Explain the anatomy of pelvis and perineum
Reading File
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Reading File
Searching Images
pelvis anatomy bony structure pelvic inlet outlet
Searching Images
perineum triangles urogenital anal anatomy
Loading Image
Loading Image
Reading File
Loading Image
Loading Image
Reading File
Finding Sources
Finding Sources
Reading File
Loading Image
I now have comprehensive material from Gray's Anatomy for Students, the THIEME Atlas, and supporting images. Let me compile the full, well-structured answer.
Anatomy of the Pelvis and Perineum
Based on Gray's Anatomy for Students, THIEME General Anatomy & Musculoskeletal System, and Campbell-Walsh-Wein Urology
1. The Bony Pelvis
The pelvis is a basin-shaped ring of bone formed by four bones:
- Two hip (coxal) bones — each comprising the ilium, ischium, and pubis, fused at the acetabulum
- The sacrum — formed by the 5 fused sacral vertebrae
- The coccyx — 4 fused coccygeal vertebrae
Key Bony Landmarks
| Landmark | Relevance |
|---|---|
| Iliac crest | Highest point of the ilium; palpable along the full length |
| Anterior superior iliac spine (ASIS) | Origin of inguinal ligament; clinical landmark |
| Posterior superior iliac spine (PSIS) | Overlies the sacroiliac joint |
| Ischial tuberosity | Weight-bearing when seated; corner of the diamond-shaped perineum |
| Ischial spine | Attachment of sacrospinous ligament; landmark for pudendal nerve block |
| Pubic symphysis | Fibrocartilaginous joint anteriorly; anterior limit of perineum |
| Pubic tubercle | Attachment of inguinal ligament |
| Sacral promontory | Upper anterior edge of sacrum; posterior limit of pelvic inlet |
Pelvic Inlet and Outlet
- Pelvic inlet (superior pelvic aperture): bounded by the sacral promontory posteriorly, the arcuate line of the ilium laterally, and the pubic symphysis anteriorly. The inlet faces anterosuperiorly.
- Pelvic outlet (inferior pelvic aperture): bounded by the coccyx posteriorly, ischial tuberosities laterally, and pubic symphysis anteriorly. It is closed by the pelvic floor.
True vs. False Pelvis
- False (greater) pelvis: above the pelvic inlet; part of the abdominal cavity, contains lower abdominal viscera
- True (lesser) pelvis: below the pelvic inlet; contains the pelvic viscera (bladder, rectum, reproductive organs)
Sexual Dimorphism
| Feature | Female | Male |
|---|---|---|
