Let’s study everything in detail in crisp, concise and conceptual way fromCOPD guidelines or gold that is required in MBBS level Especially from diagnosis and management
Reading File
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Now I have everything I need. Let me compile the comprehensive, crisp MBBS-level COPD guide.
COPD — Complete MBBS-Level Study Guide (GOLD Framework)
Sources: Goldman-Cecil Medicine, Washington Manual of Medical Therapeutics, Textbook of Family Medicine
1. DEFINITION (Conceptual Core)
COPD = persistent airflow limitation that is NOT fully reversible with bronchodilators, caused by airway/alveolar abnormalities from noxious exposures.
It encompasses two entities that coexist in most patients:
| Entity | Core Defect | Classic Type |
|---|---|---|
| Chronic Bronchitis | Mucus hypersecretion, inflammation | "Blue Bloater" |
| Emphysema | Alveolar wall destruction, loss of elastic recoil | "Pink Puffer" |
Chronic bronchitis definition (clinical): Productive cough ≥3 months/year for ≥2 consecutive years.
2. RISK FACTORS
- Cigarette smoking — far and away the #1 risk factor (dose = pack-years)
- Biomass fuel combustion (cooking/heating in poorly ventilated spaces)
- Occupational dust (mines, grain, cotton mills)
- α₁-antitrypsin (A1AT) deficiency — genetic cause; screen ALL COPD patients at least once
- Childhood respiratory infections → impaired lung growth → lower peak FEV₁
- Secondhand smoke, maternal smoking during pregnancy
3. PATHOPHYSIOLOGY (Conceptual)
Trigger: Noxious inhalation → chronic inflammation
Key imbalance: Protease > Antiprotease → alveolar destruction (emphysema)
- Normal: Neutrophil elastase balanced by A1AT
- In COPD/smoking: A1AT overwhelmed → unchecked elastase → alveolar wall breakdown
Consequences:
- Loss of elastic recoil → dynamic collapse of small airways during expiration → air trapping
- Mucus gland hypertrophy + goblet cell hyperplasia → chronic bronchitis physiology
- V/Q mismatch → hypoxemia
- Late: hypercapnia, cor pulmonale, polycythemia
4. CLINICAL FEATURES
Typical patient: >40 years, significant smoking history
Symptoms (progressive over years):
- Dyspnea on exertion (cardinal symptom)
- Chronic cough + sputum production
- Wheezing
Classic phenotypes:
| Feature | Pink Puffer (Emphysema) | Blue Bloater (Chronic Bronchitis) |
|---|---|---|
| Build | Thin, cachexic | Obese/overweight |
| Cyanosis | Absent | Present |
| Cough | Minimal | Productive, chronic |
| PaCO₂ | Normal/low | High (CO₂ retention) |
| PaO₂ | Near normal | Low |
| Cor pulmonale | Late | Early |
| Breathing | Pursed-lip, tripod | Labored |
Signs:
- Barrel chest (↑AP diameter), hyperresonance
- Diminished breath sounds, prolonged expiration
- Use of accessory muscles
- Pursed-lip breathing
5. DIAGNOSIS
Step 1: Clinical suspicion
Any patient >40 years with dyspnea, chronic cough/sputum, or risk factor exposure.
Step 2: Spirometry — THE GOLD STANDARD
Diagnostic criterion (post-bronchodilator):
FEV₁/FVC < 0.70
This confirms fixed (irreversible) airflow obstruction.
