Chronic renal failure
Reading File
Finding Sources
Finding Sources
Searching PubMed
"chronic kidney disease" management
Reading File
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
Reading File
Reading File
Reading File
Finding Sources
Reading File
Reading File
Finding Sources
Searching Images
chronic kidney disease CKD stages pathophysiology diagram
I now have all the information needed to compile a comprehensive answer. Let me synthesize it:
Chronic Renal Failure (Chronic Kidney Disease — CKD)
Definition
Chronic kidney disease (CKD) is defined as kidney damage or decreased kidney function persisting for 3 months or longer, based on:
- Glomerular filtration rate (GFR) < 60 mL/min/1.73 m²
- Albuminuria > 30 mg/day
- Pathological, blood, urine, or imaging abnormalities
— Goldman-Cecil Medicine, p. 1342
Staging (KDIGO Classification)
| Stage | Description | GFR (mL/min/1.73 m²) |
|---|---|---|
| G1 | Kidney damage, normal GFR | ≥ 90 |
| G2 | Mild decrease | 60–89 |
| G3a | Mild-to-moderate decrease | 45–59 |
| G3b | Moderate-to-severe decrease | 30–44 |
| G4 | Severe decrease | 15–29 |
| G5 | Kidney failure (ESRD) | < 15 |
Albuminuria is staged separately: A1 (<30 mg/g), A2 (30–300 mg/g), A3 (>300 mg/g). Risk of progression and complications scales with both the GFR category and albuminuria category.
— Textbook of Family Medicine, p. 1191; Goldman-Cecil Medicine
Causes / Etiology
The most common causes worldwide:
- Diabetic nephropathy (leading cause; ~40% of ESRD)
- Hypertensive nephrosclerosis
- Glomerulonephritis (IgA nephropathy, FSGS, membranous, etc.)
- Polycystic kidney disease (ADPKD, ARPKD)
- Obstructive uropathy / chronic pyelonephritis
- Lupus nephritis / vasculitis
- Drug-induced nephrotoxicity (NSAIDs, analgesics, aminoglycosides, contrast)
- Ischemic nephropathy / renovascular disease
Non-diabetic causes should be considered even in diabetic patients if GFR declines rapidly, hypertension is refractory, active urine sediment is present, or systemic disease is suspected. — Brenner & Rector's The Kidney
Pathophysiology
Nephron Loss & Hyperfiltration
Progressive nephron loss triggers compensatory hyperfiltration in surviving nephrons (increased single-nephron GFR). This initially maintains total GFR but causes glomerular hypertension → proteinuria → further glomerulosclerosis → a self-perpetuating cycle of nephron loss. GFR is therefore a poor early indicator of disease burden; significant parenchymal loss occurs before GFR drops. — Brenner & Rector's The Kidney
Key Pathways
- Renin-angiotensin-aldosterone system (RAAS) activation → hypertension, proteinuria, fibrosis
- TGF-β → tubulointerstitial fibrosis
- Oxidative stress & inflammation → endothelial injury, cardiovascular disease
- Impaired erythropoietin production → anemia
- Phosphate retention → secondary hyperparathyroidism → renal osteodystrophy
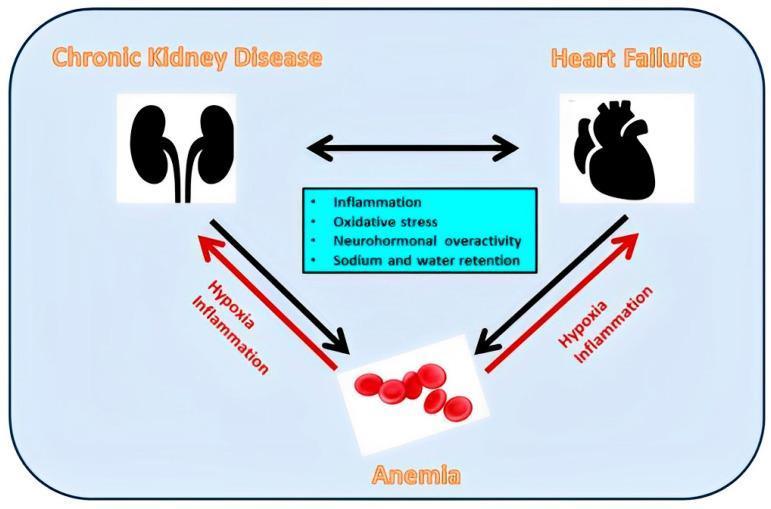
Clinical Manifestations
CKD is usually asymptomatic in early stages (G1–G2). Manifestations emerge progressively:
Stages G1–G2
- New/worsening hypertension
- Proteinuria (may cause edema in nephrotic range)