| Pelvic inlet | Round/oval (gynecoid) | Heart-shaped |
| Pelvic outlet | Wider | Narrower |
| Subpubic angle | >80° (often ~100°) | ~70° |
| Sacrum | Shorter, broader, less curved | Longer, narrower, more curved |
| Overall shape | Shallow and wide | Deep and narrow |
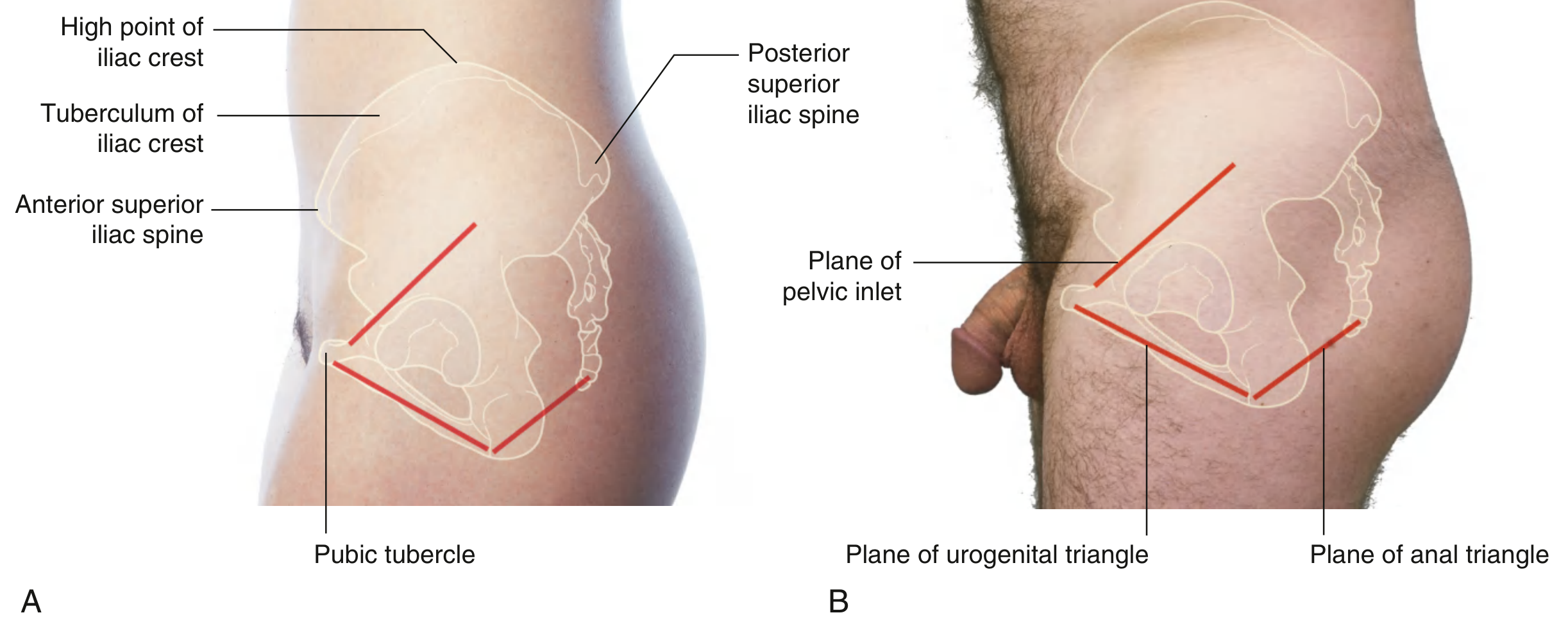
2. Joints of the Pelvis
- Pubic symphysis: secondary cartilaginous (fibrocartilaginous) joint; slightly mobile, especially in pregnancy
- Sacroiliac (SI) joints: synovial joints anteriorly, syndesmosis posteriorly; transmit trunk weight to the lower limbs
- Sacrococcygeal joint: fibrocartilaginous; slight flexion/extension
Ligaments
- Sacrotuberous ligament: sacrum/coccyx → ischial tuberosity; converts the greater and lesser sciatic notches into foramina
- Sacrospinous ligament: sacrum → ischial spine; landmark for pudendal nerve block
- Iliolumbar ligament: L4–L5 transverse processes → iliac crest; stabilises the lumbosacral junction
3. Pelvic Walls and Floor
Lateral Wall Muscles
| Muscle | Origin | Insertion | Action |
|---|---|---|---|
| Obturator internus | Inner surface of obturator membrane | Greater trochanter | Lateral rotation of thigh |
| Piriformis | Anterior sacrum | Greater trochanter | Lateral rotation; abduction of flexed thigh |
Both help form the lateral walls of the pelvic cavity and serve as important landmarks for pelvic nerves and vessels.
Pelvic Diaphragm (Pelvic Floor)
The pelvic diaphragm is a hammock-shaped musculofascial sheet that closes the pelvic outlet (except for the urogenital hiatus anteriorly). It consists of:
Levator ani — the most important component, made of three parts:
- Puborectalis: origin — superior pubic ramus on both sides; insertion — loops around the anorectal junction, forming the anorectal angle (~90°); critical for fecal continence; innervation — pudendal nerve and sacral plexus (S2–S4)
- Pubococcygeus: pubis → anococcygeal ligament and coccyx; innervation — pudendal nerve (S2–S4)
- Iliococcygeus: tendinous arch of the obturator fascia → iliococcygeal raphe and coccyx; innervation — pudendal nerve (S2–S4)
Coccygeus (ischiococcygeus): ischial spine → inferior sacrum and coccyx; innervation — sacral plexus (S4–S5); completes the pelvic diaphragm posteriorly
Function of the pelvic diaphragm: supports pelvic organs against intra-abdominal pressure; controls urinary/fecal continence; contributes to the birth canal during labour.
