Adult onset stil disease explanation and management
Reading File
Finding Sources
Searching PubMed
"adult-onset Still's disease" AND management
Finding Sources
Searching PubMed
"adult-onset Still disease" treatment
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Loading Image
Searching Images
adult onset Still disease salmon pink rash fever
I now have all the material needed for a comprehensive answer. Let me compile it.
Adult-Onset Still Disease (AOSD)
Overview
Adult-onset Still disease (AOSD) is a rare systemic autoinflammatory disorder — not autoimmune — characterized by the triad of quotidian spiking fevers, polyarthritis, and an evanescent salmon-pink rash. The term was coined by Bywaters in 1971 for adults presenting with a syndrome identical to systemic juvenile idiopathic arthritis (sJIA). It is a diagnosis of exclusion; infection and malignancy must be ruled out first.
Epidemiology
- Primarily affects young adults, with onset before age 30 in the majority; rarely occurs after age 60
- Slight female predominance
- Estimated prevalence: 1–34 per million; incidence ~0.16–0.4 per 100,000/year
- No consistent HLA association, though HLA-DRB1:11 linkage has been reported
— Dermatology 2-Volume Set 5e; Fitzpatrick's Dermatology Vol. 1–2
Pathogenesis
The etiology is unknown. AOSD is considered a macrophage-driven autoinflammatory disease (an "inflammasomopathy"):
- Triggered in genetically susceptible individuals, possibly by infectious agents (enteroviruses, herpesviruses, bacteria causing pneumonia/enterocolitis) — but no agent has been consistently implicated
- Key cytokines involved: IL-1β, IL-6, IL-18, TNF-α, IFN-γ — all markedly elevated
- IL-18 in particular appears pathogenic; levels correlate with disease activity and macrophage activation syndrome (MAS)
- The disease shares pathogenesis with sJIA, though familial cases are uncommon
— Dermatology 2-Volume Set 5e; Fitzpatrick's Dermatology Vol. 1–2
Clinical Features
Fever
- Hallmark: daily quotidian spiking fever ≥39°C, typically occurring in the late afternoon or early evening, resolving within hours
- Fever precedes other manifestations in many cases; it is often the presenting complaint
Skin Rash
- Occurs in ~85–95% of patients; the most distinctive sign
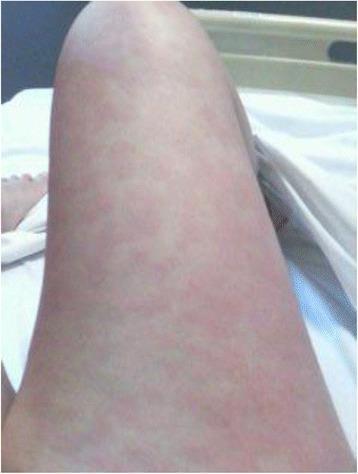
- Classic (evanescent) rash: salmon-pink maculopapular eruption, asymptomatic, appearing synchronously with fever spikes and fading within hours
- Favors pressure sites; demonstrates the Koebner phenomenon; most common on trunk but can involve extremities, palms, and soles
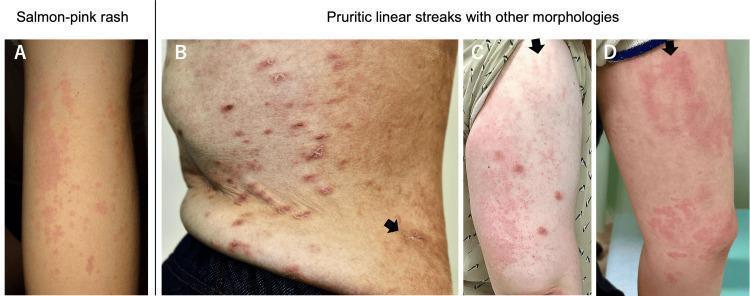
Atypical (persistent) variants — now increasingly recognized:
- Persistent pruritic papules and plaques, often with linear distribution (flagellate pattern)
- Persistent erythematous eyelid edema (can mimic dermatomyositis)
- Flagellate erythema
- Atypical persistent lesions are associated with a worse prognosis and a possible link to malignancy
Arthritis
- Occurs in 65–100% of patients
- Arthralgia/arthritis, often polyarticular; carpal ankylosis is a distinctive long-term feature
- Joint disease can be the dominant feature in the "chronic articular" phenotype
Other Systemic Features
- Sore throat / pharyngitis (common early symptom, often at onset)
- Lymphadenopathy (cervical most common) and splenomegaly
- Hepatomegaly with elevated transaminases
- Serositis: pleuritis, pleural effusions; pericarditis (up to 50%), cardiac tamponade (rare); myocarditis
- Pulmonary involvement: rare (fibrosis, pulmonary arterial hypertension)
- Renal: nephritis (rare)
Disease Patterns
Three recognized clinical courses:
- Monocyclic (self-limited, single episode) — ~20%
- Polycyclic / intermittent (recurrent flares with remissions) — ~30%
- Chronic articular (persistent disease, dominant joint involvement) — ~50%
Laboratory Findings
| Test | Finding |
|---|---|
| Ferritin | Markedly elevated; >3× normal in ~60%; sometimes >4,000 ng/mL |
| Glycosylated ferritin | <20% (normally 50–80%); highly characteristic |
| WBC | Leukocytosis ≥10,000/mm³ in 85%; ≥80% neutrophils in 69% |
| CRP | Elevated in ~93% |
| ESR | Elevated (≥20 mm/h) in 85% |
| Liver enzymes | Elevated in ~62% |
| Platelets | Thrombocytosis (>400 × 10⁹/L) in ~46% |
| Hemoglobin | Anemia <10 g/dL in 50–75% |
| ANA, RF, anti-CCP | Negative or low titer |
A markedly elevated ferritin with glycosylated ferritin fraction <20% is strongly suggestive of AOSD, though not pathognomonic.