- Incidental electrolyte or urinalysis abnormalities
Stages G3–G4
- Anemia (fatigue, weakness, exertional dyspnea) — due to ↓ erythropoietin
- Renal osteodystrophy — pathologic fractures, soft-tissue/vascular calcification
- Hyperphosphatemia → elevated Ca×P product → calciphylaxis, vascular calcification → LV hypertrophy, heart failure
- Metabolic acidosis — normal anion gap at G3b; high anion gap (retained phosphate/sulfate) at G4–G5
- Hyperkalemia — especially with RAAS blockade; mild (5.0–5.5 mEq/L) to severe (>6.5 mEq/L) at advanced stages
- Malnutrition / muscle and fat wasting
- Sexual dysfunction — amenorrhea, impotence, oligospermia
Stage G5 — Uremic Syndrome (GFR <15 mL/min/1.73 m²)
- Fluid overload / hypertension
- Peripheral neuropathy
- Pruritus (uremic)
- Pericarditis (uremic)
- GI symptoms — nausea, vomiting, anorexia
- Encephalopathy — altered mental status, seizures
- Increased infection risk
— Goldman-Cecil Medicine, pp. 1342–1343
Diagnosis
Systematic evaluation includes:
- Serum creatinine + eGFR (CKD-EPI equation preferred; MDRD also used)
- Urine albumin-to-creatinine ratio (ACR)
- Complete urinalysis (casts, hematuria, proteinuria)
- Renal ultrasound (size, echogenicity, obstruction, cysts)
- Serum electrolytes, bicarbonate, CBC, PTH, phosphate, calcium
- HbA1c if diabetic etiology suspected
- Complement, ANA, ANCA if glomerulonephritis suspected
- Kidney biopsy — when etiology is uncertain and affects management
Key point: Serum creatinine alone is inadequate — a "normal" creatinine may correspond to substantially reduced GFR in older patients, women, or those with low muscle mass. — Textbook of Family Medicine, p. 1192
Management
Principles
Management is cause-specific + stage-based, cumulative across stages. — Goldman-Cecil Medicine, p. 1341
Lifestyle & Diet
- Sodium restriction (<2 g/day) for hypertension
- Protein intake: 0.6–0.8 g/kg/day at G3–G5 (slows solute retention, may slow progression)
- Total calories: 25–35 kcal/kg/day (prevent protein-calorie malnutrition)
- Mediterranean/DASH diet; tobacco cessation; physical activity
- Registered dietitian involvement is essential
Blood Pressure Control
- Target SBP <130 mmHg (some guidelines recommend <120 mmHg)
- ACE inhibitor or ARB — first-line for albuminuria with or without diabetes; reduces albuminuria and slows GFR decline
- Add diuretics or calcium-channel blockers as needed
- Finerenone (non-steroidal mineralocorticoid receptor antagonist) — effective in diabetic CKD with albuminuria (20 mg/day if eGFR >60; 10 mg/day if eGFR 25–59)
SGLT2 Inhibitors & GLP-1 Agonists
SGLT2 inhibitors (canagliflozin 100 mg, dapagliflozin 5 mg, empagliflozin 10 mg daily) reduce albuminuria, slow GFR decline, and reduce risk of kidney failure and cardiovascular events — in both diabetic and non-diabetic CKD with albuminuria. GLP-1 agonists also reduce albuminuria in type 2 diabetes. — Goldman-Cecil Medicine, p. 1343
Glycemic Control
- HbA1c target similar to non-CKD diabetes; may be less strict in elderly/comorbid patients
Lipid-Lowering Therapy