4. Pelvic Viscera
Urinary Bladder
- Lies in the retropubic space (space of Retzius) posterosuperior to the pubic symphysis
- Has four parts: apex, body, fundus, and neck
- The neck is continuous with the urethra; in males, it is closely related to the prostate
- Peritoneum covers the superior surface; the posterior surface is separated from the rectum (in males) by the rectovesical pouch or from the uterus (in females) by the vesicouterine pouch
Urethra
- Female urethra: ~4 cm long; short, straight course inferiorly through the pelvic floor directly into the perineum (vestibule)
- Male urethra: ~20 cm long; divided into prostatic, membranous, and spongy portions; passes through the prostate, the deep perineal pouch/perineal membrane, and then through the erectile tissues of the penis. Has a fixed anterior angle at the perineal membrane and a mobile angle in the penile shaft
Rectum and Anal Canal
- The rectum begins at the rectosigmoid junction (S3 level) and follows the sacral curve
- Three lateral flexures create the Houston's valves
- The rectum becomes the anal canal as it passes through the pelvic floor; the anorectal angle (~90°) maintained by puborectalis is key for continence
- The anal canal has an internal anal sphincter (smooth muscle; involuntary) and external anal sphincter (striated; voluntary; innervated by pudendal nerve S2–S4)
Reproductive Organs
Male:
- Prostate: sits at the neck of the bladder, encircles the urethra; ~3 cm long; has three zones (peripheral, central, transitional); surrounded by a fascial capsule; closely related to the rectum posteriorly (basis of digital rectal exam)
- Seminal vesicles: lie posterior to the bladder, superior to the prostate; join with the vas deferens to form the ejaculatory ducts which pass through the prostate to open into the prostatic urethra at the verumontanum
- Vas deferens: enters the pelvis via the deep inguinal ring, crosses the ureter ("water under the bridge"), and joins the seminal vesicle
Female:
- Uterus: lies in the lesser pelvis between the bladder and rectum; consists of fundus, body, isthmus, and cervix; normally anteverted and anteflexed; supported by the broad, round, uterosacral, and cardinal ligaments
- Broad ligament: a double layer of peritoneum flanking the uterus; contains the fallopian tube (in the mesosalpinx), the round ligament (in the mesometrium), and the ovary (attached by the mesovarium)
- Uterosacral ligaments: uterine cervix → sacrum; maintain cervical position
- Cardinal ligaments (Mackenrodt's): cervix/upper vagina → lateral pelvic wall; main support against uterine prolapse
- Ovaries: lie in the ovarian fossa (lateral pelvic wall, below the bifurcation of the common iliac artery); attached to the uterus by the ovarian ligament and to the pelvic wall by the suspensory ligament of the ovary (infundibulopelvic ligament), which carries the ovarian vessels
5. Pelvic Blood Supply
Arteries
The internal iliac artery (hypogastric artery) is the main supply to the pelvic viscera and walls. It arises from the common iliac artery at the level of the sacroiliac joint (L4–L5 disc level) and divides into:
Anterior division:
- Superior vesical artery → upper bladder, proximal ureter
- Inferior vesical artery (males) / vaginal artery (females) → bladder base, prostate/vagina
- Obturator artery → medial thigh muscles
- Internal pudendal artery → perineum (crosses through lesser sciatic foramen, runs in Alcock's canal)
- Inferior gluteal artery → gluteal muscles
- Uterine artery (females) → uterus; crosses the ureter at the base of the broad ligament ("water under the bridge")
- Middle rectal artery → middle rectum
Posterior division:
- Iliolumbar artery
- Lateral sacral arteries
- Superior gluteal artery (largest branch)
The ovarian/testicular arteries arise directly from the aorta (L2 level) and enter the pelvis via the infundibulopelvic ligament.
