Diffuse erythematous skin lesions in hiv
Reading File
Finding Sources
Finding Sources
Searching PubMed
"HIV" AND "erythematous skin lesions" AND dermatology
Searching the Web
diffuse erythematous skin lesions HIV differential diagnosis causes management
Reading File
Finding Sources
Searching Images
diffuse erythematous rash HIV skin lesions
Searching PubMed
"HIV" AND "dermatologic manifestations" AND "skin"
Finding Sources
Finding Sources
Loading Image
Loading Image
Reading File
Reading File
Reading File
Finding Sources
Finding Sources
I now have comprehensive information to provide a thorough answer. Let me synthesize everything.
Diffuse Erythematous Skin Lesions in HIV
Erythematous skin lesions in HIV patients span a wide differential that varies critically with CD4 count, stage of infection, ART status, and morphology. The framework below organizes causes by clinical context.
Clinical Approach: Key Diagnostic Anchors
| Factor | Implications |
|---|---|
| CD4 > 500 | Acute seroconversion rash, seborrheic dermatitis, psoriasis |
| CD4 350–500 | Seborrheic dermatitis (severe), psoriasis, herpes zoster |
| CD4 200–350 | Drug reactions, eosinophilic folliculitis, secondary syphilis |
| CD4 < 200 | Eosinophilic folliculitis, PPE, Norwegian scabies, Kaposi sarcoma, deep fungal, IRIS |
| On ART recently | Drug hypersensitivity, IRIS |
1. Acute HIV Seroconversion Exanthem
The classic initial presentation. Occurs 2–6 weeks after primary infection in ~70% of symptomatic cases.
- Morphology: Diffuse, non-pruritic maculopapular erythematous eruption on face, trunk, palms, and soles
- Associations: Fever, pharyngitis, lymphadenopathy, myalgias/arthralgias, mucosal ulcers (oral/genital)
- Differential: Drug eruption, secondary syphilis, EBV/CMV exanthem
- Diagnosis: HIV RNA viral load (very high), p24 antigen; antibody tests may still be negative
- Harrison's 22E, p. 445
2. Morbiliform (Measles-like) Maculopapular Rash — Differential by Morphology
Per the Hong Kong AIDS guidelines, this pattern in HIV suggests:
- Acute retroviral syndrome (most common)
- Drug reaction (especially abacavir, nevirapine, NNRTIs)
- Secondary syphilis — always keep in differential for diffuse erythematous rash
3. Drug Hypersensitivity Reactions
A major cause, particularly in patients on ART.
- Abacavir (NRTI): Hypersensitivity in ~5% of patients; fever + rash + GI upset. Life-threatening on re-challenge. Associated with HLA-B*57:01 — screen before prescribing. - Lippincott Pharmacology
- Nevirapine, efavirenz: Maculopapular rash in 15–30%; can progress to SJS/TEN
- Sulfonamides (e.g., TMP-SMX for PCP prophylaxis): Rash in up to 60% of HIV patients
- Rash may be morbiliform or erythrodermic (>90% body surface area involvement)
4. Seborrheic Dermatitis
One of the most common HIV-associated dermatoses; prevalence and severity track inversely with CD4 count.
- Morphology: Erythematous, scaly/greasy patches on face (nasolabial folds, eyebrows, scalp), upper chest
- In advanced HIV: diffuse involvement across the trunk and extremities
- Pathogenesis: Malassezia spp. overgrowth in setting of immune dysregulation
- Treatment: Topical antifungals (ketoconazole shampoo/cream), low-potency topical steroids, calcineurin inhibitors; treat underlying HIV
- Fitzpatrick's Dermatology, p. 3151
5. Psoriasis
Can be the presenting sign that triggers HIV testing when atypical.
- Most common variant in HIV: plaque psoriasis (erythematous, well-demarcated plaques with silvery scale on extensors)
- HIV-specific variants: erythrodermic psoriasis (particularly in sub-Saharan Africa), rupioid psoriasis, palmoplantar involvement (keratoderma blennorrhagica)
- Paradoxically worsens despite CD4 depletion; may flare with IRIS
- Treatment: Topical (mild) → phototherapy (moderate) → acitretin → ART (first-line for moderate-severe); biologics used very cautiously due to immunosuppression risk
- Fitzpatrick's Dermatology
6. Eosinophilic Folliculitis (EF)
- CD4 typically < 250–300 cells/mm³
- Morphology: Intensely pruritic, follicle-centered erythematous papules/pustules on the midline — face, scalp, neck, upper trunk
- Distinct from bacterial folliculitis; biopsy shows eosinophilic infiltration
- Treatment: ART is first-line; symptomatic relief with antihistamines, topical steroids, phototherapy (UVB), itraconazole
7. Papular Pruritic Eruption (PPE)
- More common in tropical/subtropical HIV populations; CD4 < 200
- Morphology: Pruritic, symmetric erythematous papules — predominantly on distal extremities (unlike EF)
- Likely represents hypersensitivity to insect bites in the setting of immune dysregulation
- Treatment: ART; topical steroids, antihistamines, UVA/UVB phototherapy
8. Secondary Syphilis
Always in the differential for diffuse erythematous rash in HIV.
