immunity in scrofuloderma
2. Histopathology (Biopsy — Gold Standard for Morphology)
- Caseating epithelioid granulomas in the dermis
- Langhans giant cells surrounded by epithelioid histiocytes
- Central caseous necrosis
- Peripheral lymphocytic infiltrate
3. Microbiological Investigations
- Ziehl-Neelsen (ZN) stain: AFB (acid-fast bacilli) may be seen in discharge/biopsy — key exam point
- Culture on Lowenstein-Jensen (LJ) medium: Gold standard for confirmation; slow (6–8 weeks)
- CBNAAT/GeneXpert (Nucleic Acid Amplification Test): Rapid molecular diagnosis; also detects rifampicin resistance
4. IGRA (Interferon-Gamma Release Assay)
- QuantiFERON-TB Gold or T-SPOT.TB
- Positive; more specific than Mantoux (no false positives with BCG)
5. Imaging
- Chest X-ray: Look for pulmonary TB (primary focus)
- Ultrasound neck: Assess underlying lymph node involvement, matting, cold abscess
- CT scan: Defines extent of deep tissue involvement
Differential Diagnosis
| Condition | Differentiating Feature |
|---|---|
| Actinomycosis | Sulphur granules in discharge; jaw/neck; Gram+ filamentous organisms |
| Botryomycosis | Bacterial; Gram stain shows cocci/rods |
| Sporotrichosis | Lymphocutaneous pattern; fungal (Sporothrix schenckii) |
| Syphilitic gumma | Tertiary syphilis; VDRL/TPHA positive; non-caseating gumma |
| Hidradenitis suppurativa | Axilla/groin; recurrent abscesses; no TB |
| Atypical mycobacterial infection | Culture differentiates (M. avium, M. scrofulaceum) |
| Lymphoma with cutaneous involvement | Biopsy; lymph node histology |
Treatment
Anti-TB Regimen (Standard WHO/RNTCP/NTEP)
2HRZE / 4HR
| Phase | Duration | Drugs |
|---|---|---|
| Intensive phase | 2 months | Isoniazid (H) + Rifampicin (R) + Pyrazinamide (Z) + Ethambutol (E) |
| Continuation phase | 4 months | Isoniazid (H) + Rifampicin (R) |
- Total duration: 6 months for cutaneous TB (most forms)
- Some guidelines recommend 9 months if bone/joint involvement coexists
- Daily regimen preferred over intermittent (NTEP, India)
Adjunctive Measures
- Treat underlying focus (lymph node drainage if very large and tense; surgical excision rarely needed)
- Incision and drainage alone is contraindicated — risk of chronic sinus formation and spread
- Nutritional support, address HIV/immunosuppression
Monitoring
- Clinical response (healing of ulcers, closure of sinuses) expected within 2–3 months
- Liver function tests (HRZE are all hepatotoxic — especially INH, RIF, PZA)
- Ophthalmic review if on Ethambutol (ethambutol optic neuropathy)
Prognosis & Complications
- Good prognosis with complete anti-TB therapy
- Residual scarring is universal — characteristic cord/bridge scars
- Complications:
- Secondary bacterial infection
- Lymphedema from lymph node destruction
- Contractures due to extensive fibrosis
- Marjolin's ulcer (squamous cell carcinoma arising in chronic scrofuloderma scar — rare but important exam point)
High-Yield Mnemonics & Exam Traps
| Point | Details |
|---|---|
| "Scrofula" = cervical TB lymphadenitis | Scrofuloderma = when scrofula breaks through skin |
| Cold abscess | No heat/redness — classic for TB abscess |
| Bridging scars = pathognomonic | Ask in MCQs |
| ZN stain positive | Unlike lupus vulgaris (AFB rarely seen) — scrofuloderma has more bacilli |
| Do NOT I&D | Incision alone worsens disease |
| Marjolin's ulcer risk | In long-standing unhealed scrofuloderma |
| Most common cutaneous TB in India | Lupus vulgaris (not scrofuloderma) |
| Scrofuloderma vs. Lupus vulgaris | LV = hematogenous spread + apple jelly nodules on diascopy; Scrofuloderma = direct extension + cold abscess |
Summary Box (Quick Recall)
Scrofuloderma = Cutaneous TB caused by direct extension (per continuitatem) from underlying TB focus (most commonly cervical lymph nodes) → cold abscess → ulcer with undermined edges → discharging sinuses → heals with bridging cord scars (pathognomonic). Diagnosed by caseating granuloma on histology + AFB on ZN stain. Treated with 2HRZE/4HR.
This is a shared conversation. Sign in to Orris to start your own chat.