Additional findings:
- ↑ TLC, FRC, RV (hyperinflation, air trapping)
- ↓ DLCO in emphysema (alveolar destruction)
Step 3: GOLD Spirometric Severity Grading
(Based on post-bronchodilator FEV₁ % predicted, in patients with FEV₁/FVC < 0.70)
| GOLD Grade | Severity | FEV₁ % Predicted |
|---|---|---|
| 1 | Mild | ≥80% |
| 2 | Moderate | 50–79% |
| 3 | Severe | 30–49% |
| 4 | Very Severe | <30% |
Step 4: GOLD ABCD Classification (combines symptoms + exacerbation risk)
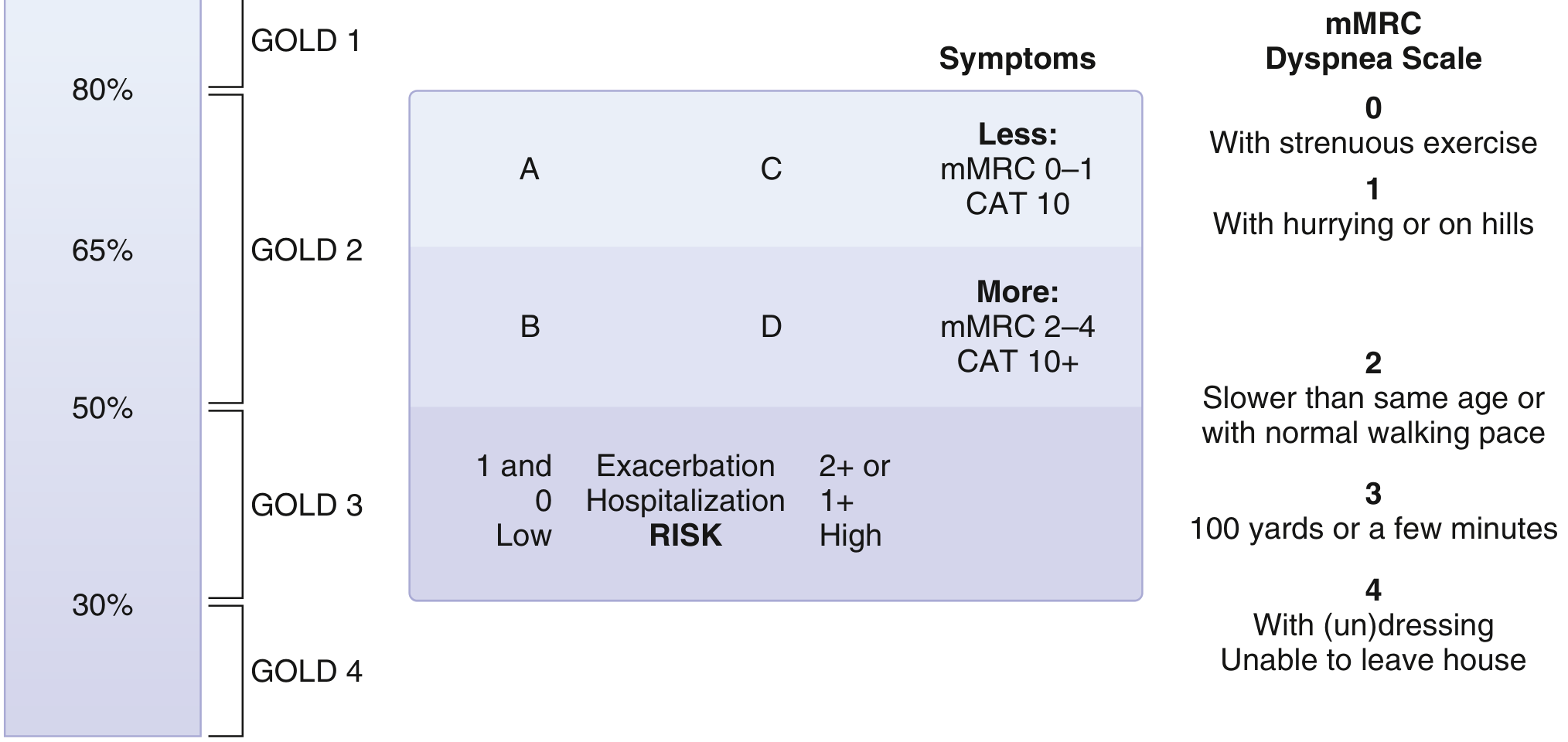
| Group | Exacerbations | Symptoms | Spirometry |
|---|---|---|---|
| A | 0–1 (no hospitalization) | Mild (mMRC 0–1 or CAT <10) | Any |
| B | 0–1 (no hospitalization) | More (mMRC ≥2 or CAT ≥10) | Any |
| C | ≥2 or ≥1 hospitalization | Mild (mMRC 0–1 or CAT <10) | Any |
| D | ≥2 or ≥1 hospitalization | More (mMRC ≥2 or CAT ≥10) | Any |
Key concept: ABCD groups guide therapy; GOLD 1–4 grades guide prognosis.