- Polymorphic rash: macules, papules, targetoid lesions on trunk, palms, soles
- May be atypical and more florid in HIV — shown in the image below
- Diagnose with RPR/VDRL + confirmatory FTA-ABS or TPPA
- Treatment: Benzathine penicillin G
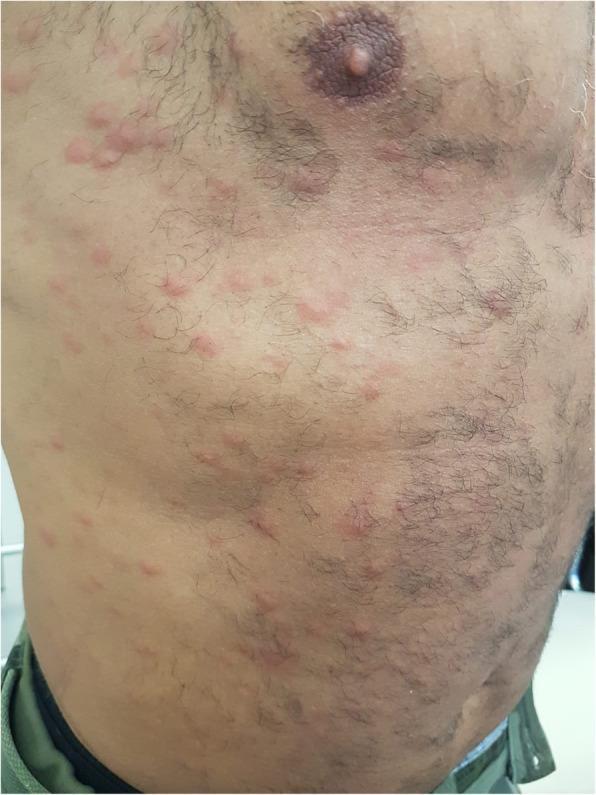
9. Norwegian (Crusted) Scabies
- Occurs with severe immunosuppression
- Morphology: Erythroderma (diffuse erythema + hyperkeratotic scale), especially hands, feet, scalp, face; highly contagious
- Differs from classic scabies by massive mite burden (millions vs. 10–15)
- Treatment: Ivermectin + topical permethrin; isolation
10. Kaposi Sarcoma (KS)
- AIDS-defining; caused by HHV-8 (KSHV); CD4 typically < 200
- Morphology: Red-to-violaceous/brown macules, papules, and plaques — may be widespread and erythematous in early stages
- Favors face, lower extremities, mucosal surfaces
- Diagnosis: Skin biopsy (spindle cells, slit-like vascular spaces)
- Treatment: ART (lesions may regress); chemotherapy (liposomal doxorubicin) for extensive disease
11. Immune Reconstitution Inflammatory Syndrome (IRIS)
- Occurs in up to 20% of patients starting ART, typically within the first 2–3 months
- Previously subclinical infections or dermatoses "unmask" or paradoxically worsen
- Cutaneous manifestations: eosinophilic folliculitis flares, molluscum, herpes, KS, psoriasis
- Management: Continue ART; prednisone 1 mg/kg (taper) for significant reactions; avoid steroids in KS-IRIS
- Fitzpatrick's Dermatology, p. 141
12. Other Causes by Morphology
| Morphology | Consider |
|---|---|
| Erythroderma (>90% BSA) | Drug reaction, psoriasis, Norwegian scabies, seborrheic dermatitis |
| Follicular papules/pustules | Bacterial/fungal/eosinophilic folliculitis, acne |
| Nodular with erythema | Bacillary angiomatosis (Bartonella spp.), deep fungal (cryptococcosis, talaromycosis in SE Asia) |
| Ulcerated erythematous base | HSV, CMV, mycobacterial, deep fungal |
| Targetoid/multiform | Drug reaction (erythema multiforme), secondary syphilis |
Diagnostic Algorithm
Diffuse erythematous rash in HIV patient
↓
1. Check CD4 count + viral load + ART history
2. Drug history — new medication in last 1–8 weeks?
3. Morphology classification (morbiliform, follicular, erythrodermic)
4. Always obtain RPR/VDRL (syphilis)
5. Skin biopsy if diagnosis unclear
6. Culture/PCR if infectious etiology suspected
Key investigations: CBC with differential (eosinophilia → drug, EF), RPR, HSV/VZV PCR, KOH scrape (fungal), skin biopsy, HLA-B*57:01 before abacavir.
References: Harrison's Principles of Internal Medicine 22E (2025); Fitzpatrick's Dermatology 9E; Dermatology 2-Vol Set 5E (Elsevier); National HIV Curriculum — Cutaneous Manifestations; Mohseni Afshar Z et al. Int J Microbiol 2023 [PMID 37496761]
This is a shared conversation. Sign in to Orris to start your own chat.