— Fitzpatrick's Dermatology Vol. 1–2
Diagnosis: Classification Criteria
AOSD is a diagnosis of exclusion. Two validated criteria sets are used:
Yamaguchi Criteria (1992) — most widely used
Requires ≥5 criteria, of which ≥2 must be major, plus no exclusion criteria
Major:
- Fever ≥39°C lasting ≥1 week
- Arthralgia lasting ≥2 weeks
- Typical salmon-pink maculopapular rash coinciding with fever
- Leukocytosis ≥10,000/mm³ with ≥80% neutrophils
Minor:
- Pharyngitis or sore throat
- Lymphadenopathy and/or splenomegaly
- Abnormal liver enzymes
- Negative ANA and RF
Exclusion criteria: active infection (especially EBV, sepsis), malignancy (especially lymphoma), inflammatory disease (polyarteritis nodosa)
Fautrel Criteria (2002)
Requires 4 major, OR 3 major + 2 minor — no exclusion criteria required
Major: Spiking fever ≥39°C · Arthralgia · Transient erythema · Pharyngitis · Neutrophils ≥80% · Glycosylated ferritin fraction ≤20%
Minor: Typical rash · Leukocytosis >10,000/mm³
The Fautrel criteria include glycosylated ferritin as a specific major criterion and require no exclusions, making it easier to apply.
— Fitzpatrick's Dermatology Vol. 1–2 (Table 66-5)
Histopathology
Evanescent lesions: Interstitial and perivascular neutrophil-dominant mixed infiltrate with lymphocytes — indistinguishable from sJIA
Persistent/atypical lesions: Additional epidermal changes — acanthosis, spongiosis, necrotic keratinocytes in the spinous layer
Complications
Macrophage Activation Syndrome (MAS)
- The most dangerous complication (~10% of patients); a form of secondary hemophagocytic lymphohistiocytosis (HLH)
- Heralded by a change from spiking to continuous fever, worsening hepatosplenomegaly, lymphadenopathy, cytopenias, and CNS dysfunction
- Ferritin often 5,000–10,000 ng/mL
- Coagulopathy (prolonged PT/PTT), triglycerides elevated, fibrinogen decreased
- Life-threatening: requires urgent treatment
Management
Treatment is stepwise based on severity:
Step 1 — Mild-Moderate Disease
- NSAIDs / high-dose aspirin: useful in mild systemic disease; majority require escalation
- Corticosteroids (prednisone 40–60 mg/day): cornerstone of acute management; controls fever, rash, and serositis
Step 2 — Steroid-Sparing / Corticosteroid-Dependent Disease
- Methotrexate (7.5–20 mg/week): most commonly used DMARD, especially for persistent arthritis and steroid tapering
- Hydroxychloroquine: sometimes used for milder disease
Step 3 — Refractory / Severe Disease (Biologics)
| Agent | Target | Notes |
|---|---|---|
| Anakinra (IL-1R antagonist) | IL-1 | Highly effective in systemic form; first choice in many centers |
| Canakinumab (anti-IL-1β) | IL-1β | Long-acting; approved for sJIA; increasingly used in AOSD |
| Tocilizumab (anti-IL-6R) | IL-6 | Effective, especially for systemic inflammation without predominant joints |
| TNF inhibitors (etanercept, infliximab) | TNF-α | Particularly useful in chronic polyarticular disease |
| Rituximab (anti-CD20) | B cells | Used for refractory disease |
| Ruxolitinib (JAK inhibitor) | JAK-STAT | Emerging evidence, especially for refractory MAS |
IL-1 and IL-6 blockers are increasingly used as first-line therapy for moderate-to-severe disease with prominent systemic inflammation (as opposed to purely articular disease).
MAS Management
- High-dose IV corticosteroids (first-line)
- Cyclosporine for corticosteroid-resistant cases
- Anakinra / canakinumab (IL-1 blockade)
- Etoposide for refractory/fulminant HLH
- Emapalumab (anti-IFN-γ) in refractory cases
— Dermatology 2-Volume Set 5e; Fuster & Hurst's The Heart 15e; Fitzpatrick's Dermatology Vol. 1–2
Differential Diagnosis
| Condition | Distinguishing features |
|---|---|
| Sepsis / EBV / viral syndrome | Positive cultures/serology, different fever pattern |
| Lymphoma | Lymph node biopsy, no typical rash |
| Schnitzler syndrome | Monoclonal IgM gammopathy, bone pain (hyperostosis), urticarial rash |
| Dermatomyositis | Interface dermatitis on biopsy, myositis-specific antibodies, Gottron's papules |
| SLE | Positive ANA/dsDNA, photosensitive rash, renal involvement |
| Reactive arthritis | Preceding infection, asymmetric oligoarthritis, HLA-B27 |
| AOSD rash vs. urticaria | AOSD rash: non-pruritic, evanescent, salmon-pink, fever-synchronous |
Prognosis
- Monocyclic: favorable; disease resolves within 1 year
- Chronic articular form: risk of joint destruction and disability; may need long-term DMARDs/biologics
- MAS: ~10% mortality even with treatment in severe cases
- Atypical persistent cutaneous lesions are associated with higher risk of associated malignancy — vigilance is warranted
This is a shared conversation. Sign in to Orris to start your own chat.