Membrane potential
Reading File
Finding Sources
Searching the Web
membrane potential physiology overview
Reading File
Reading File
Reading File
Loading Image
Reading File
Finding Sources
Reading File
Reading File
Loading Image
Here is a comprehensive overview of membrane potential, drawn from Guyton & Hall, Costanzo Physiology, and Medical Physiology.
Membrane Potential
Definition
Membrane potential (Vm) is the electric potential difference across a cell membrane, measured as the intracellular potential relative to the extracellular potential. By convention, the extracellular fluid is set at 0 mV. In resting excitable cells (nerve and muscle), the interior is negative relative to the exterior.
Resting Membrane Potential (RMP)
The RMP of most excitable cells falls between −70 and −90 mV:
- Large nerve fibers: ~−70 mV
- Skeletal muscle: ~−90 mV
- Erythrocytes: as low as ~−10 mV
How It Is Measured
A microelectrode (glass micropipette filled with electrolyte, tip < 1 µm, resistance > 1 MΩ) is impaled through the membrane. A voltage is recorded between the intracellular tip and an indifferent electrode in the extracellular fluid.
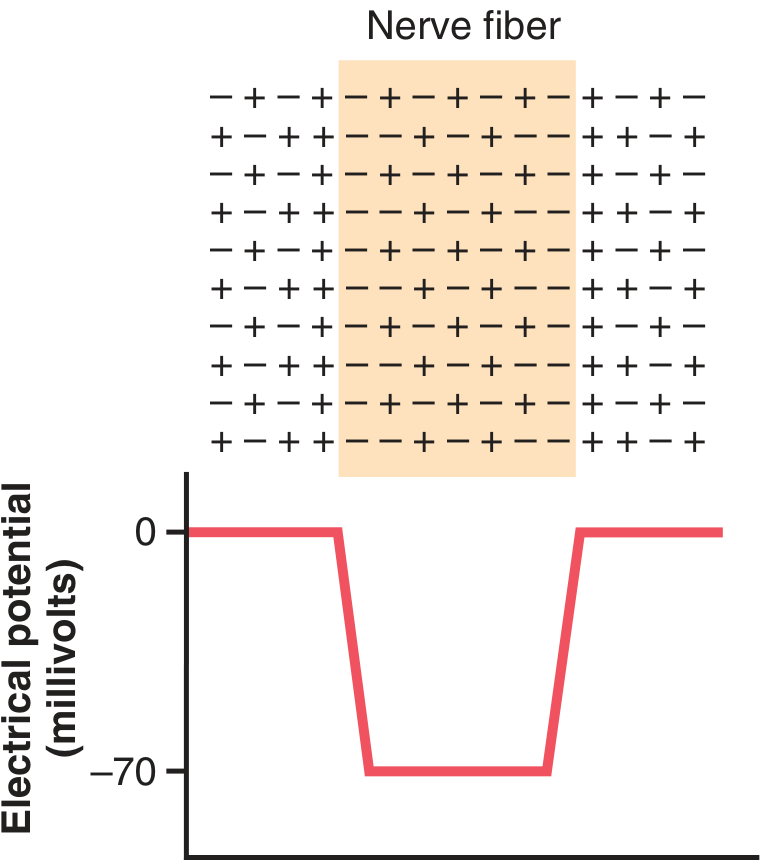
Figure: Charge distribution across a nerve fiber and the resulting electrical potential. Outside the fiber = 0 mV; inside = −70 mV. — Guyton & Hall
Ionic Basis: Why Is the Inside Negative?
Ion Concentration Gradients
The Na⁺-K⁺ ATPase pump actively establishes and maintains these gradients:
| Ion | Outside | Inside | Nernst Potential |
|---|---|---|---|
| K⁺ | 4 mEq/L | 140 mEq/L | −94 mV |
| Na⁺ | 142 mEq/L | 14 mEq/L | +61 mV |
| Ca²⁺ | 1.0 mM | 0.0001 mM | +123 mV |
| Cl⁻ | 116 mM | 4.2 mM | −89 mV |
Differential Permeability
At rest, the membrane is ~100× more permeable to K⁺ than to Na⁺ (via K⁺ "leak" channels). K⁺ therefore diffuses down its concentration gradient (out of the cell), carrying positive charge outward and leaving the inside negative.
