Left eyelid hordeolum or stye ... Write a prescription mention eye hygiene alongside the medication and if system antibiotic needed or not .
Reading File
Finding Sources
Finding Sources
Searching PubMed
hordeolum stye treatment management
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Reading File
Loading Image
I have all the information needed. Here is the complete clinical write-up:
External Hordeolum (Stye) — Left Eyelid
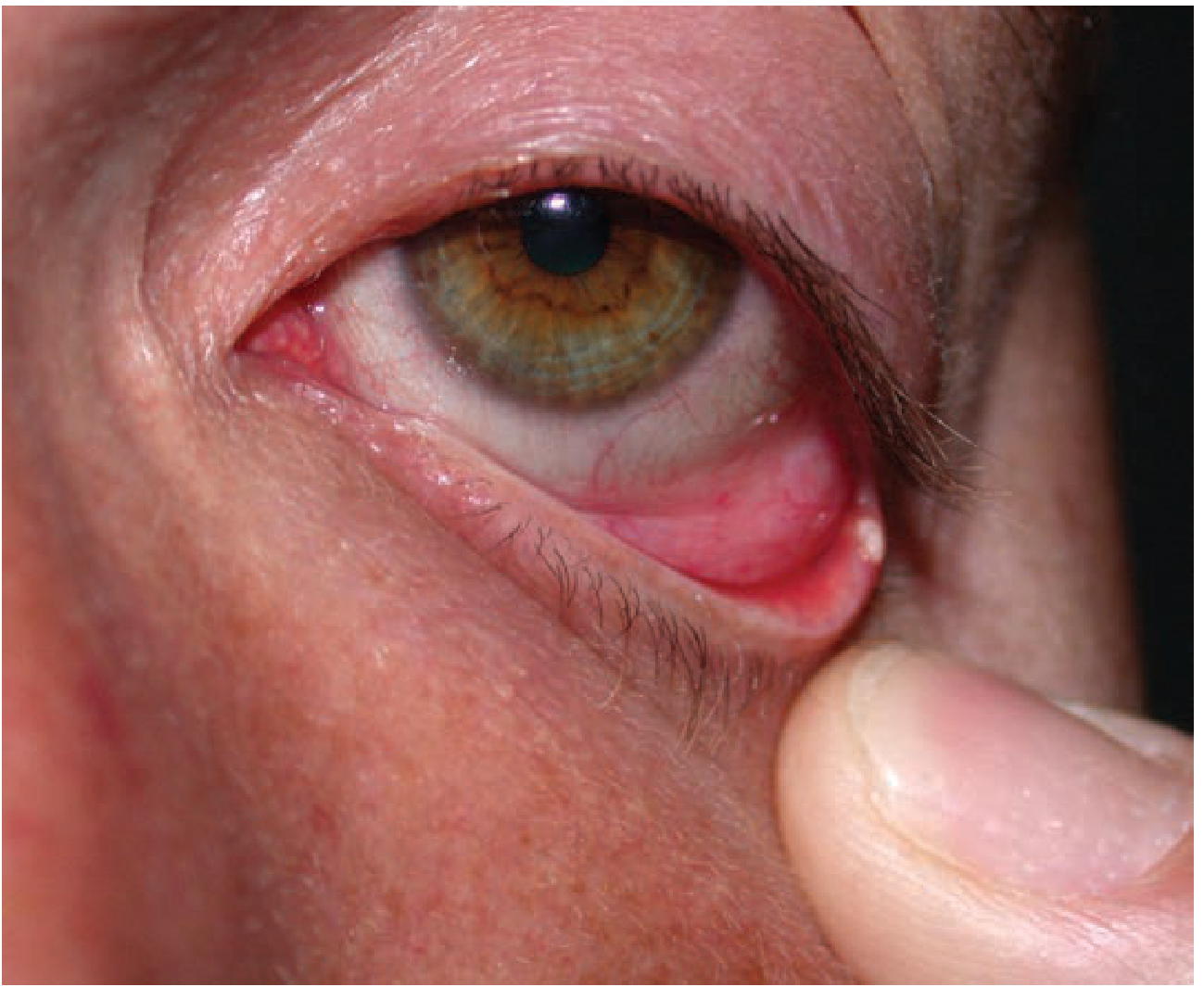
Background
A hordeolum is an acute staphylococcal abscess of the eyelid glands:
- External hordeolum (stye) — abscess of a lash follicle and the glands of Zeis or Moll; presents as a tender pustule at the eyelid margin
- Internal hordeolum — abscess of a meibomian gland; pustule visible on the inner tarsal surface
The typical organism is Staphylococcus aureus. It can occasionally evolve into preseptal cellulitis if untreated.