Venous Drainage
- Pelvic venous plexuses (vesical, prostatic, uterovaginal, rectal) drain into the internal iliac veins
- The prostatic venous plexus (of Santorini) connects with the vertebral venous plexus — a route for prostate cancer metastasis
6. Pelvic Nerves
Lumbosacral Plexus
Formed by anterior rami of L4–S3; gives rise to:
- Femoral nerve (L2–L4) — exits through greater sciatic foramen
- Obturator nerve (L2–L4) — exits through obturator canal
- Sciatic nerve (L4–S3) — largest nerve; exits below piriformis through greater sciatic foramen
- Superior gluteal nerve (L4–S1) — above piriformis
- Inferior gluteal nerve (L5–S2) — below piriformis
- Posterior cutaneous nerve of the thigh (S1–S3)
Pudendal Nerve (S2–S4)
The principal nerve of the perineum:
- Exits the pelvic cavity through the greater sciatic foramen (below piriformis)
- Crosses the ischial spine (landmark for pudendal block)
- Re-enters through the lesser sciatic foramen
- Runs in the pudendal canal (Alcock's canal) on the lateral wall of the ischiorectal fossa
- Branches: inferior rectal nerve, perineal nerve (superficial and deep branches), dorsal nerve of the penis/clitoris
Autonomic Innervation
- Sympathetic: presacral nerve (superior hypogastric plexus) → hypogastric nerves → inferior hypogastric plexus; controls ejaculation, vasoconstriction
- Parasympathetic: pelvic splanchnic nerves (S2–S4, "nervi erigentes") → inferior hypogastric plexus; controls erection, bladder detrusor contraction, rectal emptying
- Inferior hypogastric (pelvic) plexus: paired plexuses on the lateral pelvic wall integrating sympathetic + parasympathetic input to all pelvic viscera