- Statins recommended (cardiovascular benefit); however, no direct benefit on CKD progression
Management of Specific Complications
| Complication | Target | Treatment |
|---|---|---|
| Anemia | Hb 90–110 g/L | Treat iron deficiency first; then erythropoiesis-stimulating agents (ESA, e.g., darbepoetin alpha 0.45 μg/kg q4 weeks) when Hb <9 g/dL; HIF-stabilizers (non-US approved for pre-dialysis) |
| Metabolic acidosis | Bicarbonate >22 mmol/L | Sodium bicarbonate 650 mg BD, titrate to target |
| Metabolic bone disease / Secondary HPT | Ca 2.2–2.35, PO₄ <1.8 mmol/L | Phosphate binders; active vitamin D (calcitriol 0.25–0.5 μg/day); calcimimetics (cinacalcet 30 mg/day) on dialysis; parathyroidectomy if refractory |
| Hyperkalemia >5.5 mEq/L | K <5.5 mEq/L | Dietary restriction (<2 g/day K); potassium-binding agents; loop diuretics; insulin/glucose for acute elevations; dialysis if severe |
| Malnutrition | Adequate intake | Dietitian support; 25–35 kcal/kg/day |
| Edema (nephrotic) | — | Diuretics ± albumin infusion if refractory |
— Comprehensive Clinical Nephrology 7th Ed., p. 1123; Goldman-Cecil Medicine, pp. 1343–1345
Referral to Nephrology
Refer when:
- eGFR < 30 mL/min/1.73 m² (stage G4–G5)
- ACR ≥ 300 mg/g (A3)
- Rapid progression (sustained GFR drop >5 mL/min/1.73 m²/year or change of GFR category)
- Unexplained hematuria, resistant hypertension, persistent K abnormalities, hereditary kidney disease
— Comprehensive Clinical Nephrology 7th Ed., Box 82.1
Kidney Replacement Therapy (Stage G5)
When conservative care no longer controls uremic symptoms:
- Hemodialysis — most common; thrice-weekly; high risk of cardiovascular complications
- Peritoneal dialysis — home-based; continuous or intermittent
- Kidney transplantation — preferred; extends life and quality of life over dialysis
Shared decision-making and advance care planning should begin well before uremia develops. — Goldman-Cecil Medicine, p. 1345
Prevention
- Primary: Treat hypertension, diabetes, obesity; avoid nephrotoxic drugs; healthy lifestyle
- Secondary: Early detection via ACR + eGFR screening in at-risk patients (diabetics, hypertensives, family history of CKD); RAAS blockade and SGLT2 inhibition to slow progression
- Tertiary: Prevent cardiovascular complications (leading cause of death in CKD)
Key Points to Remember
- CKD is defined by persistence >3 months — acute kidney injury can mimic CKD until chronicity is established.
- Serum creatinine is unreliable alone — eGFR and ACR together define risk.
- Cardiovascular disease is the #1 cause of death in CKD, not kidney failure.
- SGLT2 inhibitors are now established as kidney-protective in both diabetic and non-diabetic CKD with albuminuria.
- ESAs should target Hb 10–11 g/dL only — higher targets worsen cardiovascular outcomes.
- Avoid NSAIDs, iodinated contrast, gadolinium, and other nephrotoxins.
Sources: Goldman-Cecil Medicine (22nd Ed.); Comprehensive Clinical Nephrology (7th Ed.); Brenner & Rector's The Kidney; Textbook of Family Medicine (9th Ed.)
This is a shared conversation. Sign in to Orris to start your own chat.