📋 Prescription
Patient: __________________ Date: 12/05/2026
Diagnosis: External hordeolum (stye) — Left upper/lower eyelid (circle one)
Rx
1. Erythromycin ophthalmic ointment 0.5%
Apply a thin ribbon to the left eyelid margin
b.i.d. × 10 days
(Alternative: Bacitracin oint. 500 units/g — or — Tobramycin oint. 0.3% b.i.d. × 10 days)
Antibiotic ointment is preferred over drops for hordeolum because it prolongs contact time at the eyelid margin.
🧼 Eye Hygiene Instructions (Non-Negotiable — First-Line Therapy)
| Step | Instruction |
|---|---|
| Warm compresses | Apply a clean warm (not hot) compress to the closed left eye for 10–15 minutes, 4× per day (q.i.d.). Reheat the cloth as needed to maintain warmth throughout. This is the single most important step — it softens the secretion and promotes spontaneous drainage. |
| Gentle massage | After each warm compress, gently massage over the lesion toward the eyelid margin with a clean fingertip to encourage drainage. |
| Lid scrubs | Using a cotton swab or clean lint-free pad moistened with dilute baby shampoo (1 drop in 1 cup of cooled boiled water) or commercial lid-scrub pads (e.g., Sterilid, OcuSoft), gently scrub along the base of the lashes once daily. This removes crust, bacteria, and debris. |
| No squeezing | Do not attempt to squeeze or puncture the stye — this risks spreading the infection. |
| No eye make-up | Avoid eyeliner, mascara, and eye shadow on the affected eye until fully resolved. Discard any eye cosmetics used around the time of infection. |
| No contact lenses | Avoid contact lens wear until the lesion resolves. |
| Hand hygiene | Wash hands thoroughly before and after touching the eye area. |
| Do not share | No sharing of towels, pillowcases, or face cloths with others during the infection. |
⚕️ Systemic Antibiotics — Are They Needed?
In the uncomplicated external hordeolum: NO systemic antibiotics are indicated.
Warm compresses + topical antibiotic ointment are sufficient in the vast majority of cases. Systemic antibiotics are reserved exclusively for the following situations:
| Situation | Action |
|---|---|
| Significant surrounding preseptal (periorbital) cellulitis (eyelid erythema spreading beyond the stye, diffuse warmth, edema) | Oral antibiotics indicated — e.g., Amoxicillin-clavulanate 875/125 mg p.o. b.i.d. × 7 days, or Clindamycin 300 mg t.i.d. × 7 days if penicillin-allergic |
| Recurrent or multiple hordeola, or associated ocular rosacea / blepharitis | Consider doxycycline 20–50 mg p.o. daily (low-dose, for anti-inflammatory and antibacterial effect) — long-term use under specialist supervision |
| Failed medical therapy after 2–3 weeks / abscess not draining | Refer to ophthalmologist for incision and drainage (I&D) — do not attempt in primary care |
| Systemic signs (fever, lymphadenopathy, immunocompromise) | Escalate to systemic antibiotics + ophthalmology referral |
⚠️ Note: Tetracyclines (doxycycline) are contraindicated in pregnancy, nursing women, and children ≤8 years.