7. The Perineum
The perineum is the region inferior to the pelvic floor, between the thighs and buttocks. It is diamond-shaped and bounded by:
- Anteriorly: pubic symphysis
- Laterally: ischiopubic rami and ischial tuberosities
- Posteriorly: tip of the coccyx
A transverse line between the two ischial tuberosities divides it into two triangles.
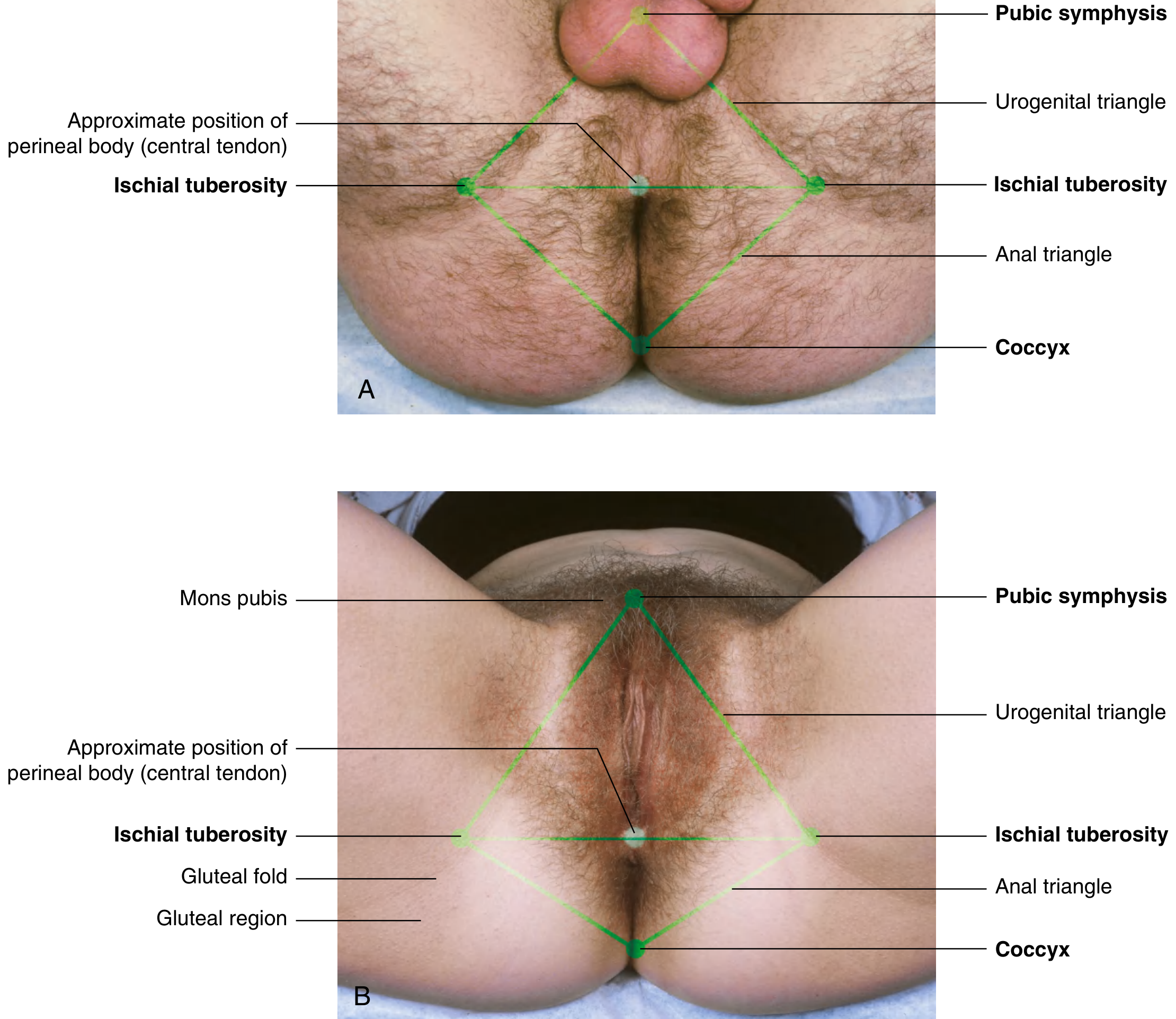
7a. Anal Triangle
- Boundaries: transverse line between ischial tuberosities (base), coccyx (apex), sacrotuberous ligaments (sides)
- Contents: anal aperture (anal canal), ischioanal (ischiorectal) fossa on each side
- Ischioanal fossa: fat-filled wedge-shaped space bounded medially by the pelvic diaphragm, laterally by the obturator internus fascia. Contains the pudendal canal (with pudendal nerve and internal pudendal vessels). The fat allows expansion of the anal canal during defecation. Infections here → perianal abscess/fistula.
7b. Urogenital Triangle
- Boundaries: pubic symphysis (apex), ischial tuberosities (base), ischiopubic rami (sides)
- Contains the perineal membrane and the perineal pouches
Perineal Membrane
A tough fibromuscular sheet that spans the anterior perineum. It is pierced in males by the urethra; in females by the urethra and vagina.
Superficial Perineal Pouch (below the perineal membrane)
Contains the superficial perineal muscles and the erectile tissues:
| Structure | Male | Female |
|---|---|---|
| Ischiocavernosus | Covers crura of penis; maintains erection | Covers crura of clitoris |