Symptom tools:
- mMRC Scale (0–4): 0 = only with strenuous exertion → 4 = too breathless to leave house
- CAT Score (0–40): ≥10 = significant impact
Investigations
| Test | Purpose |
|---|---|
| Spirometry | Diagnosis (essential) |
| CXR | Exclude alternatives; shows hyperinflation, flat diaphragm, bullae, ↓vascular markings |
| CT chest | Detects emphysema, airway thickening, air trapping; guides surgery candidacy |
| ABG | Severe COPD — assess hypoxemia/hypercapnia |
| A1AT level | Screen all COPD patients once |
| Peripheral eosinophils | >300 cells/μL → consider ICS |
| 6-min walk test | Functional capacity, prognosis |
| ECG/Echo | Detect cor pulmonale |
6. STABLE COPD MANAGEMENT
Principle: Goals of treatment
- Reduce symptoms and improve exercise tolerance
- Reduce frequency/severity of exacerbations
- Slow disease progression
- Prolong survival
A. Smoking Cessation — #1 MOST IMPORTANT INTERVENTION
- Only intervention proven to slow FEV₁ decline
- NRT (nicotine patch/gum), Varenicline, Bupropion
- Counseling + pharmacotherapy = best combo
B. Pharmacotherapy — Inhaled Route is Preferred
Classes of drugs:
| Class | Examples | Mechanism | Key Side Effects |
|---|---|---|---|
| SABA | Salbutamol/Albuterol, Levalbuterol | β₂-agonist, bronchodilation | Palpitations, tremor, tachycardia |
| SAMA | Ipratropium | Muscarinic antagonist | Dry mouth, urinary retention |
| LABA | Salmeterol, Formoterol, Indacaterol, Olodaterol | Long-acting β₂-agonist | Palpitations, hypokalemia |
| LAMA | Tiotropium, Umeclidinium, Glycopyrronium | Long-acting muscarinic antagonist | Dry mouth, constipation, glaucoma |
| ICS | Fluticasone, Budesonide, Beclomethasone | Anti-inflammatory | Oral candidiasis, hoarseness, ↑ pneumonia risk |
| PDE-4 inhibitor | Roflumilast | Anti-inflammatory | Diarrhoea, nausea, weight loss, depression |
| Theophylline | Oral | Nonspecific PDE inhibitor, bronchodilator | Narrow therapeutic index; arrhythmias, seizures |
Key rules for ICS:
- Never monotherapy in COPD
- Indicated if eosinophils >300 cells/μL, or persistent exacerbations on LABA+LAMA
- Withdraw if <2 exacerbations/year AND eosinophils <300 cells/μL
C. Initial Pharmacotherapy by ABCD Group
| Group | First Choice |
|---|---|
| A | A bronchodilator (SABA or SAMA as needed) |
| B | LABA or LAMA |
| C | LAMA (preferred over LABA) |
| D | LAMA ± LABA; if CAT >20 → LABA+LAMA; if eosinophils >300 → ICS+LABA |
Escalation concept: A → B = add long-acting agent; C/D = LABA+LAMA → add ICS if still exacerbating and eos >300.
D. Non-Pharmacological Therapy
| Intervention | Notes |
|---|---|
| Pulmonary rehabilitation | All patients (especially post-exacerbation, pre-surgery). Aerobic + strength training. Improves exercise tolerance and quality of life. |
| Long-term oxygen therapy (LTOT) | Improves survival — only non-pharmacological intervention proven to do so |
| Vaccinations | Influenza (annual), Pneumococcal, COVID-19 |
| NIV (BiPAP) | Nocturnal hypercapnia with PaCO₂ ≥52 mmHg |
| LVRS | Lung volume reduction surgery for upper-lobe emphysema + low exercise capacity |
| Lung transplant | End-stage COPD |
LTOT Indications (memorize)
- PaO₂ ≤55 mmHg or SpO₂ ≤88% at rest
- PaO₂ 56–59 mmHg or SpO₂ <89% if cor pulmonale, right heart failure, or polycythemia (Hct >55%)
7. ACUTE EXACERBATION OF COPD (AECOPD)
Definition
Acute worsening of respiratory symptoms beyond normal day-to-day variation → requiring change in therapy.
