Hydronephrosis treatment
Reading File
Finding Sources
Searching PubMed
"hydronephrosis"[MeSH Terms] AND "treatment"[MeSH Terms]
Finding Sources
Finding Sources
Searching PubMed
"hydronephrosis"[MeSH Terms] AND management
Reading File
Reading File
Reading File
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Finding Sources
Reading File
Reading File
Reading File
Reading File
Loading Image
I now have comprehensive information from multiple authoritative sources. Here is a thorough synthesis:
Hydronephrosis: Treatment
Hydronephrosis is dilation of the renal pelvis and calyces due to obstruction or, less commonly, vesicoureteral reflux. Treatment is directed at the underlying cause and adjusted for severity, acuity, and degree of renal impairment.
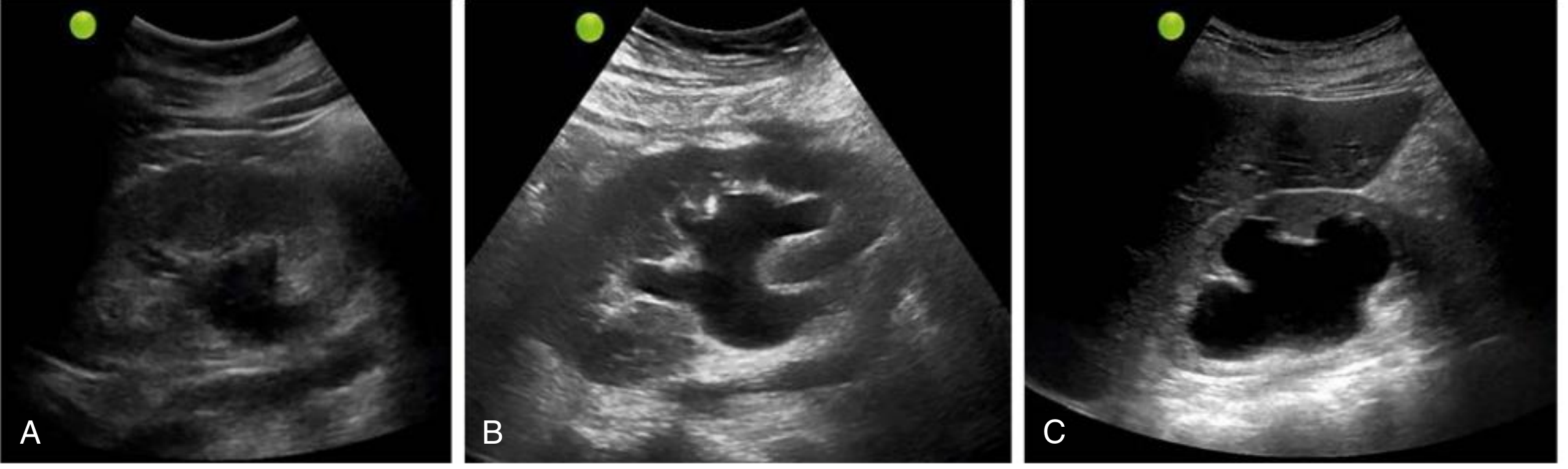
1. General Principles
Treatment is dictated by three factors: location of obstruction, underlying cause, and degree of renal impairment. Close collaboration between nephrology and urology is essential when kidney function is compromised.
- Complete bilateral obstruction (or obstruction of a solitary kidney) causing AKI is a medical emergency — prompt decompression is required to salvage renal function.
- Dialysis is rarely needed for obstructive AKI but may be required to optimize the patient for intervention (e.g., to correct life-threatening hyperkalemia before instrumentation).
- Post-obstructive diuresis is expected after relief of obstruction and may require IV fluid/electrolyte replacement for several days.
"The rapid relief of obstruction will limit permanent kidney damage, but kidney function may not recover immediately if acute tubular injury has resulted from obstruction or any accompanying sepsis." — Comprehensive Clinical Nephrology, 7th Ed.
2. Emergent Decompression
A. Lower Urinary Tract Obstruction (below the bladder)
- Urethral catheterization is the first step (urethral stricture, BPH, posterior urethral valves, neurogenic bladder).
- If a catheter cannot be passed: suprapubic cystostomy.
B. Upper Urinary Tract Obstruction (ureters/renal pelvis)
Two approaches:
| Method | Route | Notes |
|---|---|---|
| Percutaneous nephrostomy (PCN) | Anterograde | Preferred for emergent upper tract decompression; can be done under local anesthesia; allows subsequent antegrade studies to define obstruction |
| Ureteral stent (JJ/double-J) | Retrograde (cystoscopic) | Usually requires general anesthesia; preferred if PCN contraindicated (e.g., therapeutic anticoagulation) |
PCN is the preferred emergent approach for upper urinary tract obstruction with AKI. It achieves renal function recovery in >70% of patients, avoids dialysis, and allows time to plan definitive surgery. PCN is generally not feasible in therapeutic anticoagulation. Major complications (abscess, hematoma) occur in <5%.
- If both kidneys are obstructed, nephrostomy should be placed first in the kidney with better-preserved parenchyma; bilateral nephrostomies may be needed.
- Pyonephrosis (infection + obstruction): PCN is therapeutic alongside antibiotics — this is an urgent indication.
3. Treatment by Cause
Urolithiasis (most common cause of ureteral obstruction)
- Pain relief (NSAIDs, opioids), elimination of the stone, treatment of infection.
- Small stones (<5 mm): watchful waiting ± alpha-blockers (tamsulosin) to facilitate passage.