| Bulbospongiosus | Surrounds corpus spongiosum; assists ejaculation | Covers vestibular bulb; narrows vaginal introitus |
| Superficial transverse perineal | Ischial tuberosity → perineal body | Ischial tuberosity → perineal body |
| Erectile tissue | Corpora cavernosa + corpus spongiosum | Clitoris + vestibular bulbs |
| Glands | Bulbourethral (Cowper's) glands (in deep pouch) | Greater vestibular (Bartholin's) glands |
All superficial perineal muscles are innervated by the perineal branch of the pudendal nerve (S2–S4).
Deep Perineal Pouch (above the perineal membrane, within the urogenital diaphragm)
Contains:
- Deep transverse perineal muscle: stabilises the perineal body
- Sphincter urethrae (external urethral sphincter): voluntary control of micturition
- In males: bulbourethral (Cowper's) glands open into the spongy urethra
- In females: sphincter urethrovaginalis surrounds both urethra and vagina
- Urethra (and vagina in females) pass through this space
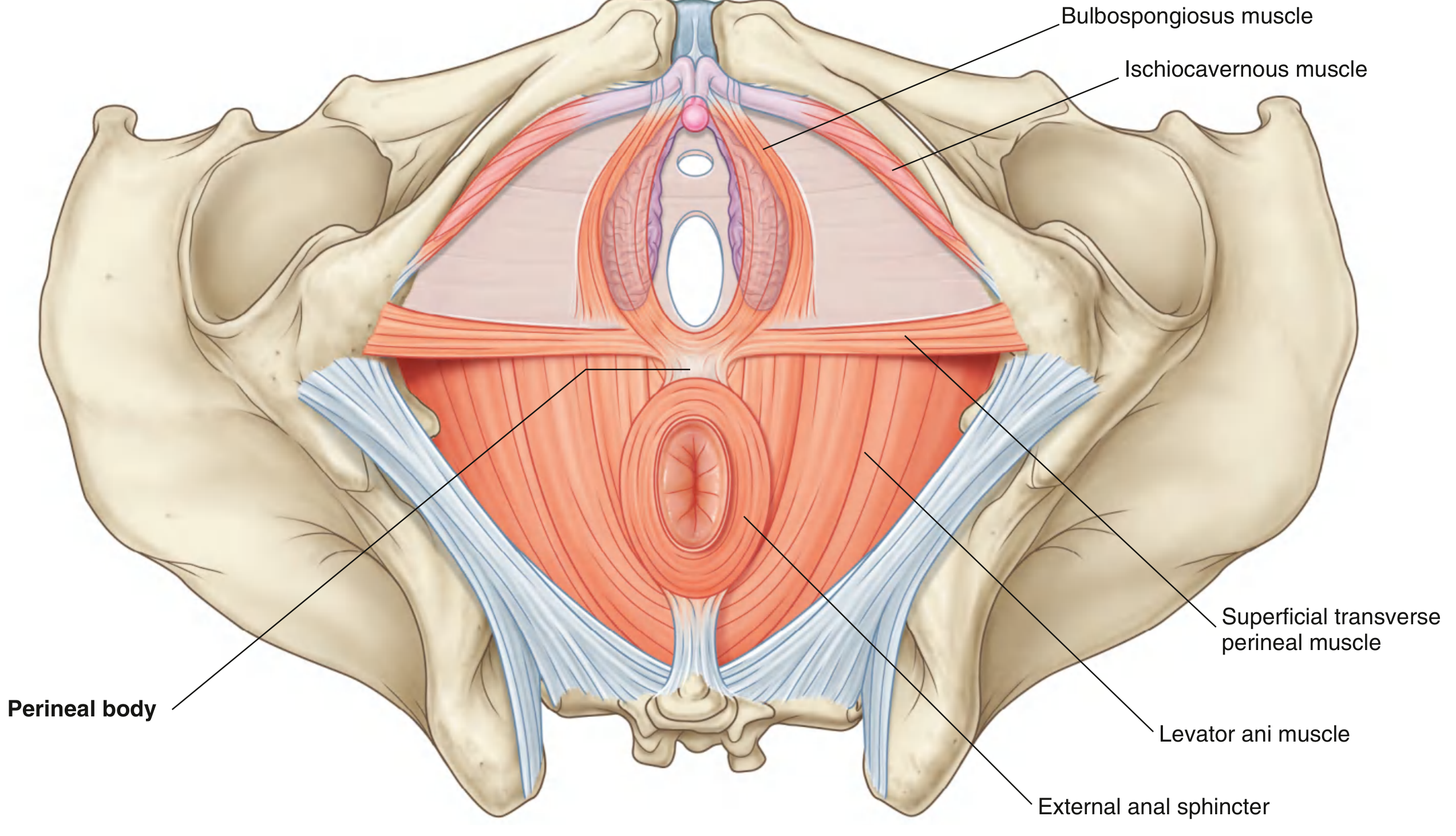
7c. Perineal Body (Central Tendon of the Perineum)
A poorly defined fibromuscular node at the midpoint of the transverse line between the ischial tuberosities. It is the critical structural crossroads of the perineum where the following converge:
- Levator ani (pelvic diaphragm)
- Bulbospongiosus
- Superficial and deep transverse perineal muscles
- External anal sphincter
- (in females) perineal fibers of the rectovaginal septum
The perineal body is critical for pelvic floor integrity. Its disruption during childbirth (perineal tear or episiotomy) can lead to pelvic organ prolapse and fecal/urinary incontinence.