Triggers:
- Respiratory infection (most common) — viral > bacterial
- Air pollution, non-compliance, cardiac causes
Cardinal symptoms: ↑ dyspnea + ↑ cough + ↑ sputum (volume/purulence)
Assessment
- ABG: assess hypoxemia, hypercapnia, pH
- CXR: exclude pneumonia, pneumothorax, pulmonary edema
- ECG: detect arrhythmias
Treatment (Stepwise)
1. Bronchodilators
- SABA ± SAMA (ipratropium) via nebuliser — first-line
- Combine albuterol + ipratropium in acute setting
2. Systemic Corticosteroids
- Prednisolone 30–40 mg orally for 5 days (not longer — no added benefit >2 weeks)
- Reduces treatment failures by ~46%, shortens hospital stay
- ↑ risk of hyperglycemia
3. Antibiotics
- Indicated if: ≥2 cardinal symptoms (especially purulent sputum), signs of pneumonia, need for mechanical ventilation
- Agents: amoxicillin-clavulanate, azithromycin, doxycycline, or fluoroquinolone
4. Controlled Oxygen
- Target SpO₂ 88–92% (avoid over-oxygenation → suppresses hypoxic drive in CO₂ retainers)
- Recheck ABG 30 minutes after starting O₂
5. NIV (BiPAP)
- Indication: pH <7.35 with PaCO₂ >45 mmHg + RR >25 — reduces need for intubation
6. Mechanical Ventilation
- When NIV fails or is contraindicated
- Indications: pH <7.25, PaO₂ <40 mmHg, mental status change (confusion/lethargy)
Indications for Hospitalization
- Severe dyspnea not responding to initial treatment
- New cyanosis or change in mental status
- Failure of outpatient therapy
- Significant comorbidities (CHF, arrhythmia)
- Underlying pneumonia
Indications for ICU
- pH <7.25 or PaCO₂ >60 mmHg or PaO₂ <40 mmHg
- Hemodynamic instability
- Altered consciousness
8. QUICK DIFFERENTIATORS — COPD vs. ASTHMA
| Feature | COPD | Asthma |
|---|---|---|
| Age of onset | >40 yrs | Any age (often childhood) |
| Smoking | Strong association | Not required |
| Airflow limitation | Fixed (irreversible) | Reversible |
| Post-bronchodilator FEV₁/FVC | <0.70 persists | Normalizes |
| DLCO | Often ↓ (emphysema) | Normal |
| Eosinophilia | Variable | Common |
| Diurnal variation | Minimal | Marked |
9. HIGH-YIELD MNEMONICS / EXAM FACTS
- COPD diagnosis = Spirometry: post-BD FEV₁/FVC <0.70
- GOLD 1–4 = Mild/Moderate/Severe/Very Severe (FEV₁ cutoffs: 80, 50, 30%)
- GOLD A–D = Symptom + exacerbation risk matrix → guides initial inhaler choice
- Only proven survival benefits: Smoking cessation + LTOT (in hypoxemic patients)
- LAMA > LABA for exacerbation prevention (Group C)
- ICS not monotherapy; adds pneumonia risk; use when eos >300 or persistent exacerbations
- AECOPD O₂ target = 88–92% (not 100%)
- Systemic steroids for exacerbations = 5 days (not >2 weeks)
- A1AT screen — every COPD patient at least once
- Roflumilast (PDE-4 inhibitor) = for severe COPD with chronic bronchitis phenotype + frequent exacerbations
- β-blockers are NOT contraindicated in COPD (for CV indications)
10. COMPLICATIONS OF COPD
- Cor pulmonale — RV hypertrophy from pulmonary hypertension (chronic hypoxia → vasoconstriction)
- Polycythemia — compensatory response to chronic hypoxemia
- Spontaneous pneumothorax — bullae rupture
- Respiratory failure — Type 2 (hypercapnic) in advanced disease
- Lung cancer — strong association; screen with low-dose CT if ≥20 pack-years, age 50–80, quit ≤15 years ago
- OSA-COPD overlap — higher risk of hypercapnia and pulmonary hypertension
Sources: Goldman-Cecil Medicine 26e | Washington Manual of Medical Therapeutics | Textbook of Family Medicine 9e
This is a shared conversation. Sign in to Orris to start your own chat.