Follow-Up
- Review in 2–3 weeks if no improvement
- Urgent review if spreading erythema, fever, or visual change — to rule out preseptal/orbital cellulitis
- Persistent nodule after 4 weeks → refer ophthalmology for possible intralesional triamcinolone injection or incision and curettage (I&C)
- Recurrent or atypical chalazion/hordeolum in older patients → pathology specimen to exclude sebaceous carcinoma
Prescriber: __________________ Signature: __________________
Sources: The Wills Eye Manual 7th ed., §6.2; Tintinalli's Emergency Medicine 9th ed., Ch. 241; Goodman & Gilman's Pharmacological Basis of Therapeutics; Rosen's Emergency Medicine 9th ed., Ch. 57
2
Asking for Preferences
The user likely means the internal hordeolum (meibomian gland abscess) — which was listed as point #2 in the previous answer. Here is the prescription for that:
Internal Hordeolum — Left Eyelid
(Acute staphylococcal abscess of the meibomian gland — pustule on the inner tarsal surface)
Patient: __________________ Date: 12/05/2026
Diagnosis: Internal hordeolum — Left eyelid
Rx
1. Erythromycin ophthalmic ointment 0.5%
Apply to the left eyelid margin (and inner lid if tolerated)
b.i.d. × 10 days
(Alternative: Tobramycin 0.3% ointment b.i.d. × 10 days — or — Bacitracin 500 units/g ointment b.i.d. × 10 days)
Internal hordeola sit deeper within the tarsal plate (meibomian gland), so topical antibiotic penetration is limited — warm compresses and massage are especially critical.
🧼 Eye Hygiene Instructions
| Step | Instruction |
|---|---|
| Warm compresses | Clean warm compress over the closed left eye, 10–15 minutes q.i.d. Reheat the cloth frequently to maintain adequate warmth throughout each session. |
| Firm massage | After each compress, press and massage the eyelid firmly (from the outer skin surface) toward the lid margin to express the gland contents. This is particularly important for internal hordeola since the duct opens onto the inner lid. |
| Lid scrubs | Once daily: clean the lash line with a cotton-tipped applicator moistened with diluted baby shampoo or commercial lid-scrub pads (OcuSoft/Sterilid). |
| No squeezing | Do not attempt self-drainage — the tarsal plate is rigid and uncontrolled pressure risks rupture into the orbit. |
| No eye make-up | Avoid all eye cosmetics until fully resolved. Discard any previously used eye cosmetics. |
| No contact lenses | Stop contact lens wear until resolution. |
| Hand hygiene | Wash hands before and after any lid contact. |
⚕️ Systemic Antibiotics
Routine uncomplicated internal hordeolum: NOT required.
Internal hordeola are managed identically to external ones — warm compresses + topical antibiotics are the standard of care.
Systemic antibiotics are indicated only if:
| Condition | Regimen |
|---|---|
| Spreading preseptal cellulitis (diffuse lid erythema, edema, warmth beyond the lesion) | Amoxicillin-clavulanate 875/125 mg p.o. b.i.d. × 7 days |
| Penicillin allergy | Clindamycin 300 mg p.o. t.i.d. × 7 days |
| Recurrent lesions or associated ocular rosacea | Doxycycline 100 mg p.o. b.i.d. × 1–2 weeks, then taper to 20–50 mg daily (long-term, under specialist care) — contraindicated in pregnancy, nursing, and children ≤8 years |
| Systemic signs (fever, lymphadenopathy, immunocompromise) | Systemic antibiotics + urgent ophthalmology referral |
Follow-Up & Escalation
- Review in 2–3 weeks if no improvement
- Eyelid eversion + slit lamp exam to confirm diagnosis and locate the internal pointing of the abscess
- No resolution after 3–4 weeks → refer ophthalmology for incision and drainage from the inner tarsal surface (performed under local anaesthesia — the approach is from the conjunctival side to avoid skin scarring)
- Recurrent or atypical lesion in an older patient → biopsy to exclude sebaceous carcinoma
- Signs of preseptal/orbital spread (proptosis, restricted eye movement, pain on eye movement, visual change) → urgent ophthalmology referral same day
Prescriber: __________________ Signature: __________________
Sources: The Wills Eye Manual 7th ed. §6.2; Tintinalli's Emergency Medicine 9th ed. Ch. 241; Goodman & Gilman's Pharmacological Basis of Therapeutics; Rosen's Emergency Medicine 9th ed. Ch. 57
Create a patient education handout on stye care and prevention
Reading File
Running Command
Running Command
Writing File
Running Command
Running Command
Running Command
The file is valid. Here it is:
Stye Patient Education Handout
Word Document · DOCX
The handout is a fully formatted, colour-coded single-page Word document. Here's what's inside:
| Section | Content |
|---|---|
| What is a Stye? | Plain-language explanation + two-column box distinguishing external vs internal hordeolum |
| Symptoms | Bulleted checklist of what to expect |
| Home Care Steps | Numbered icon-table: warm compress → massage → lid scrubs → antibiotic ointment with full instructions per step |
| What NOT to Do | Red-highlighted table — no squeezing, no make-up, no contact lenses |
| Prevention | Sub-sections on hand hygiene, cosmetic hygiene, contact lens care, daily lid hygiene |
| When to See a Doctor Urgently | Red alert box with red-flag warning signs |
| Key Reminders | Yellow summary box with 5 take-home points |
| Footer | Date + textbook sources |
Designed to be printed on A4 and handed to patients directly. Let me know if you'd like any changes — language level, language translation, logo, clinic name, or additional content.
