Squint
Reading File
Finding Sources
Searching PubMed
strabismus squint classification management
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Reading File
Searching Images
strabismus squint esotropia exotropia eye deviation
I now have comprehensive content. Here is a thorough overview of squint (strabismus):
Squint (Strabismus)
Strabismus is misalignment of the visual axes of the two eyes. "Squint" is the colloquial/British term used interchangeably with strabismus.
Epidemiology
- Affects ~4% of the population
- Amblyopia co-occurs in approximately 50% of strabismus patients
- Amblyopia without strabismus accounts for the other 50% of amblyopia cases
Classification
Strabismus is broadly classified by:
Direction of Deviation
| Term | Eye position |
|---|---|
| Esotropia | Inward (convergent, "crossed eyes") |
| Exotropia | Outward (divergent) |
| Hypertropia | Upward |
| Hypotropia | Downward |
| Cyclotropia | Rotational (torsional) |
Constancy
- Tropia: manifest deviation (always present)
- Phoria: latent deviation (only manifest when fusion is disrupted, e.g., by cover test)
Comitance
- Concomitant (comitant): angle of deviation is the same (<5Δ variability) in all positions of gaze — implies no muscle or nerve pathology
- Incomitant: angle varies with gaze position — suggests a paretic or restrictive cause
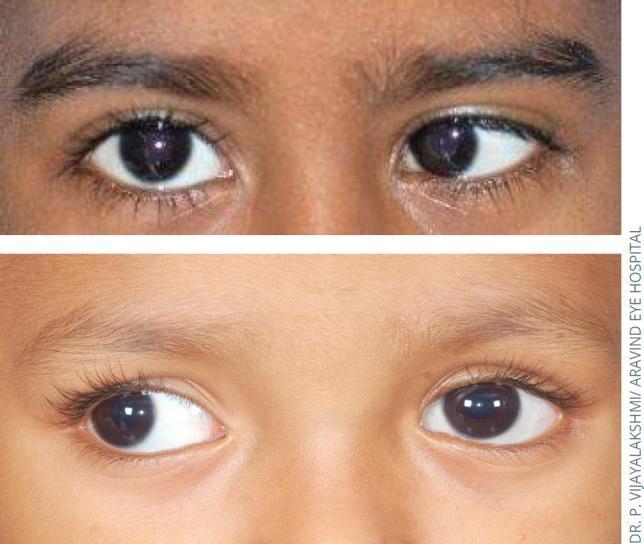
Esotropia — Detailed Classification (Table 18.1, Kanski)
Accommodative
- Refractive (fully accommodative): due to uncorrected hypermetropia (+2 to +7D), normal AC/A ratio; presents 18 months–3 years; fully corrected by spectacles
- Partially accommodative: reduced but not eliminated by full spectacle correction
- Non-refractive (convergence excess): high AC/A ratio — near deviation > distance deviation; bifocals may help
Non-accommodative
- Early-onset (essential infantile) esotropia: onset <6 months; large angle (>30Δ); alternating fixation; cross-fixation in lateral gaze; may mimic bilateral 6th nerve palsy
- Microtropia: small angle (<5Δ), often with amblyopia and eccentric fixation
- Sensory esotropia: due to poor vision in one eye
- Consecutive esotropia: follows over-correction of exotropia
- Acute-onset esotropia: sudden onset in older children/adults; needs neurological evaluation
- Cyclic esotropia: esotropia alternates on a regular 48-hour cycle
- Divergence insufficiency/paralysis
Exotropia
- Constant (early-onset): large, constant angle; frequently associated with neurological anomalies
- Intermittent exotropia: most common type overall; begins as exophoria breaking into exotropia with fatigue, bright light, or inattention; children often close one eye in sunlight
- Distance excess: larger deviation for distance
- Basic: equal deviation near and distance
- Convergence insufficiency: larger deviation for near
- Sensory exotropia: secondary to visual loss in the deviating eye
- Consecutive exotropia: follows over-correction of esotropia
Causes
- Central: abnormalities of oculomotor nuclei / cranial nerves (III, IV, VI palsies)
- Refractive: uncorrected hypermetropia (esotropia) or myopia (exotropia)
- Anatomical: structural muscle abnormalities
- Sensory: reduced vision in one eye
- Restrictive: orbital pathology (e.g. thyroid eye disease), fibrosis syndromes
Consequences — Amblyopia
Amblyopia ("lazy eye") is the key functional consequence: the brain suppresses the image from the misaligned eye, leading to reduced best-corrected visual acuity.
Types:
- Strabismic: monocular suppression of the deviating eye
- Anisometropic: difference in refractive error ≥1D between eyes
- Stimulus deprivation: media opacity (cataract), ptosis covering the pupil
- Bilateral ametropic: high symmetric hypermetropia
- Meridional: uncorrected astigmatism
Critical period: visual plasticity up to ~7–8 years for strabismic amblyopia; possibly into the teens for anisometropic amblyopia.
Diagnosis
Clinical Tests
- Corneal light reflex (Hirschberg test): penlight held at 33 cm; normally symmetric reflex in both pupils. Decentration indicates deviation (~1 mm displacement ≈ 7Δ)
- Cover test (most important): patient fixates a target; cover one eye and observe the other for movement
- Cover-uncover test: detects tropias
- Alternating cover test: detects phorias
- Red reflex: helps detect media opacities causing deprivational amblyopia
- Cycloplegic refraction: mandatory in all children with esotropia (atropine or cyclopentolate)
- Prism and alternate cover test: quantifies the angle
Warning Signs Requiring Urgent Evaluation
- Any esotropia in infancy — rule out retinoblastoma (white reflex / leukocoria)
- Acute-onset diplopia — may indicate intracranial pathology (CN III/IV/VI palsy, raised ICP)
Treatment
Amblyopia Treatment (First)
- Patching (occlusion) of the better-seeing eye — most effective; duration depends on age and severity
- Atropine penalisation (1% atropine to the better eye): equally effective to patching; useful when compliance with patches is poor
- Both modalities must be started before age 7–8 years for best outcomes; treatment before age 2–3 years gives the best prognosis
- Failure after 6 months of effective occlusion → further improvement unlikely
Refractive Correction
- Full cycloplegic refraction with spectacles is mandatory
- Fully accommodative esotropia: spectacles alone correct the deviation
- Convergence excess: bifocals reduce the near deviation
- Myopic exotropia: full myopic correction may control exodeviation
Surgery
Indications: residual deviation after optical correction, cosmesis, non-accommodative esotropia, intermittent exotropia progressing to constant
- Early-onset esotropia: bilateral medial rectus recession — goal is alignment within 8Δ (peripheral fusion with central suppression acceptable)
- Exotropia: lateral rectus recession ± medial rectus resection
- Timing: most surgeons operate before age 2 years for infantile esotropia to maximise binocularity
Botulinum Toxin
- Can be injected into the antagonist muscle (e.g., medial rectus in esotropia) as an alternative or adjunct to surgery, particularly for small to moderate deviations
Key Points
| Feature | Esotropia | Exotropia |
|---|---|---|
| Direction | Inward | Outward |
| Common cause | Hypermetropia (accommodative) | Myopia, neurological |
| Amblyopia risk | Higher (constant) | Lower (often intermittent) |
| Medical Rx | Spectacles (accommodative type) | Spectacles (myopia) |
| Surgical Rx | Medial rectus recession | Lateral rectus recession |
Sources: Kanski's Clinical Ophthalmology, 10th ed. — Goldman-Cecil Medicine — Textbook of Family Medicine, 9th ed.
This is a shared conversation. Sign in to Orris to start your own chat.