7d. External Genitalia
Male:
- Penis: composed of two corpora cavernosa (dorsal; erectile) and corpus spongiosum (ventral; contains urethra); covered by skin
- Scrotum: contains testes, epididymides, spermatic cords; temperature regulation via the cremaster muscle
- Root of the penis: anchored in the perineum (crura, attached to ischiopubic rami; bulb, attached to perineal membrane)
Female (Vulva):
- Mons pubis: fatty elevation over the pubic symphysis
- Labia majora: homologous to the male scrotum
- Labia minora: enclose the vestibule
- Vestibule: space into which the urethra and vagina open; contains the openings of the greater vestibular (Bartholin's) glands
- Clitoris: erectile structure (two crura + glans); homologous to the penis; highly innervated by the dorsal nerve of the clitoris
8. Dissection Image — Superficial Perineal Muscles (Male)
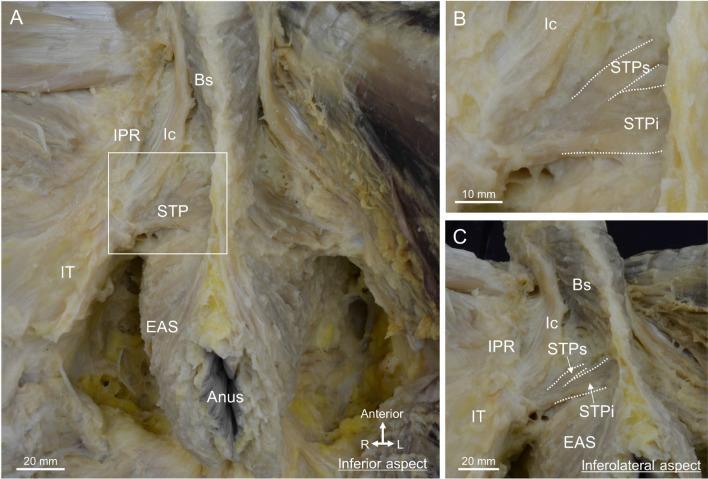
Summary: Pelvic Floor Muscles at a Glance
| Muscle | Origin | Insertion | Innervation | Function |
|---|---|---|---|---|
| Puborectalis | Superior pubic ramus (bilateral) | Loop around anorectal junction | Pudendal / S2–S4 | Maintains anorectal angle; continence |
| Pubococcygeus | Pubis (lateral) | Anococcygeal ligament, coccyx | Pudendal / S2–S4 | Supports pelvic floor |
| Iliococcygeus | Tendinous arch of obturator fascia | Iliococcygeal raphe, coccyx | Pudendal / S2–S4 | Supports pelvic floor |
| Coccygeus | Ischial spine | Inferior sacrum, coccyx | S4–S5 | Flexes coccyx; supports floor |
| Ext. anal sphincter | Anococcygeal ligament | Perineal body | Pudendal / S2–S4 | Voluntary fecal continence |
| Ext. urethral sphincter | Perineal membrane | Encircles urethra | Pudendal / S2–S4 | Voluntary urinary continence |
| Bulbospongiosus | Perineal body | Penile raphe / clitoris | Pudendal / S2–S4 | Ejaculation; narrows introitus |
| Ischiocavernosus | Ischiopubic ramus | Corpus cavernosum | Pudendal / S2–S4 | Maintains erection |
| Superficial transverse perineal | Ischial tuberosity | Perineal body | Pudendal / S2–S4 | Stabilises perineal body |
| Deep transverse perineal | Ischiopubic ramus | Perineal body | Pudendal / S2–S4 | Stabilises perineal body |
Clinical Correlates
| Condition | Anatomical Basis |
|---|---|
| Pudendal nerve block | Injection near sacrospinous ligament at the ischial spine; anesthetises the entire perineum |
| Episiotomy | Incision of the perineal body during childbirth; must avoid injuring the external anal sphincter |
| Pelvic organ prolapse | Weakness of levator ani and cardinal/uterosacral ligaments; uterus, bladder, or rectum may herniate into vagina |
| Benign prostatic hyperplasia | Enlargement of the transitional zone of prostate; compresses urethra |
| Ectopic ureter | Ureter opens distal to the internal urethral sphincter → incontinence |
| Perianal abscess | Infection of the ischioanal fat pad |
| Ureteric injury in surgery | Most common site: where uterine artery crosses over the ureter near the cervix ("water under the bridge") |
Sources: Gray's Anatomy for Students (Elsevier, 9780323934237), THIEME Atlas of Anatomy: General Anatomy & Musculoskeletal System (9781626237186), Campbell-Walsh-Wein Urology (9780323546423)
Convert it into hand written notes or downloadable file format
Reading File
Running Command
Running Command
Running Command
Running Command
Writing File
You've run out of free credits. Sign up for a free account to continue using Orris.
This is a shared conversation. Sign in to Orris to start your own chat.