Left upper eyelid external hordeolum or stye ... Write a prescription mention eye hygiene alongside the medication
Based on the authoritative sources already in context (Wills Eye Manual §6.2, Tintinalli's, Goodman & Gilman's), here is the focused prescription:
📋 PRESCRIPTION
| Patient: | _________________________________ |
| Date: | 12 / 05 / 2026 |
| Diagnosis: | External hordeolum (stye) — Left upper eyelid |
| Organism: | Staphylococcus aureus (typical) |
℞ MEDICATION
Erythromycin Ophthalmic Ointment 0.5%
Apply a thin ribbon along the left upper eyelid margin
Twice daily (b.i.d.) — morning and at bedtime — × 10 days
Disp: 1 tube (3.5 g)
How to apply: Wash hands. Gently pull down the lower lid. Squeeze a small ribbon (~1 cm) of ointment into the conjunctival sac. Blink to spread. Expect mild blurring for 1–2 minutes — this is normal.
Alternatives (if erythromycin unavailable):
- Bacitracin ointment 500 units/g — b.i.d. × 10 days, OR
- Tobramycin ophthalmic ointment 0.3% — b.i.d. × 10 days
🧼 EYE HYGIENE — Written on the Prescription (Mandatory)
Hygiene is co-equal to medication — the antibiotic ointment alone is insufficient without these measures.
1. Warm Compresses — 4× daily (q.i.d.)
Soak a clean cloth in warm (not hot) water. Apply over the closed left eye for 10–15 minutes. Reheat the cloth every 2–3 minutes to maintain warmth throughout. This softens the blocked gland and promotes natural drainage. Perform before applying the ointment each session.
2. Gentle Massage — after each warm compress
With a clean fingertip, gently press and massage the left upper eyelid toward the lash margin to encourage the gland to drain.
3. Eyelid Margin Scrub — once daily
Using a cotton-tipped applicator moistened with diluted baby shampoo (1 drop in a cup of cooled boiled water) or commercial lid-scrub pads (OcuSoft / Sterilid), gently scrub along the base of the upper lashes.
4. Hand hygiene — wash hands thoroughly before and after all eye contact.
5. No squeezing — do not attempt to pop or puncture the stye.
6. Cosmetics & lenses — avoid eye make-up and contact lenses on the affected eye until fully healed. Discard any mascara or eyeliner used around the time of onset.
⚕️ SYSTEMIC ANTIBIOTICS
Not required for this uncomplicated external hordeolum.
Prescribe systemic antibiotics only if preseptal cellulitis develops (spreading eyelid erythema, diffuse warmth, fever) — in that event: Amoxicillin-clavulanate 875/125 mg p.o. b.i.d. × 7 days (or Clindamycin 300 mg t.i.d. if penicillin-allergic).
🔁 FOLLOW-UP & ESCALATION
| Timeframe | Action |
|---|---|
| 2–3 weeks | Review if no improvement |
| Not resolved at 4 weeks | Refer ophthalmology — intralesional triamcinolone injection or incision & drainage (I&D) |
| Any time — spreading redness, fever, restricted eye movement, visual change | Urgent same-day ophthalmology referral → rule out preseptal/orbital cellulitis |
Prescriber: _________________________ Signature: _________________________
Sources: The Wills Eye Manual 7th ed. §6.2; Tintinalli's Emergency Medicine 9th ed. Ch. 241; Goodman & Gilman's Pharmacological Basis of Therapeutics
This is a shared conversation. Sign in to Orris to start your own chat.