- Larger stones: ureteroscopy with laser lithotripsy or extracorporeal shock wave lithotripsy (ESWL) or percutaneous nephrolithotomy (PCNL) depending on size/location.
Ureteropelvic Junction (UPJ) Obstruction
The most common surgically correctable cause in children; often detected prenatally.
Conservative management is appropriate for asymptomatic infants/children with preserved renal function — up to 25% will ultimately require surgery for pain, infection, or declining split renal function on diuretic renography.
Indications for surgery:
- Diminished renal function on split renogram
- Massive hydronephrosis
- Symptomatic obstruction (pain, recurrent UTI, stones)
- Declining function on serial imaging
Surgical options:
| Procedure | Description | Notes |
|---|---|---|
| Dismembered pyeloplasty (Anderson-Hynes) | Resects the obstructed segment, reanastomoses ureter to pelvis in a dependent funnel shape | Gold standard; open, laparoscopic, or robotic — success rate >95% |
| Robot-assisted laparoscopic pyeloplasty | Minimally invasive dismembered pyeloplasty | Now preferred in most centers; comparable outcomes to open with better cosmesis and less morbidity |
| Foley Y-V plasty | For dilated extrarenal pelvis combined with dyskinetic segment | Used when creating a more funnel-shaped UPJ is needed |
| Endopyelotomy | Percutaneous or ureteroscopic incision through the obstruction, followed by stenting | ~80% success; preferred for failed primary repair or when concurrent nephrolithiasis requires treatment |
| Balloon dilation | Dilation of the stenotic segment | High recurrence rate — not preferred as primary treatment |
"The remarkable growth of robotic urological surgery has allowed for many more surgeons to become proficient with robot-assisted pyeloplasty, and this has become a preferred option." — Smith & Tanagho's General Urology, 19th Ed.
Laparoscopic/robotic pyeloplasty results in significantly less morbidity with long-term outcomes comparable to open surgery. — Comprehensive Clinical Nephrology, 7th Ed.
BPH / Bladder Outflow Obstruction
- Medical therapy (first-line for most):
- Alpha-1 blockers: tamsulosin, alfuzosin (relax smooth muscle)
- 5α-reductase inhibitors: finasteride, dutasteride (reduce prostate volume)
- Caution: medical therapy is NOT appropriate for high-pressure chronic retention with renal impairment — these patients need surgical decompression.
- Surgical options:
- TURP — gold standard for decades
- HoLEP (Holmium laser enucleation) — superior outcomes for large glands (>100 mL), suitable for anticoagulated patients; 7-year follow-up shows non-inferiority to TURP with less reoperation
- Greenlight laser vaporization
- Newer minimally invasive approaches: UroLift (prostatic urethral lift implants), Aquablation (robotic waterjet), Rezum (water vapor therapy) — aim to preserve sexual function
- Patients with very high post-void residuals (>1 L) or weak detrusor: clean intermittent self-catheterization (CISC) or permanent suprapubic catheter
Malignant Obstruction
- Long-term PCN or ureteral stenting as palliation (metallic stents may give more durable decompression than polymer stents).
- Where ureters are impassable: extra-anatomic stents tunneled subcutaneously from kidney to bladder.
- Chemotherapy-responsive tumors (e.g., lymphoma): systemic treatment may relieve obstruction.
- A "realistic medicine" approach is essential — surgical diversion in terminal malignancy can reduce quality of life.
Retroperitoneal Fibrosis
- Ureterolysis (surgically freeing ureters from fibrous encasement) — can be performed robotically; may offer cure.
- Corticosteroids ± ureteral stenting for acute phase, especially in IgG4-related disease.
Neurogenic Bladder (causing bilateral hydroureteronephrosis)
Goal: maintain low intravesical pressures to protect kidneys.
- Clean intermittent self-catheterization (CISC)
- Anticholinergics
- Intradetrusor botulinum toxin-A injection
- Augmentation cystoplasty (surgical bladder enlargement) for refractory cases
Posterior Urethral Valves (children)
- Mild–moderate: transurethral valve fulguration/ablation (endoscopic).
- Severe with azotemia/sepsis: antibiotics + catheter drainage ± vesicostomy.
- Most severe: percutaneous loop ureterostomies to preserve renal function; then valve ablation and urinary tract reconstruction after stabilization.
- ~50% have associated VUR; resolves spontaneously in ~1/3 after valve ablation; the remainder require surgical correction.
Hydronephrosis of Pregnancy
- Usually physiologic and requires no treatment; resolves within weeks to months postpartum.
- Ureteral stent insertion in symptomatic gestational hydronephrosis does not generally add benefit over conservative management — reserved for complicated cases or additional pathologic obstruction.
4. Monitoring Renal Recovery
- A nephrostomy can be used to gauge potential for functional recovery in chronic obstruction — failure to recover after several weeks of drainage suggests irreversible damage.
- If the obstruction is relieved but there is concurrent rejection in a transplant kidney: biopsy is essential to guide management.
- Repeat diuretic renography (MAG3 scan) confirms operative success after pyeloplasty when radiographic improvement is disappointing.
Key Sources
- Comprehensive Clinical Nephrology, 7th Ed. (Chapters 61, 63)
- Smith & Tanagho's General Urology, 19th Ed.
- Campbell-Walsh-Wein Urology, 4th Ed.
- Harrison's Principles of Internal Medicine, 22nd Ed.
This is a shared conversation. Sign in to Orris to start your own chat.