Three Contributions to the RMP
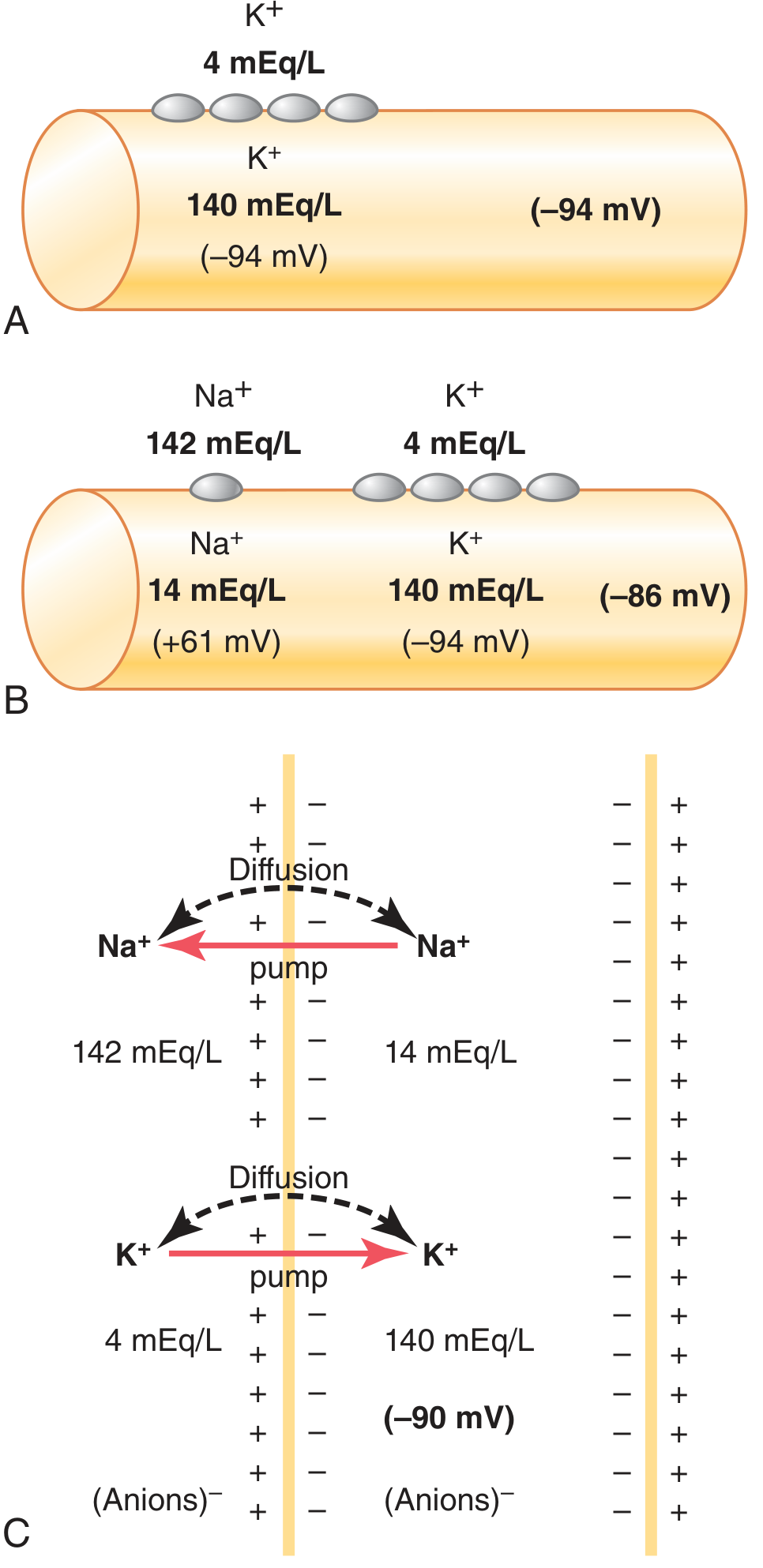
Figure 5.5: Establishment of RMP under three conditions. — Guyton & Hall
| Component | Contribution |
|---|---|
| K⁺ diffusion potential | Major driver: K⁺ leaving the cell → ~−94 mV if K⁺ were the only ion |
| Na⁺ diffusion potential | Small inward leak of Na⁺ offsets K⁺ effect → combined Goldman potential ~−86 mV |
| Na⁺-K⁺ pump (electrogenic) | Pumps 3 Na⁺ out for every 2 K⁺ in → adds ~−4 mV (small direct effect) |
| Overall RMP | ~−90 mV |
Key Equations
Nernst Equation
Predicts the equilibrium potential for a single ion:
$$E_x = \frac{-61.5 \text{ mV}}{z} \log_{10} \frac{[X]_i}{[X]_o} \quad \text{(at 37°C)}$$
- For K⁺ (z = +1): slope = −61.5 mV per 10-fold change in [K⁺]
- For Na⁺ (z = +1): E_Na ≈ +61 mV
- For Ca²⁺ (z = +2): slope = ~−30 mV per decade
Goldman (Goldman-Hodgkin-Katz) Equation
Accounts for multiple ions simultaneously, weighted by their relative permeabilities (P):
$$V_m = \frac{RT}{F} \ln \frac{P_{K}[K^+]o + P{Na}[Na^+]o + P{Cl}[Cl^-]i}{P{K}[K^+]i + P{Na}[Na^+]i + P{Cl}[Cl^-]_o}$$
Chord Conductance Equation
Weights each ion's equilibrium potential by its relative conductance (g):
$$E_m = \frac{g_{K^+}}{g_T}E_{K^+} + \frac{g_{Na^+}}{g_T}E_{Na^+} + \frac{g_{Cl^-}}{g_T}E_{Cl^-} + \frac{g_{Ca^{2+}}}{g_T}E_{Ca^{2+}}$$
Ions with the highest conductance at rest (K⁺, Cl⁻) drive the RMP toward their equilibrium potentials. Ions with low conductance (Na⁺, Ca²⁺) have little influence at rest.
Role of the Na⁺-K⁺ ATPase
The pump has two roles:
- Indirect (dominant): Maintains the K⁺ and Na⁺ concentration gradients that power diffusion potentials. Blocking the pump with cardiac glycosides only shifts Vm by ~1.4 mV acutely — confirming that the pump's direct electrogenic contribution is minor.
- Direct (electrogenic, minor): 3 Na⁺ out / 2 K⁺ in per ATP → net export of 1 positive charge → adds ~−4 mV to the RMP.
Key Concepts
| Term | Meaning |
|---|---|
| Depolarization | Vm becomes less negative (moves toward 0 or positive) |
| Hyperpolarization | Vm becomes more negative |
| Repolarization | Vm returns toward RMP after depolarization |
| Equilibrium potential (Ex) | Vm at which there is no net flux of ion X (chemical and electrical forces balance) |
| Threshold | Vm at which an action potential is triggered (~−55 mV in neurons) |
Clinical Relevance
- Hyperkalemia raises extracellular [K⁺] → reduces K⁺ concentration gradient → RMP becomes less negative → cells partially depolarize → increased excitability initially, then inexcitability (e.g., cardiac arrhythmias, muscle weakness)
- Hypokalemia → more negative RMP → hyperpolarization → reduced excitability
- Local anesthetics (e.g., lidocaine) block Na⁺ channels, preventing depolarization
- Cardiac glycosides (e.g., digoxin) inhibit Na⁺-K⁺ ATPase, indirectly raising intracellular [Ca²⁺] (via Na⁺/Ca²⁺ exchanger)
Sources: Guyton and Hall Textbook of Medical Physiology; Costanzo Physiology 7th Ed.; Medical Physiology (Boron & Boulpaep)
This is a shared conversation. Sign in to Orris to start your own chat.